Introduction
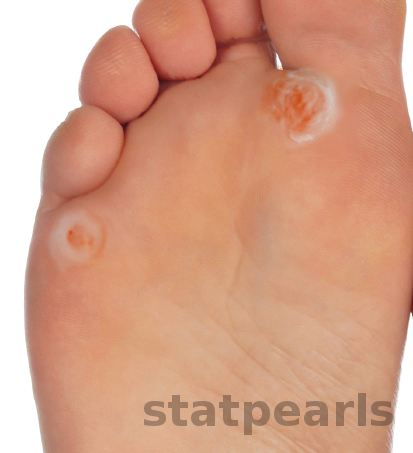
A clavus or clavi (plural) is a frequently encountered condition in the out-patient clinic, known colloquially as a corn. It is one of the many hyperkeratotic lesions of the foot and therefore requires differentiation from other etiologies such as calluses or plantar warts. A clavus is a well-demarcated thickened area of the epidermis that has a central core. This skin lesion is most commonly found on the foot and is often painful. A clavus results from repeated friction, pressure, or trauma to a specific area of the foot. A callus is another hyperkeratotic skin lesion that is similar to a clavus. It is an area of thickened epidermis with less defined borders and is also the result of repeated mechanical stress. Additionally, calluses lack the painful central core seen with clavi. Calluses most commonly present on the hands and feet. The older and the physically active are most commonly affected by clavi. Treatment focuses on symptomatic relief and lifestyle modification to prevent future clavus formation. By treating this painful and sometimes life-altering skin lesion, physicians can have a profound impact on their patients’ lives.[1][2][3]
Etiology
Clavi are the result of microtrauma to the epidermis; this is usually in the form of repeated pressure or friction to the affected area. Other factors such as physical activity, ill-fitting footwear, and foot deformities causing bony prominences contribute to the development of clavi. Diabetic patients and people exposed to unequal frictional forces or gait abnormalities are at increased risk of developing a clavus. The most common location is the foot, including the dorsolateral aspect of the fifth interphalangeal joint, between the toes, and on the sole. The foot is extremely susceptible to the development of clavi due to the amount of repeated mechanical stress introduced to the area daily.[1][2]
Epidemiology
Patients over 65 years of age are most commonly affected by painful clavi. The epidermis undergoes many changes with age, resulting in a thinner and dryer protective layer; this could contribute to a higher prevalence of clavi in the older population. There is also a slight female predominance, most likely due to an increase in ill-fitting footwear.[3]
Pathophysiology
Repeated mechanical stress to a specific area of the epidermis causes hyperkeratosis, defined as the hypertrophy or hyperplasia of the cells within the stratum corneum. Hyperkeratosis is a normal physiologic protective mechanism of the epidermis. It becomes pathological when a clavus forms and causes the patient to experience pain. This pain results in the central core of the clavus pressing on underlying nervous structures.[3][4]
Histopathology
Histopathological evaluation is not necessary for the diagnosis of clavus. Therefore, a biopsy of the lesion is a rarity. Tissue biopsy of a clavus will demonstrate the increased thickness of all epidermal layers (acanthosis), including a marked increase in the stratum corneum. There will also be a decrease in keratinocyte density and an abnormal rete ridge pattern. Dermal changes may include fibrosis.[5]
History and Physical
Clavi diagnosis is by clinical presentation. The history and physical exam are the physician’s greatest tools when making the diagnosis. The clinician should obtain a history from the patient about symptomatology, physical activity, footwear, and home treatment. On physical exam, there will be a sharply demarcated, well-circumscribed area of rough, thickened skin. Most importantly, there will be a translucent core in the center of the lesion. This core presses into the underlying dermis resulting in pain and inflammation. The central core is a distinguishing feature from other hyperkeratotic lesions such as calluses or plantar warts.
There are two types of clavi: soft and hard. Hard clavi are most commonly located on the dorsum of interphalangeal joints of the toes and are dry, rough, horny skin lesions. Soft clavi occurs in interdigital spaces of the foot where moisture content is high. These lesions can be extremely painful for the patient. Look for well-circumscribed macerated tissue in between toes.
A physician may have difficulty distinguishing a clavus from a plantar wart. There are differentiating characteristics that separate the two skin conditions. The central core is a defining feature in a clavus. Next, skin lines will be preserved with the hyperkeratosis of a clavus and will be absent in a plantar wart. Deep palpation by the physician to a clavus will cause pain; this is not the case with plantar warts unless there is severe hyperkeratosis causing pressure on underlying nerves. Finally, pinpoint, dark, hemorrhagic foci seen with plantar warts are absent in a clavus.[6]
Evaluation
The basis of the diagnosis of a clavus is on location, symptomatology, and morphology of the lesion. Dermoscopy can aid in the differentiation of hyperkeratotic lesions. The loss of skin lines and punctate hemorrhages seen with plantar warts will be absent in clavi.[7] Plain film X-rays of the foot can be utilized to identify underlying bony prominences contributing to the formation of the skin lesion, which can aid the physician in the decision to refer the patient to a surgeon.[6]
Treatment / Management
It is important to remember that clavi are the result of trauma to the epidermis and not a disease of the epidermis. Treatment of clavi can be performed in the family medicine office and does not require specialist referral unless there are refractory skin lesions.[8]
There are three principal points to address when treating a clavus:
1) Provide symptomatic relief to the patient. This is possible by the physician paring down the lesion with a 15 blade scalpel and removing the central core of the clavus. The patient almost instantly experiences relief to the affected area. Patients can also be instructed to reduce the size of the clavus at home by soaking the affected foot in warm water and using a pumice stone or emery board to remove the hyperkeratotic material. Topical keratolytics, such as 10 to 15% salicylic acid, can be applied to the clavus with some benefit. However, improper application or over-application of the keratolytic increases the chance of chemical burns and damage to the surrounding epidermis. Therefore, most recommend against the use of topical over-the-counter products such as salicylic acid.
2) Address the mechanical etiology causing the hyperkeratosis and formulate a treatment plan that includes padding and properly fitting footwear. This is among the most critical aspects of the treatment plan. The clavus is a result of repeated friction or pressure to the affected area. Therefore, the physician needs to investigate the causes of the skin lesion to prevent a recurrence. The padding of the toes and sole is crucial to reduce the amount of mechanical stress to the afflicted area. Adhesive pads, silicone sleeves, and foam toe spacers can all function in this capacity. Patients require education on the necessity for properly fitted footwear. They should have their feet measured for proper sizing and buy shoes with low heels, a soft upper portion, and a roomy toe box. Finally, when treating soft clavi, the patient must be educated on ways to minimize excess moisture of the feet.[2]
3) Consider surgical consultation with an orthopedic surgeon or podiatrist if conservative management fails. Surgical correction of foot deformities and bony prominences should be performed by a surgeon to realign the foot, minimize mechanical stress, and prevent painful lesions.[6][9]
Differential Diagnosis
- Callus
- Plantar wart
- Common wart
- Foreign body granuloma
- Plantar porokeratosis
- Tinea pedis - if a soft clavus
Prognosis
A clavus is a chronic recurrent issue for many patients. However, skin lesions will cease to recur following the elimination of mechanical stress from the affected area. For recalcitrant clavi, a surgical referral is needed to minimize the mechanical stress.[2]
Complications
Clavi are very common in the older population and are a significant cause of foot pain. Untreated or recurrent painful clavi can affect the mobility of the patient, which in turn affects their independence. Foot pain correlates with functional limitations, decreased ability to complete activities of daily living, and increases the risk of falls. Therefore, it is crucial to treat and prevent the formation of clavi, especially in the older population.[10]
Deterrence and Patient Education
Patient education is of utmost importance for the proper treatment and prevention of further clavi formation. The physician must outline to the patient the causative factors behind their condition and measures that need to be taken to prevent recurrences, helping to ensure proper adherence to the treatment plan by the patient.
One potential issue encountered during the treatment plan is the need for proper fitting foot-wear, which can be problematic because the patient will need to discard his or her old shoes and buy new ones that fit correctly. Patients will be more apt to follow this plan if the physician takes time to explain thoroughly the necessity of properly fitting shoes.
Enhancing Healthcare Team Outcomes
To improve patient outcomes, treatment of clavi require an interprofessional approach. The center of the healthcare team is the patient. Environmental stressors are at the heart of the disease process. Therefore, it is necessary for the physician and the patient to work together to conduct a thorough investigation of the causes of the trauma and ways to mitigate future stress to the area, which will require a cooperative patient that is willing to make life alterations to prevent future recurrence of the clavus. The healthcare team may also include referral to an orthopedic surgeon or podiatrist if a clavus is resistant to conservative management.
Nursing will assist in educating the patient, help with minor in-office surgical procedures, and assess treatment effectiveness and compliance, reporting findings to the physician and charting their observations. Pharmacists can make recommendations for products available in the pharmacy, including pads, insoles, pumice stones, salicylic acid formulations, and so on; they should coordinate with the patient's physician to ensure the message to the patient is consistent. Clavi are not a dangerous condition, but they still are best addressed through the efforts of an interprofessional healthcare team working collaboratively to provide patient care leading to the best outcomes. [Level-V]