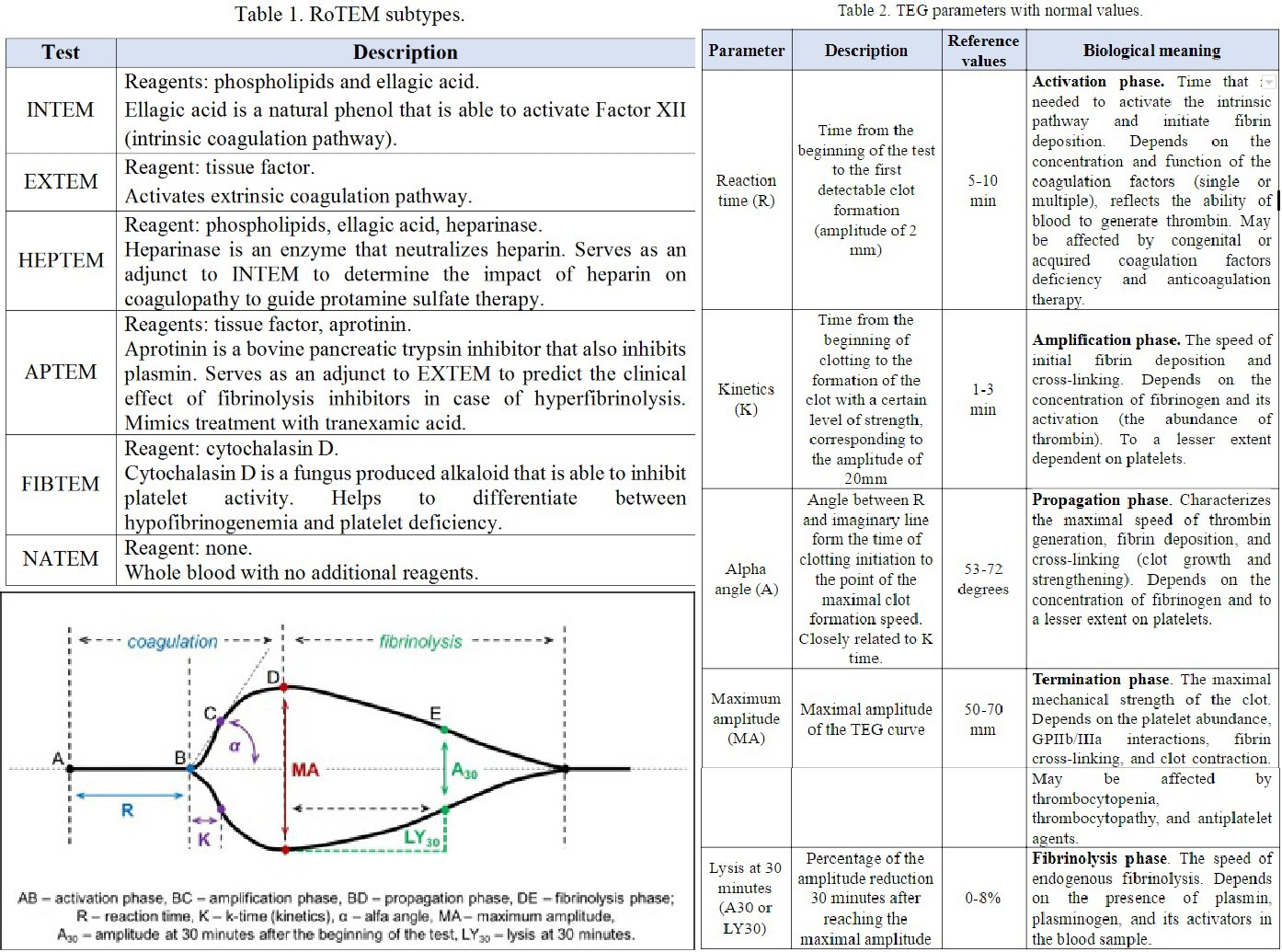
[1]
Sobrino J, Shafi S. Timing and causes of death after injuries. Proceedings (Baylor University. Medical Center). 2013 Apr:26(2):120-3
[PubMed PMID: 23543966]
[2]
Brohi K, Singh J, Heron M, Coats T. Acute traumatic coagulopathy. The Journal of trauma. 2003 Jun:54(6):1127-30
[PubMed PMID: 12813333]
[3]
Barnes GD, Lucas E, Alexander GC, Goldberger ZD. National Trends in Ambulatory Oral Anticoagulant Use. The American journal of medicine. 2015 Dec:128(12):1300-5.e2. doi: 10.1016/j.amjmed.2015.05.044. Epub 2015 Jul 2
[PubMed PMID: 26144101]
[4]
Luepker RV, Steffen LM, Duval S, Zantek ND, Zhou X, Hirsch AT. Population Trends in Aspirin Use for Cardiovascular Disease Prevention 1980-2009: The Minnesota Heart Survey. Journal of the American Heart Association. 2015 Dec 23:4(12):. doi: 10.1161/JAHA.115.002320. Epub 2015 Dec 23
[PubMed PMID: 26702085]
Level 3 (low-level) evidence
[5]
Rodgers RP, Levin J. A critical reappraisal of the bleeding time. Seminars in thrombosis and hemostasis. 1990 Jan:16(1):1-20
[PubMed PMID: 2406907]
[6]
Johnson DJ, Scott AV, Barodka VM, Park S, Wasey JO, Ness PM, Gniadek T, Frank SM. Morbidity and Mortality after High-dose Transfusion. Anesthesiology. 2016 Feb:124(2):387-95. doi: 10.1097/ALN.0000000000000945. Epub
[PubMed PMID: 26569167]
[7]
HARTERT H. [Blood clotting studies with Thrombus stressography; a new Investigation procedure]. Klinische Wochenschrift. 1948 Oct 1:26(37-38):577-83
[PubMed PMID: 18101974]
[8]
Walsh M, Fritz S, Hake D, Son M, Greve S, Jbara M, Chitta S, Fritz B, Miller A, Bader MK, McCollester J, Binz S, Liew-Spilger A, Thomas S, Crepinsek A, Shariff F, Ploplis V, Castellino FJ. Targeted Thromboelastographic (TEG) Blood Component and Pharmacologic Hemostatic Therapy in Traumatic and Acquired Coagulopathy. Current drug targets. 2016:17(8):954-70
[PubMed PMID: 26960340]
[9]
Kang YG, Martin DJ, Marquez J, Lewis JH, Bontempo FA, Shaw BW Jr, Starzl TE, Winter PM. Intraoperative changes in blood coagulation and thrombelastographic monitoring in liver transplantation. Anesthesia and analgesia. 1985 Sep:64(9):888-96
[PubMed PMID: 3896028]
[10]
Shore-Lesserson L, Manspeizer HE, DePerio M, Francis S, Vela-Cantos F, Ergin MA. Thromboelastography-guided transfusion algorithm reduces transfusions in complex cardiac surgery. Anesthesia and analgesia. 1999 Feb:88(2):312-9
[PubMed PMID: 9972747]
[11]
Quarterman C, Shaw M, Johnson I, Agarwal S. Intra- and inter-centre standardisation of thromboelastography (TEG®). Anaesthesia. 2014 Aug:69(8):883-90. doi: 10.1111/anae.12748. Epub 2014 May 20
[PubMed PMID: 24841452]
[12]
Cotton BA, Faz G, Hatch QM, Radwan ZA, Podbielski J, Wade C, Kozar RA, Holcomb JB. Rapid thrombelastography delivers real-time results that predict transfusion within 1 hour of admission. The Journal of trauma. 2011 Aug:71(2):407-14; discussion 414-7. doi: 10.1097/TA.0b013e31821e1bf0. Epub
[PubMed PMID: 21825945]
[13]
Pezold M, Moore EE, Wohlauer M, Sauaia A, Gonzalez E, Banerjee A, Silliman CC. Viscoelastic clot strength predicts coagulation-related mortality within 15 minutes. Surgery. 2012 Jan:151(1):48-54. doi: 10.1016/j.surg.2011.06.023. Epub 2011 Sep 6
[PubMed PMID: 21899867]
[14]
Caprini JA, Zuckerman L, Cohen E, Vagher JP, Lipp V. The identification of accelerated coagulability. Thrombosis research. 1976 Aug:9(2):167-80
[PubMed PMID: 788222]
[15]
Caprini JA, Arcelus JI, Laubach M, Size G, Hoffman KN, Coats RW 2nd, Blattner S. Postoperative hypercoagulability and deep-vein thrombosis after laparoscopic cholecystectomy. Surgical endoscopy. 1995 Mar:9(3):304-9
[PubMed PMID: 7597604]
[16]
Ng KF. Changes in thrombelastograph variables associated with aging. Anesthesia and analgesia. 2004 Aug:99(2):449-54, table of contents
[PubMed PMID: 15271723]
[17]
Scarpelini S, Rhind SG, Nascimento B, Tien H, Shek PN, Peng HT, Huang H, Pinto R, Speers V, Reis M, Rizoli SB. Normal range values for thromboelastography in healthy adult volunteers. Brazilian journal of medical and biological research = Revista brasileira de pesquisas medicas e biologicas. 2009 Dec:42(12):1210-7
[PubMed PMID: 19882085]
[18]
Lang T, Bauters A, Braun SL, Pötzsch B, von Pape KW, Kolde HJ, Lakner M. Multi-centre investigation on reference ranges for ROTEM thromboelastometry. Blood coagulation & fibrinolysis : an international journal in haemostasis and thrombosis. 2005 Jun:16(4):301-10
[PubMed PMID: 15870552]
[19]
Coakley M, Reddy K, Mackie I, Mallett S. Transfusion triggers in orthotopic liver transplantation: a comparison of the thromboelastometry analyzer, the thromboelastogram, and conventional coagulation tests. Journal of cardiothoracic and vascular anesthesia. 2006 Aug:20(4):548-53
[PubMed PMID: 16884987]
[20]
Nielsen VG. A comparison of the Thrombelastograph and the ROTEM. Blood coagulation & fibrinolysis : an international journal in haemostasis and thrombosis. 2007 Apr:18(3):247-52
[PubMed PMID: 17413761]
[21]
Durila M. Nonactivated thromboelastometry able to detect fibrinolysis in contrast to activated methods (EXTEM, INTEM) in a bleeding patient. Blood coagulation & fibrinolysis : an international journal in haemostasis and thrombosis. 2016 Oct:27(7):828-830
[PubMed PMID: 26656899]
[22]
Wikkelsø A, Wetterslev J, Møller AM, Afshari A. Thromboelastography (TEG) or thromboelastometry (ROTEM) to monitor haemostatic treatment versus usual care in adults or children with bleeding. The Cochrane database of systematic reviews. 2016 Aug 22:2016(8):CD007871. doi: 10.1002/14651858.CD007871.pub3. Epub 2016 Aug 22
[PubMed PMID: 27552162]
Level 1 (high-level) evidence
[23]
Adler M, Ivic S, Bodmer NS, Ten Cate H, Bachmann LM, Wuillemin WA, Nagler M. Thromboelastometry and Thrombelastography Analysis under Normal Physiological Conditions - Systematic Review. Transfusion medicine and hemotherapy : offizielles Organ der Deutschen Gesellschaft fur Transfusionsmedizin und Immunhamatologie. 2017 Apr:44(2):78-83. doi: 10.1159/000464297. Epub 2017 Mar 8
[PubMed PMID: 28503123]
Level 1 (high-level) evidence
[24]
Deppe AC, Weber C, Zimmermann J, Kuhn EW, Slottosch I, Liakopoulos OJ, Choi YH, Wahlers T. Point-of-care thromboelastography/thromboelastometry-based coagulation management in cardiac surgery: a meta-analysis of 8332 patients. The Journal of surgical research. 2016 Jun 15:203(2):424-33. doi: 10.1016/j.jss.2016.03.008. Epub 2016 Mar 26
[PubMed PMID: 27363652]
Level 1 (high-level) evidence
[25]
Wikkelsø A, Wetterslev J, Møller AM, Afshari A. Thromboelastography (TEG) or rotational thromboelastometry (ROTEM) to monitor haemostatic treatment in bleeding patients: a systematic review with meta-analysis and trial sequential analysis. Anaesthesia. 2017 Apr:72(4):519-531. doi: 10.1111/anae.13765. Epub 2017 Jan 4
[PubMed PMID: 28052313]
Level 1 (high-level) evidence
[26]
Nakayama Y, Nakajima Y, Tanaka KA, Sessler DI, Maeda S, Iida J, Ogawa S, Mizobe T. Thromboelastometry-guided intraoperative haemostatic management reduces bleeding and red cell transfusion after paediatric cardiac surgery. British journal of anaesthesia. 2015 Jan:114(1):91-102. doi: 10.1093/bja/aeu339. Epub 2014 Oct 10
[PubMed PMID: 25303988]
[27]
Whiting P, Al M, Westwood M, Ramos IC, Ryder S, Armstrong N, Misso K, Ross J, Severens J, Kleijnen J. Viscoelastic point-of-care testing to assist with the diagnosis, management and monitoring of haemostasis: a systematic review and cost-effectiveness analysis. Health technology assessment (Winchester, England). 2015 Jul:19(58):1-228, v-vi. doi: 10.3310/hta19580. Epub
[PubMed PMID: 26215747]
Level 1 (high-level) evidence
[28]
Hunt H, Stanworth S, Curry N, Woolley T, Cooper C, Ukoumunne O, Zhelev Z, Hyde C. Thromboelastography (TEG) and rotational thromboelastometry (ROTEM) for trauma induced coagulopathy in adult trauma patients with bleeding. The Cochrane database of systematic reviews. 2015 Feb 16:2015(2):CD010438. doi: 10.1002/14651858.CD010438.pub2. Epub 2015 Feb 16
[PubMed PMID: 25686465]
Level 1 (high-level) evidence
[29]
Holcomb JB, Minei KM, Scerbo ML, Radwan ZA, Wade CE, Kozar RA, Gill BS, Albarado R, McNutt MK, Khan S, Adams PR, McCarthy JJ, Cotton BA. Admission rapid thrombelastography can replace conventional coagulation tests in the emergency department: experience with 1974 consecutive trauma patients. Annals of surgery. 2012 Sep:256(3):476-86. doi: 10.1097/SLA.0b013e3182658180. Epub
[PubMed PMID: 22868371]
[30]
Da Luz LT, Nascimento B, Shankarakutty AK, Rizoli S, Adhikari NK. Effect of thromboelastography (TEG®) and rotational thromboelastometry (ROTEM®) on diagnosis of coagulopathy, transfusion guidance and mortality in trauma: descriptive systematic review. Critical care (London, England). 2014 Sep 27:18(5):518. doi: 10.1186/s13054-014-0518-9. Epub 2014 Sep 27
[PubMed PMID: 25261079]
Level 1 (high-level) evidence
[31]
Veigas PV, Callum J, Rizoli S, Nascimento B, da Luz LT. A systematic review on the rotational thrombelastometry (ROTEM®) values for the diagnosis of coagulopathy, prediction and guidance of blood transfusion and prediction of mortality in trauma patients. Scandinavian journal of trauma, resuscitation and emergency medicine. 2016 Oct 3:24(1):114
[PubMed PMID: 27716278]
Level 1 (high-level) evidence
[32]
Panigada M, E Iapichino G, Brioni M, Panarello G, Protti A, Grasselli G, Occhipinti G, Novembrino C, Consonni D, Arcadipane A, Gattinoni L, Pesenti A. Thromboelastography-based anticoagulation management during extracorporeal membrane oxygenation: a safety and feasibility pilot study. Annals of intensive care. 2018 Jan 16:8(1):7. doi: 10.1186/s13613-017-0352-8. Epub 2018 Jan 16
[PubMed PMID: 29340875]
Level 2 (mid-level) evidence
[33]
Collyer TC, Gray DJ, Sandhu R, Berridge J, Lyons G. Assessment of platelet inhibition secondary to clopidogrel and aspirin therapy in preoperative acute surgical patients measured by Thrombelastography Platelet Mapping. British journal of anaesthesia. 2009 Apr:102(4):492-8. doi: 10.1093/bja/aep039. Epub
[PubMed PMID: 19286767]
[34]
Sharma P, Saxena R. A novel thromboelastographic score to identify overt disseminated intravascular coagulation resulting in a hypocoagulable state. American journal of clinical pathology. 2010 Jul:134(1):97-102. doi: 10.1309/AJCPPZ4J6CAFYDVM. Epub
[PubMed PMID: 20551273]
[35]
Kawano-Castillo J, Ward E, Elliott A, Wetzel J, Hassler A, McDonald M, Parker SA, Archeval-Lao J, Tremont C, Cai C, Pivalizza E, Rahbar MH, Grotta JC. Thrombelastography detects possible coagulation disturbance in patients with intracerebral hemorrhage with hematoma enlargement. Stroke. 2014 Mar:45(3):683-8. doi: 10.1161/STROKEAHA.113.003826. Epub 2014 Jan 14
[PubMed PMID: 24425123]
[36]
Lisman T, Porte RJ. Rebalanced hemostasis in patients with liver disease: evidence and clinical consequences. Blood. 2010 Aug 12:116(6):878-85. doi: 10.1182/blood-2010-02-261891. Epub 2010 Apr 16
[PubMed PMID: 20400681]
[37]
Mallett SV. Clinical Utility of Viscoelastic Tests of Coagulation (TEG/ROTEM) in Patients with Liver Disease and during Liver Transplantation. Seminars in thrombosis and hemostasis. 2015 Jul:41(5):527-37. doi: 10.1055/s-0035-1550434. Epub 2015 Jun 6
[PubMed PMID: 26049072]
[38]
Roullet S, Pillot J, Freyburger G, Biais M, Quinart A, Rault A, Revel P, Sztark F. Rotation thromboelastometry detects thrombocytopenia and hypofibrinogenaemia during orthotopic liver transplantation. British journal of anaesthesia. 2010 Apr:104(4):422-8. doi: 10.1093/bja/aeq022. Epub 2010 Feb 25
[PubMed PMID: 20185519]
[39]
Kozek-Langenecker SA, Ahmed AB, Afshari A, Albaladejo P, Aldecoa C, Barauskas G, De Robertis E, Faraoni D, Filipescu DC, Fries D, Haas T, Jacob M, Lancé MD, Pitarch JVL, Mallett S, Meier J, Molnar ZL, Rahe-Meyer N, Samama CM, Stensballe J, Van der Linden PJF, Wikkelsø AJ, Wouters P, Wyffels P, Zacharowski K. Management of severe perioperative bleeding: guidelines from the European Society of Anaesthesiology: First update 2016. European journal of anaesthesiology. 2017 Jun:34(6):332-395. doi: 10.1097/EJA.0000000000000630. Epub
[PubMed PMID: 28459785]
[40]
Wysowski DK, Nourjah P, Swartz L. Bleeding complications with warfarin use: a prevalent adverse effect resulting in regulatory action. Archives of internal medicine. 2007 Jul 9:167(13):1414-9
[PubMed PMID: 17620536]
[41]
Dossett LA, Riesel JN, Griffin MR, Cotton BA. Prevalence and implications of preinjury warfarin use: an analysis of the National Trauma Databank. Archives of surgery (Chicago, Ill. : 1960). 2011 May:146(5):565-70. doi: 10.1001/archsurg.2010.313. Epub 2011 Jan 17
[PubMed PMID: 21242422]
[42]
Rose AJ, Ozonoff A, Grant RW, Henault LE, Hylek EM. Epidemiology of subtherapeutic anticoagulation in the United States. Circulation. Cardiovascular quality and outcomes. 2009 Nov:2(6):591-7. doi: 10.1161/CIRCOUTCOMES.109.862763. Epub 2009 Sep 22
[PubMed PMID: 20031897]
Level 2 (mid-level) evidence
[43]
Favaloro EJ, Lippi G. Laboratory testing in the era of direct or non-vitamin K antagonist oral anticoagulants: a practical guide to measuring their activity and avoiding diagnostic errors. Seminars in thrombosis and hemostasis. 2015 Mar:41(2):208-27. doi: 10.1055/s-0035-1546827. Epub 2015 Feb 19
[PubMed PMID: 25703514]
[44]
Connolly SJ, Ezekowitz MD, Yusuf S, Eikelboom J, Oldgren J, Parekh A, Pogue J, Reilly PA, Themeles E, Varrone J, Wang S, Alings M, Xavier D, Zhu J, Diaz R, Lewis BS, Darius H, Diener HC, Joyner CD, Wallentin L, RE-LY Steering Committee and Investigators. Dabigatran versus warfarin in patients with atrial fibrillation. The New England journal of medicine. 2009 Sep 17:361(12):1139-51. doi: 10.1056/NEJMoa0905561. Epub 2009 Aug 30
[PubMed PMID: 19717844]
[45]
Giugliano RP, Ruff CT, Braunwald E, Murphy SA, Wiviott SD, Halperin JL, Waldo AL, Ezekowitz MD, Weitz JI, Špinar J, Ruzyllo W, Ruda M, Koretsune Y, Betcher J, Shi M, Grip LT, Patel SP, Patel I, Hanyok JJ, Mercuri M, Antman EM, ENGAGE AF-TIMI 48 Investigators. Edoxaban versus warfarin in patients with atrial fibrillation. The New England journal of medicine. 2013 Nov 28:369(22):2093-104. doi: 10.1056/NEJMoa1310907. Epub 2013 Nov 19
[PubMed PMID: 24251359]
[46]
Figueiredo S, Vigué B, Benhamou D, Duranteau J. Emergency reversal of heparin overdose in a neurosurgical patient guided by thromboelastography. British journal of anaesthesia. 2013 Aug:111(2):303-4. doi: 10.1093/bja/aet245. Epub
[PubMed PMID: 23858079]
[47]
Matetzky S, Shenkman B, Guetta V, Shechter M, Beinart R, Goldenberg I, Novikov I, Pres H, Savion N, Varon D, Hod H. Clopidogrel resistance is associated with increased risk of recurrent atherothrombotic events in patients with acute myocardial infarction. Circulation. 2004 Jun 29:109(25):3171-5
[PubMed PMID: 15184279]
[48]
Gum PA, Kottke-Marchant K, Welsh PA, White J, Topol EJ. A prospective, blinded determination of the natural history of aspirin resistance among stable patients with cardiovascular disease. Journal of the American College of Cardiology. 2003 Mar 19:41(6):961-5
[PubMed PMID: 12651041]
[49]
Michelson AD, Bhatt DL. How I use laboratory monitoring of antiplatelet therapy. Blood. 2017 Aug 10:130(6):713-721. doi: 10.1182/blood-2017-03-742338. Epub 2017 Jun 9
[PubMed PMID: 28600334]
[50]
Kashuk JL, Moore EE, Sabel A, Barnett C, Haenel J, Le T, Pezold M, Lawrence J, Biffl WL, Cothren CC, Johnson JL. Rapid thrombelastography (r-TEG) identifies hypercoagulability and predicts thromboembolic events in surgical patients. Surgery. 2009 Oct:146(4):764-72; discussion 772-4. doi: 10.1016/j.surg.2009.06.054. Epub
[PubMed PMID: 19789037]
[51]
Tartamella F, Vassallo MC, Berlot G, Grassi P, Testa F. Thromboelastographic predictors of venous thromboembolic events in critically ill patients: are we missing something? Blood coagulation & fibrinolysis : an international journal in haemostasis and thrombosis. 2016 Oct:27(7):804-811
[PubMed PMID: 26895213]
[52]
Liu J, Wang N, Chen Y, Lu R, Ye X. Thrombelastography coagulation index may be a predictor of venous thromboembolism in gynecological oncology patients. The journal of obstetrics and gynaecology research. 2017 Jan:43(1):202-210. doi: 10.1111/jog.13154. Epub 2016 Oct 20
[PubMed PMID: 27762468]
[53]
Toukh M, Siemens DR, Black A, Robb S, Leveridge M, Graham CH, Othman M. Thromboelastography identifies hypercoagulablilty and predicts thromboembolic complications in patients with prostate cancer. Thrombosis research. 2014 Jan:133(1):88-95. doi: 10.1016/j.thromres.2013.10.007. Epub 2013 Oct 12
[PubMed PMID: 24246296]
[54]
Brill JB, Badiee J, Zander AL, Wallace JD, Lewis PR, Sise MJ, Bansal V, Shackford SR. The rate of deep vein thrombosis doubles in trauma patients with hypercoagulable thromboelastography. The journal of trauma and acute care surgery. 2017 Sep:83(3):413-419. doi: 10.1097/TA.0000000000001618. Epub
[PubMed PMID: 28598908]
[55]
Parameswaran A, Krishnamoorthy VP, Oommen AT, Jasper A, Korula RJ, Nair SC, Poonnoose PM. Is pre-operative assessment of coagulation profile with Thrombelastography (TEG) useful in predicting venous thromboembolism (VTE) following orthopaedic surgery? Journal of clinical orthopaedics and trauma. 2016 Oct-Dec:7(Suppl 2):225-229. doi: 10.1016/j.jcot.2016.08.003. Epub 2016 Aug 24
[PubMed PMID: 28053389]
[56]
Van PY, Cho SD, Underwood SJ, Morris MS, Watters JM, Schreiber MA. Thrombelastography versus AntiFactor Xa levels in the assessment of prophylactic-dose enoxaparin in critically ill patients. The Journal of trauma. 2009 Jun:66(6):1509-15; discussion 1515-7. doi: 10.1097/TA.0b013e3181a51e33. Epub
[PubMed PMID: 19509608]
Level 3 (low-level) evidence
[57]
Kitchen DP, Kitchen S, Jennings I, Woods T, Walker I. Quality assurance and quality control of thrombelastography and rotational Thromboelastometry: the UK NEQAS for blood coagulation experience. Seminars in thrombosis and hemostasis. 2010 Oct:36(7):757-63. doi: 10.1055/s-0030-1265292. Epub 2010 Oct 26
[PubMed PMID: 20978996]
Level 2 (mid-level) evidence