Introduction
Tinea manuum is a superficial mycosis of the palms, dorsum, or interdigital folds of one or both hands. It is usually caused by dermatophytes, although rare cases caused by Hendersonula toruloidea and Scytalidium hyalinum have been reported in the literature.[1]
Tinea manuum frequently coexists with tinea pedis, but localized forms occasionally affect the hands exclusively. The condition is distributed worldwide, and, as with other dermatophytoses, contact with infected people, animals, and soil is the most common source.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Tinea manuum is caused by dermatophytes, the most common of which worldwide is Trichophyton rubrum. However, different etiologic organisms have been reported in various geographical locations, including:[2]
- Trichophyton mentagrophytes [3]
- Epidermophyton floccosum
- Trichophyton verrucosum
- Trichophyton interdigitale
- Microsporum canis
Microsporum gypseum, Trichophyton eriotrephon, and Arhroderma benhamiae have also been described, but more rarely.[4] Recently, tinea manuum has been found in patients due to Trichophyton erinacei.[5][6]
Risk factors and predispositions for tinea manuum infections and onychomycosis include:
- Male gender, diabetes mellitus, hypertension, atherosclerosis, immunosuppression
- Humid environment, excess sweating (hyperhidrosis) and maceration, prolonged use of occlusive footwear, and communal bathing or public sports facilities.
- Excoriation of the soles of the feet or picking toenails infected with tinea[7]
- Farmworkers and pet owners (eg, exotic pets, including guinea pigs and hedgehogs).[8][9][10]
- Recurrent trauma to the hands, usually work-related (eg, car mechanics, machine operators, individuals who work with chemicals)[11]
Epidemiology
An estimated 10% to 25% of the world’s population is infected by a dermatophyte. Tinea pedis and manuum are the most common clinical presentations of these infections, with tinea pedis occurring in up to 70% of adults.[12]
There are many epidemiological studies on tinea pedis, but little research is available on the epidemiology of tinea manuum. The rate of tinea manuum can range from 0.3% to 13%, with the variability based on geographic location.[11][13] Adolescent and adult males are the more commonly affected populations.[4]
One study of collected cases of tinea manuum showed that “the two feet, one hand syndrome” is the most frequent (65%) clinical presentation, followed by bilateral tinea pedis with bilateral tinea manuum (19.3%), unilateral tinea manuum (11.8%), and bilateral tinea manuum (3.9%).[2]
Pathophysiology
Differences in susceptibility, even when individuals have the same risk factors for fungal infection, provide evidence of the complex interaction between the host, agent, and environment. Recently, the immune-genetic predispositions for more severe, invasive diseases have been described in the literature with specific innate and adaptative immunity defects.[14] The cell-mediated immune response is currently accepted as being responsible for the infection control of dermatophytes.[15]
Acquired immunosuppression, as in HIV/AIDS, lymphoma, diabetes, older age, Cushing's syndrome, or use of chemotherapy or other immunosuppressive agents, predisposes the host to tinea infection. Web spaces, excess sweating, and maceration also create a more hospitable environment for better fungal growth.[16]
Mannan glycoproteins mediate the adherence of dermatophytes to the keratin-containing epithelial tissue of the host, and then proteases digest the keratin network to facilitate penetration. Trichophyton rubrum cell wall mannan has also been shown to suppress lymphocyte response.[17][18]
Dermatophytes invade and infect the stratum corneum and may persist there. The skin responds to superficial infection via the increased proliferation of keratinocytes and the production of scales. The epidermal hyperkeratosis clinically manifests as a thickening of the skin.
Histopathology
Histologic findings are similar for all dermatophyte infections. A skin biopsy will demonstrate epidermal spongiosis, parakeratosis, and a superficial inflammatory infiltrate. Clusters of neutrophils in the stratum corneum are considered an important clue for the diagnosis. Nonpigmented, regular, septated hyphae might be seen in the stratum corneum, but this is best identified with periodic acid-Schiff (PAS) or Gomori methamine silver (GMS) stains.[19]
History and Physical
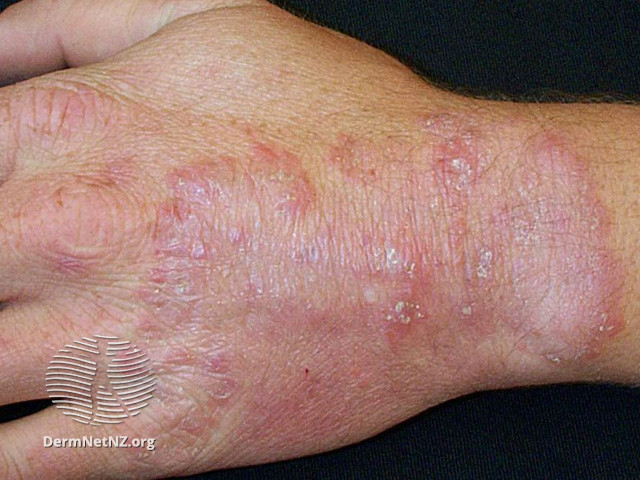
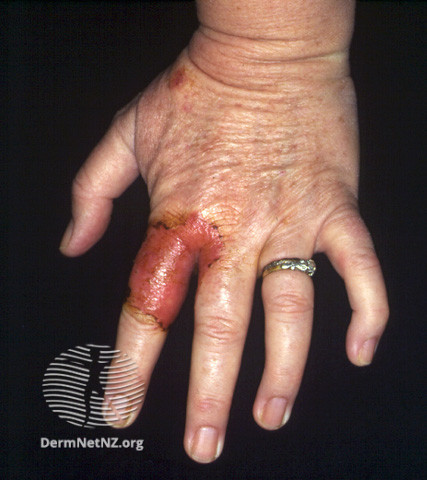
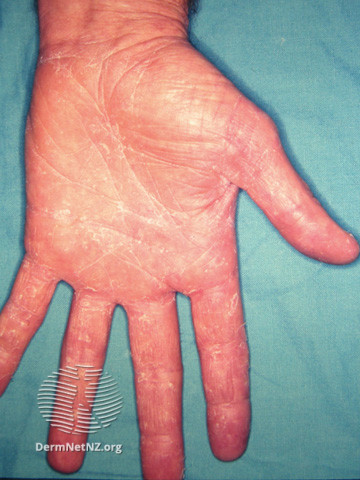
Tinea manuum might be asymptomatic, or patients can complain of thickened skin or pruritis. Infection is usually unilateral, but it can also affect both hands. The dorsum of the hand will show a similar morphology as in tinea corporis, characterized by a red plaque with an active vesicular and scaly border and centrifugal growth (see Image. Red plaque). Several concentric rings might also be seen (see Image. Concentric rings). Palmar surfaces usually have a dry, scaling appearance (see Image. Palmar surface).[20]
The most common clinical presentation is an entity known as “two-foot, one-hand syndrome. Both feet are affected in this case, and one hand presents with scaly patches or moderate to severe diffuse dryness. In some patients, onychomycosis can be present in the same hand or even in both hands.[14][21]
Zoophilic dermatophyte infections must be suspected when inflammatory lesions with pustular or vesicular plaques on a highly erythematous base are seen, especially if the lesions are localized to one hand. Patients can experience pain, itching, and swelling; rare cases might include local lymphangitis.[3][22]
Evaluation
Once a detailed medical history and clinical inspection suggest tinea manuum, mycological confirmation must be obtained. Some authors suggest that the gold standard for detecting a fungal infection must be a triple confirmation that includes a clinical exam, potassium hydroxide (KOH), and culture.[22] Other methods include:
Direct microscopy: Direct microscopy is a simple and inexpensive method to find the presence of fungal hyphae. Classically, a swab of pustular or wet inflammatory lesions or a scraping of dry, scaly lesions might be the first step. Nail clippings should be included if onychomycosis is also suspected.[20] Usually, the specimen must be treated with KOH, and the results are back within 24 hours in most laboratories. The sensitivity and specificity of KOH smears are 73.3% and 48%, respectively, so the smear should be complemented with culture. Cultures usually take 2 to 6 weeks to grow, so treatment should not be delayed while waiting for results. When available, antifungal susceptibility testing should be added to the culture to determine fungal susceptibility to terbinafine, itraconazole, and fluconazole.
Fluorescent staining: Fluorescent staining with optical brighteners might be used to increase the fungal detection rate. This stain selectively binds to chitin of the fungal cell wall and then gives an apple-green fluorescence when visualized under fluorescent microscopy.
Histopathology: Histopathology might be necessary, especially when other skin diseases are suspected in the differential diagnosis.
Dermoscopy: Dermoscopy has also been described recently as a useful and noninvasive tool that could assist in the diagnosis of tinea manuum.[23] Typical localization and distribution of the scales in the furrows and dermatoglyphics seem to be unique to this entity.[23][24]
Other methods: Other methods of dermatophyte differentiation, such as polymerase chain reaction (PCR), real-time PCR, and newer molecular methods, are being used in large institutions and for research purposes.[19]
Treatment / Management
Several topical and systemic antifungal therapy options and regimens are available. When possible, topical therapy is preferred for tinea manuum due to the risk of drug interactions and side effects of the oral treatments.
- There is no difference in cure rates among allylamines (terbinafine, naftifine), imidazoles (clotrimazole, fluconazole, itraconazole, ketoconazole), or other antifungals, such as butenafine and ciclopirox olamine.
- Regimens last 4 to 6 weeks, except for newer options like luliconazole and econazole (ecoza, spectazole), which usually require about 2 to 4 weeks of treatment.
- In addition, the anti-inflammatory effects (eg, bifonazole) and the antibacterial properties (eg, clotrimazole (gram-positive and gram-negative cocci) and isoconazole (gram-positive bacteria, including MRSA)] of several topical antifungals give specific value when choosing the agent.[19][25][26] While nystatin is effective for candida, it is not appropriate for dermatophytes; therefore, it should not be used to treat tinea manuum. (A1)
- Indications for systemic antifungals in tinea manuum include a co-infection of the nails, the involvement of two or more body areas, including the “two-foot, one-hand syndrome,” immunosuppression, recurrence of the infection, and topical therapy failure.[17] The oral options are terbinafine and itraconazole with similar rates of cure.[27][28] (A1)
- The use of corticosteroids is controversial; however, they can be beneficial in severely inflamed cases to reduce pruritus or burning sensations and, in some patients, to secure treatment adherence. When used, corticosteroid treatment should be administered simultaneously with antifungal therapy, but it should be limited to only the first week of antifungal treatment.[29]
Differential Diagnosis
The differential diagnosis for tinea manuum includes various cutaneous diseases as well as bacterial, viral, and other fungal infections.
Psoriasis: Psoriasis is usually bilateral and hyperkeratotic, with thickened palms and soles. Patches of unaffected skin are commonly seen, and vesicular lesions, ungual pitting, and oil drop signs can also be seen.
Dyshidrotic eczema: Dyshidrotic eczema is characterized by vesicles in the edges of the fingers, toes, palms, and soles that are very pruriginous and may be related to stress or seasonal allergies.
Contact dermatitis: Irritant and allergic varieties of contact dermatitis are inflammatory conditions with erythematous and pruritic skin lesions that can affect the palms and dorsum of hands, usually bilateral. Patients might notice skin lesions after contact with a foreign substance (eg, poison ivy or nickel).[12]
Dermatophyte infections: Inflammatory, bullous dermatophyte infections can be misdiagnosed as herpetic whitlow of herpes simplex infection, bacterial bullous impetigo, or cellulitis.[30][31]
Prognosis
Making the correct diagnosis and gaining compliance with an appropriate treatment regimen is critical to effecting a mycological cure. Some treatments might require several weeks, so noncompliance is a common reason for treatment failure.
Relapse or recurrence after therapy remains a concern. Infection transmission from symptom-free carriers, like family and pets, needs to be identified. Adjuvant therapies might be required to adequately control infection in the treatment-refractory patient and the carriers, and disinfectant techniques should be employed to control exposure via fomites.[16][32]
Complications
In general, most complications are due to delays in consultation and diagnosis. Medical evaluation sometimes occurs as late as months to years after the skin lesion appears.
Secondary bacterial infection and lymphangitis have been described in cases of inflammatory tinea manuum, especially in those due to a zoonotic dermatophyte.[7]
Contact dermatitis due to topical imidazole antimycotic therapy has been described as a rare complication of its use.[33] Recently, a case of disuse contractures of the flexor tendons has been reported in a patient with tinea manuum and irritant contact dermatitis.[8]
Consultations
Primary care providers will usually make the diagnosis and establish treatment; however, some cases can be challenging and might require a referral to a dermatologist or infectious disease specialist, especially in chronic or recurrent cases or for patients in whom underlying skin disease is suspected.ftinea manuum
Deterrence and Patient Education
Education of patients must focus on:
- Hygiene: Patients should be advised to wash their hands frequently to help remove pathogens on the surface of the hands.[14]
- Scratching: Patients should avoid scratching their feet or touching onychomycosis.
- Tinea pedis: Timely prevention can help prevent it from spreading from the feet to the hands.
- Possible contacts: Identify and treat possible contacts.
- Compliance: Patients should be encouraged to comply with their treatment plan and avoid self-treatment with topical corticosteroids and antibiotics. These additional and often unnecessary treatments can delay the correct diagnosis.[2]
Pearls and Other Issues
A few things that need to be considered when diagnosing and treating tinea manuum:
- When “hand eczema” is localized to one hand, consider fungal infection in the differential.
- If tinea manuum is confirmed, the feet must be examined, as the most common presentation of tinea manuum is “two feet and one hand.”
- Chronic treatment of a refractory hand dermatosis with topical corticosteroids or calcineurin inhibitors (eg, pimecrolimus [Elidel], tacrolimus [Protopic]) might impede the correct diagnosis (ie, “tinea incognito”).
- Exotic pet owners might develop inflammatory, bullous tinea manuum (usually caused by zoophilic dermatophytes) that can be misdiagnosed as bacterial or viral infections.
- Molecular biology dermatophyte diagnostics using nucleic amplification techniques have become an important part of dermatophyte infection diagnosis.
Enhancing Healthcare Team Outcomes
Early diagnosis and treatment are essential in decreasing morbidity and facilitating manual function. Primary care providers should be able to treat most cases of tinea manuum; however, if there is an uncertain diagnosis or an inadequate response to therapy, the patient should be referred to a dermatologist. A referral is also prudent if immunodeficiency is suspected or diagnosed as a predisposing factor in the development of tinea manuum.
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
References
Elewski BE, Greer DL. Hendersonula toruloidea and Scytalidium hyalinum. Review and update. Archives of dermatology. 1991 Jul:127(7):1041-4 [PubMed PMID: 2064405]
Zhan P, Geng C, Li Z, Jiang Q, Jin Y, Li C, Liu W. The epidemiology of tinea manuum in Nanchang area, South China. Mycopathologia. 2013 Aug:176(1-2):83-8. doi: 10.1007/s11046-013-9673-9. Epub 2013 Jun 14 [PubMed PMID: 23765324]
Rhee DY, Kim MS, Chang SE, Lee MW, Choi JH, Moon KC, Koh JK, Choi JS. A case of tinea manuum caused by Trichophyton mentagrophytes var. erinacei: the first isolation in Korea. Mycoses. 2009 May:52(3):287-90. doi: 10.1111/j.1439-0507.2008.01556.x. Epub 2008 Jul 11 [PubMed PMID: 18643919]
Level 3 (low-level) evidenceDaniel CR 3rd, Gupta AK, Daniel MP, Daniel CM. Two feet-one hand syndrome: a retrospective multicenter survey. International journal of dermatology. 1997 Sep:36(9):658-60 [PubMed PMID: 9352405]
Level 2 (mid-level) evidenceOgawa T, Ogawa Y, Hiruma M, Kano R, Ikeda S. Tinea manuum caused by Trichophyton erinacei. The Journal of dermatology. 2020 Sep:47(9):e344-e345. doi: 10.1111/1346-8138.15477. Epub 2020 Jun 29 [PubMed PMID: 32602141]
Watabe D, Takeda K, Amano H. Tinea manuum caused by Trichophyton erinacei from a hedgehog. European journal of dermatology : EJD. 2021 Aug 26:():. doi: 10.1684/ejd.2021.4111. Epub 2021 Aug 26 [PubMed PMID: 34463276]
Perrier P, Monod M. Tinea manuum caused by Trichophyton erinacei: first report in Switzerland. International journal of dermatology. 2015 Aug:54(8):959-60. doi: 10.1111/ijd.12291. Epub 2013 Dec 30 [PubMed PMID: 24372169]
Level 3 (low-level) evidenceVeraldi S, Schianchi R, Benzecry V, Gorani A. Tinea manuum: A report of 18 cases observed in the metropolitan area of Milan and review of the literature. Mycoses. 2019 Jul:62(7):604-608. doi: 10.1111/myc.12914. Epub 2019 Apr 24 [PubMed PMID: 30929271]
Level 3 (low-level) evidenceHarada K, Hiruma J, Maeda T, Tsuboi R. Case of tinea manuum transmitted by a hedgehog in an animal cafe. The Journal of dermatology. 2019 Oct:46(10):e344-e345. doi: 10.1111/1346-8138.14894. Epub 2019 Apr 24 [PubMed PMID: 31017686]
Level 3 (low-level) evidenceWalsh AL, Merchan N, Harper CM. Hedgehog-Transmitted Trichophyton erinaceid Causing Painful Bullous Tinea Manuum. The Journal of hand surgery. 2021 May:46(5):430.e1-430.e3. doi: 10.1016/j.jhsa.2020.06.015. Epub 2020 Aug 1 [PubMed PMID: 32753229]
Zhan P, Ge YP, Lu XL, She XD, Li ZH, Liu WD. A case-control analysis and laboratory study of the two feet-one hand syndrome in two dermatology hospitals in China. Clinical and experimental dermatology. 2010 Jul:35(5):468-72. doi: 10.1111/j.1365-2230.2009.03458.x. Epub 2009 Oct 23 [PubMed PMID: 19874338]
Level 2 (mid-level) evidenceDrake LA, Dinehart SM, Farmer ER, Goltz RW, Graham GF, Hardinsky MK, Lewis CW, Pariser DM, Skouge JW, Webster SB, Whitaker DC, Butler B, Lowery BJ, Elewski BE, Elgart ML, Jacobs PH, Lesher JL Jr, Scher RK. Guidelines of care for superficial mycotic infections of the skin: tinea corporis, tinea cruris, tinea faciei, tinea manuum, and tinea pedis. Guidelines/Outcomes Committee. American Academy of Dermatology. Journal of the American Academy of Dermatology. 1996 Feb:34(2 Pt 1):282-6 [PubMed PMID: 8642094]
Level 1 (high-level) evidenceKiraz N, Metintas S, Oz Y, Koc F, Koku Aksu EA, Kalyoncu C, Kasifoglu N, Cetin E, Arikan I. The prevalence of tinea pedis and tinea manuum in adults in rural areas in Turkey. International journal of environmental health research. 2010 Oct:20(5):379-86. doi: 10.1080/09603123.2010.484861. Epub [PubMed PMID: 20853199]
García-Romero MT, Arenas R. New insights into genes, immunity, and the occurrence of dermatophytosis. The Journal of investigative dermatology. 2015 Mar:135(3):655-657. doi: 10.1038/jid.2014.498. Epub [PubMed PMID: 25666672]
de Sousa Mda G, Santana GB, Criado PR, Benard G. Chronic widespread dermatophytosis due to Trichophyton rubrum: a syndrome associated with a Trichophyton-specific functional defect of phagocytes. Frontiers in microbiology. 2015:6():801. doi: 10.3389/fmicb.2015.00801. Epub 2015 Aug 4 [PubMed PMID: 26300867]
Nenoff P, Krüger C, Ginter-Hanselmayer G, Tietz HJ. Mycology - an update. Part 1: Dermatomycoses: causative agents, epidemiology and pathogenesis. Journal der Deutschen Dermatologischen Gesellschaft = Journal of the German Society of Dermatology : JDDG. 2014 Mar:12(3):188-209; quiz 210, 188-211; quiz 212. doi: 10.1111/ddg.12245. Epub 2014 Feb 17 [PubMed PMID: 24533779]
Sahoo AK, Mahajan R. Management of tinea corporis, tinea cruris, and tinea pedis: A comprehensive review. Indian dermatology online journal. 2016 Mar-Apr:7(2):77-86. doi: 10.4103/2229-5178.178099. Epub [PubMed PMID: 27057486]
Blake JS, Dahl MV, Herron MJ, Nelson RD. An immunoinhibitory cell wall glycoprotein (mannan) from Trichophyton rubrum. The Journal of investigative dermatology. 1991 May:96(5):657-61 [PubMed PMID: 2022872]
Nenoff P, Krüger C, Schaller J, Ginter-Hanselmayer G, Schulte-Beerbühl R, Tietz HJ. Mycology - an update part 2: dermatomycoses: clinical picture and diagnostics. Journal der Deutschen Dermatologischen Gesellschaft = Journal of the German Society of Dermatology : JDDG. 2014 Sep:12(9):749-77. doi: 10.1111/ddg.12420. Epub [PubMed PMID: 25176455]
Singri P, Brodell RT. 'Two feet-one hand' syndrome. A recurring infection with a peculiar connection. Postgraduate medicine. 1999 Aug:106(2):83-4 [PubMed PMID: 10456041]
Level 3 (low-level) evidenceAste N, Pau M, Aste N. Tinea manuum bullosa. Mycoses. 2005 Jan:48(1):80-1 [PubMed PMID: 15679673]
Level 3 (low-level) evidenceLevitt JO, Levitt BH, Akhavan A, Yanofsky H. The sensitivity and specificity of potassium hydroxide smear and fungal culture relative to clinical assessment in the evaluation of tinea pedis: a pooled analysis. Dermatology research and practice. 2010:2010():764843. doi: 10.1155/2010/764843. Epub 2010 Jun 22 [PubMed PMID: 20672004]
Jakhar D, Kaur I, Sonthalia S. Dermoscopy of Tinea Manuum. Indian dermatology online journal. 2019 Mar-Apr:10(2):210-211. doi: 10.4103/idoj.IDOJ_95_18. Epub [PubMed PMID: 30984609]
Errichetti E, Stinco G. Dermoscopy in tinea manuum. Anais brasileiros de dermatologia. 2018 Jun:93(3):447-448. doi: 10.1590/abd1806-4841.20186366. Epub [PubMed PMID: 29924225]
van Zuuren EJ, Fedorowicz Z, El-Gohary M. Evidence-based topical treatments for tinea cruris and tinea corporis: a summary of a Cochrane systematic review. The British journal of dermatology. 2015 Mar:172(3):616-41. doi: 10.1111/bjd.13441. Epub 2015 Feb 9 [PubMed PMID: 25294700]
Level 1 (high-level) evidenceRotta I, Sanchez A, Gonçalves PR, Otuki MF, Correr CJ. Efficacy and safety of topical antifungals in the treatment of dermatomycosis: a systematic review. The British journal of dermatology. 2012 May:166(5):927-33. doi: 10.1111/j.1365-2133.2012.10815.x. Epub [PubMed PMID: 22233283]
Level 1 (high-level) evidenceBell-Syer SE, Khan SM, Torgerson DJ. Oral treatments for fungal infections of the skin of the foot. The Cochrane database of systematic reviews. 2012 Oct 17:10(10):CD003584. doi: 10.1002/14651858.CD003584.pub2. Epub 2012 Oct 17 [PubMed PMID: 23076898]
Level 1 (high-level) evidenceGupta AK, Foley KA, Versteeg SG. New Antifungal Agents and New Formulations Against Dermatophytes. Mycopathologia. 2017 Feb:182(1-2):127-141. doi: 10.1007/s11046-016-0045-0. Epub 2016 Aug 8 [PubMed PMID: 27502503]
Schaller M, Friedrich M, Papini M, Pujol RM, Veraldi S. Topical antifungal-corticosteroid combination therapy for the treatment of superficial mycoses: conclusions of an expert panel meeting. Mycoses. 2016 Jun:59(6):365-73. doi: 10.1111/myc.12481. Epub 2016 Feb 24 [PubMed PMID: 26916648]
Sweeney SM, Wiss K, Mallory SB. Inflammatory tinea pedis/manuum masquerading as bacterial cellulitis. Archives of pediatrics & adolescent medicine. 2002 Nov:156(11):1149-52 [PubMed PMID: 12413346]
Sahuquillo Torralba A, Navarro Mira MÁ, Botella Estrada R. Inflammatory tinea manuum: The importance of pustules. Medicina clinica. 2017 Aug 10:149(3):e15. doi: 10.1016/j.medcli.2016.10.020. Epub 2016 Dec 1 [PubMed PMID: 27916265]
Gupta AK, Cooper EA. Update in antifungal therapy of dermatophytosis. Mycopathologia. 2008 Nov-Dec:166(5-6):353-67. doi: 10.1007/s11046-008-9109-0. Epub 2008 May 14 [PubMed PMID: 18478357]
Erdmann S, Hertl M, Merk HF. Contact dermatitis from clotrimazole with positive patch-test reactions also to croconazole and itraconazole. Contact dermatitis. 1999 Jan:40(1):47-8 [PubMed PMID: 9928806]
Level 3 (low-level) evidence