Introduction
Renal calculi are the products of crystallization of specific stone-forming components seen in about 10% of people, and 80% are calcium-based stones. The most common stone, calcium oxalate, is formed primarily due to an imbalance between calcium and oxalate levels in the body or a lack of adequate crystallization inhibitors. Hyperoxaluria is a significant contributor to nephrolithiasis, and the causes of excess urinary oxalate can be classified into primary and secondary hyperoxaluria based on etiology. Though both can present with kidney stones, they differ in the extent of disease, rapidity of onset, and local and systemic complications.[1][2]
The acute management of renal calculi has been well-studied and standardized.[3][4] It is necessary to understand when to evaluate a patient further for an underlying cause of the calculi. This evaluative process improves the patient's quality of life and prevents or delays recurrences and other complications of hyperoxaluria. In general, clinicians should offer 24-hour urine testing and preventive therapy to every nephrolithiasis patient, especially those who are strongly motivated to follow a long-term course of preventive therapy.
Even relatively small changes in urinary oxalate can have a very significant impact on kidney stone production.[5] In addition, the presence of hyperoxaluria alone, without concurrent nephrolithiasis, also has deleterious effects on the kidney, resulting in tubular toxicity, obstruction, interstitial fibrosis, and tubular atrophy. Unfortunately, an effective and specific treatment for this potential nephrotoxin is currently lacking. Therefore, clinicians caring for these patients should become familiar with the available diagnostic testing and treatments for hyperoxaluria and endpoints to measure therapy effectiveness.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Depending on etiology, hyperoxaluria can be broadly divided into primary (rare) and secondary (common).
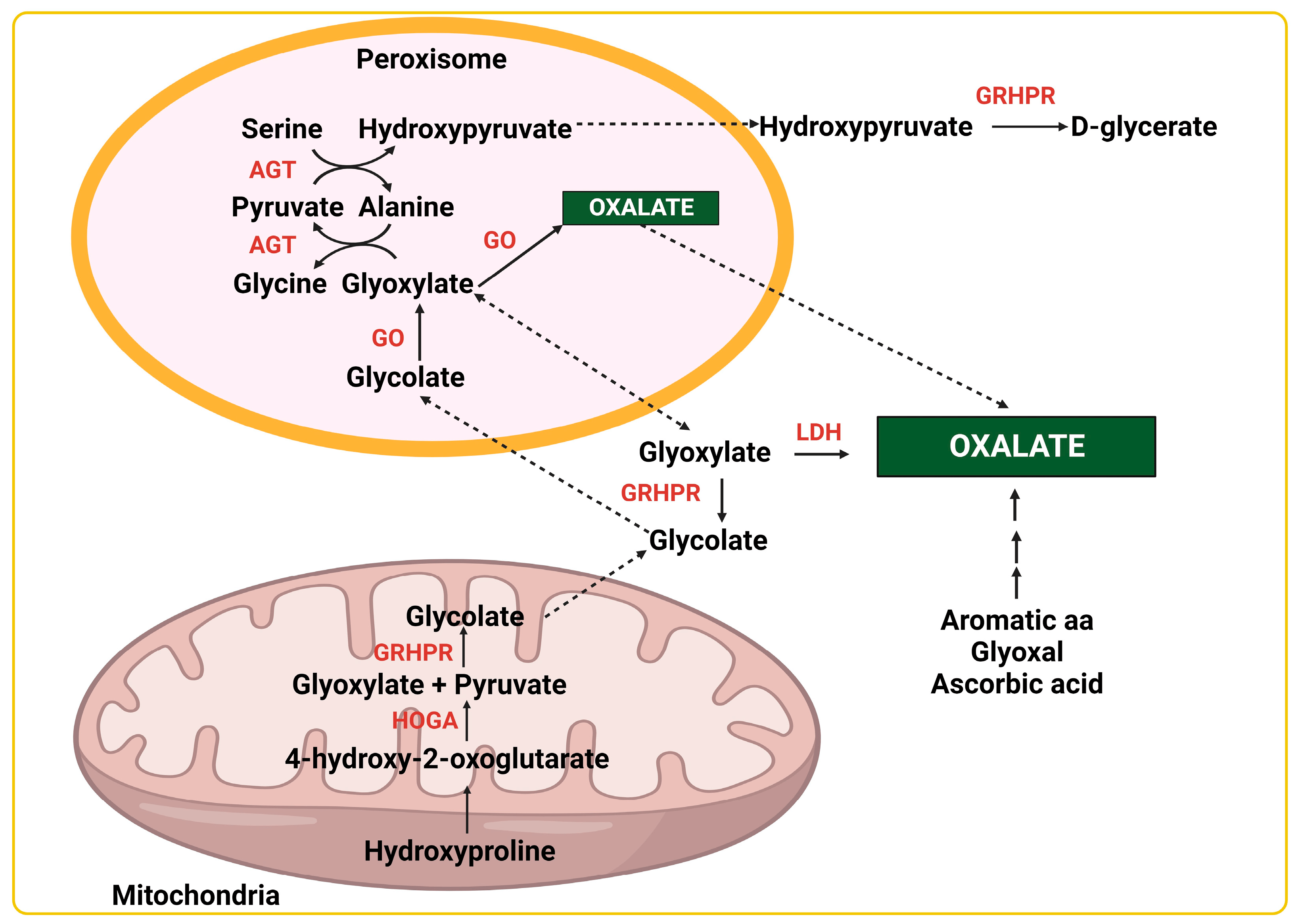
Primary Hyperoxaluria (PH) is caused by an inherent genetic defect or absence of a specific enzymatic activity, ultimately leading to significantly increased oxalate levels in the body (see Image. Pathways of Endogenous Oxalate Production). PH is inherited as an autosomal recessive trait.
Symptoms typically appear in childhood, with a median age of presentation of only 4 to 5 years old. PH often leads to multiple recurrent calcium oxalate nephrolithiasis episodes, nephrocalcinosis, and progressive renal damage, which may become end-stage renal disease (ESRD). PH type II is milder than type I, mainly due to lower urinary oxalate excretion, whereas recurrent renal stones are characteristic of PH type III.
- PH type I: Glyoxalate is produced as an intermediate molecule in hydroxyproline, glycolate, and glycine metabolism. Glyoxalate is generally catalyzed in the peroxisome of the hepatocytes by the enzyme alanine-glyoxylate-aminotransferase (AGT), which converts glyoxalate to glycine.[6] In the event of a deficiency or absence of this enzyme, glyoxalate accumulates in the cytosol, where it is converted to oxalate by lactate dehydrogenase (LDH). This vitamin B6-dependent enzyme (AGT) deficiency has been linked to the AGXT gene mutation on chromosome 2. Type I comprises 70% to 80% of all PH.[7] Between 20% and 50% of patients with this type will have advanced ESRD when diagnosed, and the median age at diagnosis is 24 years. About 80% of patients with this condition will develop ESRD by age 30.[8]
- PH type II: On chromosome 10, a specific gene codes for the enzyme glyoxalate hydroxypyruvate reductase (GRHPR), which converts glyoxalate to glycolate. A deficiency of this enzyme will lead to a buildup of glyoxalate, which LDH eventually converts to oxalate.[2][7] Presentation is milder than type I, with ESRD occurring in 20% to 25% of patients.[8]
- PH type III: This is the least common type. It is caused by a deficiency of mitochondrial enzyme 4-hydroxy 2-oxoglutarate aldolase coded by the gene HOGA1 on chromosome 9. The lack of this enzyme limits the conversion of 4-hydroxy 2-oxoglutarate into glyoxalate. This limitation will divert more of the oxoglutarate toward the oxalate-producing pathway.[2][7] Clinical presentations are less severe than types I and II; nephrolithiasis is the primary symptom.[8]
Secondary Hyperoxaluria mainly pertains to excess exogenous oxalate gained either through diet or due to intestinal pathologies. The overwhelming majority of hyperoxaluric patients will have the secondary type of the disorder. The causes of secondary hyperoxaluria include the following:
Dietary etiology
- Dietary sources include foods rich in oxalates, such as spinach, rhubarb, collard greens, nuts, beets, and tea. High dietary oxalate has been thought to play a relatively small (10% to 20%) contributory role in hyperoxaluria.[5][9]
- The 24-hour urinary oxalate increases by 1.7 mg for every 100 mg of dietary oxalate ingested.[10] This increase can be clinically significant as it has been shown that changes in 24-hour urinary oxalate excretion as small as 4 mg can increase the risk of nephrolithiasis by 60% to as much as 100%.[5]
- Increased vitamin C is a risk factor for hyperoxaluria, as vitamin C is a potential precursor to oxalate. Amounts exceeding 1000 mg of vitamin C daily are considered a possible risk factor.[7]
- Cranberry juice and concentrates are not recommended in patients with calcium oxalate stones or patients with hyperoxaluria due to their relatively high oxalate content.[11]
- Dietary calcium combines with oxalate in the intestine, which protects against excessive oxalate absorption and hyperoxaluria. Therefore, decreased calcium in the diet becomes a risk factor for hyperoxaluria.[12]
Enteric etiology
- Enteric hyperoxaluria: Free intestinal calcium will tightly bind to free oxalate, creating an insoluble molecule of calcium oxalate. This process lowers free intestinal oxalate levels and prevents excessive oxalate absorption, which the kidney would otherwise excrete. However, intestinal pathologies leading to fat malabsorption, such as bariatric surgery, cause a buildup of unabsorbed fatty acids and bile salts in the intestinal lumen that bind to the ingested dietary calcium, resulting in inadequate intestinal oxalate binding and subsequent increased oxalate absorption.
- As the malabsorption continues further in the intestinal lumen, the colon's permeability to oxalate increases, aggravating the problem. The soluble oxalate, which did not combine with calcium, diffuses passively into the blood and is eventually filtered by the kidneys, resulting in severe hyperoxaluria. In addition, vitamin B6 deficiency often ensues in these conditions, further increasing endogenous oxalate production through decreased AGT activity.[2][13]
- While usually associated with gastrointestinal bypass surgery, enteric hyperoxaluria can be found in any condition that results in chronic diarrhea, such as chronic biliary disease, various pancreatic disorders, short bowel syndrome, fat malabsorption, and irritable bowel syndrome.
Oxalobacter formigenes
- Oxalobacter formigenes are gram-negative, facultative anaerobic, oxalate-degrading bacteria normally colonizing the colon by age 3. Antibiotic use, inflammatory bowel disease, or dietary changes may disrupt the Oxalobacter colonies with subsequent increased intestinal oxalate presence.[2][13] Patients who have lost their natural Oxalobacter colonization have been found to have a 40% increase in average urinary oxalate levels compared to calcium oxalate stone formers with normal intestinal Oxalobacter.[14][15] Unfortunately, restoring natural intestinal Oxalobacter colonies is extremely difficult once they are lost. Oxalobacter formigines are relatively resistant to sulfa and penicillin antibiotics but very sensitive to tetracyclines, macrolides, and fluoroquinolones.
- Female patients who form kidney stones and have recurrent urinary tract infections have significantly higher average urinary oxalate levels than similar female patients who do not have a history of multiple infections. This difference is most likely due to the loss of intestinal Oxalobacter from the multiple courses of antibiotics used to treat frequent urinary infections.[16] A similar process is likely in patients with cystic fibrosis, who also tend to use antibiotics frequently. Urinary oxalate levels were normal in a study of patients with cystic fibrosis and those with viable intestinal Oxalobacter colonies. In contrast, more than 50% of similar patients with cystic fibrosis who had lost their Oxalobacter strains were found to be hyperoxaluric.[17]
Other causes
- Pancreatic insufficiency in patients with acute or chronic pancreatitis causes saponification due to calcium binding to unabsorbed fatty acids, leaving an excess of intestinal oxalate to be absorbed, then filtered by the kidneys and excreted in the urine.[18][19]
- Ethylene glycol, found in antifreeze, is commonly ingested accidentally or intentionally. In 2020, US poison control centers noted 6036 calls regarding ethylene glycol ingestion. Of these, 586 had at least moderate clinical effects, 30 of which resulted in death. Ethylene glycol is metabolized through alcohol dehydrogenase; an end product is oxalate. Oxalate crystals are often found in the urine of patients with ethylene glycol ingestion.[20]
- Recently, a case series from Israel found 26 patients from 2019 to 2022 who experienced acute kidney injury (AKI) after keratin hair-straightening treatments containing glycolic acid. Of the 7 kidney biopsies performed, 6 demonstrated calcium oxalate crystals, and 1 showed intratubular calcification. The glycolic acid was thought to be absorbed topically, resulting in hyperoxaluria.[21] Other case reports have shown similar presentations, and this rare diagnosis should be considered in otherwise healthy patients presenting with AKI after hair treatments.[22]
Epidemiology
The lifetime risk of nephrolithiasis in the developed world is about 10% to 15%. Men have an increased incidence compared to women. In the United States, the prevalence is about 10% in men and 7% in women, with a 10-year recurrence rate of 50%. Whites have higher rates of nephrolithiasis and hyperoxaluria than Blacks.[23]
Calcium stones comprise about 80% of all kidney stone diseases, with calcium oxalate predominating at approximately 75%.[24][25] The risk of recurrence with calcium stones is about 60% in 10 years without appropriate preventive measures.[24]
The estimated overall incidence of secondary hyperoxaluria appears to be increasing over time. Typical rates of hyperoxaluria range from 25% to 45% in all recurrent calcium stone-formers.[26] They are also higher in non-American populations; Asian countries typically have higher rates of hyperoxaluria than Western countries.[26] The reasons for this are unclear but likely due to cultural, genetic, and dietary issues. This significantly increased incidence of hyperoxaluria is also considered a significant contributing factor to the observed rise in global nephrolithiasis rates. Further studies are needed to confirm this finding.[26]
There does appear to be a protective effect from female sex hormones on oxalate excretion, while testosterone has a detrimental effect. The exact reason for this is unclear and will require more studies to elucidate.[27]
Greater body weight appears to increase urinary oxalate, but there are conflicting data on whether this is relatively proportionate between the sexes.[27][28] However, obesity is associated with higher urinary oxalate levels in both men and women. Among stone formers, patients with obesity are found to have oxalate levels about 33% higher than stone-forming patients who are not obese.[27]
Urinary oxalate excretion is higher in Whites after a controlled, high-oxalate meal than in Blacks. The reason for this is unclear but is thought to be due to genetic factors, with Whites having a higher rate of intestinal oxalate absorption than Blacks.[29][30] There does not appear to be an age-related factor concerning oxalate absorption.[31]
PH is quite rare. While usually diagnosed in the pediatric age group, it is often diagnosed very late into the course of the disease, usually only after the development of nephrocalcinosis or ESRD. PH type I is the most common and severe form of this rare disorder, accounting for 80% of those diagnosed with the condition.[32]
The prevalence of the disease ranges from 1 to 3 per 1 million population in the US, with an approximate incidence rate of approximately 1 in 100,000 live births per year in Europe and 1 in 58,000 population worldwide.[33][34] Higher rates are reported from inbred populations and in developing countries.[35] PH accounts for less than 1% of the pediatric ESRD population in USA, UK, and Japan registries.[33]
Pathophysiology
Oxalate is an organic acid produced by plants. It is primarily found in the leaves, fruits, nuts, and bark, typically in portions of the plant that can be shed. Its only function is the binding of circulating calcium initially absorbed by the plant through the root system. Therefore, a plant's oxalate load will depend not only on the type of vegetation but also on the calcium content of the groundwater in the field in which it is grown. This accounts for the large variation in oxalate levels even from the same plant variety.
Unfortunately, oxalate is typically found in portions of plants that humans often consume, particularly in green leafy vegetables like spinach. Animal food sources eaten by humans have virtually no oxalate content. Oxalate was first discovered in sheep who became sick and even died when eating in certain fields, which were later determined to have vegetation with very high oxalate levels, which the sheep were eating.
In humans, oxalate has no known beneficial or nutritional effect. It is absorbed primarily in the colon, passed through the liver, and is excreted in the proximal renal tubule. Oxalate is also generated by glycolate metabolism in the liver or converted from excess vitamin C. In the urine, oxalate forms a strong bond with calcium, forming crystals and eventually stones depending on the pH, specific gravity, concentration, and the presence or absence of various regulators of stone formation. Urinary oxalate is the single, strongest chemical promotor of kidney stones known. It is typically 15 to 20 times stronger than urinary calcium in promoting the formation of calcium oxalate kidney stones.
The solubility of oxalate at body temperature at a pH of 7 is only about 5 mg/L, so urine is usually supersaturated with oxalate in most people. It does not form stones in everyone due to the activity of urinary stone inhibitors like citrate. Oxalate forms a soluble complex with sodium and potassium; it is only when combined with calcium that it forms insoluble crystals of calcium oxalate. Calcium oxalate tends to form at a relatively low urinary pH (<7.2), while calcium phosphate will form when the urine is more alkaline (>7.2). Among urinary chemicals, oxalate is the single strongest promotor of renal calculi. Kidney stone risk increases 2.5 to 3.5 times when the urinary oxalate level increases from 20 to 40 mg daily.
From the point of view of crystallization science, stone formation results from a combination of abnormal factors that influence the chemistry, supersaturation, and rate-controlling processes involved in forming crystals of the various kidney stone-forming minerals. The principal thermodynamic driving force is the degree of supersaturation of the fluid in which this process occurs. The laws of crystallization hold for both intracellular and extracellular crystal formation. The following steps lead to the formation of calcium oxalate stones: [36]
-
Nucleation: This is the first step leading to crystallization and can occur either homogeneously or heterogeneously. Homogeneous crystal nucleation requires a greater degree of calcium oxalate supersaturation compared to heterogeneous nucleation. By contrast, heterogeneous nucleation requires lesser amounts of precipitating salts due to the presence of proteins and other organic polymers that provide chemically active surfaces that facilitate the nucleation process. Heterogeneous nucleation is the more common mechanism of human calcium oxalate crystal formation in humans.
-
Supersaturation: A relative supersaturation level measures the potential for a crystal to form in the urine. It varies with each solute, solution pH, and the balance between chemical crystal promotors and inhibitors. The level at which nucleation occurs is referred to as the formation product of the mineral concerned. This provides a range of supersaturation values to facilitate de novo crystal nucleation.
-
Crystal growth and agglomeration: Once a crystal is established, the surrounding urine facilitates the growth of this crystal. These growing crystals stagnate at sites where the urinary flow is relatively sluggish, either due to narrowing of the tubule as in the proximal tubule, when it meets the loop of Henle, at the papillary base where renal tubules bend, or at the slit-like openings of the collecting duct that structurally favor plugging. When these contact the surrounding epithelial cells, they grow into macromolecules. These travel along the length of the tubules while continuously accumulating crystals on the way.
-
Rate of crystal growth: This is determined by the relative supersaturation level as well as accompanying components that promote or decrease crystallization like magnesium, citrate, pyrophosphate, matrix substance A, various uncharacterized urinary proteins, glycoproteins, glycosaminoglycans and the polymerized form of Tamm–Horsfall protein, amongst others.
The crystallization and deposition of calcium oxalate within the renal parenchymal tissues is known as nephrocalcinosis. Together, these 2 processes of nephrocalcinosis and calcium oxalate stone formation will cause inflammation and progressive renal injury that eventually can lead to a decline in renal function and, ultimately, ESRD.[37] A glomerular filtration rate (GFR) <30 to 50 mL/min per 1.73 m² will exacerbate this condition by further decreasing urinary oxalate excretion while increasing its buildup in the plasma, leading to possible calcium oxalate deposition within secondary tissues and organs. This threshold level is known as the supersaturation point of calcium oxalate. When this level is exceeded, tissue crystallization and calcium oxalate crystal deposition will begin.[33]
Oxalate alone can also crystallize in the kidney, leading to obstruction, interstitial fibrosis, tubular toxicity, and atrophy. Nod-like protein receptor 3 (NLPR3), inflammasome activation, and macrophage infiltration are likely involved in oxalate crystal adhesion and aggregation, leading to intrarenal inflammation and renal fibrosis.[7] The Chronic Renal Insufficiency Cohort (CRIC) study was a large, multicenter prospective study that found that higher 24-hour urine oxalate excretion was likely independently associated with increased chronic kidney disease (CKD) and ESRD.[38] It is possible that elevated plasma oxalate levels from decreased GFR further hasten the progression of CKD to ESRD.[39] Oxalate nephropathy has a poor prognosis, with 40% to 50% of cases resulting in ESRD.[7] In animal models, elevated plasma oxalate levels are strongly associated with cardiac fibrosis and arterial hypertension, which may indicate similar pathology in humans.[39]
Histopathology
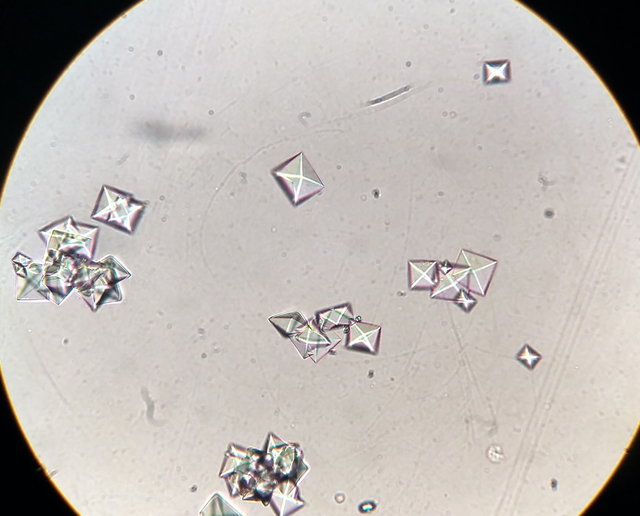
The gross appearance is unique to each type of stone. An oxalate stone reveals a nodular surface of the stone on gross examination. Calcium oxalate monohydrate is usually dark brown and extremely hard. Calcium oxalate dihydrate is lighter in color, much more fragile, and may show facets. On dissection, most calcium oxalate stones reveal concentric laminations and radial striations.[36]
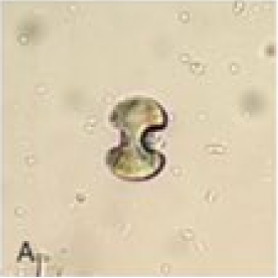
Microscopy shows significant calcium oxalate crystals (see Image. Microscopic View of Calcium Oxalate Crystals in Urine). Calcium dihydrate crystals are often described as "envelope-shaped" or "pyramidal." Calcium monohydrate crystals are described as "dumb-bell" or oval-shaped (see Image. Calcium Oxalate Monohydrated Crystals). Calcium oxalate crystals are rarely found in healthy kidneys, and 1 suggested criterion is that the oxalate crystal-to-glomeruli ratio should be >0.25 to diagnose oxalate nephropathy. Other histologic findings are acute interstitial nephritis and acute tubular necrosis, with variable interstitial fibrosis and tubular atrophy.[6][7]
History and Physical
The clinical presentation of both primary and secondary hyperoxaluria can be seen in several age groups and is preferably reviewed as renal and systemic manifestations. Patients with secondary hyperoxaluria have a lower propensity for systemic manifestations.
Renal: The renal manifestations can be seen mainly due to the increased urinary oxalate excretion and its combination with calcium, leading to calcium oxalate nephrolithiasis. A typical patient will present to the emergency department with symptoms of renal colic, including severe, acute abdominal, or flank pain radiating to the groin, often associated with nausea and vomiting. Urinary difficulties and hematuria commonly accompany this presentation. Unlike those with an acute abdomen, kidney stone patients are constantly moving, trying to find a more comfortable position, helping to make the initial diagnosis relatively easy.
Systemic: The secondary deposition of calcium oxalate, more commonly associated with PH or severe enteric hyperoxaluria, gives rise to various systemic manifestations. Based on the organ affected, these include the following:
- Heart: Conduction defects, heart blocks, and cardiomyopathy
- Hematology: Anemia due to oxalate deposition in the bone marrow that is unresponsive to erythropoietin-stimulating agents (ESA)
- Nervous system: Peripheral neuropathy, retinopathy, and cerebral infarcts
- Musculoskeletal: Bone pain, pathological fractures, and joint involvement like synovitis and chondrocalcinosis. Calcium oxalate crystal formation within tissues can be highly inflammatory, painful, and irritating.
- Vascular: Nonhealing ulcers and gangrene due to ischemia of blood vessels. There have also been reports of refractory hypotension.[33][40][41]
Evaluation
A patient presenting with acute renal colic symptoms should be investigated with a urinalysis and a noncontrast CT scan of the abdomen and pelvis. A KUB and renal ultrasound can be an alternative, but the noncontrast CT scan is the gold standard for evaluating flank pain, especially if associated with hematuria. A KUB is recommended immediately after the CT scan if any significant stones are found to aid in tracking the progress of the stone and to determine its radiopacity. Calcium oxalate stones are likely to be visible on the KUB if large enough, usually ≥2 to 3 mm. The evaluation of any underlying hyperoxaluria will be considered separately.
A chemical analysis of all urinary calculi should be done whenever possible, and their composition should be studied to determine the possible etiology. Calcium oxalate monohydrate (whewellite) and calcium oxalate dihydrate (weddellite) assume dumbbell and pyramid crystalline forms in the urine, respectively. This may sometimes help determine the underlying cause, as pure calcium oxalate monohydrate is typically seen in PH. In contrast, both pure and mixed calcium oxalate stones (monohydrate and dihydrate) are seen in secondary hyperoxaluria.[2][33][37]
Any patient suspected of hyperoxaluria should be tested for urinary oxalate excretion by collecting a 24-hour urine sample. This should preferably not be done in the hospital but rather by the patient at home while on their regular diet and usual activities. The testing is best done in a lab that conducts large numbers of urinary chemistries. Oxalate levels are typically performed in combination with other urinary chemistries to evaluate kidney stones. The other chemistries tested are typically urinary volume, pH, calcium, citrate, creatinine, magnesium, phosphate, uric acid, sodium, serum calcium, oxalate, and uric acid levels.[42] Serum oxalate levels are generally regulated in the narrow range of 1 to 3 μmol/L; however, levels can increase up to 45 μmol/L in patients with ESRD on hemodialysis and even higher than 100 μmol/L in PH.[39]
For most practical purposes, a normal 24-hour urinary oxalate level in adults would be ≤40 mg with an "optimal" level ≤25 mg. Urinary oxalate concentration should optimally be ≤20 mg oxalate/1000 mL urine.[43] Mild or moderate hyperoxaluria (usually 40 to 60 mg/day) is considered dietary hyperoxaluria. A urine oxalate to creatinine ratio is also widely utilized, although the age-specific normal limits should be used for comparison. Repeat 24-hour urine testing is recommended every 3 months until optimal levels are obtained and at least yearly thereafter.[2][33][44]
Correcting the 24-hour urine oxalate level for the patient's body surface area is somewhat controversial. The corrected value is not typically given in 24-hour urine laboratory reports; it is just the normal reference range. If using the body surface area, the urine oxalate excretion is <0.45 mmol/1.73 m² per 24 hours. Urinary oxalate excretion >1.0 mmol/1.73 m² per 24 hours is typically seen in PH or enteric hyperoxaluria. Some experts argue that the surface area correction is relatively meaningless as the crystals and stones will form based solely on the relative supersaturation level, which is not dependent on body surface area measurements.
The diagnosis of PH is rare and unusual. More often than not, it becomes apparent only after the development of ESRD and dialysis.[2][45] Patients with PH will have a 24-hour urinary oxalate level >75 mg, and many will exceed 100 mg or more per day. Some circumstances that could prompt an investigation for this condition are the following:
- An episode of renal calculi in a child, especially if younger than 5 years
- Recurring episodes of calcium oxalate renal calculi in adults
- Hyperoxaluria >100 mg/24 hours, although these high levels can also present in enteric hyperoxaluria. In enteric hyperoxaluria, calcium excretion is usually <100 mg/day, the patient often has chronic diarrhea, and there is generally severe hypocitraturia. Patients who have undergone gastric bypass surgery, such as a Roux-en-Y procedure, are far more likely to have enteric hyperoxaluria rather than PH as the cause of their calcium oxalate stone disease.
- Any patient diagnosed with calcium oxalate nephrocalcinosis, which is the deposition of calcium oxalate within the renal tissue. If a decrease in GFR accompanies this nephrocalcinosis, it is even more suggestive of PH. Nephrocalcinosis may also be caused by calcium phosphate deposition from renal tubular acidosis.
- A patient diagnosed with renal failure but without a clear underlying cause or a history of renal calculi
- If the renal stones sampled from the patient are indicative of PH type I, which are calcium oxalate monohydrate (whewellite) calculi.[46]
To differentiate between type I and II biochemically, glycolate and glycerate levels are useful if elevated. Raised urinary glycolate level is seen in PH type I and glycerate in type II.[2][37][33] For type III, an increased urinary level of 4-hydroxyoxoglutarate (HOG) and dihydroxyglutarate (DHG) suggest the diagnosis.[45]
Confirmatory tests include direct genetic testing or measuring the AGT enzyme activity following a liver biopsy. A noninvasive definitive diagnosis of PH is provided by testing for AGXT, GRHPR, and HOGA1 genes.[2]
The American Urological Association (AUA) Guidelines recommend genetic testing for PH if urinary oxalate is >75 mg/day (or >0.85 mmol/24h/1.73 m²).[47] It should also be considered in children with significant hyperoxaluria, recurrent oxalate nephrolithiasis, or nephrocalcinosis.
Genetic Screening for Nephrolithiasis and Primary Hyperoxaluria
In the United States, free genetic screening panels for nephrolithiasis are available for patients. Primary care doctors, nephrologists, and urologists can make referrals for these screening panels online (1 such company is Inivitae).
Treatment / Management
Treatment of a patient with hyperoxaluria includes conservative medical and surgical measures, along with the treatment of nephrolithiasis. Isolated renal stone treatment can be conservative, using fluids and alpha-blockers, or surgical if the stone or stones are larger than 4 mm, fail to pass, or become complicated by infection.
Fluid Intake: A greater fluid intake will increase urine volume and reduce the supersaturation of calcium oxalate. Measuring and focusing on urinary volume rather than any particular oral intake goal is preferable. It is recommended that the oral intake should be sufficient to generate at least 3000 ml of urine per day.[41][43][48] Recommendations are that patients measure their 24-hour urinary volume at home once a month until it is consistently >3 L/day.[8](B3)
Urinary Citrate and Alkalinization: Potassium citrate provides adequate urinary citrate levels and keeps the urine pH at a favorable 6.2 to 6.8. Sodium citrate can be used in cases of renal failure. Adequate urinary citrate levels (optimally at 250 to 300 mg/L or 500 to 600 mg daily total in divided doses) help prevent the aggregation of calcium oxalate crystals into stones. Potassium citrate supplements are often given along with thiazide diuretics, which decrease citrate levels when treating hypercalciuria.[2][33][49] The use of oral orthophosphates together with pyridoxine (vitamin B6) has also been proven to help reduce the formation of calcium oxalate stones.[50](B3)
Dietary Measures: Dietary modifications in secondary hyperoxaluria are useful and easily applied. Although randomized controlled trials have proven that restricting dietary calcium is detrimental, the beneficial effect of calcium supplementation in protecting against oxalate stones is less clear.[41][48] A reasonable calcium diet should be used with calcium citrate supplementation during the higher oxalate-containing meals. Iron can be substituted for calcium as a binding agent for oxalate, but calcium is more effective. Any excessive intake of vitamin C should be limited.[41][51] Oxalate-rich foods like tea, dark-leafy vegetables, spinach, kale, rhubarb, nuts, cranberries, beets, and chocolates should be limited.[48][52] (B3)
Pyridoxine: Pyridoxine (vitamin B6) should be supplemented to help patients reduce their hyperoxaluria, sometimes significantly. This has been studied extensively in type I PH. Activated vitamin B6—pyridoxal 5’-phosphate—is a cofactor for alanine-glyoxylate aminotransferase (AGT) and is thought to increase the stability and effectiveness of the AGT enzyme. Effectiveness depends on the genetic variant in AGT. Variants altering the active site binding to activated vitamin B6 and those with certain missense mutations are more responsive to this supplementation. About 30% of patients with type 1 PH are vitamin B6 responsive.[53] The dosage is 5 to 20 mg/kg per day, to a maximum of 500 mg/day, in divided doses aiming to decrease Uox by at least 30%. Type II and type III PH patients will not benefit from this therapy as their defective enzymes do not include pyridoxine as a cofactor.[54](B3)
Oxalobacter Treatments: Oxalobacter formigenes, although involved in the pathogenesis of hyperoxaluria when deficient, confer only limited benefit when given as an oral supplement. Research is ongoing to help restore it effectively to the GI tract in hyperoxaluric patients.[44][55] Several controlled trials showed oral Oxalobacter therapy could reestablish intestinal colonies in PH patients. Still, all of the trials failed to demonstrate any significant reduction in plasma or urinary oxalate compared to placebo.[55][56][57] The lack of a successful clinical effect is thought to be due to the viability of the bacteria in vivo and the possibility of insufficient treatment time. In June 2020, a lyophilized O. formigenes formulation called Oxabact was granted the Food and Drug Administration (FDA) Rare Pediatric Disease Designation and has been used successfully in case reports.[8] Different formulations of oxalate decarboxylase, which converts oxalate to formic acid and carbon dioxide, have also been studied. Usually, the enzyme is derived from fungi or bacteria. Currently, this treatment has only been tested on healthy volunteers or patients with secondary hyperoxaluria. However, results showed significant oxalate lowering in these populations.[8][58](A1)
Anti-Inflammatory Agents: NLRP3 is 1 of 3 cytosolic proteins activated by oxalate crystals, resulting in IL-1 release and causing inflammatory tubular epithelial injury. Novel inhibitors of NLRP3 and IL-1 are promising therapeutics that may be useful in the future for hyperoxaluria (both primary and secondary), as well as for CKD in general. Some of these agents are canakinumab, rilonacept, and anakinra, which are all FDA-approved for other inflammatory conditions. Canakinumab is used in anti-inflammatory diseases, like familial Mediterranean fever; rilonacept for pericarditis; anakinra is approved for inflammatory conditions, like rheumatoid arthritis.[7]
Other Therapies: Orthophosphates and pyridoxine have been successfully used to treat primary and secondary hyperoxaluria.[50] The phosphate supplement increases urinary pyrophosphate, which binds urinary calcium, while the pyridoxine helps reduce hyperoxaluria. Orthophosphates should not be used in patients with significant renal failure.[8] (B3)
Magnesium supplements (usually magnesium oxide or magnesium hydroxide) reduce oxalate absorption by binding with oxalate in the intestinal tract but may promote diarrhea when used alone.[50] As with phosphate, it works well with pyridoxine and can be used with orthophosphates. The selection of which supplement to use (orthophosphates, magnesium, or both) should be based on urinary chemistry levels of phosphate, magnesium, and renal function values. Magnesium supplementation alone may cause diarrhea. Neither orthophosphate nor magnesium supplementation will decrease endogenous oxalate production.
Cholestyramine is primarily used to manage bile acid malabsorption, increasing intestinal oxalate binding and reducing absorption. Cholestyramine will also bind intestinal oxalate directly and help reduce diarrhea, which is particularly useful in enteric hyperoxaluria. However, it can also cause constipation. In large doses, it releases chloride, which can potentially cause hyperchloremic acidosis. Cholestyramine will interfere with the absorption of many other medications and vitamins, especially thiazide diuretics, vitamin A, folic acid, and vitamin D. Lanthanum is a phosphate binder that also can bind oxalate and has been shown to lower oxalate in case reports.[53](B3)
Pentosan polysulfate (Elmiron), a synthetic glycosaminoglycan, can reduce calcium oxalate nephrolithiasis primarily by inhibiting crystal aggregation. It also appears to help lower intestinal oxalate transport and reduce urinary oxalate excretion.[59][60][61][62][63](B2)
Summary of Treatments for Secondary Hyperoxaluria
- Low fat, low oxalate diet. Avoid excessive meat intake, spinach, cranberries, kale, rhubarb, and collard greens, as these have the highest oxalate content (although the role of dietary contribution is thought to be minimal).
- Limit excess vitamin C and vitamin D
- Pyridoxine (vitamin B6) supplementation
- Normal/high calcium diet to increase intestinal oxalate binding
- Calcium citrate supplements (or iron as an alternative) with higher oxalate meals (usually lunch and dinner). One may use calcium/magnesium citrate if calcium alone is too constipating. (The optimal calcium: magnesium ratio is 2:1.)
- Potassium citrate supplementation to optimize urinary pH and 24-hour urine citrate levels. Liquid preparations are preferred in patients with bowel problems or chronic diarrhea. Low potassium, liquid citrate supplements are commercially available.
- Urinary volume optimization: Enough fluid intake to produce a minimum of 3 L daily is recommended.
- Cholestyramine will help with bile malabsorption, increase intestinal oxalate binding, and reduce diarrhea.
- Pentosan polysulfate can help lower urinary oxalate excretion, but its main benefit is reducing calcium oxalate crystal aggregation. Its use is limited now due to the risk of permanent retinal damage with prolonged administration.[64]
- Anti-diarrheal therapy should be used if there is chronic diarrhea.
- Orthophosphate or magnesium supplementation. Do not use orthophosphates in patients with significant renal failure.
- Recheck 24-hour urine testing every 3 months until optimal results are obtained, then yearly.
- In cases of severe hyperoxaluria and all children with hyperoxaluria, consider screening for primary and enteric hyperoxaluria as appropriate.
- Optimize all other urinary chemical components (calcium, citrate, uric acid) that may promote renal stone formation.
Enteric hyperoxaluria patients are also advised to consume a low-fat diet, calcium and citrate supplements, and a restriction of oxalate-rich foods.[13] Calcium citrate supplements are the primary medical treatment for enteric hyperoxaluria and can be very helpful when taken with high oxalate meals.[65] For this purpose, calcium citrate with or without magnesium is recommended. Magnesium helps avoid the constipation sometimes associated with calcium supplements. Extra vitamin D should also be avoided. The extra calcium should remain longer in the intestinal tract. Iron can be used as an alternative or supplemental oxalate binding agent, but it is less effective than calcium. Aluminum may also be used for oxalate binding, but the risk of aluminum toxicity limits its use.(B3)
Higher dietary salt causes increased urinary sodium levels that exacerbate hypercalciuria and cause an increased propensity to form calcium oxalate stones. Limiting sodium intake has been proven to help prevent recurrences of renal stones.[48][66] Excess meat protein in the diet also increases urinary calcium and uric acid excretion; therefore, it should be somewhat limited in patients with a history of renal calcium stones.[48][67][68] Potassium citrate supplements will help correct hypocitraturia. Liquid supplements are preferred due to the short transit times. Cholestyramine helps control bile acid malabsorption, improves intestinal oxalate binding directly and indirectly, and reduces diarrhea, which can be associated with enteric hyperoxaluria.[69] Finally, all other kidney stone chemical factors should be optimized as much as possible.[67] As a last resort, the GI bypass surgery can be reversed. (B2)
Treatments for Primary Hyperoxaluria
Dietary measures do not play a major role in PH as the excess oxalate in this condition is endogenous. Early, aggressive treatment is necessary to prevent loss of renal function, so utilization of all of the above measures is reasonable, including high dose pyridoxine, orthophosphate and magnesium supplementation, increased urinary volume, pentosan polysulfate (Elmiron), Lumasiran, and intensive dialysis. Liver-kidney transplants are a last-resort therapy when all other measures are insufficient.
Lumasiran and Nedosiran: In November 2020, the FDA and the European Medicines Agency approved using lumasiran for type I PH. It is the first available, effective therapy for PH short of combined liver/kidney transplantation. Lumasiran arose from a new type of therapy called small interfering RNA (siRNA) that targets specific enzymes. In this case, the targeted enzyme is the mRNA for the hepatic hydroxamic oxidase 1 gene (HOA1), which encodes glycolate oxidase. Blocking glycolate oxidase, which is chemically upstream from AGT where the genetic defect that causes PH type I is located, effectively lowers oxalate production in these individuals. Studies in adults and children have shown dramatic results, with an average 65% reduction in oxalate production and 52% of patients returning to normal oxalate levels, which were maintained for at least 6 months.[70][71][72] However, it does nothing for other types of primary or secondary hyperoxaluria. The medication is administered by a subcutaneous injection every 3 months after an initial induction phase of 4 monthly injections. It is approved for adults and children in the US and the European Union.
Nedosiran, like lumasiran, is also an RNA interference therapy designed to target hepatic lactate dehydrogenase (LDH), which converts glyoxalate to oxalate.[73] This should theoretically be effective in all 3 types of PH.[73] Experimentally, it has demonstrated dramatically lower plasma and urinary oxalate levels in type I PH. While not yet FDA-approved, a compassionate use exception was made in the case of a 17-year-old PH type I patient (originally diagnosed at age 5) who was already on aggressive, daily dialysis awaiting a combined liver-kidney transplant. The nedosiran treatment was well-tolerated and effectively decreased her serum oxalate level by about 75% despite a significant decrease in dialysis treatments from daily to the standard 3 times a week. This result has been sustained for 6 months. This success may allow the patient to avoid a liver transplant, although she will still need a new kidney. Nedosiran appears to be the first effective oxalate-lowering therapy for PH type I patients who have ESRD.[74][75] In a study with 35 PH patients (29 type I and 6 type II patients), nedosiran successfully lowered urinary oxalate significantly to normal or near-normal levels in most of these patients, with minimal adverse effects.[75](A1)
Steripentol: Steripentol is a drug initially used as an anti-epileptogenic, which was found to inhibit the activity of LDH significantly. LDH catalyzes the conversion of glyoxalate to oxalate in hepatocytes and should theoretically improve all 3 types of PH. Results of recent clinical trials are pending.[8] (B3)
Dialysis: The role of dialysis is controversial. Serum oxalate levels of 30 to 45 μmol/L lead to tissue deposition, and dialysis aims to keep the oxalate level below that to prevent supersaturation. In patients with ESRD due to PH, dialysis cannot remove oxalate as quickly as it accumulates in the blood. In these cases, a special intensive dialysis regimen has to be put into place, which has more sessions per week compared to the standard dialysis therapy, combining both hemodialysis and peritoneal dialysis to achieve maximum oxalate clearance.[2][37] This typically results in 6 to 8 hours of dialysis daily, substantially more than is needed for ESRD alone. High-flux filters are also useful.[8] Due to these drawbacks, dialysis has limited indications. Patients waiting for a liver or renal transplant, posttransplant patients with suboptimal hepatic or renal function, or older patients who are unfit for surgery are a few of the circumstances where intensive dialysis for severe hyperoxaluria might be considered.[33][76] Nedosiran, as mentioned above, is a new experimental treatment that has already demonstrated significant effectiveness in severely hyperoxaluric patients with ESRD on dialysis.[74][75](A1)
Transplant: The procedures to choose from are 1) an isolated liver transplant, 2) an isolated renal transplant, or 3) a combined liver-renal transplant. The final decision is made after considering various factors. Patients with ESRD or a GFR approaching end-stage levels may require renal transplants. A liver transplant is the only curative measure in patients with type I PH, as the problem is dysfunction/defect at the level of the hepatic AGT enzyme isolated renal transplant may be considered in patients who show a positive response to pyridoxine by increasing AGT-activated.[77] However, in most PH cases, combined liver and kidney transplantation has been demonstrated to be superior to isolated kidney transplantation for kidney graft survival, reported to be 76% for combined transplant and 14% for isolated kidney transplant at 5 years. The optimal timing of liver and kidney transplants and whether they should be performed together or sequentially is still being studied.[8](B3)
PH type II manifests due to the defective enzyme glyoxalate/hydroxypyruvate reductase (GRH is found in other tissues besides the liver; therefore, an isolated renal transplant is not recommended for these patients.[78] Patients with PH type III are not usually referred for renal transplantation as the chances of them developing ESRD are extremely low.[2][44] There is minimal data on renal transplantation in patients with secondary hyperoxaluria.[2](B3)
Experimental Treatments
Future therapies for controlling hyperoxaluria being investigated include the following: [56][79][80][81][82][83][84][85](A1)
- Vitamin E and other antioxidant supplementation
- Recombinant gene therapy to replace defective hepatic enzymes
- Intestinal oxalate transport (SLC) blockers, especially SLC26A3 and S1C26A6
- Hepatocyte cell transplantation
- Organic marine hydrocolloid (reduced urinary oxalate by 20% in 1 limited study in patients with severe enteric hyperoxaluria)
- RNA interference therapy (similar to lumasiran, utilizes lipid nanoparticles and N-acetyl galactosamine delivery systems)
- RNA interference therapy targeting non-hepatic enzymes or intestinal oxalate transport mechanisms
- Use of gene-editing technology (CRISPR) to correct specific enzyme pathways for PH. This offers the potential for a single, curative treatment.
- Vit B6, betaine, the antibiotic mitochondrial transport inhibitor dequalinium chloride (DECA), and the alkaloid emetine are being evaluated as chaperone proteins for AGT.
Experimental Plant-Based Therapies
- In early animal studies, banana stem juice appeared promising as a possible therapy for hyperoxaluria.[86]
- Lupeol is chemically a pentacyclic triterpenoid extracted from the Varuna tree (Crataeva nurvala). Lupeol has significantly reduced urinary oxalate in animals and minimized renal tubular damage.[87]
- An oxalate-digesting enzyme has been extracted from beet stems and found effective in animals.[88]
- A surprising number of various plant-based extracts have shown activity in reducing urinary oxalate levels in animals, including Bombax ceiba, Hibiscus sabdariffa, Aierva lanata, Bryophyllum pinnatum, Costus igneius, and Ipomoea eriocarpa, among others. Unfortunately, none of these plant-based remedies has been tested in hyperoxaluric humans. (B3)
Differential Diagnosis
The differential diagnosis should include conditions that lead to nephrolithiasis, specifically calcium oxalate stones and excess deposition in tissues leading to nephrocalcinosis. Some of these conditions are hypocitraturia, medullary sponge kidney, nephrocalcinosis of prematurity, and renal tubular acidosis.
Prognosis
The prognosis of hyperoxaluria depends on the type of hyperoxaluria, time of diagnosis, and early initiation of treatment, amongst other things. As outlined earlier, most patients with secondary hyperoxaluria can be controlled by dietary measures combined with increased urinary volume, optimization of all other urinary stone chemistries, and various supplements and treatments.
Studies suggest that most enteric hyperoxaluria patients have a better prognosis if medical interventions are initiated early, coupled with dietary measures that are strictly followed. Calcium citrate and potassium citrate are the primary medical treatments, with liquid therapies being preferred.
Optimization of all other urinary chemistries is also recommended. Cholestyramine is reasonable to help control both hyperoxaluria and chronic diarrhea, often associated with enteric hyperoxaluria. Reasonable control of stone production is usually possible with aggressive treatment. However, if ESRD occurs in these patients, careful monitoring of peri-transplantation and posttransplantation oxalate and maintaining an adequate urine output should be followed.[89]
Complications
The complications of calcium oxalate stones in the urinary tract include the following:
- Anuria
- Hydronephrosis
- Obstructive pyelonephritis
- Postrenal obstruction and the gradual decline of kidney function [36]
- Renal abscess
- Urine extravasation
- Urosepsis
The development of nephrocalcinosis, further leading to ESRD, is the most dangerous complication. Along with the kidneys, the involvement of the other organ systems is also seen as a complication of the long-term buildup of oxalate in the serum. Hyperoxaluria also leads to renal obstruction, tubular inflammation, tubular atrophy, and interstitial fibrosis.
Deterrence and Patient Education
Patient education in individuals with a tendency for oxalate precipitation is of utmost importance in reducing episodes of kidney stone formation. Preventing dehydration by consuming adequate water and restricting oxalate-rich food in the diet are 2 of the easiest ways to prevent recurrent stone formation. Avoiding vitamin C supplements is advisable. Sodium and protein content in the diet should be decreased along with oxalate to decrease urinary saturation.[48][52]
Additionally, patients with secondary hyperoxaluria or an underlying etiology for steatorrhea should follow a low-fat diet to prevent the entrapment of calcium ions in this luminal fat and subsequent increase in oxalate absorption.[90] In patients with PH, inheritance occurs in an autosomal recessive pattern. Therefore, genetic counseling is essential.[37]
Pearls and Other Issues
Key facts to keep in mind regarding hyperoxaluria include the following:
- Secondary hyperoxaluria is much more common than primary.
- PH types I, II, and III are caused by mutations in the AGXT, GRHPR, and HOGA1 genes, respectively.
- Type I PH is the most common, followed by types II then III.
- Most serum oxalate is generated from the liver, and dietary contribution is usually 10% to 20%, except intoxications (ethylene glycol, vitamin C) and GI surgery or malabsorption syndromes causing calcium to be unavailable to bind with oxalate in the intestines.
- Free genetic screening services for PH and nephrolithiasis are available for patients with significant hyperoxaluria.
- Genetic testing should be considered for children with recurrent oxalate stones and adults with daily urinary oxalate excretion of ≥75 mg.
- Hyperoxaluria may require multimodal approaches.
- Recently approved treatments utilize small interfering RNA technology.
- In cases where hyperoxaluria treatment has failed to normalize urinary oxalate levels, optimize the other treatable urinary chemistries (calcium, citrate, pH, uric acid) and volume as much as possible.
Enhancing Healthcare Team Outcomes
Patients suffering from renal calculi due to hyperoxaluria should receive counsel regarding all the different preventive measures to which they should adhere to avoid recurrent kidney stone formation. Primary care providers often initiate the diagnosis and counseling. The dietician is responsible for carefully crafting their diet while keeping in mind their dietary restrictions of oxalate-rich food and increased fluid intake.
Patients with recurrent episodes and children with early-onset nephrolithiasis are examples of patient groups that would understandably require a high level of motivation to follow the recommended preventive measures. If followed diligently, they can significantly decrease the recurrence rate of calcium oxalate stones. This requires a combined effort of patients, physicians, nursing staff, and dieticians.[91] Urine testing for patients with kidney stones should be strongly encouraged for all interested in reducing their risk of future kidney stone production.[43] See StatPearls' companion reference, "24-Hour Urine Testing for Nephrolithiasis Interpretation and Treatment Guidelines," for more information.
An appropriate nephrolithiasis preventive program should be combined with a regular evaluation for systemic symptoms along with kidney and liver function monitoring. Collaboration, communication, and shared decision-making are critical elements for a good outcome. This requires an interprofessional healthcare team consisting of clinicians, specialists, mid-level practitioners, nursing staff, pharmacists, and various staff for radiology and laboratory testing. The interprofessional care provided to the patient must use an integrated care pathway combined with an evidence-based approach to planning and evaluating all joint activities. Optimal patient outcomes will result.
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
References
Parmar MS. Kidney stones. BMJ (Clinical research ed.). 2004 Jun 12:328(7453):1420-4 [PubMed PMID: 15191979]
Bhasin B, Ürekli HM, Atta MG. Primary and secondary hyperoxaluria: Understanding the enigma. World journal of nephrology. 2015 May 6:4(2):235-44. doi: 10.5527/wjn.v4.i2.235. Epub [PubMed PMID: 25949937]
Level 3 (low-level) evidencePatti L, Leslie SW. Acute Renal Colic. StatPearls. 2024 Jan:(): [PubMed PMID: 28613743]
Leslie SW, Sajjad H, Murphy PB. Renal Calculi. StatPearls. 2024 Jan:(): [PubMed PMID: 28723043]
Taylor EN, Curhan GC. Determinants of 24-hour urinary oxalate excretion. Clinical journal of the American Society of Nephrology : CJASN. 2008 Sep:3(5):1453-60. doi: 10.2215/CJN.01410308. Epub 2008 Jul 23 [PubMed PMID: 18650406]
Level 2 (mid-level) evidenceBuysschaert B, Aydin S, Morelle J, Gillion V, Jadoul M, Demoulin N. Etiologies, Clinical Features, and Outcome of Oxalate Nephropathy. Kidney international reports. 2020 Sep:5(9):1503-1509. doi: 10.1016/j.ekir.2020.06.021. Epub 2020 Jul 2 [PubMed PMID: 32954074]
Bao D, Wang Y, Zhao MH. Oxalate Nephropathy and the Mechanism of Oxalate-Induced Kidney Injury. Kidney diseases (Basel, Switzerland). 2023 Dec:9(6):459-468. doi: 10.1159/000533295. Epub 2023 Jul 27 [PubMed PMID: 38089442]
Shee K, Stoller ML. Perspectives in primary hyperoxaluria - historical, current and future clinical interventions. Nature reviews. Urology. 2022 Mar:19(3):137-146. doi: 10.1038/s41585-021-00543-4. Epub 2021 Dec 8 [PubMed PMID: 34880452]
Level 3 (low-level) evidenceHolmes RP, Goodman HO, Assimos DG. Contribution of dietary oxalate to urinary oxalate excretion. Kidney international. 2001 Jan:59(1):270-6 [PubMed PMID: 11135080]
Mitchell T, Kumar P, Reddy T, Wood KD, Knight J, Assimos DG, Holmes RP. Dietary oxalate and kidney stone formation. American journal of physiology. Renal physiology. 2019 Mar 1:316(3):F409-F413. doi: 10.1152/ajprenal.00373.2018. Epub 2018 Dec 19 [PubMed PMID: 30566003]
Terris MK, Issa MM, Tacker JR. Dietary supplementation with cranberry concentrate tablets may increase the risk of nephrolithiasis. Urology. 2001 Jan:57(1):26-9 [PubMed PMID: 11164137]
Level 3 (low-level) evidenceSiener R, Bade DJ, Hesse A, Hoppe B. Dietary hyperoxaluria is not reduced by treatment with lactic acid bacteria. Journal of translational medicine. 2013 Dec 12:11():306. doi: 10.1186/1479-5876-11-306. Epub 2013 Dec 12 [PubMed PMID: 24330782]
Nazzal L, Puri S, Goldfarb DS. Enteric hyperoxaluria: an important cause of end-stage kidney disease. Nephrology, dialysis, transplantation : official publication of the European Dialysis and Transplant Association - European Renal Association. 2016 Mar:31(3):375-82. doi: 10.1093/ndt/gfv005. Epub 2015 Feb 20 [PubMed PMID: 25701816]
Sidhu H, Schmidt ME, Cornelius JG, Thamilselvan S, Khan SR, Hesse A, Peck AB. Direct correlation between hyperoxaluria/oxalate stone disease and the absence of the gastrointestinal tract-dwelling bacterium Oxalobacter formigenes: possible prevention by gut recolonization or enzyme replacement therapy. Journal of the American Society of Nephrology : JASN. 1999 Nov:10 Suppl 14():S334-40 [PubMed PMID: 10541258]
Level 3 (low-level) evidenceTroxel SA, Sidhu H, Kaul P, Low RK. Intestinal Oxalobacter formigenes colonization in calcium oxalate stone formers and its relation to urinary oxalate. Journal of endourology. 2003 Apr:17(3):173-6 [PubMed PMID: 12803990]
Siener R, Ebert D, Hesse A. Urinary oxalate excretion in female calcium oxalate stone formers with and without a history of recurrent urinary tract infections. Urological research. 2001 Aug:29(4):245-8 [PubMed PMID: 11585279]
Sidhu H, Hoppe B, Hesse A, Tenbrock K, Brömme S, Rietschel E, Peck AB. Absence of Oxalobacter formigenes in cystic fibrosis patients: a risk factor for hyperoxaluria. Lancet (London, England). 1998 Sep 26:352(9133):1026-9 [PubMed PMID: 9759746]
Demoulin N, Issa Z, Crott R, Morelle J, Danse E, Wallemacq P, Jadoul M, Deprez PH. Enteric hyperoxaluria in chronic pancreatitis. Medicine. 2017 May:96(19):e6758. doi: 10.1097/MD.0000000000006758. Epub [PubMed PMID: 28489752]
de Martines DGL, Gianotten S, F M Wetzels J, G van der Meijden WA. Secondary hyperoxaluria due to pancreatic insufficiency. The Netherlands journal of medicine. 2019 Oct:77(8):287-292 [PubMed PMID: 31814577]
Ghannoum M, Gosselin S, Hoffman RS, Lavergne V, Mégarbane B, Hassanian-Moghaddam H, Rif M, Kallab S, Bird S, Wood DM, Roberts DM, EXTRIP Workgroup. Extracorporeal treatment for ethylene glycol poisoning: systematic review and recommendations from the EXTRIP workgroup. Critical care (London, England). 2023 Feb 10:27(1):56. doi: 10.1186/s13054-022-04227-2. Epub 2023 Feb 10 [PubMed PMID: 36765419]
Level 1 (high-level) evidenceBnaya A, Abu-Amer N, Beckerman P, Volkov A, Cohen-Hagai K, Greenberg M, Ben-Chetrit S, Ben Tikva Kagan K, Goldman S, Navarro HA, Sneineh MA, Rozen-Zvi B, Borovitz Y, Tobar A, Yanay NB, Biton R, Angel-Korman A, Rappoport V, Leiba A, Bathish Y, Farber E, Kaidar-Ronat M, Schreiber L, Shashar M, Kazarski R, Chernin G, Itzkowitz E, Atrash J, Iaina NL, Efrati S, Nizri E, Lurie Y, Ben Itzhak O, Assady S, Kenig-Kozlovsky Y, Shavit L. Acute Kidney Injury and Hair-Straightening Products: A Case Series. American journal of kidney diseases : the official journal of the National Kidney Foundation. 2023 Jul:82(1):43-52.e1. doi: 10.1053/j.ajkd.2022.11.016. Epub 2023 Jan 5 [PubMed PMID: 36610611]
Level 2 (mid-level) evidenceAbu-Amer N, Silberstein N, Kunin M, Mini S, Beckerman P. Acute Kidney Injury following Exposure to Formaldehyde-Free Hair-Straightening Products. Case reports in nephrology and dialysis. 2022 May-Aug:12(2):112-116. doi: 10.1159/000525567. Epub 2022 Jul 11 [PubMed PMID: 36160636]
Level 3 (low-level) evidenceViljoen A, Chaudhry R, Bycroft J. Renal stones. Annals of clinical biochemistry. 2019 Jan:56(1):15-27. doi: 10.1177/0004563218781672. Epub 2018 Jun 13 [PubMed PMID: 29792045]
Worcester EM, Coe FL. Nephrolithiasis. Primary care. 2008 Jun:35(2):369-91, vii. doi: 10.1016/j.pop.2008.01.005. Epub [PubMed PMID: 18486720]
Han H, Segal AM, Seifter JL, Dwyer JT. Nutritional Management of Kidney Stones (Nephrolithiasis). Clinical nutrition research. 2015 Jul:4(3):137-52. doi: 10.7762/cnr.2015.4.3.137. Epub 2015 Jul 31 [PubMed PMID: 26251832]
Spradling K, Vernez SL, Khoyliar C, Morgan JB, Okhunov Z, Preminger GM, Lipkin ME, Landman J, Youssef RF. Prevalence of Hyperoxaluria in Urinary Stone Formers: Chronological and Geographical Trends and a Literature Review. Journal of endourology. 2016 Apr:30(4):469-75. doi: 10.1089/end.2015.0676. Epub 2016 Feb 9 [PubMed PMID: 26738689]
Powell CR, Stoller ML, Schwartz BF, Kane C, Gentle DL, Bruce JE, Leslie SW. Impact of body weight on urinary electrolytes in urinary stone formers. Urology. 2000 Jun:55(6):825-30 [PubMed PMID: 10840085]
Curhan GC, Willett WC, Speizer FE, Stampfer MJ. Twenty-four-hour urine chemistries and the risk of kidney stones among women and men. Kidney international. 2001 Jun:59(6):2290-8 [PubMed PMID: 11380833]
Level 2 (mid-level) evidenceLewandowski S, Rodgers A, Schloss I. The influence of a high-oxalate/low-calcium diet on calcium oxalate renal stone risk factors in non-stone-forming black and white South African subjects. BJU international. 2001 Mar:87(4):307-11 [PubMed PMID: 11251520]
Rodgers AL, Lewandowski S. Effects of 5 different diets on urinary risk factors for calcium oxalate kidney stone formation: evidence of different renal handling mechanisms in different race groups. The Journal of urology. 2002 Sep:168(3):931-6 [PubMed PMID: 12187193]
Goldfarb DS, Parks JH, Coe FL. Renal stone disease in older adults. Clinics in geriatric medicine. 1998 May:14(2):367-81 [PubMed PMID: 9536110]
Hopp K, Cogal AG, Bergstralh EJ, Seide BM, Olson JB, Meek AM, Lieske JC, Milliner DS, Harris PC, Rare Kidney Stone Consortium. Phenotype-Genotype Correlations and Estimated Carrier Frequencies of Primary Hyperoxaluria. Journal of the American Society of Nephrology : JASN. 2015 Oct:26(10):2559-70. doi: 10.1681/ASN.2014070698. Epub 2015 Feb 2 [PubMed PMID: 25644115]
Harambat J, Fargue S, Bacchetta J, Acquaviva C, Cochat P. Primary hyperoxaluria. International journal of nephrology. 2011:2011():864580. doi: 10.4061/2011/864580. Epub 2011 Jun 16 [PubMed PMID: 21748001]
Cochat P, Rumsby G. Primary hyperoxaluria. The New England journal of medicine. 2013 Aug 15:369(7):649-58. doi: 10.1056/NEJMra1301564. Epub [PubMed PMID: 23944302]
Soliman NA, Mabrouk S. Primary hyperoxaluria type 1 in developing countries: novel challenges in a new therapeutic era. Clinical kidney journal. 2022 May:15(Suppl 1):i33-i36. doi: 10.1093/ckj/sfab203. Epub 2022 May 17 [PubMed PMID: 35592622]
Khan SR, Pearle MS, Robertson WG, Gambaro G, Canales BK, Doizi S, Traxer O, Tiselius HG. Kidney stones. Nature reviews. Disease primers. 2016 Feb 25:2():16008. doi: 10.1038/nrdp.2016.8. Epub 2016 Feb 25 [PubMed PMID: 27188687]
Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Bean LJH, Gripp KW, Amemiya A, Milliner DS, Harris PC, Sas DJ, Cogal AG, Lieske JC. Primary Hyperoxaluria Type 1. GeneReviews(®). 1993:(): [PubMed PMID: 20301460]
Waikar SS, Srivastava A, Palsson R, Shafi T, Hsu CY, Sharma K, Lash JP, Chen J, He J, Lieske J, Xie D, Zhang X, Feldman HI, Curhan GC, Chronic Renal Insufficiency Cohort study investigators. Association of Urinary Oxalate Excretion With the Risk of Chronic Kidney Disease Progression. JAMA internal medicine. 2019 Apr 1:179(4):542-551. doi: 10.1001/jamainternmed.2018.7980. Epub [PubMed PMID: 30830167]
Ermer T, Eckardt KU, Aronson PS, Knauf F. Oxalate, inflammasome, and progression of kidney disease. Current opinion in nephrology and hypertension. 2016 Jul:25(4):363-71. doi: 10.1097/MNH.0000000000000229. Epub [PubMed PMID: 27191349]
Level 3 (low-level) evidenceLeumann E, Hoppe B. The primary hyperoxalurias. Journal of the American Society of Nephrology : JASN. 2001 Sep:12(9):1986-1993. doi: 10.1681/ASN.V1291986. Epub [PubMed PMID: 11518794]
Alelign T, Petros B. Kidney Stone Disease: An Update on Current Concepts. Advances in urology. 2018:2018():3068365. doi: 10.1155/2018/3068365. Epub 2018 Feb 4 [PubMed PMID: 29515627]
Level 3 (low-level) evidenceCorder CJ, Rathi BM, Sharif S, Leslie SW. 24-Hour Urine Collection. StatPearls. 2024 Jan:(): [PubMed PMID: 29494089]
Leslie SW, Sajjad H, Bashir K. 24-Hour Urine Testing for Nephrolithiasis: Interpretation and Treatment Guidelines. StatPearls. 2024 Jan:(): [PubMed PMID: 29494055]
Hoppe B. An update on primary hyperoxaluria. Nature reviews. Nephrology. 2012 Jun 12:8(8):467-75. doi: 10.1038/nrneph.2012.113. Epub 2012 Jun 12 [PubMed PMID: 22688746]
Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Bean LJH, Gripp KW, Amemiya A, Milliner DS, Harris PC, Sas DJ, Lieske JC. Primary Hyperoxaluria Type 3. GeneReviews(®). 1993:(): [PubMed PMID: 26401545]
Cochat P, Hulton SA, Acquaviva C, Danpure CJ, Daudon M, De Marchi M, Fargue S, Groothoff J, Harambat J, Hoppe B, Jamieson NV, Kemper MJ, Mandrile G, Marangella M, Picca S, Rumsby G, Salido E, Straub M, van Woerden CS, OxalEurope. Primary hyperoxaluria Type 1: indications for screening and guidance for diagnosis and treatment. Nephrology, dialysis, transplantation : official publication of the European Dialysis and Transplant Association - European Renal Association. 2012 May:27(5):1729-36. doi: 10.1093/ndt/gfs078. Epub [PubMed PMID: 22547750]
Pearle MS, Goldfarb DS, Assimos DG, Curhan G, Denu-Ciocca CJ, Matlaga BR, Monga M, Penniston KL, Preminger GM, Turk TM, White JR, American Urological Assocation. Medical management of kidney stones: AUA guideline. The Journal of urology. 2014 Aug:192(2):316-24. doi: 10.1016/j.juro.2014.05.006. Epub 2014 May 20 [PubMed PMID: 24857648]
Finkielstein VA, Goldfarb DS. Strategies for preventing calcium oxalate stones. CMAJ : Canadian Medical Association journal = journal de l'Association medicale canadienne. 2006 May 9:174(10):1407-9 [PubMed PMID: 16682705]
Leslie SW, Sajjad H. Hypercalciuria. StatPearls. 2024 Jan:(): [PubMed PMID: 28846247]
Milliner DS, Eickholt JT, Bergstralh EJ, Wilson DM, Smith LH. Results of long-term treatment with orthophosphate and pyridoxine in patients with primary hyperoxaluria. The New England journal of medicine. 1994 Dec 8:331(23):1553-8 [PubMed PMID: 7969325]
Park S, Pearle MS. Pathophysiology and management of calcium stones. The Urologic clinics of North America. 2007 Aug:34(3):323-34 [PubMed PMID: 17678983]
Noonan SC, Savage GP. Oxalate content of foods and its effect on humans. Asia Pacific journal of clinical nutrition. 1999 Mar:8(1):64-74 [PubMed PMID: 24393738]
Dejban P, Lieske JC. New therapeutics for primary hyperoxaluria type 1. Current opinion in nephrology and hypertension. 2022 Jul 1:31(4):344-350. doi: 10.1097/MNH.0000000000000790. Epub 2022 Mar 9 [PubMed PMID: 35266883]
Level 3 (low-level) evidenceHoppe B, Martin-Higueras C. Improving Treatment Options for Primary Hyperoxaluria. Drugs. 2022 Jul:82(10):1077-1094. doi: 10.1007/s40265-022-01735-x. Epub 2022 Jul 2 [PubMed PMID: 35779234]
Hoppe B, Groothoff JW, Hulton SA, Cochat P, Niaudet P, Kemper MJ, Deschênes G, Unwin R, Milliner D. Efficacy and safety of Oxalobacter formigenes to reduce urinary oxalate in primary hyperoxaluria. Nephrology, dialysis, transplantation : official publication of the European Dialysis and Transplant Association - European Renal Association. 2011 Nov:26(11):3609-15. doi: 10.1093/ndt/gfr107. Epub 2011 Apr 2 [PubMed PMID: 21460356]
Level 1 (high-level) evidenceHoppe B, Niaudet P, Salomon R, Harambat J, Hulton SA, Van't Hoff W, Moochhala SH, Deschênes G, Lindner E, Sjögren A, Cochat P. A randomised Phase I/II trial to evaluate the efficacy and safety of orally administered Oxalobacter formigenes to treat primary hyperoxaluria. Pediatric nephrology (Berlin, Germany). 2017 May:32(5):781-790. doi: 10.1007/s00467-016-3553-8. Epub 2016 Dec 6 [PubMed PMID: 27924398]
Level 1 (high-level) evidenceMilliner D, Hoppe B, Groothoff J. A randomised Phase II/III study to evaluate the efficacy and safety of orally administered Oxalobacter formigenes to treat primary hyperoxaluria. Urolithiasis. 2018 Aug:46(4):313-323. doi: 10.1007/s00240-017-0998-6. Epub 2017 Jul 17 [PubMed PMID: 28718073]
Level 1 (high-level) evidenceQuintero E, Bird VY, Liu H, Stevens G, Ryan AS, Buzzerd S, Klimberg IW. A Prospective, Double-Blind, Randomized, Placebo-Controlled, Crossover Study Using an Orally Administered Oxalate Decarboxylase (OxDC). Kidney360. 2020 Nov 25:1(11):1284-1290. doi: 10.34067/KID.0001522020. Epub 2020 Sep 3 [PubMed PMID: 35372879]
Level 1 (high-level) evidenceSenthil D, Malini MM, Varalakshmi P. Sodium pentosan polysulphate--a novel inhibitor of urinary risk factors and enzymes in experimental urolithiatic rats. Renal failure. 1998 Jul:20(4):573-80 [PubMed PMID: 9713875]
Level 3 (low-level) evidenceSenthil D, Subha K, Saravanan N, Varalakshmi P. Influence of sodium pentosan polysulphate and certain inhibitors on calcium oxalate crystal growth. Molecular and cellular biochemistry. 1996 Mar 9:156(1):31-5 [PubMed PMID: 8709973]
Fellström B, Backman U, Danielson B, Wikström B. Treatment of renal calcium stone disease with the synthetic glycosaminoglycan pentosan polysulphate. World journal of urology. 1994:12(1):52-4 [PubMed PMID: 7516780]
Nakatani T, Ishii K, Yoneda Y, Kamikawa S, Kanazawa T, Sugimoto T, Osswald H. The preventive effect of sodium pentosan polysulfate against renal stone formation in hyperoxaluric rats. Urological research. 2002 Oct:30(5):329-35 [PubMed PMID: 12389123]
Level 3 (low-level) evidenceErturk E, Kiernan M, Schoen SR. Clinical association with urinary glycosaminoglycans and urolithiasis. Urology. 2002 Apr:59(4):495-9 [PubMed PMID: 11927298]
Level 2 (mid-level) evidenceMargines JB, Hobbs SD. Pentosan Polysulfate Maculopathy. StatPearls. 2024 Jan:(): [PubMed PMID: 36944010]
Takei K, Ito H, Masai M, Kotake T. Oral calcium supplement decreases urinary oxalate excretion in patients with enteric hyperoxaluria. Urologia internationalis. 1998:61(3):192-5 [PubMed PMID: 9933846]
Level 3 (low-level) evidenceDamasio PC, Amaro CR, Cunha NB, Pichutte AC, Goldberg J, Padovani CR, Amaro JL. The role of salt abuse on risk for hypercalciuria. Nutrition journal. 2011 Jan 6:10():3. doi: 10.1186/1475-2891-10-3. Epub 2011 Jan 6 [PubMed PMID: 21211048]
Level 2 (mid-level) evidenceReddy ST, Wang CY, Sakhaee K, Brinkley L, Pak CY. Effect of low-carbohydrate high-protein diets on acid-base balance, stone-forming propensity, and calcium metabolism. American journal of kidney diseases : the official journal of the National Kidney Foundation. 2002 Aug:40(2):265-74 [PubMed PMID: 12148098]
Nguyen QV, Kälin A, Drouve U, Casez JP, Jaeger P. Sensitivity to meat protein intake and hyperoxaluria in idiopathic calcium stone formers. Kidney international. 2001 Jun:59(6):2273-81 [PubMed PMID: 11380831]
Level 3 (low-level) evidenceEusufzai S. Bile acid malabsorption: mechanisms and treatment. Digestive diseases (Basel, Switzerland). 1995 Sep-Oct:13(5):312-21 [PubMed PMID: 8542666]
Scott LJ, Keam SJ. Lumasiran: First Approval. Drugs. 2021 Feb:81(2):277-282. doi: 10.1007/s40265-020-01463-0. Epub [PubMed PMID: 33405070]
Moya-Garzon MD, Gomez-Vidal JA, Alejo-Armijo A, Altarejos J, Rodriguez-Madoz JR, Fernandes MX, Salido E, Salido S, Diaz-Gavilan M. Small Molecule-Based Enzyme Inhibitors in the Treatment of Primary Hyperoxalurias. Journal of personalized medicine. 2021 Jan 27:11(2):. doi: 10.3390/jpm11020074. Epub 2021 Jan 27 [PubMed PMID: 33513899]
Garrelfs SF, Frishberg Y, Hulton SA, Koren MJ, O'Riordan WD, Cochat P, Deschênes G, Shasha-Lavsky H, Saland JM, Van't Hoff WG, Fuster DG, Magen D, Moochhala SH, Schalk G, Simkova E, Groothoff JW, Sas DJ, Meliambro KA, Lu J, Sweetser MT, Garg PP, Vaishnaw AK, Gansner JM, McGregor TL, Lieske JC, ILLUMINATE-A Collaborators. Lumasiran, an RNAi Therapeutic for Primary Hyperoxaluria Type 1. The New England journal of medicine. 2021 Apr 1:384(13):1216-1226. doi: 10.1056/NEJMoa2021712. Epub [PubMed PMID: 33789010]
Liu A, Zhao J, Shah M, Migliorati JM, Tawfik SM, Bahal R, Rasmussen TP, Manautou JE, Zhong XB. Nedosiran, a Candidate siRNA Drug for the Treatment of Primary Hyperoxaluria: Design, Development, and Clinical Studies. ACS pharmacology & translational science. 2022 Nov 11:5(11):1007-1016. doi: 10.1021/acsptsci.2c00110. Epub 2022 Sep 21 [PubMed PMID: 36407951]
Shee K, Ahn J, Hamouche F, Mena J, Chi T, Stoller ML. Nedosiran Dramatically Reduces Serum Oxalate in Dialysis-Dependent Primary Hyperoxaluria 1: A Compassionate Use Case Report. Urology. 2021 Oct:156():e147-e149. doi: 10.1016/j.urology.2021.03.014. Epub 2021 Mar 25 [PubMed PMID: 33774044]
Level 3 (low-level) evidenceBaum MA, Langman C, Cochat P, Lieske JC, Moochhala SH, Hamamoto S, Satoh H, Mourani C, Ariceta G, Torres A, Wolley M, Belostotsky V, Forbes TA, Groothoff J, Hayes W, Tönshoff B, Takayama T, Rosskamp R, Russell K, Zhou J, Amrite A, Hoppe B, PHYOX2 study investigators. PHYOX2: a pivotal randomized study of nedosiran in primary hyperoxaluria type 1 or 2. Kidney international. 2023 Jan:103(1):207-217. doi: 10.1016/j.kint.2022.07.025. Epub 2022 Aug 22 [PubMed PMID: 36007597]
Level 1 (high-level) evidenceBobrowski AE, Langman CB. Hyperoxaluria and systemic oxalosis: current therapy and future directions. Expert opinion on pharmacotherapy. 2006 Oct:7(14):1887-96 [PubMed PMID: 17020415]
Level 3 (low-level) evidenceSaborio P, Scheinman JI. Transplantation for primary hyperoxaluria in the United States. Kidney international. 1999 Sep:56(3):1094-100 [PubMed PMID: 10469379]
Garrelfs SF, Rumsby G, Peters-Sengers H, Erger F, Groothoff JW, Beck BB, Oosterveld MJS, Pelle A, Neuhaus T, Adams B, Cochat P, Salido E, Lipkin GW, Hoppe B, Hulton SA, OxalEurope Consortium. Patients with primary hyperoxaluria type 2 have significant morbidity and require careful follow-up. Kidney international. 2019 Dec:96(6):1389-1399. doi: 10.1016/j.kint.2019.08.018. Epub 2019 Sep 3 [PubMed PMID: 31685312]
Lieske JC, Goldfarb DS, De Simone C, Regnier C. Use of a probiotic to decrease enteric hyperoxaluria. Kidney international. 2005 Sep:68(3):1244-9 [PubMed PMID: 16105057]
Straub M, Hautmann RE, Hesse A, Rinnab L. [Calcium oxalate stones and hyperoxaluria. What is certain? What is new?]. Der Urologe. Ausg. A. 2005 Nov:44(11):1315-23 [PubMed PMID: 16235094]
Peck AB, Canales BK, Nguyen CQ. Oxalate-degrading microorganisms or oxalate-degrading enzymes: which is the future therapy for enzymatic dissolution of calcium-oxalate uroliths in recurrent stone disease? Urolithiasis. 2016 Feb:44(1):45-50. doi: 10.1007/s00240-015-0845-6. Epub 2015 Dec 8 [PubMed PMID: 26645869]
Whittamore JM, Hatch M. The role of intestinal oxalate transport in hyperoxaluria and the formation of kidney stones in animals and man. Urolithiasis. 2017 Feb:45(1):89-108. doi: 10.1007/s00240-016-0952-z. Epub 2016 Dec 2 [PubMed PMID: 27913853]
Level 3 (low-level) evidenceBurns Z, Knight J, Fargue S, Holmes R, Assimos D, Wood K. Future treatments for hyperoxaluria. Current opinion in urology. 2020 Mar:30(2):171-176. doi: 10.1097/MOU.0000000000000709. Epub [PubMed PMID: 31895888]
Level 3 (low-level) evidenceLindsjö M, Fellström B, Ljunghall S, Wikström B, Danielson BG. Treatment of enteric hyperoxaluria with calcium-containing organic marine hydrocolloid. Lancet (London, England). 1989 Sep 23:2(8665):701-4 [PubMed PMID: 2570957]
Level 3 (low-level) evidenceLetavernier E, Daudon M. Stiripentol identifies a therapeutic target to reduce oxaluria. Current opinion in nephrology and hypertension. 2020 Jul:29(4):394-399. doi: 10.1097/MNH.0000000000000621. Epub [PubMed PMID: 32452916]
Level 3 (low-level) evidencePoonguzhali PK, Chegu H. The influence of banana stem extract on urinary risk factors for stones in normal and hyperoxaluric rats. British journal of urology. 1994 Jul:74(1):23-5 [PubMed PMID: 8044524]
Level 3 (low-level) evidenceMalini MM, Baskar R, Varalakshmi P. Effect of lupeol, a pentacyclic triterpene, on urinary enzymes in hyperoxaluric rats. Japanese journal of medical science & biology. 1995 Oct-Dec:48(5-6):211-20 [PubMed PMID: 8718554]
Level 3 (low-level) evidenceRamakrishnan V, Lathika KM, D'Souza SJ, Singh BB, Raghavan KG. Investigation with chitosan-oxalate oxidase-catalase conjugate for degrading oxalate from hyperoxaluric rat chyme. Indian journal of biochemistry & biophysics. 1997 Aug:34(4):373-8 [PubMed PMID: 9491647]
Level 3 (low-level) evidenceRoodnat JI, de Mik-van Egmond AME, Visser WJ, Berger SP, van der Meijden WAG, Knauf F, van Agteren M, Betjes MGH, Hoorn EJ. A Successful Approach to Kidney Transplantation in Patients With Enteric (Secondary) Hyperoxaluria. Transplantation direct. 2017 Dec:3(12):e331. doi: 10.1097/TXD.0000000000000748. Epub 2017 Nov 8 [PubMed PMID: 29536032]
Andersson H, Jagenburg R. Fat-reduced diet in the treatment of hyperoxaluria in patients with ileopathy. Gut. 1974 May:15(5):360-6 [PubMed PMID: 18668844]
Morgan MS, Pearle MS. Medical management of renal stones. BMJ (Clinical research ed.). 2016 Mar 14:352():i52. doi: 10.1136/bmj.i52. Epub 2016 Mar 14 [PubMed PMID: 26977089]