Introduction
Filariasis is a disease caused by a chronic mosquito-borne parasitic infection. Chronic infection can lead to swelling of the extremities, hydroceles, and testicular masses.[1][2][3] It is the second-largest cause of permanent deformity and disability behind leprosy worldwide. Lymphatic filariasis (LF) is currently considered a neglected tropical disease. The Global Programme to Eliminate Lymphatic Filariasis is providing mass drug administrations (MDA) to populations in endemic areas in a push to eradicate this disease.[1] Several programs exist to encourage participation with MDA.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Filariasis is caused by at least three species of nematode parasites (Wuchereria bancrofti, Brugia malayi, and Brugia timori) and is transmitted to 5 genera of mosquitoes including Aedes, Anopheles, Culex, Mansonia, and Ochlerotatus.[1]
Epidemiology
It affects 120 million people in 72 countries worldwide, mostly in the tropics and subtropical climates of Asia, Africa, the Western Pacific, South America, and the Caribbean. Four countries in America are endemic: Haiti, Dominican Republic, Guyana, and Brazil [4]. One-third of children in endemic regions are asymptomatically infected with W. bancrofti.[5] Half of the patients infected are in their 30s or 40s, and there is a 10:1 predilection for men to women.[6]
Pathophysiology
Humans are the primary reservoir for this parasitic disease, and mosquitoes are the vector. The mosquito deposits larvae into the bloodstream. They take up residence in the lymph nodes and grow into adult worms. The larvae have a predilection to deposit in femoral lymph nodes. They undergo sexual reproduction, and females give birth to countless microfilariae, which are dumped into circulation in a diurnal pattern. Females can give off eggs for approximately 5 years, and adults can live up to 9 years.[6] With the proliferation of adult worms, the lymphatics become occluded, which disrupts the lymphatic drainage and increases the susceptibility to repeated infections - most notably streptococcal and fungal infections. This acute-on-chronic inflammation leads to fibrosis and remodeling of the lymphatics, further perpetuating contractile dysfunction and leading to the dermal skin changes seen with elephantiasis.[6][7]
Histopathology
Brugia and Wuchereria species are similar in morphology and are the main cause of filariasis. They can be identified to the genus level using size, body wall composition, thickness, and morphology of the cuticle. The presence of small filarial worms in lymph nodes is pathognomonic for either Wuchereria or Brugia. Adult worms are typically found in lymph nodes in the groin or neck, whereas microfilariae are typically found in the peripheral blood.[8]
The adult worms typically range in size from 45 to 100 micrometers in diameter and are typically found in lymph node cross-section. Their descriptions include "thin, smooth cuticle which is thickened over lateral chords, three or four well-developed, low, broad muscle cells per quadrant, and relatively broad, flat lateral chords."[8]
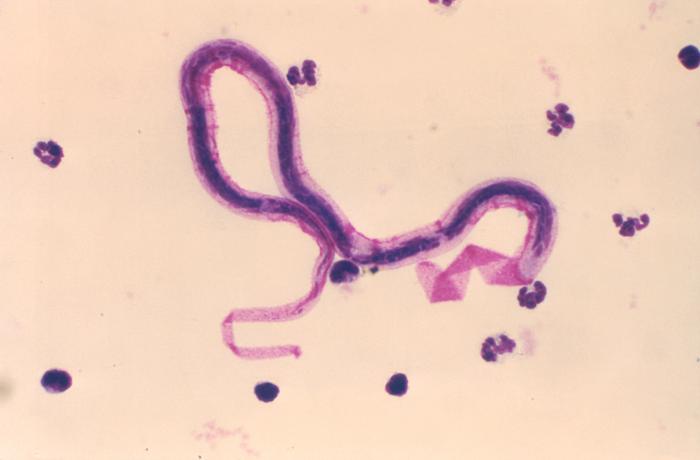
Microfilariae can be seen with a blood smear or other peripheral blood sample that is stained with either Giemsa or hematoxylin and eosin (H&E) stain. The blood samples should be taken after 8 pm. The microfilariae vary in size from 200 to 300 micrometers in length and 2 to 8 micrometers in diameter and are identified by the terminal and subterminal nuclei in the tail region.[8]
History and Physical
The most common condition of filariasis is a hydrocele.[6] Children are often asymptomatic and typically present after the onset of puberty and likely into the 2nd or 3rd decade of life.[6][9]
Additional manifestations include:
Filariatic fever - manifests with lymphangitis and lymphadenitis with nonspecific symptoms including headache, fever, chills, and general malaise.
Filarial abscess - may form causing localized swelling and pain until rupture, which results in the discharge of dead adult worms. Granulomatous reactions can lead to lumps in subcutaneous tissues.[6]
Acute dermatolymphangioadenitis (ADL) - repeated bouts of lymphangitis causing lymphedema.
Lymphedema - graded based on the extent of the condition
- Grade I: Extremity pitting edema, reversible
- Grade II: Extremity pitting or nonpitting edema, nonreversible
- Grade II: Nonpitting, nonreversible edema, with skin thickening
- Grade IV: Nonpitting, nonreversible, thickened and nodular appearance of the skin, classified as elephantiasis.[9]
Tropical pulmonary eosinophilia - an immune response to filarial infection. It causes pulmonary restrictive lung disease, wheezing, shortness of breath, and eosinophilia.[6]
Evaluation
Peripheral smear – The Centers for Disease Control (CDC) recommends preparing two thick and thin peripheral blood smear samples taken from either venipuncture or finger/heel stick. These are preferably taken after 8 pm given the night periodicity of microfilariae and stained with either Giemsa or H&E stain.[6]
PCR - for detecting antigen. Antigen detection is the preferred method of diagnosis since it also detects latent infections. However, assays for parasite antigen of W. bancrofti are currently not approved by the FDA.
Scrotal ultrasound - may reveal movements of adult worms in otherwise asymptomatic males. The "filarial dance sign" is a pattern of worm movement that can be detected in the lymphatic vessels of infected men.[10]
Treatment / Management
Medical treatments
Diethylcarbamazine (DEC) has traditionally been recommended as potential monotherapy; however, it is to be avoided if there is coinfection with Loa loa or onychomycosis as it can worsen the progression of eye disease and can cause encephalopathy.[1][6] A single combined dose of ivermectin, albendazole, and DEC resulted in clearance of microfilaria in 96% of affected patients for up to 3 years and is currently recommended by the World Health Organization (WHO) as triple therapy in areas not endemic with Loa loa.[11] Doxycycline is preferred in areas co-endemic with Loa loa and has also shown the ability to slow the inflammation and fibrosis that leads to worsening lymphedema. Doxycycline also treats Wolbachia, a genus of symbiotic bacteria that inhabit nematodes.[1][12](A1)
There is currently no vaccine for filariasis, but efforts are ongoing to develop one.[13](B3)
Surgical treatments
Surgical treatments exist for the debulking of skin and creating lymphovenous anastomosis to improve drainage. Topical coumarin and flavonoids were shown to be effective in reducing lymphedema. It is thought that increased macrophage activity leads to the reuptake of proteinaceous material.[9]
A case report documented the success of ablative carbon dioxide laser treatment of skin lesions and lymphocutaneous fistulas, which resulted in significant improvement of skin lesions. It works via causing thermal damage to dermis resulting in remodeling of superficial tissue and dermal tightening. This was done in a patient with non-filarial elephantiasis but could have an application in filarial disease.[14]
Chronic Management
Lymphedema can progress due to repeated attacks of adenolymphangitis even in the absence of LF. Strategies targeting lymphedema progression include working with patients on skin hygiene, wearing comfortable shoes, using compressive bandages, pneumatic compression, regular washing with soap and water, limb elevation, cold/heat therapy, and antibiotic and antifungal creams to prevent flares of lymphangitis.[9][15][6] (A1)
Differential Diagnosis
The differential diagnosis includes [8][9][8]:
- Several zoonotic filariasis including Onchocerca, Dirofilaria, Brugia, Dipetalonema, Loaina, Meningonema
- Lymphoma
- Testicular neoplasms
- Congenital abnormalities of lymphatics
- Pelvic malignancy
- Damage to lymph system secondary to surgery or radiation
Pertinent Studies and Ongoing Trials
The Global Programme to Eliminate Lymphatic Filariasis is aiming to eradicate filariasis by 2020. They are currently monitoring, mapping, and mass distributing drugs to endemic areas. An update provided from this program in 2010 reports reaching the halfway point towards eliminating filariasis. As of 2015, a total of 6.2 billion treatments delivered to over 820 million people. According to WHO data as of 12/2019, the following countries have eliminated lymphatic filariasis as a public health problem: Egypt, Yemen, Thailand, Vietnam, Cambodia, Sri Lanka.
Prognosis
The prognosis is good if filariasis is recognized early and treated in a timely fashion to prevent deformity. The disease typically responds to 5 annual doses of DEC with or without ivermectin or albendazole. Symptoms don’t present until later into adulthood and correlate with increasing worm burden. Elephantiasis is the most severe form and is due to many years of acute on chronic superimposed infections. There is some ability to treat lymphedema, but it is difficult to manage once reaching advanced stages of the disease.
Complications
Occult filariasis - infection of other tissues without evidence in blood.[6] It can lead to:
- Tropical pulmonary eosinophilia
- Filarial arthritis
- Filarial-associated immune complex glomerulonephritis
- Filarial breast abscesses
Loiasis - co-endemic infection. It can cause severe drug interactions including encephalopathy if treated with ivermectin.[16]
Adverse effects after receiving targeted medical therapy are likely related to systemic inflammation from filarial activity. Complications reported include fever, chills, some hemodynamic changes including changes to systolic blood pressure with no frank hypotension.[17]
Consultations
Lymphatic filariasis is rare in the United States. DEC is no longer approved by the FDA, and providers will need CDC assistance with obtaining appropriate medications and also with the confirmation of infection. Patients with a coinfection of onchocerciasis with high levels of microfilaria should have a tropical medicine consultation.
Deterrence and Patient Education
WHO-supported strategies for vector control include insecticide-treated nets, indoor spraying, personal protection, and mass drug administration for at-risk individuals.
Travelers are at little risk for developing lymphatic filariasis as it takes years of multiple exposures from infected mosquitoes to establish infection in humans, given lack of reproduction in mosquitoes.[1]
Enhancing Healthcare Team Outcomes
Lymphatic filariasis is a rare but disfiguring disease that can lead to marked morbidity if not considered. Several diagnostic and treatment recommendations are listed above. Physicians will have to work in tandem with nursing, administration, and public health officials in both confirming the diagnosis and successfully treating patients. Depending on the severity of disfigurement, they may require additional surgical consultation. The patient may need wound care and further education in hygiene and continued to follow up to prevent further attacks, which would lead to worse outcomes.
Media
(Click Image to Enlarge)
References
Rebollo MP, Bockarie MJ. Can Lymphatic Filariasis Be Eliminated by 2020? Trends in parasitology. 2017 Feb:33(2):83-92. doi: 10.1016/j.pt.2016.09.009. Epub 2016 Oct 17 [PubMed PMID: 27765440]
Maldjian C, Khanna V, Tandon B, Then M, Yassin M, Adam R, Klein MJ. Lymphatic filariasis disseminating to the upper extremity. Case reports in radiology. 2014:2014():985680. doi: 10.1155/2014/985680. Epub 2014 Feb 19 [PubMed PMID: 24707427]
Level 3 (low-level) evidenceShukla SK, Kusum A, Sharma S, Kandari D. Filariasis presenting as a solitary testicular mass. Tropical parasitology. 2019 Jul-Dec:9(2):124-126. doi: 10.4103/tp.TP_15_19. Epub 2019 Sep 18 [PubMed PMID: 31579667]
Lourens GB, Ferrell DK. Lymphatic Filariasis. The Nursing clinics of North America. 2019 Jun:54(2):181-192. doi: 10.1016/j.cnur.2019.02.007. Epub 2019 Mar 27 [PubMed PMID: 31027660]
Witt C, Ottesen EA. Lymphatic filariasis: an infection of childhood. Tropical medicine & international health : TM & IH. 2001 Aug:6(8):582-606 [PubMed PMID: 11555425]
Chandy A, Thakur AS, Singh MP, Manigauha A. A review of neglected tropical diseases: filariasis. Asian Pacific journal of tropical medicine. 2011 Jul:4(7):581-6. doi: 10.1016/S1995-7645(11)60150-8. Epub [PubMed PMID: 21803313]
Level 3 (low-level) evidenceChakraborty S, Gurusamy M, Zawieja DC, Muthuchamy M. Lymphatic filariasis: perspectives on lymphatic remodeling and contractile dysfunction in filarial disease pathogenesis. Microcirculation (New York, N.Y. : 1994). 2013 Jul:20(5):349-64. doi: 10.1111/micc.12031. Epub [PubMed PMID: 23237232]
Level 3 (low-level) evidenceOrihel TC,Eberhard ML, Zoonotic filariasis. Clinical microbiology reviews. 1998 Apr; [PubMed PMID: 9564568]
Level 3 (low-level) evidenceShenoy RK. Clinical and pathological aspects of filarial lymphedema and its management. The Korean journal of parasitology. 2008 Sep:46(3):119-25. doi: 10.3347/kjp.2008.46.3.119. Epub [PubMed PMID: 18830049]
Mand S, Marfo-Debrekyei Y, Dittrich M, Fischer K, Adjei O, Hoerauf A. Animated documentation of the filaria dance sign (FDS) in bancroftian filariasis. Filaria journal. 2003 Feb 27:2(1):3 [PubMed PMID: 12636874]
Bjerum CM, Ouattara AF, Aboulaye M, Kouadio O, Marius VK, Andersen BJ, Weil GJ, Koudou BG, King CL. Efficacy and Safety of a Single Dose of Ivermectin, Diethylcarbamazine, and Albendazole for Treatment of Lymphatic Filariasis in Côte d'Ivoire: An Open-label Randomized Controlled Trial. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 2020 Oct 23:71(7):e68-e75. doi: 10.1093/cid/ciz1050. Epub [PubMed PMID: 31641754]
Level 1 (high-level) evidenceTaylor MJ,Hoerauf A,Bockarie M, Lymphatic filariasis and onchocerciasis. Lancet (London, England). 2010 Oct 2; [PubMed PMID: 20739055]
Level 3 (low-level) evidenceKalyanasundaram R, Khatri V, Chauhan N. Advances in Vaccine Development for Human Lymphatic Filariasis. Trends in parasitology. 2020 Feb:36(2):195-205. doi: 10.1016/j.pt.2019.11.005. Epub 2019 Dec 19 [PubMed PMID: 31864894]
Level 3 (low-level) evidenceRobinson CG, Lee KR, Thomas VD. The Successful Treatment of Elephantiasis Nostras Verrucosa With Ablative Carbon Dioxide Laser. Journal of cutaneous medicine and surgery. 2018 Nov/Dec:22(6):611-613. doi: 10.1177/1203475418763548. Epub 2018 Mar 8 [PubMed PMID: 29519146]
Stocks ME, Freeman MC, Addiss DG. The Effect of Hygiene-Based Lymphedema Management in Lymphatic Filariasis-Endemic Areas: A Systematic Review and Meta-analysis. PLoS neglected tropical diseases. 2015 Oct:9(10):e0004171. doi: 10.1371/journal.pntd.0004171. Epub 2015 Oct 23 [PubMed PMID: 26496129]
Level 1 (high-level) evidenceGardon J,Gardon-Wendel N,Demanga-Ngangue,Kamgno J,Chippaux JP,Boussinesq M, Serious reactions after mass treatment of onchocerciasis with ivermectin in an area endemic for Loa loa infection. Lancet (London, England). 1997 Jul 5; [PubMed PMID: 9217715]
Level 3 (low-level) evidenceAndersen BJ, Rosa BA, Kupritz J, Meite A, Serge T, Hertz MI, Curtis K, King CL, Mitreva M, Fischer PU, Weil GJ. Systems analysis-based assessment of post-treatment adverse events in lymphatic filariasis. PLoS neglected tropical diseases. 2019 Sep:13(9):e0007697. doi: 10.1371/journal.pntd.0007697. Epub 2019 Sep 26 [PubMed PMID: 31557154]