Introduction
Cupping therapy is a therapeutic technique that utilizes a vacuum force created beneath a small vessel applied onto the skin's surface. This approach focuses on blood and autologous healing substances in a specific area, stimulating metabolic activity, improving immune function, and stabilizing blood biochemistry.[1]
History of Cupping Therapy
Cupping therapy has been a traditional practice dating back to ancient times. This therapy was practiced by the Egyptians and Macedonians around 5500 years ago, and Egyptians later introduced this method to the Greeks.[2] Cupping therapy was documented and endorsed in diverse civilizations, including China and Rome, as well as within the collective traditions (hadiths) of the Prophet Muhammad during the initial 6 centuries of the Common Era. Over time, cupping therapy extended to numerous parts of the world and has been consistently utilized, except in the United States, where it declined in popularity during the late 19th and early 20th centuries. [2]
Cupping has traditionally carried folkloric, cultural, religious, and spiritual significance within various societies. Within certain traditional Muslim communities, adhering to specific ceremonial practices was believed to improve treatment outcomes, resulting in regulations restricting the anatomical regions where cupping could be administered.[3] In traditional Eastern Medicine, cupping therapy was closely associated with acupuncture, whereas in Taoism, it was used to harmonize Qi by balancing Yin (negative energy) and Yang (positive energy).[1] In India, Ayurvedic medicine also incorporates a blood detoxification technique known as Ghati yantra, which bears similarities to wet cupping.[1] In certain less-dominant cultural and religious traditions, shamanic leaders utilized the cupping method to safeguard their communities from illnesses believed to be of demonic origin.[2]
Techniques of Cupping Therapy
Cupping is typically categorized into 2 primary procedures—wet and dry cupping. In both techniques, containers made from various materials are used to create a vacuum over a specific area of the skin. However, suction is applied in a wet cupping procedure to draw small quantities of blood and extracellular fluid from the body, typically after creating minor incisions or superficial skin abrasions, often in significantly smaller amounts than conventional bloodletting practices.[4]
Wet cupping, a traditional procedure, continues to be practiced in various regions, including China, Korea, and parts of Eastern Europe. In regions of the Middle East and Northern Africa, this practice is called Al-Hijamah in Arabic, which can be loosely translated as "restoring the body to its natural state."[1][4][5]
In recent years, cupping practices have evolved, resulting in their classification into 5 primary categories:
-
Technical types: Cupping therapy encompasses a range of technical types, which include dry, wet, flash, and massage cupping types.[4]
-
Power of suction: Cupping therapy can be applied with varying degrees of suction, typically categorized as light, medium, strong, or pulsatile suction.[4]
-
Methods of suction: Cupping therapy can be performed using different methods, such as fire, manual, and electrical vacuum cupping methods.[4]
-
Additional therapies: Cupping therapy can be combined with other therapies, including needle, mona, herbal, magnetic, laser, electrical stimulation, water, and aquatic cupping procedures.[4]
-
Conditions and area-specific: Cupping therapy can be customized to address particular conditions and target-specific areas, including cosmetic, sports-related, orthopedic, abdominal, facial, and gender-specific cupping therapies for females and males.[4]
Although wet and dry cupping techniques remain relevant in contemporary medicine, a meta-analysis of cupping therapy's effectiveness in managing back pain indicated that most studies meeting inclusion criteria primarily focused on dry cupping. This preference is likely attributed to the noninvasive nature of dry cupping than wet cupping. The potential advantages of reduced invasiveness outweighed the additional physiological impact that wet cupping might offer.[6]
Anatomy and Physiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Anatomy and Physiology
Theories Associated With Cupping Therapy
The specific mechanism through which cupping exerts its therapeutic effects remains unidentified. However, several theories have been proposed to elucidate its physiological benefits, as mentioned below.[7]
The pain-gate theory
This theory proposes that the touch, pressure, and vibrational sensations generated during cupping therapy selectively stimulate large nerve fibers. This stimulation leads to the inhibition of pain signal transmission to the brain through the dorsal horn of the spinal cord. The increased stimulation of peripheral nociceptors caused by cupping results in the upregulation of receptor-fiber units, subsequently triggering the activation of large-fiber nerves. These large fiber nerves are responsive to stimuli, and the pumping mechanism used to create suction during cupping may contribute to pain relief.[7]
The diffuse noxious inhibitory controls (DNIC) theory
This theory proposes that pain in one part of the body can be suppressed or overshadowed by pain in a different area. More precisely, DNIC refers to the findings from animal studies that illustrate pain inhibition mediated by the lower brainstem. In humans, this phenomenon is called conditioned pain modulation (CPM). The effective utilization of CPM entails using conditioning to attain a reduced pain response. Cupping therapy has been used in the treatment of idiopathic pain syndromes. However, the precise mechanism through which DNIC operates in cupping therapy remains incompletely understood. Various hypotheses have been proposed, including the potential distraction caused by the sensation of cupping, the initiation of a DNIC response, or the induction of a deoxidation effect.[7]
The reflex zone theory
This theory proposes that specific alterations in distal vascular, muscular, nervous, organ, or connective tissues could be a reflexive response to a proximal constriction of an autonomic nerve within the same or overlapping dermatome. According to this theory, the treatment approach should prioritize addressing the central restriction area rather than exclusively concentrating on the distal regions manifesting symptoms.[7] This concept resembles somato-visceral and somato-somatic reflexes in osteopathic medicine and the utilization of meridians in traditional Eastern medicine.
The release of nitric acid (NO) theory
This theory suggests that cupping therapy may stimulate the increased production of nitric oxide (NO), which controls blood flow, volume, and vasodilation. This theory is supported by the findings from animal studies that have shown an association between the release of NO and acupuncture. Due to the parallel physiological effects observed in both cupping therapy and acupuncture, it is hypothesized that cupping may similarly induce NO-mediated vasodilation and other local physiological responses. As a result, cupping therapy might promote healthy blood circulation and prevent conditions such as atherosclerosis.[7]
The activation of immune system theory
This theory proposes that cupping therapy significantly enhances the body's biochemical and mechanical immune systems. Several studies cited by Al-Bedah et al suggest that cupping therapy can increase the production of various autoimmune modulators while concurrently reducing inflammatory substances. Moreover, it is believed that these positive changes may have lasting effects beyond the duration of the cupping treatments. In addition, cupping is assumed to stimulate the activity of the thymus, support the function of the neuroendocrine system, and bolster the body's antioxidant processes.[7]
The blood detoxification theory
This theory primarily applies to wet cupping. According to this theory, the blood drawn during wet cupping is found to have elevated concentrations of various substances, including uric acid, cholesterol, urea, and triglycerides. Furthermore, the blood obtained through wet cupping is believed to contain higher levels of red blood cells, hemoglobin, hematocrit, viscosity, and mean corpuscular hemoglobin. This theory has been applied in detoxification protocols, particularly for aluminum, mercury, silver, and lead.[7]
Physiological Responses and Therapeutic Mechanisms in Wet and Dry Cupping
In both wet and dry cupping, the application of external suction leads to several physiological responses that contribute to the therapeutic effects of the therapy. These responses involve an increased blood volume, an elevated capillary filtration rate, and the expulsion of filtered and interstitial fluid into the treated area. The collected fluid contains elevated levels of disease-related and disease-causing substances, prostaglandins, and inflammatory mediators.[8]
The increased oncotic pressure in dry cupping is believed to stimulate lymphatic uptake, thereby facilitating the removal of accumulated fluids and waste products from the treated area.[9]
In wet cupping, the scratches made with a scalpel during the procedure lead to a different set of effects. These minor skin incisions stimulate inflammatory cell migration and trigger the release of endogenous opioids, which are natural substances that function as pain relievers and mood enhancers. As previously mentioned, this action contributes to an increase in both innate and acquired immunity, thereby enhancing the body's ability to fight infections and restore immune balance.[1]
Cupping therapy can target numerous anatomical sites, and the choice of these sites depends on the specific ailment or condition under treatment. Cupping is frequently administered to regions with abundant muscle tissue, such as the back, chest, abdomen, and buttocks.[1]
To minimize potential risks and increase the chances of favorable outcomes in cupping therapy, it is advisable to avoid anatomical sites with significant dense hair, limited tissue mass, and insufficient surface area for effective cup placement.[10]
Indications
Cupping is a versatile therapy that benefits overall health and effectively addresses localized and systemic complaints. Dry and wet cupping techniques can be applied for effective musculoskeletal pain relief.[11] However, dry cupping is often preferred in Western settings because it poses significantly lower risks of exposure to biohazardous fluids, making it a safer option for practitioners and patients.
Despite the lower risk, evidence suggests that wet cupping may provide patients with broader benefits.[12] Research indicates that wet cupping can be beneficial for systemic disorders, including conditions related to obesity, hypertension, autoimmune and inflammatory diseases, diabetes mellitus, psychiatric disorders, systemic infections, and skin conditions.[4][10][13]
Contraindications
Considering the contraindications when performing cupping therapy is crucial to ensure the safety and well-being of patients. These contraindications include avoiding areas with deep vein thrombosis, open wounds, or bone fractures. Notably, cupping should not be applied directly over nerves, arteries, veins, varicose veins, skin lesions, body orifices, lymph nodes, eyes, or areas of skin that are inflamed.[4] If the skin is excoriated, oozing, or infected, it is advisable to refrain from cupping, as it may result in an elevation of D-dimer levels, thereby suggesting the possibility of blood coagulation or other adverse effects.[1]
Individuals with cancer, organ failure, hemophilia, or any similar blood disorder, and any implanted electronic medical device, such as a pacemaker, are contraindicated for cupping therapy.[4] Cupping therapy is not recommended for geriatric, pediatric, pregnant, or menstruating patients. Furthermore, patients with elevated serum cholesterol are at higher risk of developing cardiovascular events related to cupping therapy.[1]
Cupping therapy should be avoided in patients who are undergoing anticoagulant treatment. Moreover, individuals with cardiovascular disease and acute infections should exercise caution when considering cupping therapy.[4] In addition, patients with elevated serum cholesterol are at higher risk of developing cupping-related cardiovascular events.[1]
Equipment
Cupping therapy sets are available in diverse configurations, and their characteristics can vary depending on the fabrication material, suction method, and intended application, as listed below.
- Fabrication material: Cupping sets can be crafted from various materials, including glass, plastic, silicone, or bamboo. Specific cupping therapy techniques may necessitate the application of a viscous fluid, such as oil or water-based lubricant, to protect the patient's skin from the cup's edge during the suction process.
- Suction method: Contemporary cupping sets may utilize a vacuum pump to create the suction (manual cupping) or rely on electrical devices (electrical cupping) to regulate the pressure.
- Specific use: Cupping sets can be customized for various therapeutic purposes to address particular ailments or body areas. For instance, cupping sets may be designed for sports-related injuries, facial rejuvenation, lymphatic drainage, or general relaxation.
Moreover, cupping sets may vary in size and shape to accommodate different body areas and patient preferences. Some cupping sets include multiple cup sizes that enable practitioners to customize the treatment based on the patient's requirements. The set may also include a specific suction method, such as manual pumps or electrical devices, to create the necessary suction for the therapy.
After cupping therapy sessions, it is essential to clean the cups thoroughly with soap and water to maintain proper hygiene standards. Consistently sanitizing the cups after each use is crucial in mitigating the risk of infection and cross-contamination.
In the wet cupping technique, prioritizing safety and hygiene is paramount as it involves drawing small amounts of blood from the patient's body. Personal protective equipment (PPE) is advisable to safeguard the patient and the practitioner. Furthermore, choosing disposable cups, vacuum pumps, and surgical blades helps minimize the risk of pathogen transmission and guarantees a sterile, single-use environment.[4]
Preparation
Dry cupping is a simple procedure that typically requires minimal preparation. The primary steps involved in preparing for dry cupping include obtaining written and verbal informed consent from the patient, ensuring that only the necessary amount of skin is exposed for treatment while maintaining the patient's dignity, privacy, and safety, and confirming that the skin is clean and dry before commencing the cupping session.
In addition to the precautions mentioned earlier, wet cupping requires additional measures due to the potential exposure to biohazardous substances. To ensure the safety of the patient and the practitioner, it is imperative that the practitioner and all personnel involved in the procedure wear appropriate PPE.
Although wet cupping can be categorized as a clean procedure, it is advisable to approach it cautiously and implement necessary measures to ensure patient safety and prevent potential complications. The below-mentioned safety protocols are recommended to be observed while performing the procedure.
- Skin preparation: Betadine should be used for prepping the skin instead of alcohol.
- Disposable equipment: Disposable surgical blades and cups should be used for every patient.
- PPE: All individuals participating in the procedure, including the cupping therapist and assistants, should wear appropriate PPE, such as sterile gloves, gowns, and drapes.
- Waste disposal: Cups, blades, and other disposable items used during the procedure should be appropriately disposed of in appropriate sharps and biohazard waste containers.
- Chaperone presence: A chaperone in the treatment room is recommended, especially when attending to patients unfamiliar with the procedure.
Technique or Treatment
Dry cupping is a simple, 1-step technique in which the cups are directly applied onto the skin's surface to generate suction without requiring additional procedures.
In contrast, traditional wet cupping follows a 2-step process that commences with superficial skin scarification, where the skin is gently scratched or incised using a scalpel or another sterile instrument. This step is followed by applying the cups to the scarified area, allowing the suction to draw out a small amount of blood and interstitial fluid.
Al-Hijamah, a more complex form of wet cupping, involves a 3-step technique. This process commences with the application of cups to the skin to generate suction, followed by superficial scarification, which is similar to the traditional wet cupping technique. However, in Al-Hijamah, an additional round of cupping is carried out following the initial scarification. Honey is frequently utilized during Al-Hijamah to safeguard the patient's skin from the cup's edge and to improve the vacuum seal. As honey is recognized for its healing properties, it is believed to support skin recovery after the procedure potentially.[1]
Researchers recommend that cups should be left on the skin for a maximum of 5 to 10 minutes during a cupping therapy session.[6] This duration is deemed adequate to attain the intended therapeutic effects without causing unnecessary discomfort or adverse reactions.
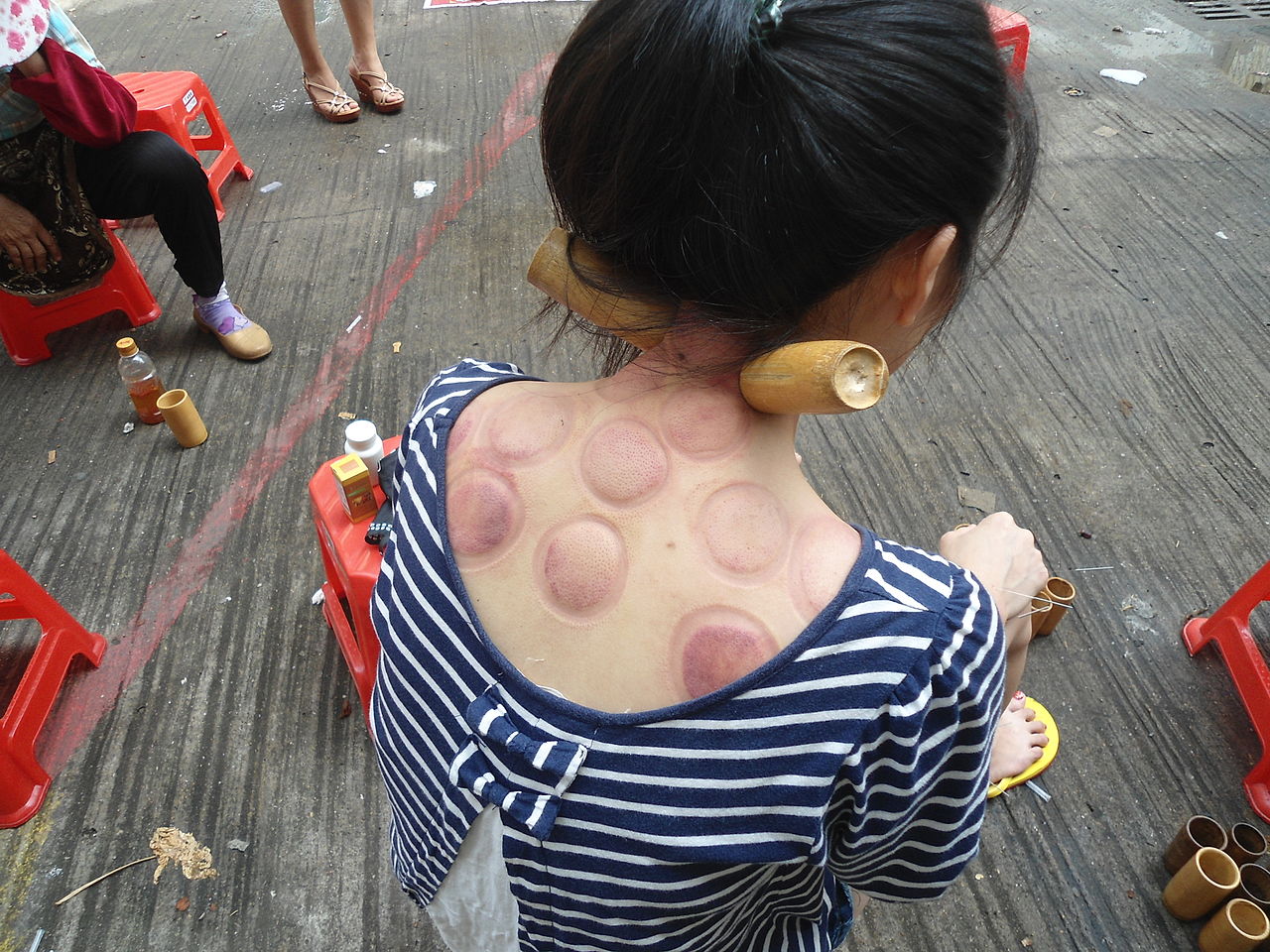
After a cupping therapy session, patients may notice residual ecchymosis on the skin, commonly referred to as cupping marks. These marks result from the suction applied during cupping and manifest as circular or oval-shaped areas of skin discoloration. The color of the marks may vary, ranging from light red or pink to dark purple, depending on the individual's skin type and the treatment's intensity. The cupping marks typically fade over time and gradually disappear within 1 to 10 days after the treatment.[6]
Suction is generated through any 1 of the 3 pumping methods mentioned below.
- Manual pumping: In this method, the cups are compressed by hand or with a mechanical device and are subsequently and swiftly placed onto the skin. The pressure release creates a vacuum, pulling the skin into the cup and creating the desired suction effect.
- Electrical pumping: This method involves using a motorized pump or vacuum device to create a suction. The pump generates negative pressure inside the cup, enabling it to adhere to the skin and yield the therapeutic effects of the treatment.
- Fire cupping: In this method, a flame is briefly ignited using methylated spirits inside the cup to eliminate the air. After extinguishing the flame, the cup is immediately placed onto the skin (see Image. Fire Cupping). As the air inside the cup cools and contracts, it generates a partial vacuum that draws the skin into the mouth of the cup, producing the desired suction effect.[1][6]
Complications
Cupping therapy is generally considered a safe procedure, with occasional reports of mild-to-moderate adverse reactions. These potential adverse effects can be categorized as preventable or nonpreventable.
Preventable adverse events of cupping therapy include scarring, burns, bullae, abscesses, blood-borne and skin infections, pruritus, anemia, and panniculitis. These issues are often attributed to instrumentation or sterile technique errors.
Nonpreventable adverse events of cupping therapy include headaches, dizziness, fatigue, vasovagal syncope, nausea, insomnia, and the Koebner phenomenon, which is described as the appearance of new skin lesions resulting from the treatment. These adverse events are categorized as nonpreventable because they largely depend on the patient's response.[4][14]
Infection, vasovagal syncope, and scarring are more frequently associated with wet cupping. Common adverse effects of dry cupping include localized erythema and ecchymosis at the cupping site(s). When using fire suction in dry cupping, there is an elevated risk of burns.[6]
Clinical Significance
Cupping therapy has demonstrated notable advantages in addressing various forms of pain, particularly musculoskeletal pain, migraines, and tension headaches.[1] Studies indicate that wet cupping reduces average headache severity by 66% and decreases headache days by 12.6 per month.[15]
Alongside alleviating headaches, cupping therapy has demonstrated effectiveness in relieving arthritic, neuritic, and musculoskeletal pain that affects the trunk, extremities, and neck.[6][10] Cupping therapy has also been used to manage respiratory issues such as cough and dyspnea, as well as to address skin conditions such as acne.[10]
A German study showcased the benefits of traditional wet cupping in treating carpal tunnel syndrome. Furthermore, research based on traditional Persian medicine yielded promising results in managing B-thalassemia and other autoimmune diseases.[3]
In summary, the evidence indicates that both dry and wet cupping techniques can offer substantial benefits in pain management, with potential advantages varying depending on the pain condition being addressed. Dry cupping has exhibited efficacy in managing generalized pain conditions, whereas wet cupping has demonstrated the most significant benefits in alleviating inflammatory-related pain conditions, such as herpes zoster infection.
Cupping therapy is currently regarded as complementary rather than a substitute for conventional medical treatments. Despite its promise in certain areas, healthcare professionals should approach cupping therapy cautiously and be mindful that the evidence supporting its effectiveness for most medical disorders remains limited.
Furthermore, healthcare professionals should be attentive to potential misconceptions regarding cupping marks. The ecchymosis resulting from the cupping therapy can occasionally resemble bruises from physical abuse. Therefore, it is crucial for healthcare providers to distinguish these marks from indications of abuse and to enhance their competence about the anticipated adverse effects of cupping therapy.
Enhancing Healthcare Team Outcomes
Detailed infection control measures are crucial to ensure the safety and effectiveness of cupping therapy. Healthcare practitioners should adhere to the below-mentioned steps to prevent infections.
-
Hand washing and use of PPE: Practitioners should wash their hands thoroughly before and after each cupping session. Furthermore, it is essential to wear suitable PPE, including gloves, masks, protective eyewear, and gowns, to prevent the transmission of infections.
-
Disinfection of treatment area: Beds or chairs used during cupping therapy should undergo comprehensive disinfection to uphold a sterile environment for patients.
-
Use of disposable equipment: Opting for disposable equipment for cups, surgical blades, and vacuum pumps is advisable, whenever possible, to reduce the risk of cross-contamination and infections.
Before the cupping session, gathering a comprehensive medical history from the patient is essential to minimize complications and adverse effects. Creating a checklist of established contraindications for cupping therapy can facilitate the initial assessment and ensure that suitable candidates undergo treatment. A comprehensive physical examination of patients should also be conducted to assess for any underlying conditions that necessitate conventional therapies or may contraindicate cupping treatment.
Cupping therapy boasts a rich history of utilization in Eastern and Western medicine, with a lineage extending over 5,000 years. Although this therapy continues to be traditionally practiced in certain regions, it has also found a place in the arsenal of various healthcare professionals. This includes allopathic and osteopathic physicians, physical therapists, sports trainers, massage therapists, chiropractors, European osteopaths, and naturopaths.
By adhering to rigorous infection control measures and considering individual patient factors, cupping therapy can emerge as a valuable and safe therapeutic modality for addressing various health disorders and fostering the overall well-being of patients.
Media
(Click Image to Enlarge)
References
Ghods R, Sayfouri N, Ayati MH. Anatomical Features of the Interscapular Area Where Wet Cupping Therapy Is Done and Its Possible Relation to Acupuncture Meridians. Journal of acupuncture and meridian studies. 2016 Dec:9(6):290-296. doi: 10.1016/j.jams.2016.06.004. Epub 2016 Sep 15 [PubMed PMID: 28010830]
Qureshi NA, Ali GI, Abushanab TS, El-Olemy AT, Alqaed MS, El-Subai IS, Al-Bedah AMN. History of cupping (Hijama): a narrative review of literature. Journal of integrative medicine. 2017 May:15(3):172-181. doi: 10.1016/S2095-4964(17)60339-X. Epub [PubMed PMID: 28494847]
Level 3 (low-level) evidenceEl-Shanshory M, Hablas NM, Shebl Y, Fakhreldin AR, Attia M, Almaramhy HH, Baghdadi H, Ayat M, Albeihany A, El-Dardear A, Ibrahim HA, Mahmoud HS, Nabo MMH, El Sayed SM. Al-hijamah (wet cupping therapy of prophetic medicine) significantly and safely reduces iron overload and oxidative stress in thalassemic children: a novel pilot study. Journal of blood medicine. 2018:9():241-251. doi: 10.2147/JBM.S170523. Epub 2018 Dec 14 [PubMed PMID: 30588142]
Level 3 (low-level) evidenceAboushanab TS, AlSanad S. Cupping Therapy: An Overview from a Modern Medicine Perspective. Journal of acupuncture and meridian studies. 2018 Jun:11(3):83-87. doi: 10.1016/j.jams.2018.02.001. Epub 2018 Feb 7 [PubMed PMID: 29436369]
Level 3 (low-level) evidenceKim S, Lee SH, Kim MR, Kim EJ, Hwang DS, Lee J, Shin JS, Ha IH, Lee YJ. Is cupping therapy effective in patients with neck pain? A systematic review and meta-analysis. BMJ open. 2018 Nov 5:8(11):e021070. doi: 10.1136/bmjopen-2017-021070. Epub 2018 Nov 5 [PubMed PMID: 30397006]
Level 1 (high-level) evidenceMoura CC, Chaves ÉCL, Cardoso ACLR, Nogueira DA, Corrêa HP, Chianca TCM. Cupping therapy and chronic back pain: systematic review and meta-analysis. Revista latino-americana de enfermagem. 2018 Nov 14:26():e3094. doi: 10.1590/1518-8345.2888.3094. Epub 2018 Nov 14 [PubMed PMID: 30462793]
Level 1 (high-level) evidenceAl-Bedah AMN, Elsubai IS, Qureshi NA, Aboushanab TS, Ali GIM, El-Olemy AT, Khalil AAH, Khalil MKM, Alqaed MS. The medical perspective of cupping therapy: Effects and mechanisms of action. Journal of traditional and complementary medicine. 2019 Apr:9(2):90-97. doi: 10.1016/j.jtcme.2018.03.003. Epub 2018 Apr 30 [PubMed PMID: 30963043]
Level 3 (low-level) evidenceObeid AM, Qari FA, Aljaouni SK, Rohaiem S, Elsayed AA, Alsayyad MM, Okmi EA. The effect of wet-cupping therapy (hijama) in modulating autoimmune activity of Hashimoto's thyroiditis: A pilot controlled study. Saudi medical journal. 2022 Jan:43(1):45-52. doi: 10.15537/smj.2022.43.1.20210755. Epub [PubMed PMID: 35022283]
Level 3 (low-level) evidenceOzdowski L, Gupta V. Physiology, Lymphatic System. StatPearls. 2024 Jan:(): [PubMed PMID: 32491765]
Nimrouzi M, Mahbodi A, Jaladat AM, Sadeghfard A, Zarshenas MM. Hijamat in traditional Persian medicine: risks and benefits. Journal of evidence-based complementary & alternative medicine. 2014 Apr:19(2):128-36. doi: 10.1177/2156587214524578. Epub 2014 Feb 25 [PubMed PMID: 24647093]
Shen WC, Jan YK, Liau BY, Lin Q, Wang S, Tai CC, Lung CW. Effectiveness of self-management of dry and wet cupping therapy for low back pain: A systematic review and meta-analysis. Medicine. 2022 Dec 23:101(51):e32325. doi: 10.1097/MD.0000000000032325. Epub [PubMed PMID: 36595746]
Level 1 (high-level) evidenceWood S, Fryer G, Tan LLF, Cleary C. Dry cupping for musculoskeletal pain and range of motion: A systematic review and meta-analysis. Journal of bodywork and movement therapies. 2020 Oct:24(4):503-518. doi: 10.1016/j.jbmt.2020.06.024. Epub 2020 Jul 30 [PubMed PMID: 33218554]
Level 1 (high-level) evidenceKang D, Shin WC, Kim T, Kim S, Kim H, Cho JH, Song MY, Chung WS. Systematic review and meta-analysis of the anti-obesity effect of cupping therapy. Medicine. 2023 Jun 16:102(24):e34039. doi: 10.1097/MD.0000000000034039. Epub [PubMed PMID: 37327262]
Level 1 (high-level) evidenceRehman A, Ul-Ain Baloch N, Awais M. Practice of cupping (Hijama) and the risk of bloodborne infections. American journal of infection control. 2014 Oct:42(10):1139. doi: 10.1016/j.ajic.2014.06.031. Epub [PubMed PMID: 25278416]
Level 3 (low-level) evidenceAhmadi A, Schwebel DC, Rezaei M. The efficacy of wet-cupping in the treatment of tension and migraine headache. The American journal of Chinese medicine. 2008:36(1):37-44 [PubMed PMID: 18306448]