Introduction
Skeletal scintigraphy, commonly referred to as a bone scan (BS), is a valuable and versatile nuclear medicine tool. The examination is most commonly performed using the radiotracer Technetium-99m (Tc99m) complexed to a diphosphonate, either methylene diphosphonate (MDP) forming Tc99m-MDP or hydroxydiphosphonate (HDP) forming Tc99m-HDP. Tc99m is the most common radionuclide used in nuclear medicine for labeling because it is relatively inexpensive and has favorable characteristics for imaging such as good spatial resolution, an ideal photopeak (140 keV) for gamma cameras and possessing a relatively short half-life (6 hours) that allows adequate time for image acquisition without excessive radiation dose to patients. The Tc99m-phosphonates first entered practice in 1971 by Subramanian and colleagues with several subsequent variations produced until the development of Tc 99m-MDP in 1975, which remains the dominant radiotracer in skeletal scintigraphy.[1] Both MDP and HDP serve as phosphate analogs which complex with the crystalline hydroxyapatite in the mineral phase of bone by a process called chemisorption.[2] Tc99m phosphonates localize to bone in proportion to osteoblastic activity as seen at sites of bony remodeling and, to a lesser extent, localizes in proportion to blood flow and its delivery of the radiotracer. Thus, increased radiotracer uptake occurs with multiple pathologic processes such as fractures, infection, malignant disease and less commonly encountered osseous diseases like Paget disease, fibrous dysplasia, osteoid osteoma, and complex regional pain syndrome. The specificity of skeletal scintigraphy, therefore, relies heavily on an appropriate clinical history and correlation with other imaging modalities in conjunction with a thorough assessment of the radiotracer uptake pattern: mono-ostotic versus polyostotic, axial versus appendicular, peri-articular versus metaphyseal or diaphyseal, focal versus fusiform or linear.
There has been a relatively recent re-emergence of fluorine-18 sodium fluoride (F18-NaF) positron emission tomography (PET) for metabolic bone imaging, secondary to temporary shortages of Tc99m and the proliferation of PET-CT technology. A calcium analog, F18-NaF was introduced in 1963, and its 511 keV photons could be imaged with general-purpose rectilinear scanners or early positron detectors.[3] Given the relatively short half-life of fluorine-18 (110 minutes) and its production via cyclotron, F18-NaF was not widely available. This, along with the introduction of Tc99m generators, the phosphate compounds, and gamma cameras, relegated F18-NaF to relative obscurity for the next 4 decades.
The advantages of modern F18-NaF PET-CT over the Tc99m-phosphonates BS include increased spatial resolution, improved target to background ratio, and increased sensitivity. Disadvantages include higher cost, slightly higher radiation dose, and potentially higher false positive rate due to increased uptake at sites of degenerative changes.[4]
Procedures
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Procedures
Skeletal scintigraphy starts with the intravenous injection of Tc99m-MDP followed by imaging at multiple time points, or phases. The adult dose of Tc99m is 10 to 30 millicuries (mCi) or 370 to 1110 megabecquerels (MBq). The dose for children under 5 years is 0.2 to 0.3 mCi per kg or 7 to 11 MBq per kg. Protocols exist with as few as one or as many as four phases of imaging: flow phase, blood pool phase, delayed phase, and 4th phase. The 4th phase, acquired 24-hours after radiotracer injection, is not commonly performed but can be helpful in patients with peripheral vascular disease and concern for osteomyelitis.[5] The flow phase is a radionuclide angiogram to assess for increased (and less commonly decreased) arterial flow to the area of concern and is obtained for 60 to 90 seconds, immediately after injection. The blood pool phase images are obtained immediately after the flow phase and extends out to 10 minutes following injection. This portion of the exam assesses for hyperemia manifest as increased soft tissue activity due to extravasation of radiotracer. The delayed phase imaging is performed 2 to 6 hours after injection and reflects the rate of bone turnover.[6] Three phase studies are most typically used to evaluate for osteomyelitis, joint prosthesis infection versus loosening, and complex regional pain syndrome. The remaining bone scan indications are imaged primarily utilizing a single, delayed-phase-only protocol. The rest of this article focuses primarily on the single-phase bone scan. Please refer to the dedicated Three Phase Bone Scan (TPBS) StatPearls article for more information on that use of bone scintigraphy.
Delayed-phase images are typically obtained as anterior and posterior projections of either the whole body and/or using spot images. Whole body images are helpful for non-focal complaints (i.e., concern for bony metastases, diffuse arthralgia, or elevated alkaline phosphatase of indeterminate etiology) while spot images are preferred for focal issues (rule out tibial stress fracture, unexplained rib pain or assess an indeterminate sclerotic femur lesion seen on x-ray). Spot images are smaller, field-of-view acquisitions that have the advantage of better spatial resolution and may be obtained in multiple projections (anterior/posterior, lateral, anterior/posterior oblique) to assist in anatomic localization of any abnormal radiotracer uptake. If anatomic localization is inadequate on spot images or is in an area of complex anatomy, a single-photon emission computed tomography (SPECT) can be performed with or without a conventional computed tomography (CT), referred to as a SPECT/CT. This allows the fusion of the gamma camera-generated images from the Tc99m-MDP SPECT with the conventional CT images for precise anatomic localization.
Indications
Skeletal scintigraphy has a wide variety of indications.
Most Common
- Detection or follow-up of osseous metastases
- Detection of radiographically occult injury
- Evaluating for the presence of osteomyelitis
- Assessing for prosthetic hardware infection or loosening
Less Common
- Evaluating a primary bone lesion
- Evaluating for avascular necrosis/bone infarcts
- Assessing bone graft viability
- Diagnosis of complex regional pain syndrome
- Screening for child abuse
- Determining the distribution of osteoblastic activity in preparation of radionuclide therapy for bone metastases
- Evaluating arthritides
- Investigating indeterminate radiographic, laboratory, or clinical findings that suggest skeletal involvement [7]
Normal and Critical Findings
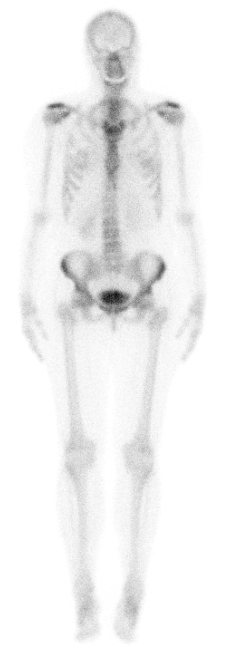
An understanding of the normal anatomic distribution of Tc99m-MDP is important for interpreting skeletal scintigraphy. Symmetric uptake should be seen throughout the osseous structures of a healthy adult. In children, additional intense uptake is present in the physes of the long bones, which represent the normal growth centers. Common areas of benign increased radiotracer accumulation are present at the acromioclavicular joints, sternoclavicular joints, sternomanubrial junction, sacroiliac joints, and pubic symphysis as well as in articular surfaces of the shoulders, hips, knees, ankles, and feet. This is likely due to the constant bony remodeling of the weight-bearing surfaces of the joints and the propensity of degenerative changes in these areas. Also, primarily in adult patients, focal increased uptake is frequently seen in the maxillary and mandibular regions due to underlying dental disease which causes reactive osteogenesis. Similarly, uptake can be present in the nasopharyngeal region of the facial bones in individuals with chronic sinus disease.
Extraosseous activity is seen in the kidneys and bladder due to the normal renal excretion of T99m-MDP. If the kidneys and bladder are not seen, this should raise suspicion of the so-called “superscan.” A superscan implies diffusely increased osseous uptake due to metastatic disease (most commonly breast or prostate cancer) or metabolic bone disease which is so intense that little or no renal excretion of the radiotracer occurs.[8]
Critical Findings
- Detection of osseous metastatic disease: most frequently occurring in the axial and proximal appendicular skeleton corresponding with sites of red marrow
- Detection of stress fracture: most commonly seen in lower body such as tibia, metatarsals and femoral necks, a site particularly critical due to the risk of progression to a displaced fracture
- Detection of osteomyelitis or hardware infection
- Detection of occult fractures in evaluation for child abuse (generally in children older than 1 year): typically seen in ribs and extremities, though it should be noted that bone scintigraphy has a low sensitivity for detection of pediatric skull fractures and classic metaphyseal corner fractures [9]
- Detection of avascular necrosis: history of sickle cell disease or chronic steroid use should raise suspicion for this entity
- Detection of incidental soft tissue uptake: may represent occult malignancy such breast cancer, malignant pleural effusion, soft tissue sarcoma, or metastatic disease in the liver
- Identification of the presence of kidneys on every bone scan; if the kidneys are not seen, a superscan should be suspected
Interfering Factors
The primary interfering factor in skeletal scintigraphy is poor renal function. Adequate evaluation of a bone scan requires clearance of the radiotracer from the soft tissues by the kidneys so that the image produced is composed mostly of gamma rays originating from Tc99m-MDP complexed with the hydroxyapatite of bone. If the kidneys are not functioning properly, the visualization of bone is limited by overlying extraosseous activity in the soft tissues which decreases target-to-background. This factor might be mitigated by obtaining a 24-hour delayed acquisition, often referred to as the fourth phase, which gives the kidneys more time to clear non-osseous uptake. This technique suffers from the limitation of T99m having a half-life of 6 hours which leaves only 6.25% of the initial activity of T99m for imaging at 24 hours. Due to similar reasons, patient dehydration can impede renal clearance of activity from the soft tissues. Thus, it is beneficial to have patients orally hydrate during the 2 to 6 hours between injection of the radiotracer and acquisition of the delayed images.
A second interfering factor in skeletal scintigraphy is the potential for poor labeling of Tc99m with MDP. Poor labeling results in unbound Tc99m-pertechnetate, commonly referred to as “free technetium” or “free tech.” Free technetium will localize to the salivary glands, thyroid, and stomach which may confound interpretation. This potential problem exists with all Tc99m labeled radiotracers and is not specific to skeletal scintigraphy.
A third interfering factor in skeletal scintigraphy is the “flare phenomenon.” This is a pattern of uptake where the osseous metastatic disease may appear worsened in the 2 to 6 months following chemotherapy. New lesions may be seen while pre-existing lesions can appear larger or more intense.[10] This change likely represents increased bone turnover as the bone heals the area of prior metastatic disease to include sclerosis of prior occult lytic lesions. This pseudo-progression will resolve on follow-up bone scans, confirming the response to therapy.
Complications
Skeletal scintigraphy relies on intravenous administration. Most of the common complications of this examination originate from a failure of proper injection.
Extravasation of the injected Tc99m-MDP into the soft tissues causes the following three problems:
- Minimal radiotracer reaches the bones and thus severely degrades visibility of osteoblastic pathology.
- The extravasated radiotracer is taken up by the lymphatic system which complicates same-day re-injection due to retention in lymph nodes which may obscure underlying bone pathology.
- The intense tracer uptake coming from the injection site degrades the image of the skeleton due to the image being derived from extraneous photons arising from the site of extravasation.
Arterial injection may also rarely occur which produces the "glove" phenomenon. The glove phenomenon is characterized by significant asymmetric uptake extending from the arterial injection site down into the fingers.[11]
Patient Safety and Education
Skeletal scintigraphy uses ionizing radiation in the form of gamma rays produced from the radiotracer Tc99m. The effective whole body dose of radiation for adults from this examination is 0.0057 millisieverts (mSv) per MBq which translates to approximately 4 mSv for a 20 mCi dose of Tc99m-MDP.[4] The effective whole body dose for children under 5 is 0.025 mSv per MBq. For reference, the average annual background radiation dose to an adult is approximately 3 mSv and it is considered acceptable for medical staff to receive up to 5 mSv annually from occupational exposures.
A small amount of Tc99m-pertechnetate is secreted in breast milk, but the estimated fetal dose is below 1 mSv (100 mrem). [12] Therefore breastfeeding does not need to be discontinued, although many providers do counsel that breastfeeding be avoided for 12-24 hours due to patient concerns and older guidelines recommending the same.[13] [12]
Clinical Significance
Skeletal scintigraphy is a versatile medical imaging tool, providing a highly sensitive examination for bone pathology, particularly in the detection of stress injury and radiographically occult fractures. A negative bone scan at 72 hours excludes a fracture in the appendicular skeleton with a sensitivity of 95% to 100%. Note that healing fractures may display increased uptake long after the initial trauma, with 60 to 80% of fractures returning to normal on bone scan in one year and 95% of fractures returning to normal by 3 years.[14] The detection of osseous stress injury is important because the patient’s activity should be modified to prevent completion of the fracture.
A bone scan can be very helpful in the evaluation of osteomyelitis. The exam is very sensitive, up to 94%; this results in an excellent negative predictive value.[15] In the setting of normal bone, the exam can also demonstrate similar specificity; however, the presence of an underlying intrinsic lesion, hardware, fracture, or recent surgery can markedly decrease specificity to as low as 34%, necessitating further imaging when the examination is positive.[16] Further imaging options in nuclear medicine include F18-FDG PET/CT or radiolabeled white blood cell (WBC) scan using In-111 or Tc99m-HMPAO labeled WBCs.
The sensitivity of bone scan for metastatic disease varies for each primary tumor. The specifics of sensitivity and specificity for each type of malignancy is beyond the scope of this article; however, the study is most accurate in the setting of osteoblastic metastases and least accurate with malignancies that typically produce osteolytic bone lesions. Given such, the common malignancies for which bone scintigraphy is known to have a high sensitivity for identifying bone metastases include breast, prostate, and lung cancer. The common malignancies for which bone scintigraphy is known to have a low sensitivity for detection of osseous metastases include multiple myeloma, renal cell carcinoma, and thyroid carcinoma.
Media
(Click Image to Enlarge)
References
Subramanian G, McAfee JG. A new complex of 99mTc for skeletal imaging. Radiology. 1971 Apr:99(1):192-6 [PubMed PMID: 5548678]
Level 3 (low-level) evidenceSubramanian G, McAfee JG, Blair RJ, Kallfelz FA, Thomas FD. Technetium-99m-methylene diphosphonate--a superior agent for skeletal imaging: comparison with other technetium complexes. Journal of nuclear medicine : official publication, Society of Nuclear Medicine. 1975 Aug:16(8):744-55 [PubMed PMID: 170385]
Level 3 (low-level) evidenceBridges RL, Wiley CR, Christian JC, Strohm AP. An introduction to Na(18)F bone scintigraphy: basic principles, advanced imaging concepts, and case examples. Journal of nuclear medicine technology. 2007 Jun:35(2):64-76; quiz 78-9 [PubMed PMID: 17496010]
Level 3 (low-level) evidenceGrant FD, Fahey FH, Packard AB, Davis RT, Alavi A, Treves ST. Skeletal PET with 18F-fluoride: applying new technology to an old tracer. Journal of nuclear medicine : official publication, Society of Nuclear Medicine. 2008 Jan:49(1):68-78 [PubMed PMID: 18077529]
Alazraki N, Dries D, Datz F, Lawrence P, Greenberg E, Taylor A Jr. Value of a 24-hour image (four-phase bone scan) in assessing osteomyelitis in patients with peripheral vascular disease. Journal of nuclear medicine : official publication, Society of Nuclear Medicine. 1985 Jul:26(7):711-7 [PubMed PMID: 3159858]
Love C, Din AS, Tomas MB, Kalapparambath TP, Palestro CJ. Radionuclide bone imaging: an illustrative review. Radiographics : a review publication of the Radiological Society of North America, Inc. 2003 Mar-Apr:23(2):341-58 [PubMed PMID: 12640151]
Van den Wyngaert T, Strobel K, Kampen WU, Kuwert T, van der Bruggen W, Mohan HK, Gnanasegaran G, Delgado-Bolton R, Weber WA, Beheshti M, Langsteger W, Giammarile F, Mottaghy FM, Paycha F, EANM Bone & Joint Committee and the Oncology Committee. The EANM practice guidelines for bone scintigraphy. European journal of nuclear medicine and molecular imaging. 2016 Aug:43(9):1723-38. doi: 10.1007/s00259-016-3415-4. Epub 2016 Jun 4 [PubMed PMID: 27262701]
Level 1 (high-level) evidenceBuckley O, O'Keeffe S, Geoghegan T, Lyburn ID, Munk PL, Worsley D, Torreggiani WC. 99mTc bone scintigraphy superscans: a review. Nuclear medicine communications. 2007 Jul:28(7):521-7 [PubMed PMID: 17538392]
Howard JL, Barron BJ, Smith GG. Bone scintigraphy in the evaluation of extraskeletal injuries from child abuse. Radiographics : a review publication of the Radiological Society of North America, Inc. 1990 Jan:10(1):67-81 [PubMed PMID: 2296698]
Pollen JJ, Witztum KF, Ashburn WL. The flare phenomenon on radionuclide bone scan in metastatic prostate cancer. AJR. American journal of roentgenology. 1984 Apr:142(4):773-6 [PubMed PMID: 6230903]
Level 3 (low-level) evidenceShih WJ, Wienrzbinski B, Ryo UY. Abnormally increased uptake in the palm and the thumb as the result of a bone imaging agent injection into the radial artery. Clinical nuclear medicine. 2000 Jul:25(7):539-40 [PubMed PMID: 10885697]
Level 3 (low-level) evidenceStabin MG, Breitz HB. Breast milk excretion of radiopharmaceuticals: mechanisms, findings, and radiation dosimetry. Journal of nuclear medicine : official publication, Society of Nuclear Medicine. 2000 May:41(5):863-73 [PubMed PMID: 10809203]
Ahlgren L, Ivarsson S, Johansson L, Mattsson S, Nosslin B. Excretion of radionuclides in human breast milk after the administration of radiopharmaceuticals. Journal of nuclear medicine : official publication, Society of Nuclear Medicine. 1985 Sep:26(9):1085-90 [PubMed PMID: 4032049]
Matin P. The appearance of bone scans following fractures, including immediate and long-term studies. Journal of nuclear medicine : official publication, Society of Nuclear Medicine. 1979 Dec:20(12):1227-31 [PubMed PMID: 536788]
Level 3 (low-level) evidenceChristian S, Kraas J, Conway WF. Musculoskeletal infections. Seminars in roentgenology. 2007 Apr:42(2):92-101 [PubMed PMID: 17394922]
El-Maghraby TA, Moustafa HM, Pauwels EK. Nuclear medicine methods for evaluation of skeletal infection among other diagnostic modalities. The quarterly journal of nuclear medicine and molecular imaging : official publication of the Italian Association of Nuclear Medicine (AIMN) [and] the International Association of Radiopharmacology (IAR), [and] Section of the Society of.... 2006 Sep:50(3):167-92 [PubMed PMID: 16868532]