Continuing Education Activity
Piedra is a superficial fungal infection of hair shafts, which presents with small nodules stuck-on to the shaft. Black piedra, caused by Piedraia hortae, is characterized by black-colored nodules and is common in the tropics, especially in individuals with long hair and poor scalp hygiene. This activity shall discuss the etiology, clinical presentation, differential diagnosis, bed-side evaluation methods, and treatment options for this condition, pertinent to the interprofessional healthcare team.
Objectives:
- Identify the etiology of black piedra.
- Review the important aspects of a patient's history and physical evaluation.
- Identify the treatment and management options available for black piedra.
- Outline interprofessional team strategies for improving care coordination and communication to advance the quick diagnosis, and optimal management of patients with black piedra to improve outcomes.
Introduction
Black piedra is a fungal infection of the hair shafts. It is also known as Trichomycosis nodosa. The fungal elements are attached to the hair shaft to form nodules along the hair shaft. It predominantly affects scalp hair, although involvement of the beard, mustache, and pubic hairs is also known. Black piedra is common in hot and humid countries like South American countries and Southeast Asian countries.[1] Black piedra is rare in Europe. It can affect humans as well as other primates.
Etiology
Black piedra results from a particular fungal species called Piedraia hortae. This fungal disease results from poor personal hygiene. It is commonly seen in people having long hair and with the excessive use of different hair oils. Practices like prolonged wearing of veils or tight hats may contribute to its development and progression. There are also reports of sexual transmission. The incidence of fungal infections is on the rise due to the opportunistic nature of the fungal organisms and the prevalence of immunodeficient conditions.[2]
Epidemiology
Black piedra is an infection of tropical and subtropical regions. However, due to worldwide travel, it may also occur sporadically in other regions, even in Europe. The exact mode of spread of piedra is not clear. The use of an infected comb or sharing of pillows and bedsheets may be the possible factors for transmission.[3] Though piedra can occur at any age, its incidence usually drops off after middle age.[4] The occurrence of both black piedra and white piedra simultaneously in a patient is extremely rare.[5][6]
Pathophysiology
The soil appears to be the primary source of infection in black piedra, although P. hortae, has also been traced in stagnant water and crops. P. hortae can produce sexual spores in the parasitic phase, which is a unique feature of this fungus among other pathogenic fungi.
Hairs with black piedra isolated from Brazilian Indians were investigated by studying serial sections with light and transmission electron microscopy.[7] P. hortae showed strong keratolytic activity; it was able to destroy both the cuticle and the hair cortex. Two well-defined types of cortex digestion appeared. The first one was parallel to the axis of hair and was produced by fungal cells that grew separating the external layers of the outer cortex. The second type was produced by active boring hyphae, forming channels as they penetrated vertical to the axis of hair.
In vivo and in vitro studies using electron microscopy and x-ray microanalysis have shown elements like phosphorus, sulfur, and calcium in the nodules that develop on hair and in culture colonies. These elements are part of the extracellular material that compacts the pseudoparenchymatous organization of the fungus. Their presence is due to the capacity of melanin-like pigments to sequester ions. They may form part of the mucopolysaccharides that constitute the extracellular material. Researchers detected contaminants such as aluminum, silicon, and iron on the surface of the nodule; these have links to the residual molecules produced during the breakdown of the cuticular keratin.[8]
In P. hortae, the cementing extracellular material that holds the nodule together is probably the main factor responsible for preserving the fungus against environmental attack and desiccation. Moreover, this compact organization can also impair successful treatment, which may explain why an untreated black piedra may run a very chronic course.
Histopathology
In histological sections or 10% potassium hydroxide (KOH) mounts, the nodules are observed to be made up of closely packed brown hyphae held in a mass by a viscous or cement-like substance. At the edges of the nodules, regularly aligned hyphae and arthroconidia, 4 to 8 microns in diameter, can be seen. In the thicker parts, club-shaped asci containing elongated ascospores may be formed. A crushed nodule reveals asci containing two to eight single-celled fusiform ascospores with a single polar filament at each end.
History and Physical
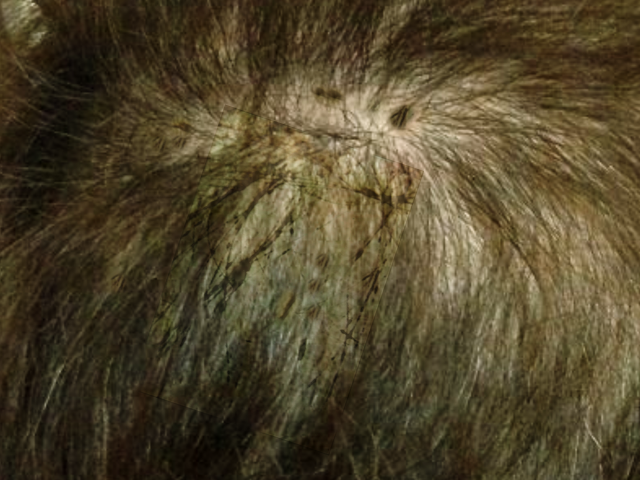
Black piedra is asymptomatic, except for the unsightly nodes visible on hair strands. On examination, the hair shaft shows firmly attached brown-black nodules, which are less than 1mm in size. These nodules are gritty on palpation. The nodules are usually multiple and vary in size from microscopic to 1 mm or more in diameter. They are oval or elongated in shape with their thickness tapering from one end to the other or from the middle to the edge. They are composed of a compact cellular substance that surrounds the hair shaft. Hair shafts affected by these nodules become weak and often break at the point of infection. The disease is chronic and can last for months or even years.
Evaluation
Trichoscopy: Hair examination using trichoscopy may provide useful information for the correct diagnosis by differentiating pseudonits from nits.[9][10][11] It shows multiple oval or elongate-shaped brown-black nodules on the hair shaft.
Direct microscopic examination (DME): DME of the crushed nodules under 10% KOH shows branched hyphae (4 to 8 microns) held together by a cement-like substance. The dematiaceous filamentous hyphae appear as chains of stout thick-walled cells resembling arthrospores. Visualization enhancement can be via lactophenol cotton blue and other colored dyes.
Fungal Culture: The culture on Sabouraud dextrose agar (SDA) medium at room temperature shows a smooth greenish-black colony with a raised and cerebriform center. The reverse side of the colonies is blackish. While performing the culture, it is noteworthy that cycloheximide does not inhibit this fungus.
The microscopic examination of the colonies shows round, dark brown, globus ascus with ascospores.
Treatment / Management
Shaving the head of all the hair is the best way to get rid of this fungal infection. However, this option may not be acceptable to females for aesthetic reasons.
Topical antifungal agents in the form of cream or shampoos are effective; 2% ketoconazole or 2% miconazole shampoo applied once a week for three weeks is effective. Non-surfactant-based leave-on lotions are also an option. Ciclopirox (0.77%) lotion or 1 to 1.5% shampoo have also been used successfully.
Older treatments include benzoic acid compound (BPC) ointment or a 1 to 2000 solution of mercury perchloride act as antifungal preparations for application to the hair after shampooing.
Oral antifungals such as terbinafine and itraconazole have been used successfully in cases resistant to topical medications.[12][13] A course of 250 mg of oral terbinafine once daily for 6 weeks was also found to be effective in the treatment of black piedra.[12]
Topical keratolytics such as 1% salicylic acid (SA) may also be added in cases non-responsive to monotherapy with antifungal shampoos.
Differential Diagnosis
- Pediculosis capitis: Black piedra is often mistaken for pediculosis capitis since lice eggs (nits) look similar to the black piedra nodules. Nits are oval in shape and white, light gray, tan, or yellowish in color. They firmly attach to the hair shaft and are difficult to remove. Nits carrying viable eggs are close to the scalp. Diagnostic confirmation is by the presence of viable eggs, nits in various stages (live and viable, open, empty/dead), or adult lice.
- White piedra: Unlike black piedra that most often occurs on the scalp hair and spares other parts of the nonglabrous skin, white piedra caused by Trichosporon spp. manifests as whitish, loose adherent material on the hair shafts that typically but not exclusively involves the scalp hair. Trichoscopy, DME under 10% KOH, and a fungal culture can easily distinguish the two conditions. The septate hyphae of Trichosporon causing white piedra are non-dematiaceous.
- Trichorexix nodosa: It is a disorder of the hair shaft characterized by easy breakability of hair and microscopically by nodes on the hair shaft. The microscopic examination of the node reveals a fractured hair. At the point of fracture, there is visible splaying out and release of individual cortical cells from the main body of the shaft of the hair.
- Monilethrix: It is a rare autosomal dominant hair disease that results in short, fragile, broken hair that appears beaded. Light microscopy, shows the hair shaft has regular elliptical, fusiform, or spindle-shaped swellings that are separated by constricted internodes.
Treatment Planning
- Shaving the head (if culturally appropriate and with patient's willful consent)
- 2% ketoconazole or 2% miconazole shampoo or 1 to 1.5% ciclopirox shampoo applied once-to-twice-a-week for 3 to 4 weeks
- Oral terbinafine 250 mg once daily for 6 weeks
- Oral itraconazole 100 mg twice-a-day after a meal, with a citrus drink for 1 to 2 weeks
- Counseling on the maintenance of good scalp hygiene, avoidance of sharing combs, etc.
Prognosis
The low spread of infection outside of its endemic habitat and the harmlessness of this disease indicates the good prognosis of this fungal infection. With the right treatment, black piedra has a favorable prognosis- patients recover fully with the restoration of normal hair.
Complications
There are no serious complications of black piedra infection. In the absence of treatment, patients with comorbidities (diabetes, immunodeficiency, and malignant tumors) may develop alopecia.
Reports exist of secondary pediculosis (head lice), as well as mixed piedra (black piedra plus white piedra in the same individual) in patients with poor scalp hygiene.[14]
Deterrence and Patient Education
Black piedra is asymptomatic, although the nodes on the hair strand look unsightly. When untreated, it may persist for months or even years. It is a communicable disease, and the patients and their close contacts must always exercise proper personal hygiene. To prevent black piedra, patients should be counseled regarding good personal hygiene, especially when traveling to tropical countries. They must avoid sharing combs, hats, and hair ornaments and avoid activities like swimming in stagnant water.
Pearls and Other Issues
Following good hygiene practices reduces the chance of getting this fungal infection. Regular and thorough washing of hair prevents fungi from accumulating on the hair. It is advisable to keep the comb clean and separate from other's hair brushes. Furthermore, avoidance of unhygienic hair practices, such as sharing combs, hair bands, or hair clips, will prevent the development of this disease.
Enhancing Healthcare Team Outcomes
Management of black piedra requires an interprofessional team that includes the primary caregiver, specialty-trained nurse practitioner, and dermatologist. Since the disease is asymptomatic, it may go undetected for several months. Poor personal hygiene and the sharing of hair-care products further spread this infection. Even though the disorder is benign, it reflects poor aesthetics.
The primary caregiver, nurse practitioner, and pharmacist should educate, especially those living in or planning to travel to hot and humid countries, about the risk of contracting this fungal infection. Coordinated health education by primary caregivers and nursing staff about good hygiene practices like the regular washing of hair, keeping the comb clean and avoidance of sharing combs, clips, and hairbands will prevent the development of this infection.
Treatment of this infection involves the complete shaving of the head; however, this option may not be acceptable to some females due to aesthetic reasons. In such cases washing the hairs with azole antifungals like 2% ketoconazole or 2% miconazole shampoos once a week can eliminate the infection. Oral terbinafine 250 mg once daily for 6 weeks can cure the infection in cases resistant to topical agents; such instances necessitate a medication reconciliation and dosage checking to avoid adverse effects, with concerns reported to the team. The pharmacist should verify dosing, perform medication reconciliation, and reinforce medication compliance to ensure cure. If there are concerns, the pharmacist should discuss them with the interprofessional team. Also, family members should avoid sharing personal care items with the infected individual. Nurses can monitor for treatment compliance and verify the inclusion of close contacts in the prevention regimen; it is crucial to screen the family members and close contacts of the patient for signs and symptoms of this disease and treat accordingly to avoid re-infection. All these activities among various members of the interprofessional healthcare team must be communicated to the entire team to ensure optimal treatment and results. [Level 5]
Outcomes
With treatment, the outcomes are excellent, but recurrences are frequent if the lifestyle is not changed.