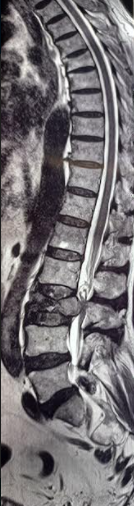
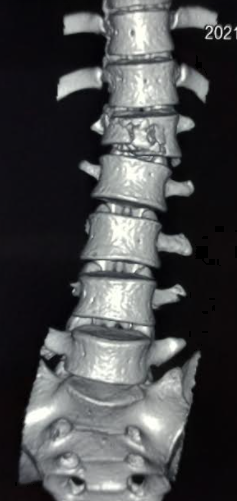
Continuing Education Activity
Vertebral fractures can result from trauma and metastatic disease but, in most cases, are the result of osteoporosis. This activity describes the evaluation and treatment of vertebral fractures and highlights the appropriate use of surgical intervention and the role of the healthcare team in managing patients with this condition.
Objectives:
- Identify the various etiologies of vertebral fractures.
- Review the steps for the evaluation of vertebral fractures.
- Explain the management options available for vertebral fractures.
- Summarize interprofessional team strategies for improving care coordination and communication to advance vertebral fracture treatment and improve outcomes.
Introduction
The vertebrae are bones in the spine joined by articulations that not only protect the spinal cord but also allow axial loading and support of the limbs. The spine is made up of 33 vertebrae. The word 'vertebra' originates from the Latin word meaning 'joint or articulation' or from the word 'vertere' meaning “to turn.” Embryologically the vertebral body is formed by the fusion of adjacent sclerotomes. Cancellous spongy bone fills the center and then comes together to create the superior and inferior endplates. Cortical compact bone then covers the rest of the cancellous bone. The endplates are made of thickened cancellous bone and are responsible for providing nutrients and attachments to the disk. These bones are made up of a ventral cylinder mass of cancellous bone called the body and a dorsal vertebral cortical arch. The ventral body has two pedicles coming off that lead to the lamina and join dorsally to make up the spinous process. Two adjacent vertebrae form the vertebral foramen between each pedicle bilaterally. Anterior to the vertebral body is the anterior longitudinal ligament that runs from the skull down to the sacrum and aids in limiting extension. Immediately posterior to the body is the posterior longitudinal ligament that runs from the tectorial membrane to the sacrum and aids in limiting flexion. The laminae connect by the discontiguous ligamentum flavum and help preserve upright posture. The interspinous ligament fortifies the spinous processes. The facet joints are covered and stabilized with a ligamentous capsule, and each body gets affixed to a disk above and below that aids in diffusing axial loads. Zygapophyses (greek=yoke) or articular processes sprout off the pedicle at the laminar junction, are encased in hyaline cartilage, and depending on the degree of angulation, determine spine movement. A thorough understanding of the bony and ligamentous anatomy is important when evaluating and treating a vertebral fracture.
Vertebral fractures result from improper axial loading with or without a rotational component and/or distraction/dislocation in the setting of trauma, osteoporosis, infection, metastatic, or other bone diseases.[1][2]
Fracture classification systems were designed to guide treatment decisions. Systems evaluate spinal stability, neurological deficit, location, the extent of damage to the bony elements, and associated ligamentous complexes. One of the first models to classify traumatic thoracolumbar fractures and pathomorphology was the three-column system of Denis. The anterior column is made up of the anterior longitudinal ligament, annulus fibrosus, and the anterior part of the vertebral body. The middle column includes the posterior part of the vertebral body, annulus, and posterior longitudinal ligament (PLL). The posterior column includes all the structures posterior to the PLL. Three system types currently prevail in classifying traumatic fractures: the Spine Trauma Study Group developed the Subaxial Injury Classification and Severity scale (SLICS) and Thoracolumbar Injury Classification and Severity score (TLICS). While in 1994, the AO spine classification was proposed (a two-column model) but has had poor intraobserver and interobserver reliability.
Etiology
Osteoporosis is the most common precipitating factor for vertebral fracture. However, trauma, cancer, chemotherapy, infection, long-term steroid use, hyperthyroidism, and radiation therapy are also known to weaken bones that can lead to compression fractures. The etiology of lower bone density can be related to smoking, alcohol abuse, lower estrogen levels, anorexia, kidney disease, medications, proton pump inhibitors, and other medications. Risk factors include female gender, osteoporosis, osteopenia, age greater than 50, history of vertebral fractures, smoking, vitamin D deficiency, and prolonged use of corticosteroids.[3]
Trauma is the second most common cause of spine fracture, and motor vehicle accidents are the number one cause of spinal cord injury. A spinal cord injury occurs from C1 to L2, the approximate level of the cauda equina. Injuries below the conus are cauda equina injuries. According to the National Spinal Cord Injury Statistical Center, other high-ranking causes of spinal cord injury include falls and gunshot wounds. Osteomyelitis infection accounts for admission incidence of 4.8 of 100000 patients.[4]
Epidemiology
Estimates are that over 200 million people have osteoporosis.[5] Osteoporosis affects up to 30% of women.[3] Vertebral compression fractures affect more than 1.5 million Americans annually, 10.7 per 1000 women and 5.7 per 1000 men.[4][6] If the clinician diagnoses a vertebral compression fracture, there is a fivefold increase in the new incidence of fracture, and two fractures increase the risk by twelvefold.[6][7][8] These fractures result in chronic and acute pain, reduced quality of life, loss of self-esteem, social isolation, increased risk of falls and fractures, and an approximate mortality rate twice that of matched controls.[9] The most common levels for compression fractures caused by osteoporosis are at the thoracolumbar junction T11-L2. Traumatic spine fractures estimates are 160000 per year, with 50% affecting the thoracolumbar junction. They are more frequent in men with an average age of 30.[10]
Pathophysiology
Peak bone density occurs approximately between the ages of 18 and 25. Bone remodeling is a part of the normal physiological activity where osteoclasts, assisted by transcription factors, degrade bone matrix, and osteoblasts are signaled to rebuild the bone. Osteoporosis is a degenerative pathway resulting from excessive bone resorption or inadequate formation of new bone and results in a decrease in cancellous bone density, thereby weakening its architecture and structure. Subsequently, a rapid increase in bone remodeling increases fragility to the point that low impact movement leads to compression fractures.[11]
The spine acts to stabilize three forces of compression, distraction, and torsion.[12] In trauma, the bony pathomorphology results from axial loading with or without flexion leading to various degrees of compression fracture ranging from mild to severe burst fractures. A compression fracture only involves the anterior column, while the burst fracture affects the anterior and middle columns via the vertebral body. A seat belt injury can result in the failure of the middle and posterior columns through a flexion force tearing the spinous ligaments—a fracture-dislocation results from a rotational or shear force combined with axial or tension loading.
Infection and other spine diseases cause erosion of the vertebral body. The spine begins to collapse, causing deformity and potentially resulting in a compression/burst type fracture affecting the anterior and middle columns.
History and Physical
When should osteoporotic compression fractures be high on the differential diagnosis? Both men and women are subject to vertebral compression fractures. However, one in four women with vertebral fractures goes undiagnosed.[13] Patients with compression fractures will typically present with acute or chronic back pain. Symptoms include a sudden onset of pain that may be related to impact movements. This pain is focal at the level of disease. There is increased pain during standing or walking, a decrease in pain when lying down, and increased pain over the palpated affected area. This condition can lead to increases in kyphotic and lumbar deformity, loss of activity in daily life, constipation, decreased respiratory drive, deep vein thrombosis due to prolonged inactivity, and social problems. The physical exam can reveal loss of height, loss of muscle tone, and change in sagittal balance. Vertebral column fractures are typically not related to myelopathic signs, and radicular pain unless severe or involve some form of spinal canal stenosis/compression.
The acute trauma patient will undergo CT of the spine after securing the airway, ensuring breathing and hemodynamic stability. A full neurological evaluation, including rectal tone, is undertaken to assess spinal cord injury and classified under the ASIA scale. Intubated patients who are unable to participate in the exam will be evaluated based on reflexes and responses to painful stimuli. The basis for evaluation for vertebral fractures is in the clinical guidelines.
Back pain is often the chief complaint among patients diagnosed with vertebral erosion due to infection or bone disease. Palpating over the spine can identify areas of concern and warrant further imaging studies.
Evaluation
Elderly patients or those with osteoporosis or who are at risk of osteoporosis who present with mechanical ground-level falls or low impact trauma complaining of acute back pain should undergo CT to evaluate for compression fractures. Osteoporosis can be diagnosed with a vertebral body fracture alone and/or a DEXA scan with a value of less than -2.5. Imaging is the gold standard in assessing vertebral column fractures. Lateral radiographs of the spine can be diagnostic of both osteoporosis and vertebral column fractures. Measurements of the adjacent vertebral bodies can be taken and compared with the segment in question. CT is considered the best modality for evaluating spinal fractures. CT allows the clinician to evaluate the spine in three planes to properly grade the extent of pathology. CT can also be used to guide toward a DEXA scan.[14] An MRI can show the relationship between bony structures, soft tissues, and acuity. Dual-energy X-ray absorptiometry (DEXA scan) is considered the gold standard for diagnosing osteoporosis (with a T score less than -2.5) but is not useful for diagnosing compression fractures.
In 1993, Vertebral Fracture Assessment Using a Semiquantitative Technique, by Genant et al., was published and evaluated osteoporotic fractures; this has wide acceptance and utilization. The scale looks at the shape of the vertebrae and measures the loss of height (LOH). It starts at grade 0 for normal vertebrae, grade 1 for mild fracture of 20 to 25% LOH, grade 2 for moderate fracture 25 to 40% LOH, grade 3 for severe fracture showing LOH at greater than 40% [15]. Biomarkers can help diagnose osteoporosis but do not serve as a diagnostic measure for compression fractures.
The classification schemes for all fractures of the entire spine are listed below for completion, as compression deformities can also occur in the setting of multiple traumatic fractures, as well as a component of a more severe injury.
The cervical spine divides into upper and lower sections. Upper cervical spine injuries are related to the occiput, atlas (C1), and axis (C2). Subaxial cervical injuries are from C3-C7. Due to anatomical differences, the remainder of the spine can subdivide into thoracic levels, T1-T10, thoracolumbar junction T11-L1 (where more than half of these fractures occur), and the lumbar spine L2 to L5.[10][16][17]
Occipital condyle fractures are usually the result of high-speed trauma. Anderson and Montesano classify these injuries based on morphology and type of injury.
- Type I results from impaction via an axial force resulting in a comminuted fracture with an intact tectorial membrane and alar ligaments but is considered unstable when bilateral.
- Type II is basioccipital fractures that involve the occipital condyle and are usually stable.
- Type III is an avulsion fracture that results from forced rotation and lateral bending as the alar ligaments pull away from the bone. These are treatable with rigid orthosis or halo vest.[18]
Atlanto-occipital injuries are from occiput to C2. Atlanto occipital dislocation (AOD) represents less than 1% of cervical spine injuries but is highly fatal due to anoxia due to respiratory arrest after bulbar cervical dissociation. This dislocation can classify into three types:
- Type I is an anterior dislocation of the occiput relative to the atlas.
- Type II is a distraction injury in a longitudinal axis.
- Type III is a posterior dislocation of the occiput relative to the atlas.
The basion-axial interval (BAI) measures from the inferior tip of the clivus to the superior extension of the posterior axial line, off the cortical margin of the body of C2. The basion dental interval (BDI) measures the distance from the basion to the closest point on the tip of the dens and should be less than 8.5 mm in adults and 10.5 mm in children. The Powers ratio can only be used to assess Type I dislocations. It is a measurement from the basion to the posterior arch of C1 divided by the measurement of the opision to the anterior arch of C1 and should be less than 1.[19] Measuring the condylar gap evaluates the distance between the occipital condyle and superior articular surface of C1 and should be less than 1.4 mm. Patients with AOD should continue with cervical immobilization without traction and undergo internal fixation and fusion. If MRI only demonstrates moderate signal abnormality, some elect for halo vest or collar stabilization.
Atlantoaxial rotatory subluxation injuries are classified using the Fielding and Hawkins system that assesses the transverse atlantal ligament (TAL), facet injury, and anterior displacement (AD).[20]
- In Type I, the TAL is intact. The facet injury is bilateral. The AD is less than or equal to 3 mm. The patient may require a soft collar for support.
- In Type II, the TAL is injured. There is unilateral facet injury. The AD is 3.1 to 5 mm, and the patient will require a hard collar.
- In Type III, the TAL is injured. There is bilateral facet injury. The AD is greater than 5 mm.
- Type IV has a posteriorly displaced odontoid.
Type III and IV subluxation injuries are unstable and require halo stabilization. Subluxation that cannot be reduced with a halo vest or gentle traction should receive surgical fixation and arthrodesis.
In the anterior atlantoaxial subluxation, there is transverse atlantal ligament injury with an increase in the atlanto-dental interval or odontoid process fracture with a normal ADI measurement.
- A Type I injury is a tear in the TAL and requires surgical stabilization.
- A Type II injury results from the C1 tubercle detaching from TAL and can heal with halo vest immobilization.
Atlas (C1) fractures account for nearly 7% of cervical spine fractures.[21] These classify as Types I-III.
- Type I is a fracture that involves a single arch.
- Type II is a four-point burst fracture. This is a classic Jefferson fracture that has expanded its definition to include two and three-point fractures. The fracture stability gets determined by the status of the TAL and will require either cervical immobilization and or surgical stabilization.
- Type III is a lateral mass fracture of the atlas.
Axis (C2) fractures can vary, including hangman's fractures, odontoid fractures, and other parts. The hangman's fracture results from hyperextension and axial loading with resulting bilateral pars interarticularis fractures and can often be managed with cervical immobilization. The Levine classification of the hangman's fractures evaluates fracture line, angulation between endplates, and anterior subluxation.
- Type I is a vertical pars fracture with less than 3 mm of subluxation of C2 on C3 and no angulation.
- Type IA demonstrates non-parallel fracture lines with vertebral foramen extension, with C2 subluxed 2 to 3 mm anterior on C3, and a high incidence of paralysis.
- Type II includes the pars fractures with C2-C3 disc rupture, injury to PLL, subluxation of C2 on C3 greater than 3 mm, and can often be reduced with traction.
- Type IIA is an oblique fracture with subluxation less than 3 mm and angulation up to 15 mm treated with surgical arthrodesis without traction.
- Type III includes fractures through the pars with bilateral C2-C3 facet disruption, C2 free-floating posterior arch, C3 ALL disruption, and requires closed reduction without cervical traction.
If any fracture extends through the vertebral foramen, a CTA should be obtained to evaluate for vertebral artery injury.
Odontoid fractures are classified using the Anderson and D’Alonzo system.
- Type I is through the tip, likely the result of alar ligament avulsion and considered unstable.
- Type II is through the base of the neck and is unstable.
- Type IIA is through the base of the neck but with bone fragments and is unstable.
- Type III is through the body of C2 and is usually stable.
The Spine Trauma Study Group created the subaxial cervical spine injury classification and severity scale (SLICS) to evaluate fractures from C3-C7. The SLICS scale evaluates morphology, discoligamentous complex, and neurological status. Morphology gives 1 point for compression fracture, 2 points for burst fracture, 3 points for distraction injury, 4 points for rotation/translation like teardrop fracture (flexion with axial loading), facet dislocation, or bilateral pedicle fractures. The discoligamentous complex includes the anterior longitudinal ligament (ALL), posterior longitudinal ligament, ligamentum flavum, facet capsule, interspinous, and supraspinous ligaments. The DLC scoring is 1 point for indeterminate injury where there is an isolated widening of the spinous process and no facet malalignment. 2 points are given for disrupted as seen in perched or diastatic facets with widened anterior disc space. The neurological status is given 1 point for nerve root injury, 2 points for complete spinal cord injury and 3 points for incomplete spinal cord injury, and +1 for continuous cord compression with neurological deficit. This table was designed to indicate that adding up points for a score of greater than or equal to five is an indication for surgery.
Isolated injury to the spinous processes due to avulsion is called a clay shoveler’s fracture and can occur with whiplash, neck hyperflexion, or direct blow to the neck. These fractures are stable and do not require intervention.
In evaluating compression and burst fractures of the thoracic and lumbar spine on sagittal CT, always measure the angulation, retropulsion of fragments, listhesis, and loss of height. Look for any abnormal separation of spinous processes that may warrant an MRI to evaluate for ligamentous injury. Axial CT will allow clear visualization of pedicles and retropulsion of bony fragments into the canal. The thoracolumbar injury classification and severity (TLICS) scale provides for the classification of fractures and guidance for intervention.
TLICS scale evaluates bony images, neurologic status, and integrity of the posterior ligamentous complex. Evaluation of bony pathomorphology gives compression and burst fractures 1 point, distraction injuries 2 points, translational/rotational injury 3 points. Neurological status with nerve root injury or complete spinal cord injury is 2 points each, and incomplete spinal cord or cauda equina injury is given 3 points each. The posterior ligamentous complex is given 2 points for suspicion of injury and 3 points for definitive injury. A score of 5 or higher is a strong argument for surgical stabilization of the patient. Certainly, any incomplete spinal cord injury should be taken to the OR within 24 hours for the best possible outcome. Patients should remain on thoracolumbar precautions until there is a determination of spine stability and a treatment plan is in place.
Minor fractures of the thoracic or lumbar spine are considered stable and do not require intervention when there is no neurological deficit include spinous processes, articular processes, isolated laminar fractures, and transverse processes (unless accompanied by brachial plexus or lumbosacral plexus injuries).
MRI will be utilized to verify disc and ligamentous injury. A CT myelogram is an option for patients unable to obtain an MRI.
Individuals who use IV drugs, who are immunocompromised, or have diabetes, who present with back or neck pain not attributed to trauma and who have labs demonstrating elevated CRP, WBC, and or ESR should be evaluated for an infectious etiology of osteomyelitis and discitis that could lead to spinal instability due to bony erosion. A CT will demonstrate the erosion of bony elements. An MRI will evaluate for abscess, disc, and soft tissue injury.
Treatment / Management
Conservative management of acute osteoporotic compression fractures with goals of reducing pain and improving functional status includes acetaminophen, ibuprofen, opioids, physiotherapy, rehabilitation programs, and bed rest. Bracing for compression fractures is often done for patient comfort and is unlikely to influence spinal stability.[22] A small study did support the use of semirigid thoracolumbar orthosis for gait improvement.[23] Treatment of the underlying disease that leads to vertebral column fracture is the recommended approach.
For persistent pain and the failure of conservative treatments, surgical intervention is necessary. A 2018 Cochrane review was not able to support vertebroplasty for treating acute to subacute osteoporotic vertebral fractures.[24] However, several large clinical studies followed for at least 12 months have concluded that mortality rates following vertebral column fractures are significantly higher for patients treated conservatively versus vertebroplasty and balloon kyphoplasty, while only one study concluded no difference.[25][26][27][28][29][30]
Vertebroplasty is usually an outpatient procedure that takes one to two hours where under guided imaging, a needle gets inserted into the vertebral body, and cement is injected. This cement hardens quickly and stabilizes the fracture. Kyphoplasty is a very similar procedure, but in this case, a balloon is used to expand the vertebral body before injecting the cement.
The goals of managing spine fractures are to ensure spinal stability and preserve neurological function.
Patients with SCI will need ICU admission, central and arterial lines, and possible airway support. Spinal cord injury can lead to unopposed parasympathetic stimulation resulting in vasodilation and hypotension. Norepinephrine or dopamine will provide both alpha and beta stimulation and should be used to maintain blood pressure with a MAP goal of greater than 85 for seven days. Acute trauma patients should remain in both cervical and thoracolumbar precautions until cleared.
The treatment goal for vertebral fractures is clinical stability as evaluated mechanically and neurologically, assessing the spines' ability to handle physiologic loads properly without resulting in neurological injury and simultaneously preventing deformity and pain. Classifying the acute traumatic fracture correctly will then allow for the appropriate choice of surgical stabilization or conservative management and have been discussed above. Always treat the underlying cause of the fracture.
Those who present with osteomyelitis and discitis will undergo 6 to 8 weeks of targeted IV antibiotics after biopsy leads to a microbial diagnosis. Often these patients can undergo conservative management and do not require surgical intervention. A biopsy can also be utilized to determine metastatic disease if this is also on the differential.
Differential Diagnosis
Older patients presenting with acute back pain should be evaluated with imaging to assess for vertebral column fracture. If imaging is positive for vertebral fractures outside the trauma setting, the underlying cause should be sought out; these will include osteoporosis, metastatic disease, and primary bone pathology. All high-impact trauma patients should undergo imaging diagnostics.
Prognosis
Single osteoporotic compression fractures can lead to more fractures. Treatment of the underlying disease is warranted to decrease the risk of future vertebral column fractures. Vertebroplasty and balloon kyphoplasty have been shown to lead to a reduction in pain, decrease in mortality and morbidity, and improved quality of life. Traumatic compression fractures will often heal on their own and likely will not require surgical intervention. However, those with unstable vertebral fractures will undergo surgical stabilization. Those who have incomplete spinal cord injuries may see an improvement in outcome if decompressed early.
Complications
Conservative treatment measures can lead to extended use of NSAIDs resulting in gastric ulcers and GI bleeds. Opioid use can lead to altered mental status and addiction. Untreated vertebral fractures can lead to significant kyphotic deformities and continued spinal degeneration. Pain can limit mobility and lead to constipation, deep vein thrombosis, pneumonia, deconditioning, falls, and subsequent fractures. There are also complications from kyphoplasty that include: cement leakage, intradiscal extravasation, and cement emboli.[31][32] Surgical intervention includes but is not limited to the risk of hardware failure, surgical site infections, blood loss, and neurologic deficits.
Consultations
If the patient has failed conservative measures for vertebral column fracture, they can obtain a referral to a neuro-interventionalist, orthopedic spine surgeon, or neurosurgeon for surgical consultation. Patients with acute traumatic spine fractures can have an evaluation by either an orthopedic spine surgeon or neurosurgeon. An infectious disease specialist should provide consult for help in managing both osteomyelitis and discitis.
Deterrence and Patient Education
Those suffering osteoporotic vertebral column fractures can focus on preventing new fractures and treating the underlying condition that will lead to improved quality of life. Weight-bearing exercises and muscle strengthening are critical parts of building strong bones. Healthy food choices, smoking cessation, and limited alcohol consumption should be part of a comprehensive treatment plan. For those with osteoporosis, bisphosphonates or other anti-osteoporosis medications can be used to reduce the risk of fractures.[33] Trauma patients who undergo bracing or surgical intervention will follow up with their doctor in the outpatient setting for continued monitoring.
Enhancing Healthcare Team Outcomes
The US Preventive Services Task Force recommends that all women aged 65 have routine screening for osteoporosis. The task force made no formal recommendations for men. They were also unable to recommend supplementation with either vitamin D or calcium daily, stating insufficient evidence in the primary prevention of fractures.[34] Current recommendations from the National Osteoporosis Foundation continue to recommend a diet that includes calcium, vitamin D, exercise, an assessment for risk factors leading to falls, cessation of smoking, and limiting excessive alcohol intake.[35]
Screening includes but is not limited to: bone mineral density testing, height measurements, vertebral imaging, and checking biochemical markers.[6]
Patients with osteoporosis can receive treatment with current FDA-approved medications that include bisphosphonates, estrogen agonist/antagonist, calcitonin, hormone therapy, tissue-selective estrogen complex, parathyroid hormone, and receptor activator of nuclear factor kappa-B ligand inhibitor.[35][36] A pharmacist should be involved with the selection of agents and dosing for osteoporosis and counseling the patient on potential adverse effects of these drugs. They can also perform a medication reconciliation to check for drug-drug interactions and alert the rest of the healthcare team should there be any reason for concern.
Primary care clinicians, including nurses, should emphasize the prevention of osteoporosis by making lifestyle changes. Patients should be told to stop smoking, limit alcohol intake, become physically active, eat a healthy diet, and maintain a healthy weight. Open communication between the team can help improve outcomes in patients with vertebral fractures.
Providers who take X-rays of the spine need to be familiar with the radiographic signs of vertebral column fractures; these include family practitioners and even chiropractors, who should refer appropriately when they encounter such conditions.
Should the patient require surgical intervention for vertebral fracture, an orthopedist or neurosurgeon should take the case, depending on the specific issues and the structures involved. Surgical and orthopedic specialty trained nurses can be significant assets, preparing the patient for the procedure, assisting during the procedure, monitoring the patient post-operatively, administering medication, and consulting with the pharmacy if necessary.
Vertebral column fractures and their underlying conditions require the efforts of an interprofessional healthcare team working collaboratively to ensure the best possible patient outcomes. [Level 5]