Introduction
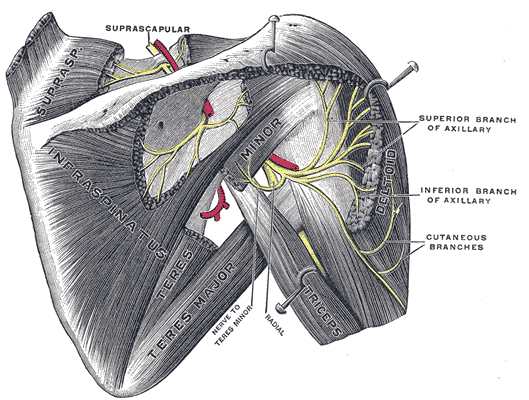
Suprascapular nerve injury has recently gained popularity as a leading cause of shoulder pain and weakness. The course of the nerve through narrow osseoligamentous structures renders it susceptible to compressional and traction injuries at the suprascapular and spinoglenoid notches. Knowledge of the anatomy of the nerve is necessary to diagnose and provide the best clinical outcomes in cases of suprascapular nerve injury.[1] See Image. The Anterior Divisions, the Suprascapular, Axillary, and the Radial Nerves.
Structure and Function
The suprascapular nerve is a branch from the upper trunk of the brachial plexus, it innervates the infraspinatus and the supraspinatus muscles. It originates in the posterior triangle of the neck, where it runs to the upper part of the scapula downward and laterally parallel to the belly of the omohyoid muscle, then it runs under the suprascapular ligament to the supraspinatus fossa. Here it provides muscular innervation to the infraspinatus and supraspinatus muscles.[1]
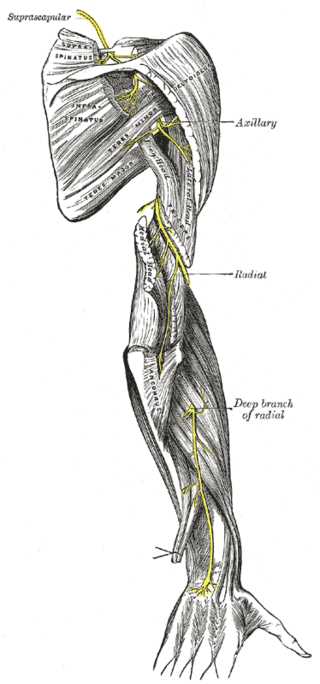
The suprascapular nerve is a mixed nerve, it has both a motor and sensory parts. The suprascapular nerve gives sensory branches to the acromioclavicular and glenohumeral joints, which serve as sensory innervation. The motor part of the suprascapular nerve innervates the supraspinatus and infraspinatus muscles, respectively. The suprascapular nerve originates from the upper trunk of the brachial plexus, the ventral rami of the fifth and sixth cervical nerves from the upper trunk of the brachial plexus join to form the suprascapular nerve, and in approximately 18% of the population, the ventral ramus of the fourth cervical nerve is also involved. The suprascapular nerve branches from the upper trunk and runs along the posterior triangle of the neck. During its course, it runs to the upper part of the scapula downward and laterally parallel to the belly of the omohyoid muscle, then it runs under the suprascapular ligament to the supraspinatus fossa. In the supraspinous fossa, it runs under the supraspinatus muscle and branches twice for innervation before curving around the lateral border of the spine of the scapula, through the spinoglenoid notch, and into the infraspinous fossa. In the infraspinous fossa, the nerve branches innervate the infraspinatus muscle.[1][2][3][4] See Image. The Anterior Divisions, Suprascapular and Axillary Nerves of the Right Side.
Embryology
The suprascapular nerve arises from the ventral rami of the fifth and sixth cervical nerves and in some population the ventral ramus of the fourth cervical nerve. Motor nerve roots originate from the ventral ramus of the spinal cord. The ventral (motor) plate begins as a ventrolateral thickening of the intermediate zone of the neural tube. The intermediate zone gives rise to motor neuroblasts of the ventral and lateral horns. Branched axons beginning at the motor neuroblast exit the spinal cord and become the ventral (motor) roots. The basal plate later becomes the dorsal horn of the spinal cord. the neural crest migrates to the nerve and then they differentiate to form the Schwan cells. [5]
Blood Supply and Lymphatics
The suprascapular artery and vein run along with the suprascapular nerve to provide the nerve its blood supply. The suprascapular artery can function either as a branch of the thyrocervical trunk or as a direct branch of the subclavian artery. The artery runs inferolateral to the anterior scalene muscles, phrenic nerve, subclavian artery, and brachial plexus, crossing posterolateral and parallel to the clavicle. Then the nerve passes superior to the transverse scapular ligament while the suprascapular nerve passes inferior to it, while entering the supraspinous fossa. Finally, the artery courses laterally to the scapular spine (deep to the acromion) and then gains entry to the infraspinous fossa, which is on the posterior surface of the scapula. The suprascapular vein travels parallel to the artery. The lymphatic drainage for the upper limb and area along the suprascapular nerve distribution is primarily from the subscapular (posterior) nodes.The subscapular nodes consist of six or seven lymph nodes that lie along the posterior axillary fold. These lymph nodes run along the course of the subscapular blood vessels. The subscapular, pectoral, and humeral nodes’ efferent drainage passes through the central nodes. The central nodes consist of three or four nodes found deep within the pectoralis minor near the base of the axilla, and in close proximity to the second part of the axilla. Efferent drainage from the central nodes passes to the apical nodes, which lie at the apex of the axilla by the medial side of the axillary vein and the first part of the axillary artery. Efferent vessels that arise from the apical group run across the cervico-axillary canal. These efferent vessels combine to form the subclavian lymphatic trunk. The subclavian lymphatic trunk may join the jugular and bronchomediastinal trunk to form the right lymphatic duct, or it may enter the right venous angle by itself.
Muscles
The suprascapular nerve has a motor and sensory innervation. Its motor innervation is to the supraspinatus and infraspinatus muscles. The supraspinatus and infraspinatus muscles are two of the four muscles that make up the glenohumeral (shoulder) joint. The supraspinatus muscle originates from the supraspinous fossa of the posterior scapula. It then attaches to the superior facet of the greater tubercle of the humerus. With innervation from the suprascapular nerve, the supraspinatus initiates and aids the deltoid in abduction of the arm, and acts in synergy with the rotator cuff muscles. The infraspinatus muscle originates from the infraspinous fossa of the posterior scapula. It then wraps around the lateral proximal humerus to attach to the middle facet of the greater tubercle. The infraspinatus acts to laterally rotate the arm and act in synergy with the rotator cuff muscles.
Physiologic Variants
There is not much literature on variants of the suprascapular nerve. Literature by Polguj et al. describes three variants in the relationship betweenthe superior transverse scapular ligament, suprascapular vessels, and nerve. The first variant, which is the most common, is where the suprascapular artery runs superior to the superior transverse scapular ligament, while the nerve and vein run inferior to the ligament. The second is where both the artery and vein run superior to the ligament, and the nerve runs inferior. The third variant, which is the least common, is where the artery, vein, and nerve pass inferior to the superior transverse scapular ligament.
Surgical Considerations
The suprascapular nerve is at risk during massive rotator cuff repairs. Literature has described the nerve in close proximity to the operative field used in rotator cuff repairs. The nerve is susceptible near the glenoid rim, rotator cuff footprint, and lateral border of the acromion. The nerve is at risk of injury near these areas during a double interval slide technique for arthroscopic cuff repairs.
The nerve is also at risk for compression neuropathy at the suprascapular and spinoglenoid notch. The nerve should be taken into careful consideration in the manner of suprascapular nerve blocks for the treatment of shoulder pain. Injury to the nerve may also occur when operating in the regions of the neck, shoulder, and scapula.
Clinical Significance
The supraspinatus and infraspinatus receive its innervation from the suprascapular nerve. When there are signs of atrophy to these muscles, the nerve is usually at risk for compression neuropathy. If both muscles show signs of atrophy, then the compression is at the level of the suprascapular notch. When there is isolated atrophy in the infraspinatus muscle the level of compression is at the spinoglenoid notch.