Continuing Education Activity
Shared psychotic disorder (folie à deux) is a rare disorder characterized by sharing a specific delusion among two or more people in a close relationship. The inducer (primary) who has a psychotic disorder with delusions influences another individual or more (induced, secondary) based on a delusional belief. It is commonly seen among two individuals, but in rare cases, can include larger groups. This activity outlines the presentation and management of shared psychotic disorder and highlights the role of the interprofessional team in improving the care of patients with this condition.
Objectives:
- Review risk factors for shared psychotic disorder.
- Describe the pathophysiology of shared psychotic disorder.
- Outline the treatment and management options available for shared psychotic disorder.
- Describe the importance of collaboration and communication amongst an interprofessional team to improve outcomes for those affected by shared psychotic disorder.
Introduction
Shared psychotic disorder (folie à deux) is a rare disorder characterized by sharing a delusion among two or more people in a close relationship. The inducer (primary) who has a psychotic disorder with delusions influences another nonpsychotic individual or more (induced, secondary) based on a delusional belief. It is commonly seen among two individuals, but in rare cases, can include larger groups. For example, it can occur in a family and is called folie à famille.[1][2]
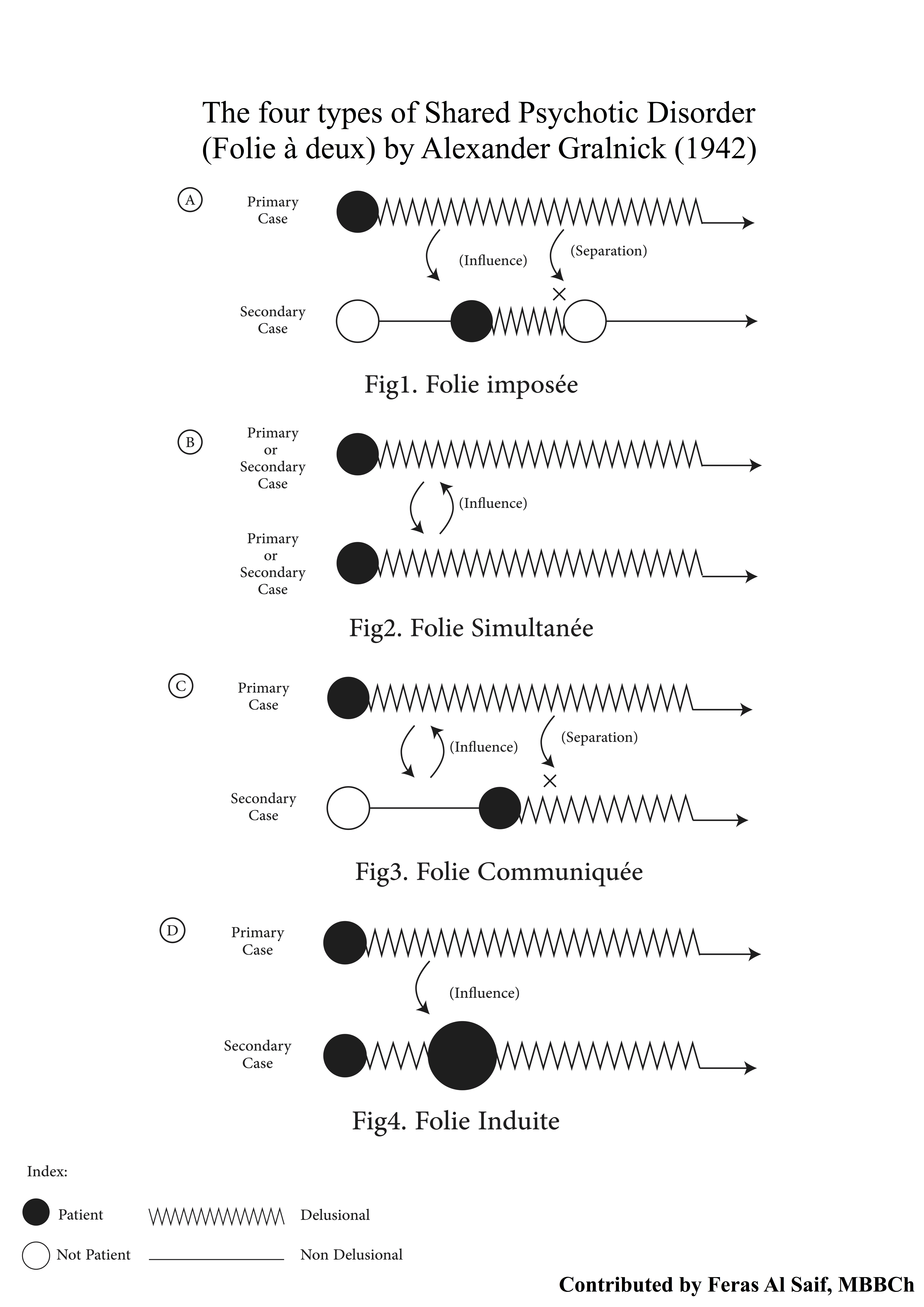
Jules Baillarger was the first to report this condition in 1860. During the 19th century, psychiatrists in Europe suggested different names. In France, it has been called "folie communiquee"(communicated psychosis) by Baillarger. In German psychiatry, it was named "Induziertes Irresein" by Lehman and Sharfetter. In 1877 Lasegue and Falret coined the term “folie à deux.” The French word “folie à deux" means madness shared by two. In the early 1940s, Gralnick, in his review of 103 cases of folie à deux, described four types of this disorder. He defined it as a psychiatric entity characterized by the transfer of delusions from one person to one or several others who have a close association with the primarily affected person. The four types are as follows:
- Folie imposee (imposed psychosis) - Described by Lasegue and Falret in 1877. The delusions are transferred from an individual with psychosis to an individual without psychosis in an intimate relationship. The delusions in the induced individual soon disappear once the two are separated.
- Folie simultanee (simultaneous psychosis) - Described by Regis in 1880. Both partners share the psychosis simultaneously. They both have risk factors through long social interactions that predispose them to develop this condition. There are reports of sharing genetic risk factors among siblings.
- Folie communiquée (communicated psychosis) - Described by Marandon de Montyel in 1881. This type is similar to folie imposee; however, the delusion in the secondary partner occurs after a long period of resistance. Also, the secondary partner will maintain the delusion even after separation from their partner.
- Folie induite (induced psychosis) - Described by Lehmann in 1885. In this type, new delusions are assumed by an individual with psychosis who is being influenced by another individual with psychosis.
This disorder was first listed in the Diagnostic and Statistical Manual of Mental Disorders, Third Edition (DSM-III) as shared paranoid disorder. In the next edition (DSM-IV), the term changed to shared psychotic disorder. In the latest edition, DSM-5, it was removed as a separate disease entity. It now is included in the section on other specified schizophrenia spectrum and other psychotic disorders. ICD-10 lists it as induced delusional disorder.[2]
Etiology
The exact cause of shared psychotic disorder is still unknown. However, certain risk factors associated with it include the following:
- Length of the relationship: Numerous studies highlight the role of long relationship duration as an essential factor for developing this condition. It is crucial to understand that the attachment with the inducer plays a key role in adopting the delusion.[3]
- Nature of the relationship: The majority of cases reported are among family members. The commonest relationship is between married or common-law couples, and the second most common is between sisters.[3]
- Social isolation: Most reported cases indicate poor interaction with society. A confused individual can undergo influence under frightening conditions in the absence of social comparison. The information received by the secondary individual is in harmony with what the primary individual felt. The conviction of certain ideas will eventually prevail as the only solution to maintain a mutual relationship.[4]
- Personality disorder: Individuals usually show features of a personality disorder. The usual description for them is neurotic, introverted, and emotionally immature. Some case reports noticed features of premorbid personality disorders especially dependent (passive), schizoid, and schizotypal.[5][6]
- Untreated mental disorder in the primary: An untreated individual with chronic mental conditions can be a social risk factor of influence to the other partner or family. The commonest diagnosis in the primary is a delusional disorder followed by schizophrenia and affective disorder.[3]
- Cognitive impairment: It has been noted that the secondaries lack good judgment and intelligence.[4]
- Comorbidity of the secondary: An individual diagnosed with a mental disorder, including schizophrenia, bipolar affective disorder, depression, dementia, or intellectual disability, carries a risk of being influenced by another mentally ill person.[4]
- Life events: Stressful life events that affect the relationship can influence behavior in the individual to accept certain delusions or lessen their ability to resist their feelings or emotions. For example, a wife who has been suffering from delusions for several years starts accusing her husband, who has erectile dysfunction, of being in a relationship with a mistress or that the mistress is “stimulating him with sildenafil and narcotics.” He will eventually accept this belief because of his unstable, passive personality condition, as well as the serious situation from which he suffers.[5]
- Communication difficulties: Having difficulty sharing ideas can be a reason for preferring isolation. It is suggested that improving communication among dyad relationships through multiple-conjoint psychotherapy may help both partners understand the different points of view that will collapse in the presence of rigid, mindless thinking.[7]
- Age: Previous studies reported age differences, the older of the two in the relationship being an inducer and the younger being the induced. However, recent studies do not support this finding.[2]
- Gender: The disorder is more common among females, both as a primary or secondary.[2]
Epidemiology
The incidence and prevalence of shared psychotic disorder are difficult to estimate. However, some studies report that it is responsible for 1.7 to 2.6% of psychiatric hospital admissions.[8] This figure may, however, be underestimated as it is underdiagnosed and often missed in clinical practice. Psychiatrists may treat the primary while not being aware that the delusions exist in others.[9] Some authors even argue that the disorder is not rare.[3]
Pathophysiology
Shared psychotic disorder usually is chronic, and both the primary and secondary individuals share the original delusion(s). The shared delusion(s) occur under unique circumstances and can be of any type. The most common type of delusion is persecutory, followed by grandeur. There are racial variations. For example, in Japanese communities, persecutory delusions are the commonest followed by religious delusions.[4][10] There may be other psychiatric features such as social withdrawal, hallucinations, or suicidal thoughts.[11] Functionality is generally preserved compared with other disorders. There may be significant impairment in a particular aspect of life, especially when the delusions are not confronted.
The concept of the dominant-submissive relationship is derived from the psychodynamic theory. The role of the primary is rigid and possessing (dominant) while the submissive is less intelligent, passive, less resilient to suggestions, isolated, and/or physically handicapped. [6] Some authors have emphasized the existence of a role reversal between partners due to the complexity of the disorder.[7]
History and Physical
Presentation depends on the type of shared delusion. One partner usually faces a problem in society that involves the intervention of a psychiatrist. Often, this problem is supported or under the influence of the other partner. Both exhibit unrealistic, fixed, false beliefs which are unshakable. They might be paranoid, fearful, and suspicious of a neighbor or someone in their community. One might seek mental assessment after risky behavior, unreal claims, or recent assault. The secondary partner can be mistakenly referred and usually discovers that other people within their social sphere share the same belief as the primary. There can be under-treated or undiagnosed cases within the community that last for several years before being discovered. Sometimes partners who shared particular delusions can be admitted to the hospital together because of risky behavior or assault on themselves or others.
General description: The couples usually are groomed and well dressed.
Behavior: Defensive attitude or angry behavior can occur towards an interviewer who challenges the patient's delusion(s).
Speech: The patient's speech usually is coherent and relevant.
Mood and Affect: Mood is usually congruent with the delusion; a paranoid patient may be irritable, while a grandiose patient may be euphoric.
Thought: The form of thought is usually goal-oriented. The delusions are shared either entirely or partially; often are not bizarre in content; are systematically structured; overvalue social, cultural, or religious beliefs beyond the community norms; and can include homicidal or suicidal ideation.
Perceptions: They are less likely to express abnormal perceptions unless there are predisposing factors. Sometimes the secondary is the only person who experiences some form of hallucinations.
Orientation and Cognition: The patient is usually oriented to time, place, and person unless driven by their delusion. Memory and cognition generally are not affected.
Risks: It is crucial to evaluate the patient for suicidal or homicidal ideation and plans. If there is a history of aggression with an adverse outcome, then hospitalization should be considered.
Insight and Judgment: Most commonly, patients and their partners have no insight into their mental illness. Judgment is assessable by inquiring about past behavior and a future plan.[9][12][13]
Evaluation
As with any other psychiatric disorder, no specific labs are necessary for shared psychotic disorder. Most of the investigations, whether imaging or laboratory tests, should be considered to rule out any organic cause. A urine toxicology screen is vital to rule out any substance-induced disorder. If there are no organic or substance-induced disorders, a full psychiatric assessment should be next. It is helpful to ask for collateral history about both partners from a third person. It is common to take a history only from one of the partners because of strict social isolation, which can be very challenging. After taking a history, the psychiatrist should conduct a complete mental status examination. Collecting further details from other members of the family or friends should help in evaluating the patient. The primary partner can be defensive and misleading to encapsulate the delusion, concealing the symptoms for years.
Treatment / Management
Treatment should be tailored on a patient-by-patient basis. If there is an undertreated patient, efforts should be made to encourage increased adherence to the treatment plan. There have been suggestions that separation from the primary improves the condition significantly. After admission, the influence of the primary partner gradually disappears. However, it is worth noting that recent data suggest that separation by itself can be insufficient or may aggravate the condition.[3][14] Treating both partners with medication, whether alone (antipsychotics or antidepressant) or in combination (mood stabilizers and antipsychotics) and (antidepressants and antipsychotics), may help improve the condition.[3] Starting medication indicates that the patient's condition is severe and likely to express residual symptoms. It is critical to follow up with patients due to a possible alternative diagnosis. Psychotherapy can be offered to both partners either individually or as conjoined-psychotherapy.[7] Electroconvulsive therapy is an option.[3]
Differential Diagnosis
Formulating a differential diagnosis must include a history of the association between both partners. The onset of the condition usually precedes the onset of the shared delusion(s). The diagnosis of shared psychotic disorder should always be made only after ruling out any organic cause or substance-induced disorder.
- Schizophrenia/Schizoaffective: This can be differentiated by the secondary reporting symptoms that are not influenced by the primary, such as hallucinations, disorganized speech, or negative symptoms. In the case of schizoaffective, an affective component should be present.
- Mood Disorder with Psychotic features: This condition has a specific delusion that is mood-congruent and not shared but expressed independently.
If the delusions do not disappear when the partners are separated, it is important to reassess and consider an alternative diagnosis.
Prognosis
The prognosis of shared psychotic disorder is challenging to estimate, as it depends on multiple risk factors, including the primary's mental disorder and the secondary's biopsychosocial predisposing factors. Theoretically, children are more likely to benefit from separation than adults. Adherence to the management plan in both partners most likely will result in a better outcome than being untreated. An assessment of the nature and the duration of exposure to the delusion can provide clues to the potential outcomes of the disorder. Having premorbid personality features or predisposing risk factors can complicate the condition, leading one to consider an alternative diagnosis.[6]
Complications
These patients are not discovered easily due to a lack of insight. They are usually referred after a complication, namely acting on their delusions and jeopardizing their life or others. For example, a patient acts on their paranoid delusions via multiple accusations then commits an assault. Having delusions of grandeur or religious delusions also can be hazardous to others.[9]
Deterrence and Patient Education
Patients and their families may benefit from online resources. Websites often provide information about shared psychotic disorder along with information on support programs and resources. Additionally, any member of the healthcare team is well-positioned to educate patients and their families directly.
Enhancing Healthcare Team Outcomes
Patients with shared psychotic disorder can go undiagnosed because only the primary partner is registered for treatment in a classic presentation. The level of tolerance and harmony among the two patients can add a significant challenge to the clinician in identifying each partner's role. Awareness of the nature of the dyad relationship dynamics is necessary. Most patients lack insight, which causes a substantial barrier to early discovery and management. The failure to adhere to treatment is an additional challenge to the clinician. A key aspect is understanding the impact of the delusions on both partners. A board-certified psychiatric pharmacist should work with the team to select the best agents for optimal therapeutic results with minimal adverse effects. A holistic approach that assesses and manages the biopsychosocial factors should help improve outcomes. The psychotherapist, mental health nurse, and psychiatrist should continue to follow these patients because relapse is common due to noncompliance with treatment.
Shared psychotic disorder requires a comprehensive interprofessional team approach that includes physicians, specialists, specialty-trained nurses, and pharmacists, working together as a team for optimal treatment and outcomes. [Level V]