Continuing Education Activity
Lacerations are a common patient chief complaint, and the understanding of key history and physical exam information can speed patient care. This activity outlines lacerations and explains the role of the healthcare team in evaluating and treating patients who present with lacerations.
Objectives:
Describe the critical points of the history and physical exam needed to describe the laceration accurately.
Review the risk factors of poor incision healing.
Outline the considerations required for the selection of the appropriate laceration repair material.
Describe the importance of improving care coordination between interprofessional team members to improve outcomes for patients affected by lacerations.
Introduction
Lacerations are a pattern of injury in which skin and underlying tissues are cut or torn. Healthcare providers encounter lacerations regularly. It was reported in 2005 that nearly 12% of all ER visits, or 13.8 million visits occurred for laceration care.[1] Lacerations can be managed in the outpatient setting as well, depending on the location and severity of the injury.
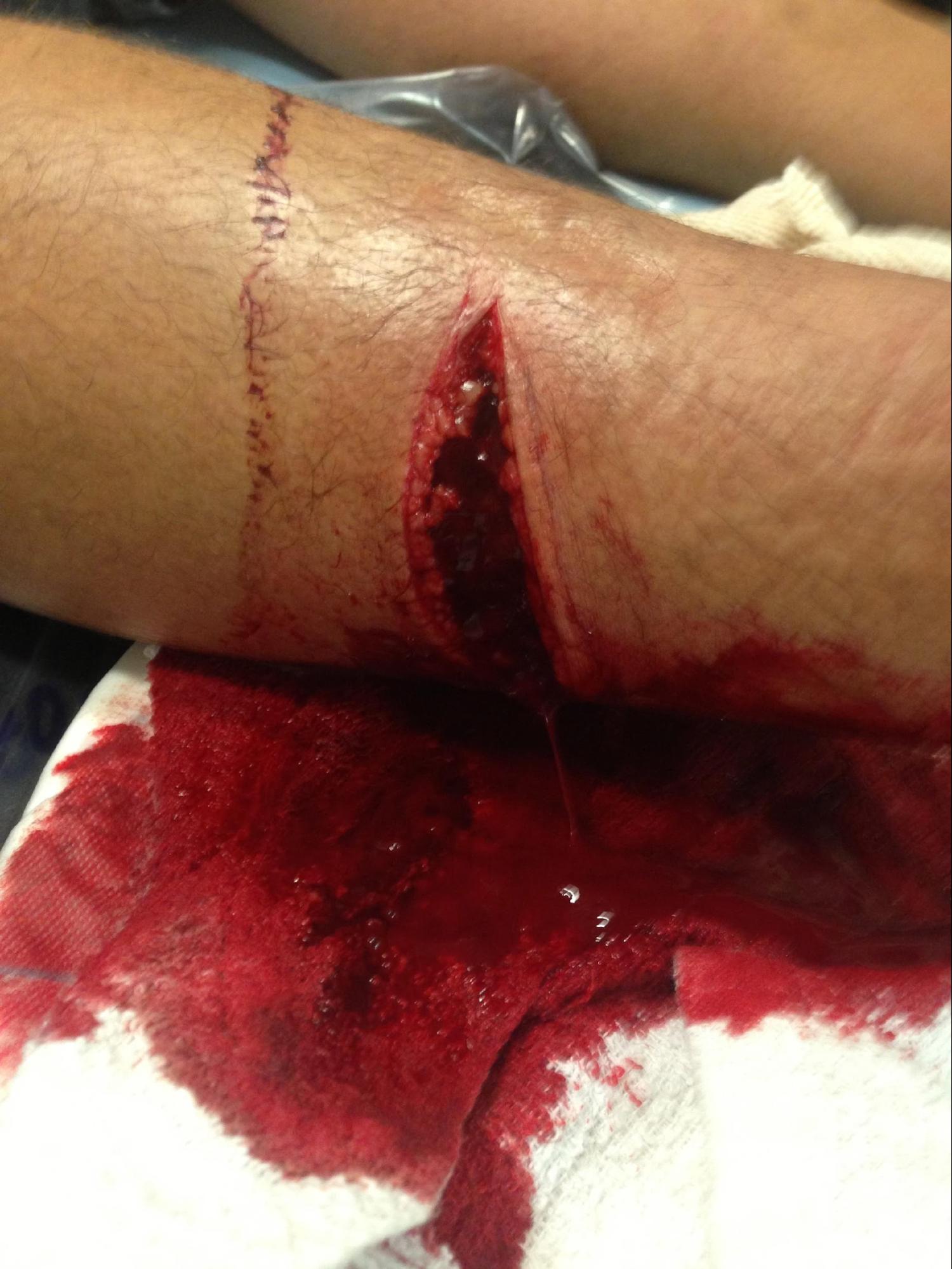
The clinical presentation of lacerations can be highly variable based on location, depth, width, and length. Due to this highly variable presentation, the healthcare team must have a strong understanding of the critical history and physical exam items each laceration requires. See Image. Laceration of the Right Lower Leg and Flexor Tendon Laceration.
Anatomy and Physiology
When approaching a laceration, a basic understanding of the anatomy of the skin can aid in understanding the depth of lacerations. Also, a knowledge of the stages of wound healing will assist in patient education and follow up care.
The skin is made up of three layers:
- Epidermis: most superficial layer, contains no nerve endings or blood vessels. There are four layers to the epidermis in all areas except in the palms of the hands and soles of the feet, where there are five layers.
- Dermis: Contains nerves, vessels, glands, and connective tissue.
- Fascia: a combination of connective tissue and adipose tissue.
The four stages of wound healing are:
- Hemostasis: Beginning immediately, the contracture of smooth muscles and tissue compressing small vessels. Platelets also begin to aggregate, activating the clotting cascade to produce initial fibrin clots.
- Inflammation: Beginning immediately and lasting up to 30 days, Neutrophils activated through the complement cascade begin phagocytosis of dead tissue. After the first 72 hours, macrophages respond and continue phagocytosis for the duration of this stage.[2]
- Proliferation: Beginning at day seven and lasting the next several weeks, angiogenesis begins taking place, accounting for underlying erythema seen at the site. Also, during this time, fibroblasts begin to replace the inflammatory mass, and collagen is laid down to replace fibrin clots.
- Maturation: beginning after several weeks, this stage can last from 6 to 12 months. Collagen is remodeled from type III to type I. At this stage, the scar should flatten, and the underlying erythema will resolve. Patients should be advised at this stage to massage the scar as well as avoid direct sunlight to reduce the risk of hyperpigmentation of the scar.
Indications
To best assess the future care requirements of any laceration, the healthcare team must first review the patient's history as well as do a complete physical examination of the wound and nearby structures.
Pertinent history items include:
- Time of initial injury
- Location of laceration and extremity injuries have an increased risk of infection.
- Measurements of laceration, including length, width, and depth. As the depth and width of injuries increase, the risk of infection increases.[3]
- Mechanisms of injury, such as crush, sharp object, and shear from fall. Crush injuries with localized tissue injury have an increased risk of infection and scarring.[4]
- Age, because at the extremes of age, there is a risk of poor healing.
- Past medical history, specifically any history of diabetes mellitus, chronic renal failure, obesity, malnutrition, or any use of immunosuppression drugs such as chemotherapy medications.[5]
- Allergies, specifically to latex, anesthetics, or antibiotics.
- Immunization status, note the patient's tetanus vaccine history. Current guidelines for tetanus are:
- Adults with greater than or equal to three previous tetanus doses:
- Clean wounds: Tdap (tetanus, reduced diphtheria, pertussis) or Td (tetanus, reduced diphtheria) only if it has been over 10 years since their last vaccination.
- Dirty/complex wounds: Tdap or Td if more than 5 years since their last vaccination.
- Adults with under 3 previous tetanus doses:
- All wounds: Tdap or Td required; if dirty/complex, they will also require immunoglobulin treatment.
- Children:
- Under 7 years old: DTaP (diphtheria, tetanus, pertussis) vaccine is the recommendation; if pertussis is contraindicated, give DT (diphtheria, tetanus) vaccine.
- 7 to 9 years old: Td vaccine recommended.
- Over 10 years old: Tdap is preferred in patients who have never received it and have no contraindications; if age or contraindications exist, use the Td vaccine.
Keys to a good physical exam of lacerations:
- Ensure appropriate lighting, gauze, and rinse materials are easily accessible before beginning the exam.
- Establish hemostasis: Hemostasis should be established to allow for visualization of underlying structures and foreign objects, utilizing direct pressure.
- Detailed neurologic exam: The clinician should perform a complete sensation exam at and below the level of injury before the use of any anesthesia to assess for any nerve injury. A quick method to evaluate for nerve injury is two-point discrimination using a standard paper clip, always comparing to the patient's noninjured side.[6]
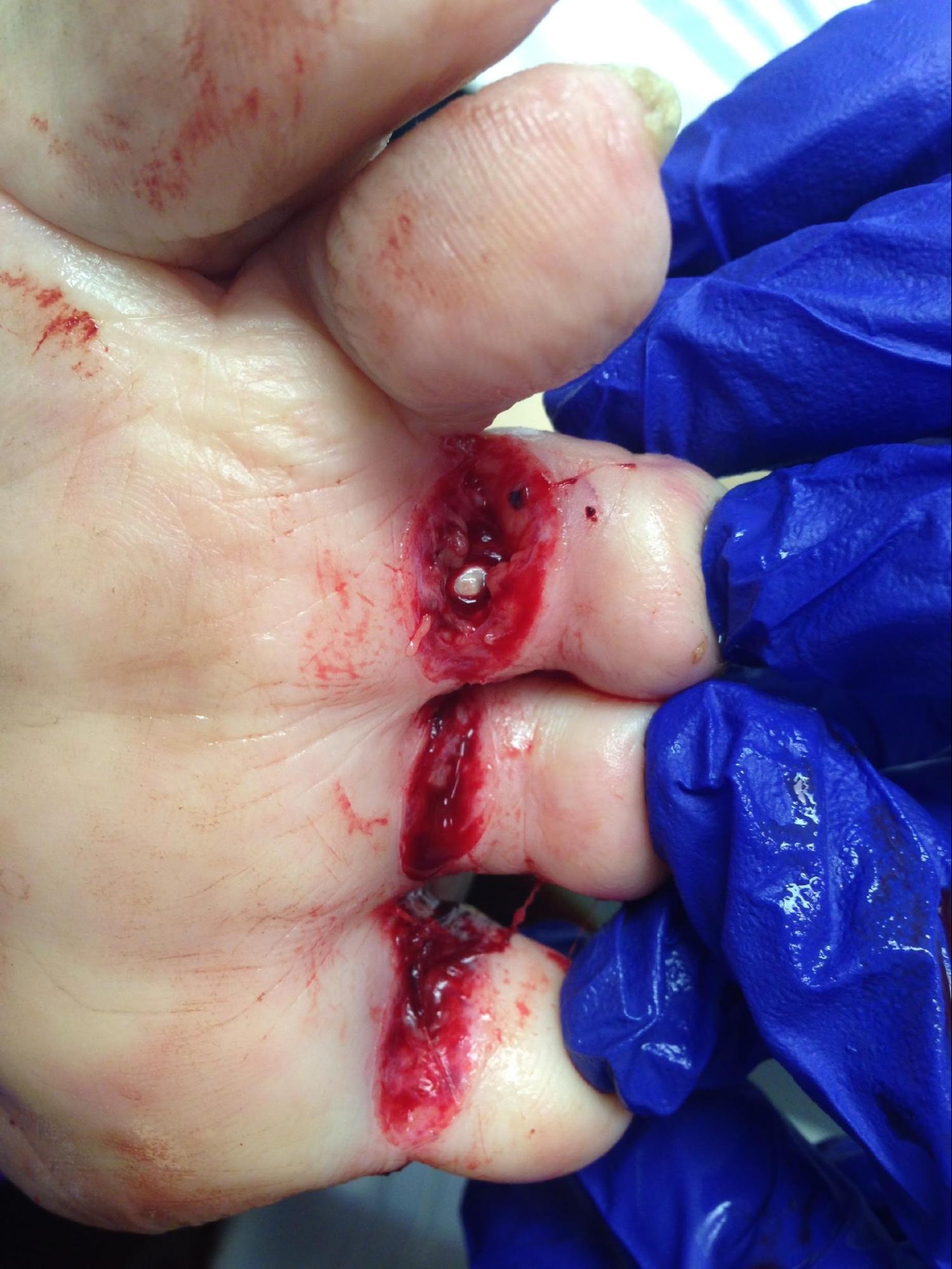
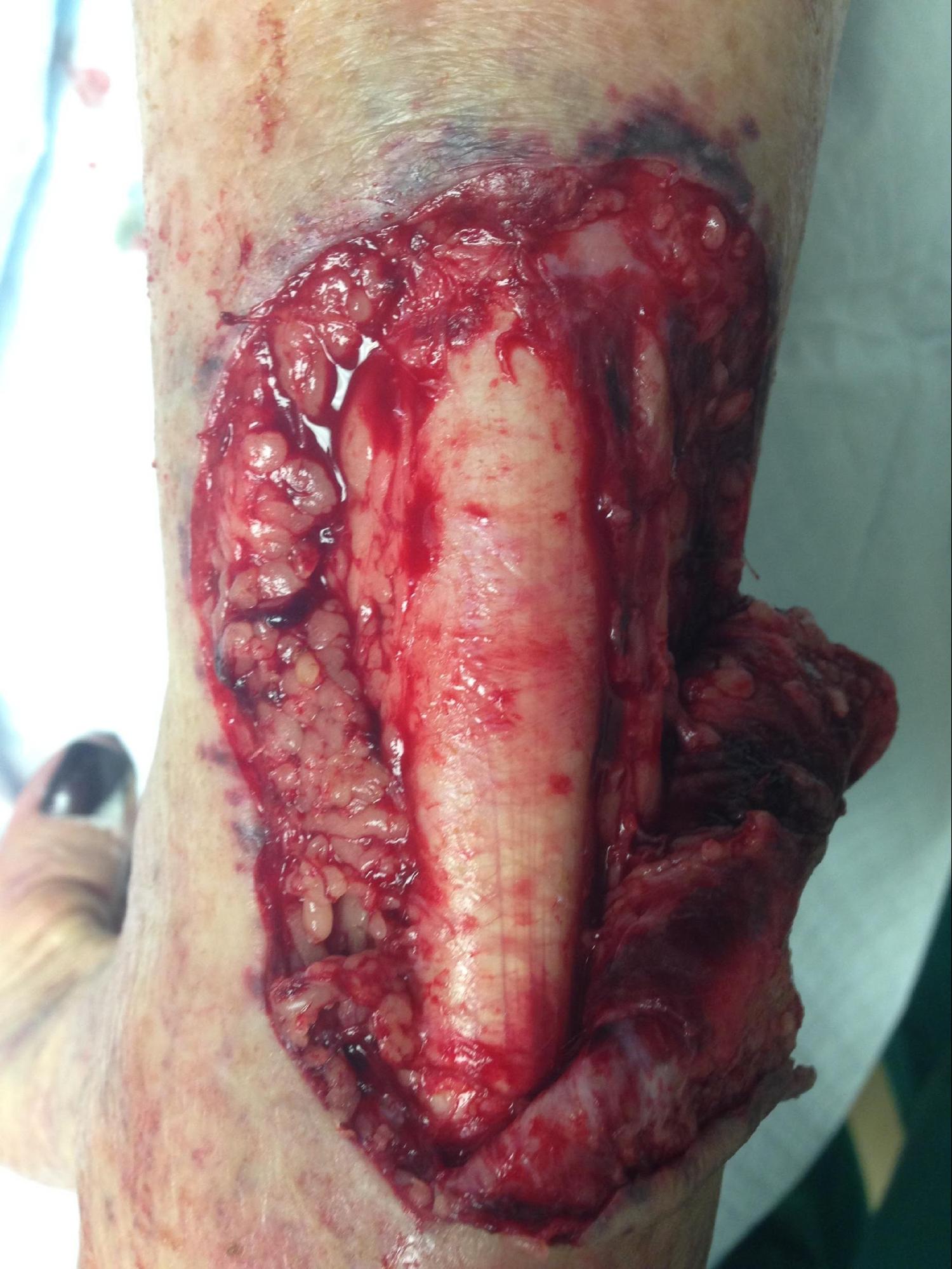
- Detailed musculoskeletal exam: Examine any joints involved in the laceration for injury, along with an active and passive range of motion exam above and below the joint to assess for tendon injury (see Image. Laceration of the Posterior Ankle Exposing the Achilles Tendon).
- Detailed Vascular exam: Assess capillary refill in the distal to the wound if on the extremities, and compare to noninjured side always. If accessible, Doppler ultrasound can be utilized to assess underlying vascular integrity, following from above the laceration to below.
- Foreign bodies, if observed, should be removed, as they can increase the patient's risk of infection or poor wound healing. If there is any concern about retained foreign bodies, imaging should be obtained.
Contraindications
Contraindications to the repair of a laceration include:
- Bite wounds of any type
- Overt infections of the nearby skin
- Lacerations greater than 24 hours old
Equipment
The equipment required for the closure of lacerations can vary depending on the location and characteristics of the wound. Necessary supplies required for any laceration repair include but are not limited to the local anesthetic drawn up with a small gauge needle (greater than 27 gauge), needle holders, forceps, scissors, gauze, and the appropriate closure device (suture, staple, glue) for the wound.
The selection of local anesthetic is dependent on patient allergies, accessibility, and location of the injury. True allergies to anesthetics are rare. If there is a concern for amide allergies, the use of ester anesthetics or preservative-free amides should be options as reactivity is thought to be due to the preservatives. The use of epinephrine with local anesthetic was previously cautioned in fingers, toes, nose, penis, and ears. However, current research shows the concerns of local ischemia to be unsupported.[7]
The selection of repair material varies based on the location, depth, length, and width of the laceration. The decision between absorbable and nonabsorbable sutures will depend on the depth and method planned for closure. Current studies have shown that the selection of absorbable gut vs. nonabsorbable suture materials in the external closure of lacerations produces similar infection rates and aesthetic outcomes over the long term.[8]
The use of staples for the closure of scalp lacerations is a quick and secure method of care.
The use of staples for the closure of scalp lacerations is a quick and secure method of care. Due to the higher risk of scarring, staples should only be used on thicker skin and when appropriate, follow up can be obtained for their removal.[9] The use of tissue adhesives can be an option when the laceration overlies an area with minimal tension and is easily approximated. The most significant concern for their use is the successful closure of the wound, which hinges on appropriate cleaning and preparation of the wound. Steri-strips are another alternative for primary closure of lacerations with no tension and not overlying a joint, but due to the requirement of added adhesives such as benzoin, there is a risk of local skin reaction that reduces their functionality for lacerations care.[10]
Also of note, the use of sterile vs. nonsterile gloves has been examined by many studies, and found that due to the contaminated nature of lacerations at presentation, there is no statistical difference in infection with the use of nonsterile gloves.[11]
Personnel
The personnel requirements for the primary closure of a laceration vary based on the complexity of the wound. In the most basic of repairs, a single provider can perform the technique alone. As the complexity of the laceration increases, there may be an increased need for other personnel to hold pressure, manage supplies, and reduce tension across the wound.
Preparation
A helpful mnemonic in preparing for any laceration is LACERATE[12]:
- L - Look at the wound to assess repair options
- A - Anesthetize the wound
- C - Clean the wound
- E - Equipment setup
- R - Repair the wound
- A - Assess the results, anticipate complications
- T - Tetanus Immunization
- E - Educate the patient about wound care
Careful step-by-step planning of the procedure and gathering of all the required supplies ahead of time can aid in reducing the duration and difficulty of any closure. Preparation of the room in which the procedure will take place by turning on lights, moving trays and tables, positioning the patient's bed, and localizing waste receptacles all aid in reducing the risk of contamination during the procedure.
Technique or Treatment
Local anesthesia is used to clean and repair lacerations appropriately. Selection of the anesthetic, as stated previously, will depend on patient allergies and accessibility at the care facility. Several steps can be taken to reduce patient discomfort while administering the local anesthetic, such as:
- Buffering the solution at a rate of 9 mL of lidocaine to 1 ml of 8.4% sodium bicarbonate.[13]
- Warming the anesthetic to body temperature.[14]
- Utilizing small needles (greater than 27 gauge) for the administration of the anesthetic.
- Infusing the anesthetic slowly.
- Injecting through the edges of clean wounds vs. new punctures.[15]
- Utilizing topical anesthetics such as EMLA (eutectic mixture of local anesthetics) cream or TAC solutions (tetracaine, adrenaline, and cocaine) before infiltration with a local anesthetic.[16]
- Placing ice contained within a sterile glove over the injection site for 2 minutes before injection has been found to reduce pain from the local anesthetic.[17]
After local anesthesia, the next step is irrigation of the wound to remove any foreign objects and clotted blood, allowing for complete visualization of the laceration. Most commonly performed utilizing a saline solution, some research has shown that in simple lacerations on healthy immunocompetent patients, tap water can be utilized to irrigate the wound.[18]
Following irrigation, the laceration can now be closed using whichever method best suits its location and size. If suturing, there is no specific guide for which technique to use, but general technique recommendations are as follows:
- Simple interrupted sutures are versatile and the right choice for most wounds.
- Horizontal/ Vertical mattress sutures are both utilized to evert wound edges but have an increased risk of scar formation.
- Deep sutures can be employed to reduce tension on the superficial sutures and help reduce future scarring, but care must be taken to ensure the wound is clean before placing deep sutures due to the increased risk of infection.
Following primary closure, placement of either antibiotic ointment or petroleum-infused gauze over the sutures with overlying gauze affixed by tape is advised. [19] Educate patients on keeping the wound clean and give follow-up instructions for when they can have the sutures removed. General guidelines for removal vary depending on the location of repair, the complexity of repair, and suture utilized. Sutures left in place too long can increase the risk of infection and scarring.
- General suture removal timelines:
- Face: 3 to 5 days
- Scalp and arms: 7 to 10 days
- Trunk, Legs, hands, and feet: 10 to 14 days
- Palms or soles: 14 to 21 days
Complications
- Missed foreign bodies
- Missed tendon injuries
- Missed nerve injuries
- Infections
- Dehiscence of the wound[20]
Clinical Significance
Lacerations are a common chief complaint of patients, and their management must be well understood by the healthcare team to provide appropriate care to patients.
Enhancing Healthcare Team Outcomes
Lacerations are seen and managed by many clinicians, including nurse practitioners. However, only those professionals with anatomical and basic surgical knowledge should close lacerations. Even the most simple laceration can become infected or develop into a keloid. Before closing any laceration, the wound must be clean.
Laceration presentation can vary drastically, and while the primary care team can manage simple lacerations, the below guidelines should aid team decision making on when to consult general surgery or other specialty services.
- Guidelines for when to seek surgical consultation:
- Deep wounds of hands or feet
- Full-thickness lacerations of eyelid, lip, or ear
- Lacerations involving nerves, arteries, bones, or joints
- Penetrating wounds of unknown depth
- Severe crush injuries
- Severely contaminated wounds requiring drainage
- Wounds with substantial concern about the cosmetic outcome[21]
There are many instances where a laceration may not be safe to close, and in such situations, a wound care nurse should be involved to follow the patient. These patients require education about wound care and dressing changes. If the nurse notices complications such as infection or dehiscence, they should refer the patient back to the clinician.
Nursing can work with applying and/or changing wound dressings and administering medication for pain control and antimicrobial agents. Pharmacists can make antibiotic recommendations as well as for pain and perform medication reconciliation. If they become infected, the pharmacist should make antibiotic recommendations to the clinician based on local resistance as well as custom and practice.
The outcomes of laceration repair depend on the mechanism, location, and complexity. For optimal outcomes, prompt consultation with a specialist is recommended, and an interprofessional team approach must be leveraged for the best patient care and good outcomes. [Level 5]
Nursing, Allied Health, and Interprofessional Team Interventions
The prompt collection and dissemination of pertinent patient history can aid the healthcare team in assessing the severity of the laceration. The understanding of how to appropriately aid in hemostasis through direct pressure can significantly aid in the complete assessment of the patient. Nurses also play a vital role in dressing change, wound care, and timely removal of sutures/staples.
Nursing, Allied Health, and Interprofessional Team Monitoring
Nurses should monitor patients for the following signs:
- Hypotension (weakness, dizziness, pallor)
- Infection (fever, erythema, gross puss)
- Neurovascular injury (paresthesias, distal weakness, pulselessness, numbness)
- Signs of wound infection
- Adverse effects of the local anesthetic