Continuing Education Activity
There are many different indications for hand splinting. These include phalanx fractures, conditions requiring immobilization of the metacarpophalangeal and distal interphalangeal joints, metacarpal fractures, thumb strains, and de Quervain syndrome. Some commonly used types of hand splints include dorsal distal phalanx splints, hairpin splints, dynamic finger splints, ulnar gutter splints, radial gutter splints, dorsal splints with extension hoods, and thumb spica splints. If there are open fractures present, an orthopedic referral is needed for evaluation and should not be delayed by splint placement. This activity reviews the indications for hand splints and highlights the role of the interprofessional team in the management of affected patients.
Objectives:
- Review the indications for a hand splint.
- Explain how a hand splint is applied.
- Describe potential complications of hand splints.
- Outline interprofessional team strategies for enhancing care coordination and communication to advance the treatment of hand disorders with hand splints and improve outcomes.
Introduction
The hand is very versatile in its abilities. To assure that it functions at its highest level, it is important to maintain its functionality and mobility.
Anatomy and Physiology
The hand consists of five digits. These are numbered one through five, starting with the thumb as digit one and the little finger digit five. The metacarpals articulate with the wrist bones and are numbered in a similar fashion to the digits. Digits two through four have three phalanges: proximal phalanx, intermediate phalanx, and distal phalanx. The first digit has a proximal and distal phalange. The metacarpophalangeal joint (MCP) is the articulation between the metacarpal bone and the proximal phalanx. The proximal interphalangeal joint (PIP) is the articulation between the proximal phalanx and the intermediate phalanx. The distal interphalangeal joint (DIP) is the articulation between the intermediate phalanx and the distal phalanx. The flexor tendons are on the volar aspect of the hand. The flexor digitorum profundus inserts on the distal phalanx. The flexor digitorum superficialis inserts on the intermediate phalanx. The extensor tendons run on the dorsal aspect of the hand. The extensor digitorum has a median band that attaches to the intermediate phalanx, and two lateral bands that attach to the distal phalanx.
Indications
There are many different indications for hand splinting. Phalanx fractures have a variety of splinting options. Splints are needed to treat fractures of the distal phalanx as well as avulsion fractures at the distal phalanx. Dorsal distal phalanx and hairpin splints are designed to immobilize the distal phalanx in these situations. Dorsal and volar finger splints are used to immobilize the digit from the MCP joint to the DIP joint. Dynamic finger splinting is used to provide immobilization and support to the injured digit while allowing mobility at the MCP and PIP joint of the uninjured digit. The ulnar gutter splint is used for phalanx and metacarpal fractures that are on the medial (ulnar nerve distribution) of the hand. Radial gutter splints are used to treat phalanx and metacarpal fractures on the lateral aspect of the hand, often second and third digits. When there are multiple metacarpal or phalanx fractures, a dorsal splint with extension hood can be placed. Thumb spica splints should be used for first metacarpal and phalanx fractures as well as thumb strains and de Quervain syndrome.[1][2][3][4]
Contraindications
There are few contraindications associated with splinting the hand. If there are open fractures present, an orthopedic referral is needed for evaluation. Do not delay orthopedic referral due to splint placement.
Personnel
Often, splinting can be performed by one person. An assistant, however, is generally helpful.
Preparation
Before the hand is immobilized, it is important to confirm that the fracture has been sufficiently reduced if indicated. This is most commonly done with radiographic verification of reduction. Please place all equipment at the bedside. Again, any open fractures need an orthopedic consultation.
Technique or Treatment
General Overview
All splints need to be properly placed and dressed. A soft cotton bandage, such as Webril, is placed on the skin to prevent any skin breakdown and to allow room in the splint for any inflammatory processes to complete their course. Separate the digits by placing 4 x 4 gauze between each finger. The plaster, such as ortho-glass, is then placed against the cotton bandage. The plaster should be soaked in water and then excess water removed before application. An elastic band is wrapped around the injured area that will hold that bandage and plaster in place. The elastic band is then secured in place. The splint should be held in the position of best reduction until the plaster hardens. [5][6][7][8]
Dorsal Distal Phalanx Splints
A metallic splint with sponge rubber padding is placed on the dorsal aspect of the digit spanning the fracture site. It is recommended that the digit is splinted in full extension.
Hairpin Splint
A thin piece of metal is placed covering the distal phalanx. This is not a structurally supportive splint. This splint functions better to protect the distal end of the finger from further injury.
Dynamic Finger Splinting
Using a metallic splint with sponge rubber padding splint the injured finger side by side with an adjacent uninjured finger. The two digits are taped together for immobilization.
Ulnar Gutter Splint
A soft cotton bandage is placed from the distal palmar crease extending to the mid-forearm. The first, second, and third digits are generally not immobilized with this splint. Plaster is then cut to the same length and placed on the medial (ulnar nerve distribution) side of the hand. The plaster is placed laterally, extending to the volar and dorsal aspects of the hand. The plaster should extend far enough to immobilize the fourth and fifth digits. The MCP joint should be flexed 50 to 90 degrees. The DIP and PIP joints are splinted in extension.
Radial Gutter Splint
A soft cotton bandage is placed from the distal palmar crease extending to the mid-forearm. The fourth and fifth digits are not generally immobilized with this splint. Plaster is cut to the same length and placed on the medial side of the hand (median nerve distribution). An opening needs to be made in the plaster for the thumb. The splint is placed laterally extending to the volar and dorsal aspects of the hand. The plaster should extend far enough to immobilize the second and third digits. The MCP joint should be flexed 50 to 90 degrees. The DIP and PIP joints are splinted in extension.
Dorsal Splint With Extension Hood
A soft cotton bandage is placed from the DIP joint to the mid-forearm, sparing the thumb. In a dorsal forearm splint, plaster is placed to extend and cover the second, third, fourth, and fifth digits. The plaster should extend past the DIP joint. The MCP joint is splinted in in 50 to 90 degrees of flexion. The PIP and DIP joints are splinted in extension. An elastic bandage is placed over the splint.
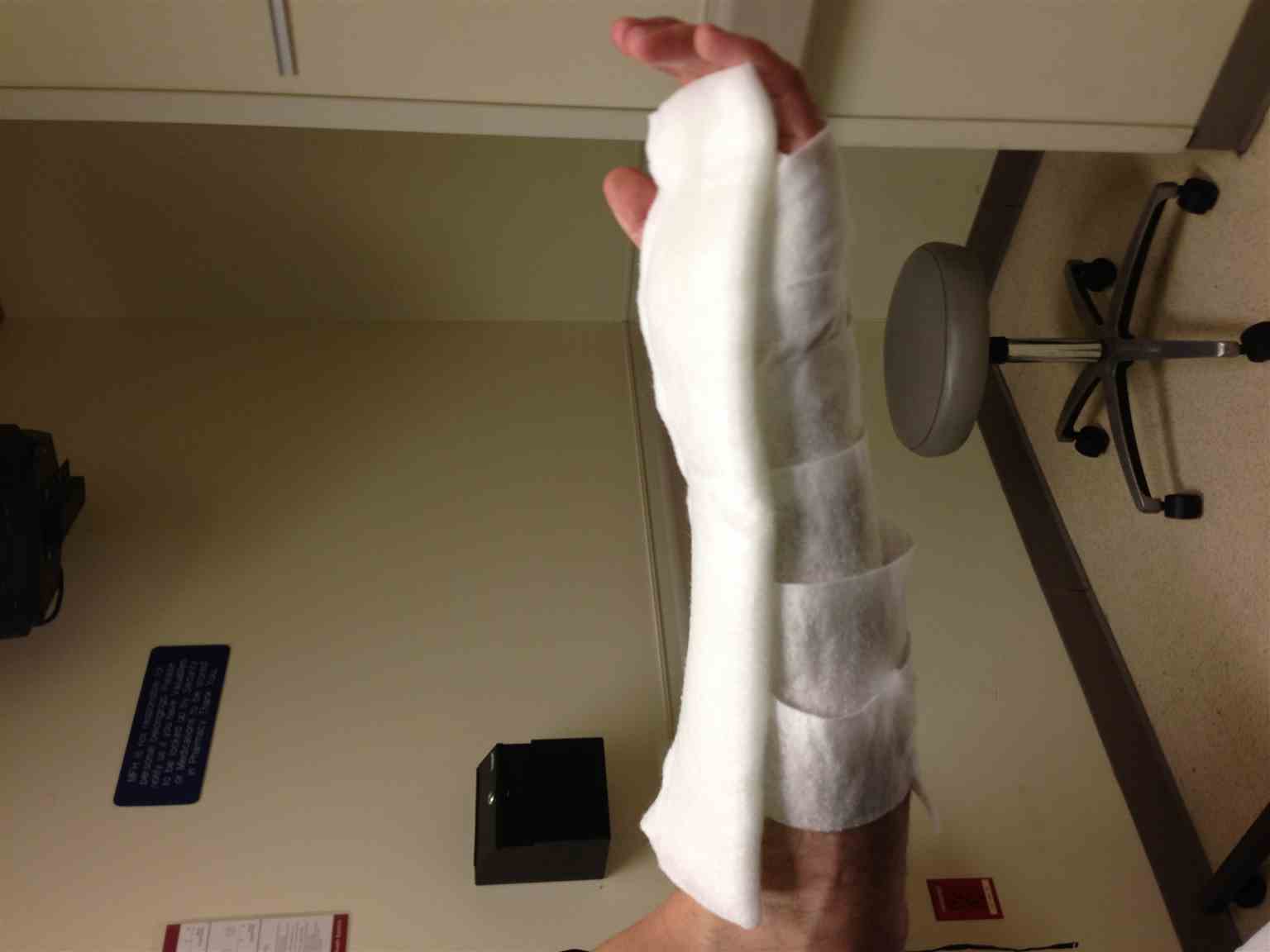
Thumb Spica Splint
A soft cotton bandage is placed from the mid-hand to the mid-forearm. A stockinet is placed over the thumb in order to protect from friction due to the plaster. Plaster is placed encompassing the thumb to the mid-forearm. The hand is positioned as if holding a can of soda; this is with the thumb abducted with the first interphalangeal joint in extension. The plaster should extend past the interphalangeal joint in order to fully immobilize the thumb. The wrist is splinted in a neutral position.
Complications
There are many complications that are associated with splint application. Inflammation and swelling of injuries can cause compartment syndrome, nerve impingement, pressure sores, skin breakdown, skin infection, and vascular compromise. Soft cotton bandages should also be placed on the skin to prevent any thermal injury from plaster reaction after the plaster has been soaked in water.
Clinical Significance
It is imperative that hand injuries are splinted with proper technique. As the proper technique is followed, the versatile capabilities of the hand are preserved, nerve impingements are avoided, and the full range of motion is retained. In certain settings, evaluation by an orthopedic specialist is not readily available and the hand should be splinted to prevent further injury prior to a proper follow-up appointment.
Enhancing Healthcare Team Outcomes
Hand splints are used to treat many disorders and can be effective for symptom relief. However, all healthcare workers including therapists and nurses who apply hand splints should ensure that the patient has close followu up. Hand splints can be associated with many complications, which if neglected can lead to malpractice litigation. At discharge the patient should be provided with thorough instructions on follow up, symptoms to observe and when to retrun to the emergency department.