Continuing Education Activity
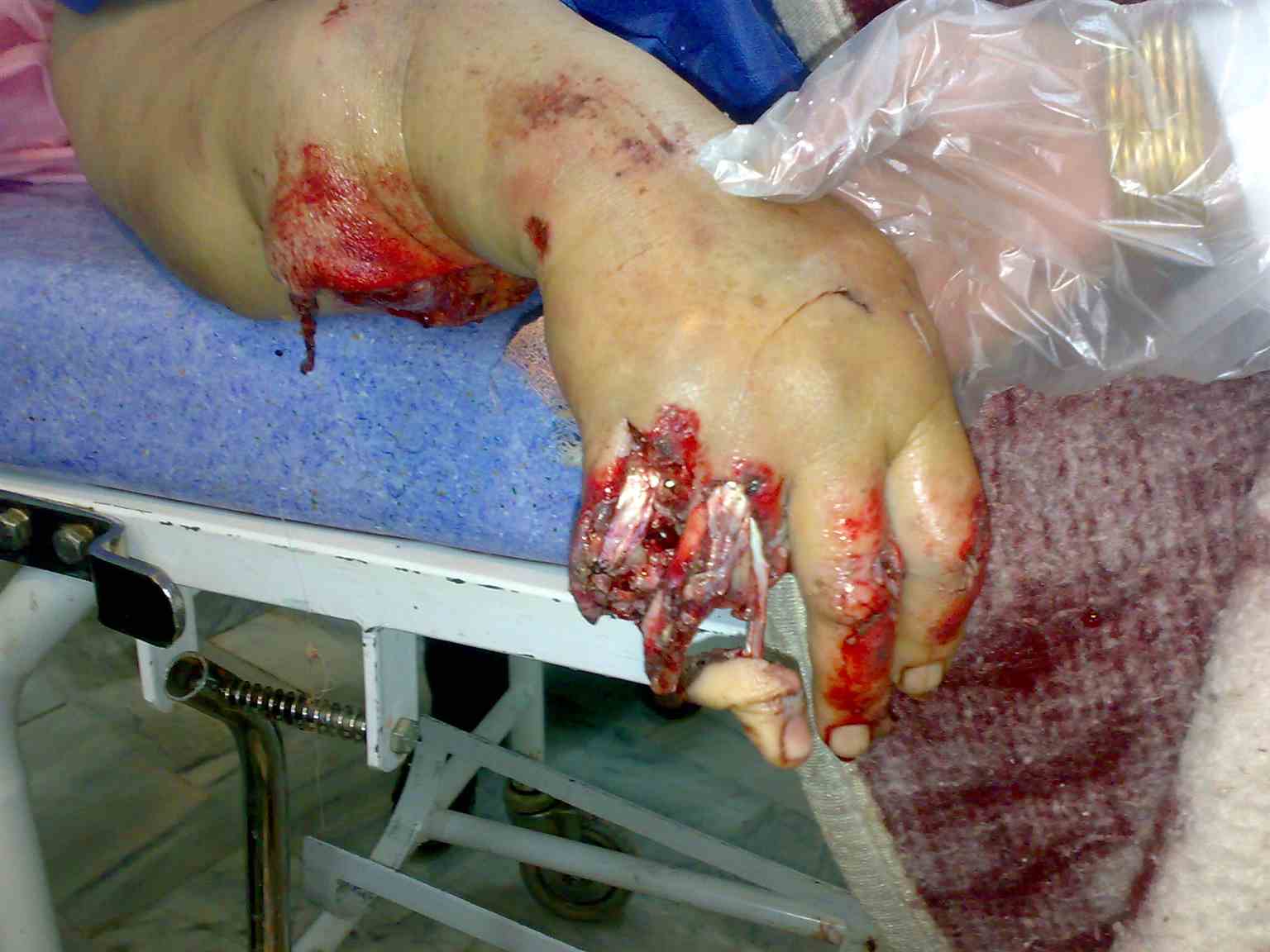
Upper extremity amputations are a procedure commonly done in a variety of circumstances including infection, trauma, cancer, disease progression or congenital malformations. The level at which the amputation occurs can greatly impact a patient's outcomes and level of care required by health care professionals. This activity aims to review anatomy, indications, surgical techniques and special considerations/complications that may arise so that an interprofessional team may provide optimal care to patients who may need this procedure.
Objectives:
- Describe the functional anatomy of each level of upper extremity amputation.
- Review the complications that may occur postoperatively in amputees and methods of treatment.
- Summarize the epidemiology of upper extremity amputations.
- Explain the importance of an interprofessional approach when caring for patients with upper extremity amputations.
Introduction
The prevalence of amputations was 1.6 million in 2005, with projections that the prevalence may double by the year 2050.[1] Part of this increase, after years of decline, might be related to the diabetes epidemic that will eventually force amputation in some patients. The risk of limb loss increases with age (greatest risk is age 65 and above). For upper limb amputations, trauma is the leading cause, accounting for 80% of acquired amputations, occurring in men aged 15 to 45 years. Second most prevalent is cancer/tumors and vascular complications of diseases. Amputations are named by the level at which they have been performed. In ascending order, there is trans-phalangeal, trans-metacarpal, trans-carpal, wrist disarticulation, trans-radial, elbow disarticulation, trans-humeral, shoulder disarticulation, and forequarter amputation. Trans-phalangeal accounts for 78% of all upper extremity amputations. Although various clinical considerations exist, depending on the level of amputation; ultimately the goal in any amputation is to save all feasible length as this directly correlates with improved functional status.[2][3]
Anatomy and Physiology
The upper extremity is a highly complex limb with neurovascular bundles, lymphatics, muscles and bones that come together and form a functional appendage to perform our daily activities. For the scope of this article, the focus will be on the bony structures and anatomical considerations as pertaining to upper limb amputations.
Shoulder
The shoulder is composed of the clavicle and scapula which articulates with the proximal humerus. The joints that occur are the sternoclavicular, acromioclavicular, scapulothoracic and glenohumeral joint. The intrinsic muscles that hold the scapula and clavicle to the humerus include the deltoid, teres major, supraspinatus, infraspinatus, teres minor, subscapularis, trapezius, latissimus dorsi, levator scapulae, rhomboid major, rhomboid minor, serratus anterior, pectoralis minor, subclavius, coracobrachialis, biceps brachii, and triceps brachii. Nerve innervations into all these muscles arise from C5 through T1 which form the brachial plexus.[4] Three types of upper limb amputations occur in this area. First, the forequarter amputation involves the resection of the clavicle and all structures distally.[5] Next is shoulder disarticulation, which involves complete removal of the humerus from the glenoid. When possible, the scapula should be retained to prevent disfigurement of the back. Additionally, rotator cuff tendons should be sutured together over the glenoid wing. The deltoid should be attached to the inferior glenoid and lateral scapular border to fill the subacromial space. Lastly, transhumeral amputations can occur at any length of the humerus.[6][7]
Elbow
The elbow is a non-weight bearing synovial hinge joint consisting of articulations between the humerus, radius, and ulna. The joints that occur here are the ulnohumeral, radiohumeral and radioulnar. Stability of the elbow comes from the trochlea of the humerus articulating with the ulnar olecranon allowing for flexion and extension of the joint. Further stability is maintained by the medial collateral ligament and lateral collateral ligament. The crossover of multiple muscles over the joint further allows for pronation and supination of the forearm. Nervous innervation at the level of the elbow includes several nerves. The musculocutaneous nerve innervates the biceps brachii. The radial nerve innervates five muscles including the lateral brachialis, anconeus, supinator, brachioradialis and triceps brachii. The ulnar nerve and median nerve innervate forearm and hand muscles.[8] The amputation occurring in this region is elbow disarticulations. Elbow disarticulations involve removing the radius and ulna completely from the humerus.[7]
Forearm
Trans-radial amputations happen at this level. The muscles of the forearm are divided into intrinsic and extrinsic muscles. The intrinsic muscles pronate and supinate the radius and ulna for the full range of motion of 180 degrees to occur. The extrinsic muscles flex and extend the digits of the hand. Overall, there are twenty muscles of the forearm, split into the anterior flexor compartments and posterior flexor compartments. Additionally, the biceps tendon normally attaches to the radial tuberosity of the radius. The main nerves in this region are the median, ulnar and radial nerves. The median nerve has a branch called the anterior interosseous nerve which innervates the flexor pollicis longus and partially the flexor digitorum profundus. The radial nerve branches into the posterior interosseous nerve which supplies the supinator, extensor muscles, and abductor pollicis longus.[9] Transradial amputations can further classify into very short, short, medium and long; based on the length preserved.[7]
Wrist
The wrist is composed of two rows (proximal and distal) of carpal bones. The proximal 4 bones are the scaphoid, lunate, triquetrum and pisiform which articulate with the radius and ulna for wrist motion. The distal row includes the trapezium, trapezoid, capitate, and hamate.[10] The palmar and dorsal radiocarpal ligaments, as well as the ulnar and radial collateral ligaments, provide joint stability.[11] A wrist disarticulation involves the removal of the carpal bones and all structures distally.
Hand
The remainder of the hand is five sets of bones that make up the palm and each of the five digits. The metacarpal bones articulate with the carpal bones proximally. Moving more distally, the metacarpals articulate with the proximal phalanges, followed by the intermediate phalanges in digits 2 to 5 and finally the distal phalanges. Nerves in this area are the median, radial and ulnar nerve. The median nerve branches into the recurrent branch to supply the thenar eminence. The remainder of the median nerve branches to form the palmar digital nerves of the first three digits. The ulnar nerve branches to form the deep branch and superficial branch, innervating muscles of the fourth and fifth digit. The radial nerve branches into the superficial radial nerve which innervates the first three and a half digits. The other branch of the radial nerve is the posterior interosseous branch. The muscles in between the metacarpals are the dorsal and palmar interossei muscles which are responsible for finger spreading. The hypothenar muscles are formed by the abductor digiti minimi, the flexor digiti minimi and the opponens digiti minimi that allow the fifth digit motion towards the thumb and also flexion of the MCP joint. The lumbricals attach from the metacarpals to the proximal phalanges and permit the fingers to straighten and flex the MCP joints.[12] Amputations in this region can involve distal tip removal, intermediate phalanges removal or proximal phalanges removal.[13]
Indications
- Trauma beyond repair
- Irreparable loss of the blood supply
- Malignancy
- Severe contracture
- Infection
- Congenital deformities
- Burns
- Thermal/electrical injury
- Frostbite
- Peripheral Vascular disease
- Complications from diabetes
Contraindications
Hemodynamic instability
Better functional status with the limb, without risk of a worsening condition.[14]
Personnel
Various health care specialists are involved in the various phases of limb amputation and rehabilitation. An internist, physiatrist, vascular surgeon or an orthopedic surgeon can all perform initial evaluations. Surgeons from a variety of fields such as orthopedics, vascular, general surgery may become involved based on the complexity of the procedure. Plastic surgeons assist in providing an aesthetically pleasing result. Postoperatively, wound care physicians and infectious disease specialists may be called in for cases of delayed wound healing, wound dehiscence or infection. For rehabilitation; occupational therapists, physical therapists, and physiatrists play an essential role in optimizing functional outcomes. Prosthetists will help fit a patient for a prosthesis suited to their lifestyle. Psychologists and psychiatrists may play a role in emotional counseling after limb loss.
Preparation
From a surgical point of view, standard sterile gowning and draping procedures should be standard procedure when performing an amputation in the operating room setting[15] Pre-operatively, it is standard procedure to use antibiotics for surgical resection of long bones.[16] Common choices include vancomycin or first-generation cephalosporins, but others may be added depending on the injury.[17] For smaller injuries and amputations such as traumatic fingertip amputation, current research is unclear on the efficacy of prophylactic antibiotics.[18] However, antibiotics may still be used at the surgeon's discretion.
Technique or Treatment
Surgical techniques will vary based on the disease pathologies in the area, anatomical variations and unanticipated complications that may arise during surgery. This discussion will focus on the main approaches and principles used in each type of upper extremity amputation, moving distally to proximal.
Transcarpal
Transcarpal amputations are a common type of amputation and occur due to a variety of reasons including trauma, peripheral vascular issues, and infection. It is preferable to more proximal amputations because flexion and extension of the wrist are preserved, improving overall function. In most cases, the initial incision results in a long full thickness palmar flap and a shorter dorsal flap at a 2 to 1 ratio. The finger flexor and extensor tendons are separated from their distal insertions and allowed to retract into the proximal wound. The median and ulnar nerves are sectioned and retract deep into the proximal site where more padding is available to cushion if neuroma formation occurs postoperatively. From a vascular point of view, the radial and ulnar arteries and their branches are ligated just proximal to the surgical site. The bone of the intended carpals is removed. Rough edges are smoothened and closure is done with padding from the finger tendons, when possible. Performing a thumb amputation will cause a patient to lose pinch and grasp and should be done with functional consideration in mind.
Wrist Disarticulation
A wrist disarticulation is preferred over any shorter amputations, but it is noted that finger dexterity and wrist flexion/extension are sacrificed. An incision is made circumferentially starting and ending 1.5cm distal to the radial and ulnar styloid processes respectively. The arteries and nerves are ligated similar to a trans-carpal amputation. Louis, Hunter, and Keating describe a technique to decrease the risk of a post-operative neuroma. This involves starting just distal to the cubital fossa and extending an incision proximally. Double ligation of the median, ulnar and superficial radial nerves are done at this level to coax neuroma formation away from the future site of the prosthetic wall.[19] It is also important to preserve the triangular fibrocartilage and avoid damage to the distal radioulnar joint during the disarticulation because this can affect pronation and supination in the future. Once the wrist is disarticulated, the protruding lateral edges of the radius and ulna may be shaped to allow for better closure. This is ultimately closed with the remaining full thickness palmar flap and the short dorsal flap that is made in a 2 to 1 ratio to provide appropriate padding and wound healing.
Transradial
Forearm length preservation is essential to allow some degree of pronation and supination as well as a greater arc of motion. The underlying soft tissue of the forearm contains relatively avascular structures such as fascia and tendon creating suboptimal padding of the residual limb. Thus, flaps are generally created at a 1 to 1 ratio and reflected proximally. Vessels, nerves and muscle bellies are transected similar to the methods above. For prosthetic fitting, it is preferable to have at least 4cm of the ulna preserved. In some cases, transposing the biceps tendon to the proximal ulna to help the resting approximation is helpful in preserving elbow flexion.
Transhumeral and Elbow disarticulations
For an elbow disarticulation, two incisions for skip flaps are made, starting at the humeral epicondyles and stopping at approximately 3cm distal to the tip of the olecranon posteriorly and just distal to the insertion of the biceps tendon anteriorly. The lacertus fibrosus is divided which exposes the neurovascular bundle underneath and releases all the pronator attachments from the medial epicondyle. The radial nerve is found between the brachialis and brachioradialis and transected. The ulnar nerve is similarly transected, and both nerves are allowed to retract into the proximal wound. The extensor muscles are transected about 7cm distal to the joint. The anterior, radiohumeral and ulnohumeral capsules are then divided, and forearm is disarticulated. The posterior flap is moved medially and sutured to the soft tissues of the medial epicondyle. Of note, the posterior flap made to be longer than the anterior skip flap to provide adequate padding at the humeral end. For patients with smaller muscle mass and subcutaneous tissues, the humerus may be covered with a flap of brachialis, biceps or triceps.
Transhumeral amputations are similar to an elbow disarticulation with a few important considerations. Amputations are typically made 4 cm proximal to the elbow joint to allow for the prosthetic elbow lock mechanisms to appear equal to normal elbow location of the opposite arm. Two incisions creating an anterior and posterior flap are again created. Neurovascular structures are identified and divided similarly to elbow disarticulations. Extensor muscles are resected about 7cm distal to the joint line to again create a posterior flap that is longer than the anterior flap for appropriate padding and closure.
Transhumeral amputations at or above the pec major insertion up to the level of surgical neck of the humerus, function as a shoulder disarticulation because the rotation of the humerus will no longer be possible, but it still may be preferable to complete shoulder disarticulation since the shoulder contour is preserved. The technique for this amputation requires a patient to be in “beach chair” or “sloppy lateral decubitus” position which gives easy access to both anterior and posterior shoulder. The incision starts at the anterior coracoid, which outlines the inferior to the superior curve of the deltoid to its posterior insertion. A second incision is made crossing the axilla to connect the two ends of the first incision. The humeral insertions of the deltoid and pec major are freed. Underlying them is pec minor which remains attached to the coracoid and coracobrachialis which is removed from the origin to expose the neurovascular bundle and branches of the brachial plexus. In specific, the axillary artery, radial, ulnar, median and musculocutaneous nerves are isolated and resected to allow retraction deep to pec minor. The axillary nerve innervation to the deltoid is carefully left intact to help preserve the deltoid muscle bulk for residual limb padding and prosthetic fit. Teres major and latissimus dorsi are divided near their insertions of the bicipital groove. The humerus is then cut and rounded. The final flap covering the head of the humerus consists of the long head of triceps, both heads of biceps and coracobrachialis. Pec major is pulled laterally and attached to the humerus. The deltoid flap covers the rest of the humerus and is attached to the axilla. All flaps are mindfully attached with appropriate tension and to allow for optimal aesthetic healing.
Shoulder disarticulation
This amputation is performed similar to a humeral amputation above the level of pec major, with some considerations. Once the incisions are made, muscle insertions are freed appropriately on the humerus and neurovascular bundles are exposed; then the axillary artery is ligated and divided. The acromial branch of the thoracoacromial artery that course towards the acromion is also ligated and retracts. Short external rotator muscles are exposed and subsequently divided by placing the arm in full internal rotation. Conversely, extreme external rotation allows dissection of the anterior capsule and subscapularis. Once the humeral head is disarticulated from the joint, all the exposed muscles are secured in the glenoid cavity to fill the hollow space and flaps are smoothened as needed to obtain desirable shoulder contour
Forequarter (Interscapulothoracic) amputation
This amputation involves removing the full upper limb and shoulder joint from the scapula and thoracic wall. This extensive procedure is indicated mostly in patients with malignant tumors that infiltrate the shoulder muscles or severe trauma. There are 2 approaches, anterior and posterior.
The anterior approach starts with an incision from the lateral border of the sternocleidomastoid, extending laterally across the clavicle, crossing the acromioclavicular joint and the superior scapular spine. The incision then goes inferiorly along the vertical border of the scapula to the scapular angle. The lower part of the incision begins at the middle third of the clavicle and progresses along the deltopectoral groove and connects to the upper part of the incision at the angle of the scapula. The clavicular portion of the pectoralis major is reflected to expose the clavicle, and the external jugular vein is retracted from the field. The clavicle is resected at the lateral sternocleidomastoid to preserve the contour of the neck. Disarticulation occurs at the acromioclavicular joint. An incision is made in the medial subclavian muscle to release insertions of the pectoralis major and minor to further expose the subclavian artery and vein, which are subsequently ligated. The brachial plexus is dissected and sectioned to allow retraction superiorly. Further muscles and soft tissue that hold the shoulder joint to the chest wall are separated, and limb is removed. The closure is done by suturing the remaining muscles, including the pectoralis major and trapezius over the lateral chest wall for additional padding.
The more popular posterior approach allows for easy mobilization of the limb and gain of vascular control before the more challenging anterior dissection occurs. First, a posterior cervicoscapular incision is made to expose the underlying muscle groups. The trapezius, latissimus dorsi, and superior scapular attachments are divided. Cauterization of the transverse cervical and scapular arteries is done as they are exposed. The medial subclavian muscle is divided to expose the clavicle which is then resected from the lateral border of the sternocleidomastoid. A second pectoroaxillary incision is made to expose the pectoralis major and minor which are further divided. The brachial plexus is again dissected out, the shoulder joint is disarticulated, and the upper limb is removed. The closure is similar to the anterior approach.[20]
Target Muscle Reinnervation
Target muscle reinnervation (TMR) is a surgical technique that applies to all upper extremity amputation patients that are candidates for a myoelectric prosthesis. This technique involves taking motor nerves that are transected during an amputation and attaching them to the motor nerves of muscles remaining in the upper extremity or trunk. This procedure is typically done during the amputation itself but is possible during revision surgeries as well. It allows for reinnervation of new target muscles so that signals may transmit to the prosthesis and the patient can use it intuitively. If the amputation is done in such a way that there are few residual muscles, then TMR may be performed on trunk muscles instead.[21]
Complications
- Phantom limb pain/sensations: A feeling of pain or sensations in the “missing limb” may occur; this is likely to be neuropathic and treatment is generally with neuropathic pain medication such as gabapentin and pregabalin. Other classes such as opioids, NSAIDs, and acetaminophen are not as effective.
- Residual limb pain: This is likely to be musculoskeletal and localized in nature due to the remodeling of scar tissues, fascia, and muscles. Treatment includes wound care and systemic medications such as NSAIDs, Acetaminophen, opioids and in some cases muscle relaxants. Desensitization techniques may also be used such as compression, tapping, massage, and other modalities.
- Edema: Localized swelling is a complication that is very likely to occur in amputations and has the best outcome when control is started soon after surgery, with an immediate post-operative rigid dressing (IPROD). In the weeks following amputation, edema can further be controlled by compressive dressings, massage, elevation and in patients who have co-morbidities affecting fluid balance, use of diuretics.
- Contracture formation: Contractures are a musculoskeletal condition causing rigidity or hardening of muscles, tendons or other tissues leading to deformity and rigidity of joints; this is a long term complication that arises through mechanisms that are not completely clear. It is thought that decreased neural activation, protracted placement of a joint with the muscle in the short position and muscle atrophy are all contributing risk factors for formation.[22] Thus, the management of this complication involves stretching maneuvers to preserve the range of motion and strengthening to preserve muscle bulk.
- Body Asymmetry: An amputation creates weight distribution changes and can modify the center of gravity leading to compensatory mechanisms in function and gait, which can lead to pain, spasms or discomfort in other areas of the body.
- Skin Breakdown: In the weeks following an amputation, skin break down at the site of surgery can occur for a variety of reasons including poor wound healing due to co-morbidities, excessive bleeding, infection, edema, and poor dressing techniques. In the long term, this complication may arise due to assistive devices or prostheses that a patient may use. As a note, it is imperative to help shape the residual limb into a proper cylindrical or conical shape with smooth edges so that during prosthetic use, skin breakdown complications decrease.
- Cosmetic acceptability: Cosmetic acceptability post amputation can have emotional and mental side effects on a patient. Using an aesthetically appealing surgical technique, fitting the patient with a skin tone matched prosthesis, and minimal bracing may help mitigate this concern.
- Neuroma: Over time, as nervous tissue remodels, a mass of soft tissue and nerves may form. These are often benign but can be painful. Conventional treatments may include neuropathic pain medications or nerve blocks.[23]
Clinical Significance
Each type of amputation has clinical significance in functional ability, aesthetics and prostheses management. The following discussion highlights the most commonly seen clinical scenarios for each level of amputation.
Forequarter: When possible, this amputation should occur at the lateral margin on the sternocleidomastoid insertion to preserve the contour of the neck.
Transhumeral: Length should be preserved as much as possible for improved shoulder range of motion and prosthesis use. A minimum of 5 to 7 cm of the humerus should be retained for proper prosthesis fit. Further, there should be minimal periosteal stripping to prevent the occurrence of bony spurs, and rough edges require removal. Generally, the anterior and posterior fascia over the flexor and extensor muscle groups are sutured together to cover the end of the humerus. Biceps and triceps myoplasty preserves the strength of prosthetic control and myoelectric signals.
Elbow disarticulation: This amputation is preferred over transhumeral amputations because the humeral rotation is still preserved. For children, it is most suitable to preserve the epiphysis of the humerus in the residual limb to allow for growth and avoid revision. The posterior muscle flap is made to be longer than the anterior so that it can be wrapped and cushioned at the end of the humerus.
Transradial: It is crucial to preserve the length of the residual limb as much as possible to allow for improved pronation, supination, and prosthetic fit. For instance, a very short amputation allows for zero degrees of rotation, short allows 0 to 60 degrees, the medium allows 60 to 100 degrees, and long allows for 100 to 120 degrees. A minimum of 5 cm of the forearm preservation is needed for prosthetic fit and to allow platform weight bearing in patients with lower extremity disability. In some instances, the biceps tendon gets transferred to the ulna and tension of the muscle must be carefully calibrated to avoid elbow flexion contractures.[7] In some special situations, when one forearm bone is considerably longer than the other one, it may be preferable to create a one bone forearm rather than decrease prosthetic function by shortening the longer one.
Wrist: Additionally, the radial and ulnar styloid are resected to minimize bony protrusions and make prosthetic use comfortable. Of note, the radio-ulnar joint is preserved to allow for more forearm rotation.
Hand: Removal of specific sets of phalanges can have various effects. Radial amputation is the removal of the first and second proximal phalanges onward which can compromise pinch grasp. Thumb amputation is functionally compromising due to loss of palmar grip, side to side and tip to tip pinch. In patients with thumb loss, they can learn alternative grasps with the remaining digits.[24]
Enhancing Healthcare Team Outcomes
Amputations as a whole lead to functional loss and affect a patient both physically and mentally. As a result, the rehabilitation goals are often to make a residual limb functional, painless and aesthetically pleasing. When considering upper limb function or quality in the post-operative rehabilitation process, there is no standardized test or scale to quantify these metrics objectively. The outcome measure used which serves the closest to this is the Disabilities of the Arm, Shoulder, and Hand (DASH) Outcome Questionnaire; however, other questionnaires exist such as the use/abandonment of prosthesis and return to work.[25][26] In several retrospective survey-based studies, results concluded that many patients (at least 50 to 73%) could return to work post amputation; but the probability of doing so is dependent on the level of amputation, and in many cases, accommodations that may be necessary.[27] One such accommodation is the use of prostheses; however, surveys reveal that as many as 33.75% of patients with proximal upper limb issues rejected their prostheses due to various reasons (fit, comfort, ease, and aesthetics) and did not find them useful in activities of daily living or employment.[28] Thus, it is vital that in the postoperative fitting process, a patient’s functional needs be intimately understood to find a device that will accomplish functional goals. Physicians, therapists, and representatives from device-fitting agencies must fill this gap.
From a mental health viewpoint, there are well-documented cases and level I evidence to the psychological and social consequences of upper extremity amputation. Amputation is shown to affect mental state, work, functional capacity, and body image. Mechanism and circumstances of amputation, particularly in the case of trauma may lead to the development of acute stress disorder or post-traumatic stress disorder (PTSD).[29] PTSD was found to be more associated with work-related traumas. To this end, early recognition, counseling and use of techniques such as confronting and re-processing intrusive thoughts, graded work exposure, and on-site job evaluations are essential in maintaining the psychological health of patients. One study proposes a treatment algorithm with these techniques, which improved all symptoms except avoidance reactions.[30]
In summary, amputations require the cooperation of an interprofessional health care team that includes physicians, specialists, surgeons, specially-trained nurses, and physical and occupational therapists, all working and communicating together to bring about optimal patient care and outcomes.