Continuing Education Activity
This program addresses the escalating challenge of type 2 diabetes, particularly in the USA, where clinicians are increasingly confronted with this condition among younger demographics. Acarbose, an approved adjunctive therapy for adults with type 2 diabetes, plays a crucial role in managing this prevalent health concern. The curriculum delves into the indications, contraindications, interactions, monitoring protocols, and other therapeutic aspects essential for an interprofessional healthcare team. By participating in this educational session, healthcare professionals will gain a comprehensive understanding of acarbose therapy, enabling them to make informed decisions and collaborate effectively to tailor treatment plans for improved patient outcomes.
Objectives:
Identify the mechanism of action of acarbose.
Identify the potential adverse effects of acarbose.
Determine appropriate monitoring for acarbose therapy.
Compare interprofessional team strategies for improving care coordination and communication when using acarbose to improve patient outcomes for glucose control.
Indications
FDA-Approved Indications
The treatment of adults with type 2 diabetes as an adjunct to diet only or diet and exercise, depending on the patient's health status.
Based on the combined data of 6 placebo-controlled trials in patients with type 2 diabetes using acarbose as monotherapy, researchers noted the following changes from baseline glycosylated hemoglobin (hemoglobin A1c) by dose:
- 25 mg, 3 times daily: reduced by 0.44
- 50 mg, 3 times daily: reduced by 0.77
- 100 mg, 3 times daily: reduced by 0.74
- 200 mg, 3 times daily: reduced by 0.86
- 300 mg, 3 times daily: reduced by 1.00
Although the acarbose 300 mg, 3 times daily regimen is superior to lower doses at lowering hemoglobin A1c, the approved maximum daily dose of acarbose is 100 mg 3 times daily. There is no statistically significant difference in hemoglobin A1c reduction between the 50 mg, 3 times daily regimen, 100 mg, 3 times daily regimen, and the 200 mg, 3 times daily regimen.
Li J. et al found that diabetes mellitus patients who took metformin and acarbose alone or in combination therapy were more likely to survive hospitalization from COVID-19.[1]
Off-Label Uses
Type 1 Diabetes
Acarbose is not FDA-approved for treating type 1 diabetes; studies have been conducted to evaluate its safety and efficacy in this patient population. In a study of 121 patients with type 1 diabetes, acarbose 50 mg, 3 times daily for 2 weeks, followed by 100 mg, 3 times daily, reduced 2-hour postprandial glucose significantly. There were no differences between the placebo group and the acarbose group in hemoglobin A1c lowering or episodes of hypoglycemia.[2]
In 2 subsequent, single-center, placebo-controlled studies, 40 patients with type 1 diabetes mellitus were given metformin for 6 months after acarbose replaced metformin. The study results demonstrated that acarbose significantly decreased the 2-hour postprandial blood glucose concentration compared to the baseline. Compared to metformin therapy, the acarbose therapy group showed a statistically significant decrease in low-density lipoprotein (calculated), triglycerides, and total cholesterol. Acarbose use also led to a statistically significant reduction in regular insulin use.[3]
Prediabetes
Acarbose is not FDA-approved for the treatment of prediabetes. Acarbose has also undergone evaluation as a potential pharmacologic option for preventing the progression from prediabetes to type 2 diabetes. In a study of patients with impaired glucose tolerance tests, participants were randomized to acarbose 100 mg, 3 times daily, or placebo 3 times daily. Thirty-two percent of the acarbose group developed type 2 diabetes mellitus compared to 42% in the placebo group, resulting in a statistically significant hazard ratio of 0.75.[4]
Weight Loss
The effect of acarbose on weight loss has also been a research target. In an analysis of post-marketing data of 67,682 patients, the data revealed acarbose to decrease body weight significantly, independent of baseline body weight. Acarbose also significantly reduced fasting plasma glucose, postprandial glucose, hemoglobin A1c, and postprandial glucose concentrations.[5]
Acarbose may produce weight loss by increasing glucagon-like peptide-1.[6] Lazzaroni E. et al conducted a systematic analysis of the literature on non-insulin-lowering drugs for weight loss in patients with type 2 diabetes.[7] Acarbose reduced weight by less than 3.2%, canagliflozin reduced weight from 3.2% to 5%, and tirzepatide reduced weight by more than 5%.
Aging
Gupta S. et al conducted a 3-month study in mice to evaluate the anti-aging effects of acarbose.[8] 20-month-old C57BL/6 male and female mice were given a standard diet or a diet with 1000 ppm of acarbose. The acarbose-treated mice had decreased age-related lesions of the heart and kidney. Acarbose's anti-aging and anti-inflammatory effects appear mediated through the ERK1/2 signaling and the p38-MAPK pathways.[9]
Stroke
An in-vitro study suggests that acarbose could help treat ischemic stroke by decreasing mitochondrial and lysosomal dysfunction and changing gene expression to improve cellular survival.[10]
Polycystic Ovarian Syndrome
Yang Q. et al studied the treatment of polycystic ovarian syndrome with impaired glucose tolerance using acarbose and diet. This treatment helped improve the ovulation and pregnancy rate of the patients.[11]
Mechanism of Action
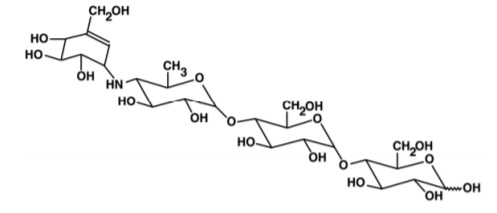
Acarbose is a complex oligosaccharide (see Image. Acarbose Chemical Structure) that acts as a competitive, reversible inhibitor of pancreatic alpha-amylase and membrane-bound intestinal alpha-glucoside hydrolase. Pancreatic alpha-amylase hydrolyzes complex carbohydrates to oligosaccharides in the small intestine. Intestinal alpha-glucosidase hydrolase breaks down oligosaccharides, trisaccharides, and disaccharides (sucrose, maltose) to monosaccharides (glucose, fructose) in the brush border of the small intestine. By delaying the digestion of carbohydrates, acarbose slows glucose absorption, reducing postprandial glucose blood concentrations.
Pharmacokinetics
Absorption
Acarbose acts locally in the gastrointestinal (GI) tract with low systemic bioavailability (less than 2% gets absorbed as the active drug, and 35% as metabolites).
Metabolism
Acarbose is metabolized in the GI tract by intestinal bacteria and digestive enzymes.
Elimination
The kidneys filter the absorbed drug, and 51% of an oral dose gets eliminated in feces.
Administration
Dosage Forms
Acarbose is available as a 25 mg, 50 mg, or 100 mg oral tablet and should be administered orally 3 times daily with the first bite of each meal.
Adult Dosing
Initial dosing is 25 mg orally, 3 times daily. However, starting with once-daily dosing may limit GI adverse effects. From 25 mg by mouth, 3 times daily, the dose can be titrated every 4 to 8 weeks to reach desired glycemic control while limiting GI adverse effects. The maximum daily dose is 100 mg, 3 times daily.
- If the patient weighs less than 60 kg, the dose should not exceed 50 mg, 3 times daily.
- Patients with renal dysfunction (serum creatinine greater than 2.0 mg/dL) have not been studied.
- Safety and efficacy have not undergone evaluation in pediatric patients.
- Studies have not established the safety of acarbose in pregnant patients.
- Nursing mothers should not use acarbose.
Gruden S. et al conducted a study on 67 obese middle-aged Caucasian men with treatment regimens that included orlistat and acarbose modified-release oral capsules to determine the safety of this experimental dosage form.[12] Three dosages were examined: 60/20, 90/30, and 120/40 mg orlistat/mg acarbose, respectively. The 3-dose combinations were found to be well-tolerated. The combination of orlistat and acarbose could help better control weight in patients with diabetes mellitus.
Mabate B. et al conducted in vitro research on combining fucoidan and acarbose to treat diabetes mellitus.[13] Fucoidan is a natural product that, when combined with acarbose, produces about 70% inhibition of alpha-glucosidase. This combination could decrease the dose of acarbose needed to lower plasma glucose and thus reduce the side effects of acarbose.
Drug-Drug Interactions
- Acarbose may decrease the bioavailability of digoxin and valproic acid.
- Acarbose may increase hypoglycemic risk when combined with other anti-diabetic agents that cause hypoglycemia.
- Digestive enzymes, including amylase, lipase, and protease, may decrease the effectiveness of acarbose.
- Therapy requires monitoring with other agents that affect blood glucose concentrations.
Adverse Effects
The most common adverse effects are GI symptoms, including flatulence, diarrhea, and abdominal pain. A high carbohydrate diet may worsen the adverse effects on the GI tract. GI symptoms tend to become reduced throughout treatment. Adherence to acarbose pharmacotherapy can be a problem because of side effects.[14]
Elevated serum transaminases may occur during acarbose therapy. Elevations are usually asymptomatic and reversible once drug therapy is discontinued.
Hypoglycemia should not occur with acarbose monotherapy. However, the therapy can increase the risk of hypoglycemia when used with antidiabetic agents that cause hypoglycemia, such as sulfonylureas or insulins.
Post-marketing reports include cases where there were rare occurrences of pneumatosis and cystoides intestinalis with alpha-glucosidase inhibitor use.
Jiang L et al conducted a retrospective cross-sectional study on muscle mass and function in patients with type 2 diabetes mellitus who were on plasma glucose-lowering therapy.[15] Acarbose decreased skeletal muscle index, handgrip strength, and gait speed the most compared with drug-naïve patients and patients taking insulin, metformin, and sulfonylureas monotherapy.
Contraindications
Acarbose use is contraindicated in patients with known hypersensitivity, diabetic ketoacidosis, liver cirrhosis, inflammatory bowel disease, or colonic ulceration. This medication is also contraindicated in patients with intestinal obstruction or those predisposed to intestinal obstruction; patients with chronic intestinal disease, including those who have issues with digestion or absorption; or conditions that the increased gas formation in the intestine will worsen.
Monitoring
One to 2-hour postprandial blood glucose concentrations and glycosylated hemoglobin require monitoring to assess efficacy. Serum transaminase concentrations should be checked every 3 months for the first year of therapy. The clinician should decrease the dose or discontinue therapy if concentrations become elevated during treatment.
Toxicity
Overdose with acarbose will not cause hypoglycemia but may increase GI adverse effects. Patients should not have food or beverages that contain carbohydrates for 4 to 6 hours if an overdose occurs.
If a patient experiences hypoglycemia while taking acarbose in combination with other antidiabetic medications, the patient should receive instructions to use glucose (gel, tablets, etc). Acarbose will prevent the breakdown of sucrose (table sugar) and delay glucose absorption, failing to correct hypoglycemia quickly. Severe hypoglycemia may require intravenous glucose or intramuscular glucagon administration.
Enhancing Healthcare Team Outcomes
Acarbose is a commonly used medication for managing type 2 diabetes mellitus. While the drug is helpful, it is not a highly effective agent when used as monotherapy. Because the drug works in the gastrointestinal system, the most common adverse effects are gastrointestinal upset/bloating. Hence, the prescribing clinicians (MD, DO, NP, PA), nurses (especially certified diabetes educators), and pharmacists must educate the patient on how to use the drug. Further, patients should receive counsel to avoid cola beverages, as the adverse abdominal symptoms may worsen.
While hypoglycemia is extremely rare with this agent, one should consider other antidiabetic drugs as the cause if it occurs. The patient should be treated for hypoglycemia and then counseled on preventing further low-sugar episodes. Only through patient education can the side effects be limited, and as with any medication, acarbose management is best by an interprofessional healthcare team across various disciplines, who engage in open communication with other team members regarding any changes in the patient's status so appropriate corrective action can be taken if necessary.