Learning Outcome
- List the risk factors for aspiration pneumonia.
- Describe the presentation of aspiration pneumonia.
- Identify nursing interventions in caring for patients with aspiration pneumonia.
- Describe the complications of aspiration pneumonia.

Aspiration pneumonia is an infectious pulmonary process that occurs after oropharyngeal fluids enter the lower respiratory tract. The aspirated fluid can be oropharyngeal secretions, particulate matter, or gastric content. Aspiration pneumonia requires high bacterial content in the aspirated fluid. If the inhaled fluid is sterile, as is the case with gastric fluid that becomes devoid of bacterial colonies due to its low pH, aspiration pneumonitis occurs. Aspiration pneumonitis is a chemical injury that does not require antibiotic therapy. In contrast, aspiration pneumonia will not resolve without appropriate antibiotic therapy. The mortality rate from aspiration pneumonia is largely dependent on the volume and content of aspirate and can range up to 70%.[1][2][3][4]
Failure of the natural defense mechanisms like the closure of the glottis and cough reflex increases the risk of aspiration. Common risk factors for aspiration include altered mental status, neurologic disorders (especially acute stroke and dementia), esophageal motility disorders, protracted vomiting, and gastric outlet obstruction. Although the common organisms involved in the etiology of community-acquired pneumonia are Streptococci, Haemophilus, and gram-negative bacilli, the etiology of aspiration pneumonia depends on the content of aspirate. A prospective study of 95 patients showed that gram-negative bacilli contributed to 49% of the infections, followed by anaerobes at 16%. The major anaerobes isolated were Fusobacterium, Bacteroides, and Peptostreptococcus. In hospital-acquired aspiration pneumonia, common etiology includes gram-negative organisms, specifically Pseudomonas aeruginosa.[5][6][7]
Conditions that increase the risk of aspiration pneumonia (AP) include:[8][9][10]
Advanced age is strongly associated with AP, with many older adults exhibiting "silent" microaspirations that may not be clinically apparent.[8] In patients 70 years or older hospitalized with pneumonia, the prevalence of dysphagia was reported at 91.7%, with silent aspiration in more than 50% of the cases. Still, advanced age does not directly predict the risk of AP. Frailty, poor nutritional status, and poor mobility in older adults are considered better markers for the risk of AP than chronologic age.[10]
By some estimates, 3 to 50% of the patients with stroke may develop AP.[8] Silent aspiration following a cerebrovascular event is seen in up to 40 to 70% of the patients.[10] Up to 11% of the patients who are hospitalized with Parkinson disease or dementia can develop AP over a 3-month period.[8] AP is also a common complication of multiple sclerosis, motor neuron diseases, Huntington disease, Down syndrome, and cerebral palsy.[8] Head and neck cancers, along with their treatments, also increase the risk of AP. Up to 70% of patients with head and neck cancer can develop AP in their lifetime.[8]
In addition to the above predisposing factors, one of the most important risk factors for AP is the extent of bacterial colonization in oral secretions. A high prevalence of bacterial colonization in oropharyngeal secretions can provide sufficient "bacterial load" for inoculation, even if the amount of aspiration is small. In a population-based case-control study of patients with CAP, poor oral health was noted as a risk factor for infection. Poor oral health has been identified as a definitive risk factor for pneumonia in hospitalized patients as well.[10]
The common clinical features that should raise suspicion for aspiration include sudden onset of dyspnea, fever, and hypoxemia, along with radiological findings of infiltrates in gravity-dependent areas of the lungs. The site involved depends on the position of the patient at the time of aspiration. The lower lobes are involved when patients aspirate in an upright position, and the superior lobes are involved when aspiration occurs in the recumbent position.
Vital sign assessment is imperative as hypoxia can quickly occur. In patients with severe infection, hypotension and tachycardia will also be present.
A high level of suspicion is required to diagnose aspiration pneumonia, especially in critically ill hospitalized patients. In suspected cases, antibiotic treatment should be initiated immediately. Although radiologic imaging is required to make the diagnosis, imaging studies should not delay the treatment.
The commonly utilized imaging studies are chest x-rays, computed tomography of the chest, and chest ultrasonography. They are required to demonstrate the presence of pulmonary infiltrates.
Most patients have unwitnessed overt aspiration or silent microaspirations during sleep. This makes it difficult to distinguish between AP and community-acquired pneumonia. In addition, patients with overt aspiration need not develop AP. This is especially true in patients with high-volume gastric content aspiration, which usually results in aspiration pneumonitis without aspiration pneumonia.
The British Thoracic Society recommends the following diagnostic workup in the evaluation of patients with suspected AP:[8]
Antibiotic therapy is required for the treatment of AP. The antibiotic of choice for community-acquired aspiration pneumonia is amoxicillin or ampicillin/sulbactam. Macrolides such as azithromycin should only be used in areas where regional pneumococcal resistance to macrolides is less than 25%. In patients with penicillin allergy, a respiratory fluoroquinolone such as levofloxacin or moxifloxacin may be used. Cephalosporins with macrolides or doxycycline can be considered in some cases as well.[11]
Aspiration preventive strategies should include a multifaceted approach with speech-language pathologists and dieticians helping restore effective swallowing and cough, nursing and oral hygienists helping reduce oral bacterial load, and nutritionists ensuring adequate hydration and caloric intake when patients are given modified consistencies of solids and liquids.[8]
Patients who are at risk for aspiration syndromes should be evaluated prior to the occurrence of an overt aspiration event or AP. Clinical assessment by nurses and triage staff is of paramount importance in the identification of patients with a high aspiration risk. Many different screening tools are available, with no clear evidence identifying the superiority of one screening tool over another. In frail elderly patients who do not have clearly identifiable risks of aspiration (such as an acute stroke), simple screening tools should be implemented to detect aspiration risk at first medical contact. One recent study identified the following 4 questions to screen for aspiration risk:[12]
An affirmative answer to any of the above questions implies impaired swallowing. The pilot study for this screen reported very high sensitivity with a specificity of 80.4%. The advantage of this screening tool is that it is easy to use, and it consists of very few items that may be administered by any individual in the healthcare setting without any specific training.[12]
A definitive diagnosis of aspiration requires a videofluoroscopy swallowing study (VFSS), which is a modified barium swallowing study. Barium visible beneath the true vocal cords confirms aspiration. If this occurs without any throat clearing or coughing, it is called a ‘silent’ aspiration. It is important to note that aspiration, especially microaspiration, is an episodic phenomenon that cannot be reliably excluded using a single VFSS study.[8]
When aspiration is identified, multiple different strategies are utilized to prevent the risk of AP. The chin-tuck or chin-down method is used to provide physical support to the pharyngolaryngeal musculature by asking the patient to touch the chin against the chest during swallowing.[8]
Oral care, especially that provided via mechanical techniques (toothbrush as opposed to chlorhexidine rinses), has shown a reduction in AP frequency and deaths in a number of studies. Current guidelines recommend non-foaming fluoride toothpaste in these patients to minimize the risk of aspiration.[8]
Modifying the viscosity of fluids and the texture of food in patients with impaired swallowing is used to prevent the risk of AP worldwide. However, this places the patient at increased risk of malnutrition and dehydration, especially those with underlying dementia. In addition, thickened textures can increase pharyngeal residue. Smaller volumes (one teaspoon at a time) are recommended in these patients to minimize residue and subsequent aspiration events.[8]
Balancing adequate nutrition while minimizing the risk of aspiration is of prime importance. Current guidelines suggest enteral feeding in patients who have no oral intake for more than 3 days or if less than 50% of nutritional requirement is met for more than 10 days.[8]
The management of aspiration pneumonia is with an interprofessional team that consists of a nurse practitioner, primary care provider, internist, infectious disease specialist, radiologist, and pulmonologist. Besides treating pneumonia, it is important to educate the staff looking after the patient on further prevention of aspiration. This means having the head of the bed elevated, close monitoring of oxygen status, and regularly suctioning the oral cavity in patients with swallowing difficulties.
The key to minimizing poor outcomes associated with this disease is to identify patients at risk for AP before it occurs. A multifaceted interprofessional team of clinicians, nurses, speech-language pathologists, nutritionists, and pharmacists is required to accomplish this goal. The clinical nurse can help screen for impaired swallowing using high-sensitivity screening tools to ensure every patient with impaired swallowing is identified. Speech-language pathologists can then help make the diagnosis of impaired swallowing and provide the patient with swallowing recommendations to minimize the risk of aspiration. The clinical nurse is essential at this juncture to ensure that the patient understands these recommendations and is able to perform them adequately. The clinical nutritionists help ensure that the patient receives adequate hydration and caloric intake when on modified diets. Clinical pharmacists help clinicians minimize adverse medication side effects (such as sedation) to decrease the risk of AP. In addition, they also help ensure that the patients receive the correct formulations of medications, especially if the pills need to be crushed. A collaborative interprofessional team. as outlined above, can greatly reduce the risk of AP and improve clinical outcomes for patients who are affected by this disease.
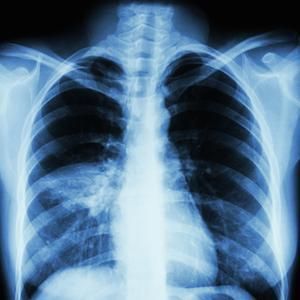
Ventilator-Associated Aspiration Pneumonia. Chest radiograph showing ventilator-associated aspiration pneumonia.
Melvil, Public Domain, via Wikimedia Commons.
Simpson AJ, Allen JL, Chatwin M, Crawford H, Elverson J, Ewan V, Forton J, McMullan R, Plevris J, Renton K, Tedd H, Thomas R, Legg J BTS clinical statement on aspiration pneumonia. Thorax. 2023 Feb [PubMed PMID: 36863772]
Teramoto S The current definition, epidemiology, animal models and a novel therapeutic strategy for aspiration pneumonia. Respiratory investigation. 2022 Jan [PubMed PMID: 34782300]
Almirall J, Boixeda R, de la Torre MC, Torres A Aspiration pneumonia: A renewed perspective and practical approach. Respiratory medicine. 2021 Aug-Sep [PubMed PMID: 34087609]
Košutova P, Mikolka P. Aspiration syndromes and associated lung injury: incidence, pathophysiology and management. Physiological research. 2021 Dec 30:70(Suppl4):S567-S583 [PubMed PMID: 35199544]
Yoshimatsu Y, Melgaard D, Westergren A, Skrubbeltrang C, Smithard DG. The diagnosis of aspiration pneumonia in older persons: a systematic review. European geriatric medicine. 2022 Oct:13(5):1071-1080. doi: 10.1007/s41999-022-00689-3. Epub 2022 Aug 25 [PubMed PMID: 36008745]
Mandell LA, Niederman MS. Aspiration Pneumonia. The New England journal of medicine. 2019 Feb 14:380(7):651-663. doi: 10.1056/NEJMra1714562. Epub [PubMed PMID: 30763196]
Mandell LA, Wunderink RG, Anzueto A, Bartlett JG, Campbell GD, Dean NC, Dowell SF, File TM Jr, Musher DM, Niederman MS, Torres A, Whitney CG, Infectious Diseases Society of America, American Thoracic Society. Infectious Diseases Society of America/American Thoracic Society consensus guidelines on the management of community-acquired pneumonia in adults. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 2007 Mar 1:44 Suppl 2(Suppl 2):S27-72 [PubMed PMID: 17278083]
Metlay JP, Waterer GW, Long AC, Anzueto A, Brozek J, Crothers K, Cooley LA, Dean NC, Fine MJ, Flanders SA, Griffin MR, Metersky ML, Musher DM, Restrepo MI, Whitney CG. Diagnosis and Treatment of Adults with Community-acquired Pneumonia. An Official Clinical Practice Guideline of the American Thoracic Society and Infectious Diseases Society of America. American journal of respiratory and critical care medicine. 2019 Oct 1:200(7):e45-e67. doi: 10.1164/rccm.201908-1581ST. Epub [PubMed PMID: 31573350]
Komiya K, Rubin BK, Kadota JI, Mukae H, Akaba T, Moro H, Aoki N, Tsukada H, Noguchi S, Shime N, Takahashi O, Kohno S. Prognostic implications of aspiration pneumonia in patients with community acquired pneumonia: A systematic review with meta-analysis. Scientific reports. 2016 Dec 7:6():38097. doi: 10.1038/srep38097. Epub 2016 Dec 7 [PubMed PMID: 27924871]
Gupte T, Knack A, Cramer JD. Mortality from Aspiration Pneumonia: Incidence, Trends, and Risk Factors. Dysphagia. 2022 Dec:37(6):1493-1500. doi: 10.1007/s00455-022-10412-w. Epub 2022 Jan 31 [PubMed PMID: 35099619]
Won JH, Byun SJ, Oh BM, Park SJ, Seo HG. Risk and mortality of aspiration pneumonia in Parkinson's disease: a nationwide database study. Scientific reports. 2021 Mar 23:11(1):6597. doi: 10.1038/s41598-021-86011-w. Epub 2021 Mar 23 [PubMed PMID: 33758213]
Yanagita Y, Arizono S, Tawara Y, Oomagari M, Machiguchi H, Yokomura K, Katagiri N, Iida Y. The severity of nutrition and pneumonia predicts survival in patients with aspiration pneumonia: A retrospective observational study. The clinical respiratory journal. 2022 Jul:16(7):522-532. doi: 10.1111/crj.13521. Epub 2022 Jul 5 [PubMed PMID: 35789107]
Kumar NR, Norwood BS. Sphingomonas Paucimobilis Pneumonia Complicated by Empyema in an Immunocompetent Patient: A Case Report and Concise Review of Literature. Cureus. 2022 May:14(5):e24820. doi: 10.7759/cureus.24820. Epub 2022 May 8 [PubMed PMID: 35693369]
Martinez K, Mangat GK, Sherwani N, Glover DO M, Silver Md M. Veillonella Intrapulmonary Abscess With Empyema. Cureus. 2023 Sep:15(9):e45210. doi: 10.7759/cureus.45210. Epub 2023 Sep 14 [PubMed PMID: 37842426]
Baijens LW, Clavé P, Cras P, Ekberg O, Forster A, Kolb GF, Leners JC, Masiero S, Mateos-Nozal J, Ortega O, Smithard DG, Speyer R, Walshe M. European Society for Swallowing Disorders - European Union Geriatric Medicine Society white paper: oropharyngeal dysphagia as a geriatric syndrome. Clinical interventions in aging. 2016:11():1403-1428 [PubMed PMID: 27785002]
Dziewas R, Michou E, Trapl-Grundschober M, Lal A, Arsava EM, Bath PM, Clavé P, Glahn J, Hamdy S, Pownall S, Schindler A, Walshe M, Wirth R, Wright D, Verin E. European Stroke Organisation and European Society for Swallowing Disorders guideline for the diagnosis and treatment of post-stroke dysphagia. European stroke journal. 2021 Sep:6(3):LXXXIX-CXV. doi: 10.1177/23969873211039721. Epub 2021 Oct 13 [PubMed PMID: 34746431]
Cosentino G, Avenali M, Schindler A, Pizzorni N, Montomoli C, Abbruzzese G, Antonini A, Barbiera F, Benazzo M, Benarroch EE, Bertino G, Cereda E, Clavè P, Cortelli P, Eleopra R, Ferrari C, Hamdy S, Huckabee ML, Lopiano L, Marchese Ragona R, Masiero S, Michou E, Occhini A, Pacchetti C, Pfeiffer RF, Restivo DA, Rondanelli M, Ruoppolo G, Sandrini G, Schapira AHV, Stocchi F, Tolosa E, Valentino F, Zamboni M, Zangaglia R, Zappia M, Tassorelli C, Alfonsi E. A multinational consensus on dysphagia in Parkinson's disease: screening, diagnosis and prognostic value. Journal of neurology. 2022 Mar:269(3):1335-1352. doi: 10.1007/s00415-021-10739-8. Epub 2021 Aug 21 [PubMed PMID: 34417870]
Tsang K, Lau ES, Shazra M, Eyres R, Hansjee D, Smithard DG A New Simple Screening Tool-4QT: Can It Identify Those with Swallowing Problems? A Pilot Study. Geriatrics (Basel, Switzerland). 2020 Feb 27 [PubMed PMID: 32120993]
O'Keeffe ST. Use of modified diets to prevent aspiration in oropharyngeal dysphagia: is current practice justified? BMC geriatrics. 2018 Jul 20:18(1):167. doi: 10.1186/s12877-018-0839-7. Epub 2018 Jul 20 [PubMed PMID: 30029632]