Continuing Education Activity
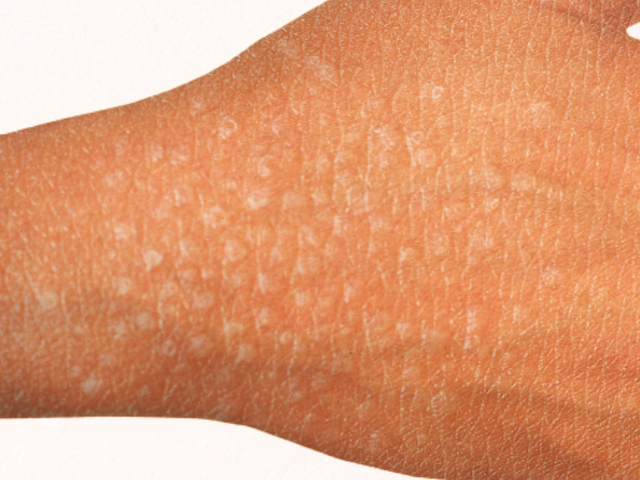
Lichen nitidus is a rare benign condition characterized by extensive 1- to 2-mm skin-colored papules commonly occurring on upper extremities, chest, abdomen, or genitalia. It typically occurs in children and young adults as a self-limited process with no long-term sequelae. Most patients remain asymptomatic and may only seek treatment if pruritus or a generalized distribution is present.
Objectives:
- Review the etiology of lichen nitidus.
- Describe the presentation of lichen nitidus.
- Summarize the treatment options for lichen nitidus.
- Outline potential patient cosmetic concerns with lichen nitidus and the treatment options to address them that the clinician can explain to the patients.
Introduction
Lichen nitidus is a rare chronic inflammatory condition first described in 1907 by Pinkus. This uncommon cutaneous eruption has clearly defined clinical and histopathological characteristics with an unknown etiology and pathogenesis.[1] It most commonly presents in children and young adults and does not favor one sex or race.[2][3] Lichen nitidus presents as multiple, discrete, shiny, flat-topped, pale to skin-colored papules, 1 to 2 mm in diameter. These lesions commonly present on the limbs, abdomen, chest, and penile shaft.[2][3] It is usually asymptomatic, so treatment is generally for symptomatic or cosmetically disturbing lesions.[2]
Etiology
Lichen nitidus is a rare skin condition with an unknown etiology. Although genetic factors have been implied as a potential cause because some cases reported in the literature have been familial.[3] The close association between lichen nitidus and lichen planus has lead to speculation they may be different manifestations of similar etiologic factors, but based on immunohistochemical analysis, lichen nitidus is not a variant of lichen planus.[1] In the literature, lichen nitidus has been reported to correlate with Crohn disease, Niemann-Pick disease, amenorrhea, and can occur in patients after tattoos.[3][4][5] Generalized lichen nitidus has been reported to be associated with Down's syndrome. Also, there are reported cases in advanced human immunodeficiency virus (HIV) and a case of generalized lichen nitidus following treatment of interferon-alpha and ribavirin for hepatitis C.[1][5] The variant of lichen nitidus, generalized purpuric lichen nitidus, is extremely rare, and a case report exists of an eruption following nivolumab treatment, which is an immune checkpoint inhibitor that activates T lymphocytes in patients with cancers such as melanoma and non-small cell lung carcinoma.[6][7]
Epidemiology
Lichen nitidus does not discriminate between males and females on presentation and is most common in children and young adults, although reports exist of cases of lichen nitidus in older adults.[2][3] Lichen nitidus does not exhibit a predilection for any race.[4]
Pathophysiology
Lichen nitidus is a chronic inflammatory condition with definitive clinical and histopathological features but obscure pathophysiology.[1][2] Even though the pathophysiology is unclear, the hypothesis is that lichen nitidus presents from an underlying immune mechanism or associated with immune alterations in patients.[1][3] There have been reports of lichen nitidus associated with other cutaneous diseases such as lichen planus erythema nodosum, vitiligo, and lichen spinulosus.[1] The suggested pathophysiology is an allergen that may cause antigen-presenting cells (Langerhan cells) to active a cell-mediated response, resulting in lymphocyte accumulation forming the discrete inflammatory papules seen in lichen nitidus containing a large number of Langerhan cells.[8] Also, in theory, viruses, mycobacteria, treponemal species, and streptococcus, and any other active infectious agent could activate a cell-mediated response initiating the accumulation of lymphocytes resulting in the formation of the inflammatory papules seen in lichen nitidus.[1]
Histopathology
Lichen nitidus has definitive histopathological characteristics. The hallmark of lichen nitidus is a well-circumscribed granulomatous infiltrate of lymphocytes, macrophages, Langerhans giant cells, and multinucleated epithelioid histiocytes in the papillary dermis bordered by extensions of epidermal ridges. This sharply circumscribed inflammatory infiltrate generally spans 4 to 5 dermal papillae within the dermis, giving a "ball-in-clutch" configuration.[1][3][4][9][10] Early lichen nitidus lesions have more lymphocytes present, while later lesions are more granulomatous with occasional giant cells noted.[3] The epidermis is thinned and parakeratotic with hydropic degeneration of basal keratinocytes and cytoid bodies.[3][10]Generalized purpuric lichen nitidus has the same histopathological features as lichen nitidus in addition to subepidermal hemorrhages.[6]
There have been some reports of lichen nitidus being a variant of lichen planus, but both cutaneous conditions have distinct histopathological entities. Lichen planus has more uniform lymphocytes within the infiltrate that makes up mostly T helper cells (CD4+). Both have inflammatory changes and the ball-in-claw infiltrating the stratum spinosum, a thinning epidermis, and hyperkeratotic papules, but parakeratotic papules present in lichen nitidus, and orthokeratotic papules occur in lichen planus.[3]
History and Physical
Lichen nitidus usually presents as asymptomatic, shiny, flat-topped, fleshy pink to dark brown papules. They are typically 1 to 2 mm in diameter. In patients with darker skin lesions can appear as light spots. Lesions commonly present on the neck, trunk, limbs, abdomen, and penile shaft. The involvement of mucous membranes, palms, soles, and nails are rare, but there are reports.[2][3][4] If lichen nitidus is symptomatic, the patient mainly complains of mild sporadic pruritus.[3] Koebner phenomenon is a hallmark of lichen nitidus, as seen in lichen planus, but is not present in all cases.[3][4]
Rarely lichen nitidus will present only on the palms and soles and will usually present with lichen nitidus lesions in other locations.[11]
If lesions present in the oral mucosa, they will be flat, greyish papules.[3][12]
Nail involvement is rare but will present with longitudinal furrowing and ridging on the nail plate from inflammation of the nail matrix. Nail involvement usually presents with the generalized variant of lichen nitidus, and patients are more likely to have palmar involvement. If the nail fold is involved, nonspecific periungual inflammation or violaceous shiny papules can be seen [2]. Thickening, ridging, pitting, or detachment are also visible in affected nails.[12]
Reported variants of lichen nitidus[1][4]:
- Confluent
- Hemorrhagic
- Linear
- Perforating
- Spinous follicular
- Vesicular
- Generalized
- Actinic
Purpuric lichen nitidus (hemorrhagic) is rare and will present with red-brown papules due to underlying hemorrhage within the lesions. Cases have been reported to develop in patients similar to pigmented purpuric dermatosis.[6] Purpuric generalized lichen nitidus is very uncommon. Histologically subepidermal hemorrhages within lesions are noted. Degenerative changes take place within capillary vessels, which explains the extravasation of erythrocytes.[13]
Actinic lichen nitidus usually presents as pinpoint lichenoid papules in photo distributed areas. It commonly presents in pediatrics and adults with Fitzpatrick skin types of IV to VI. Actinic lichen nitidus characteristically demonstrates annular plaques and can have similar histological features to lichen planus. It is thought to be a variant of a polymorphous light eruption.[4][14]
Lichen nitidus in a linear distribution can mimic lichen spinulosus.[1]
Evaluation
The diagnosis of lichen nitidus can be made clinically. Skin biopsy does provide a definitive diagnosis and has distinct histopathological features as mentioned above.
Dermoscopy
Dermoscopy can be a useful tool when clinically diagnosing lichen nitidus. Smooth, white, well-circumscribed 1-2mm circular areas are seen with a brown shadow reflected. The well-circumscribed white circles can correlate with the epidermal acanthosis seen on histopathology. The brownish shadow reflected off of the white circles is the underlying epithelioid cells and lymphocytes in the dermal papilla. Dermoscopy can be helpful well differentiating between other cutaneous conditions.[9]
In patients who have palmoplantar involvement, hyperkeratotic pits and well-defined depressions with thin scales have been noted on dermoscopic assessment.[11]
Treatment / Management
Patients usually are asymptomatic, and lesions usually resolve within months to a year. Treatment is usually for symptomatic or cosmetically disturbing lesions.[2][3]
Reported treatment options[6][8][12][15]:
- Topical corticosteroids
- Systemic corticosteroids
- Topical calcineurin inhibitors (tacrolimus)
- Acitretin
- Narrow UVB rays
- Photochemotherapy (PUVA)
- H1 receptor antagonist
- Astemizole
- Dinitrochlorobenzene immunotherapy
- Itraconazole
- Isoniazid
- Cyclosporine
- Systemic Isotretinoin
In chronic or persistent forms of lichen, nitidus topical or systemic corticosteroids are options.[3]
In patients who have generalized lichen nitidus, the resolution is less predictable.[8] PUVA is effective for generalized involvement of the upper and lower extremities.[3] Topical or systemic corticosteroids, astemizole, and dinitrochlorobenzene immunotherapy have also been reported as effective treatment options for generalized lichen nitidus.[8]
Acitretin has been reported to have good results in patients with involvement of palms and soles.[3]
If there is nail involvement, intramatricial injections of corticosteroids are a treatment option.[2]
Narrowband UVB has less carcinogenic risk compared to broadband UVB or PUVA The mechanism for treatment is unknown but is thought to impair cellular immunity by depleting the number of epidermal Langerhans cells.[8]
Cyclosporine reported in a case report was beneficial for generalized purpuric lichen nitidus.[6]
A case of systemic isotretinoin used for treatment was reported successful. Retinoids are thought to suppress inflammation by reducing the migration of neutrophils and eosinophils to the dermis and also have antiproliferative effects. The dose reported was isotretinoin 40 mg daily, and researchers noted regression after four months. This case was a patient who had cosmetic fears and diffuse pruritus.[15]
The papules seen in lichen nitidus can lead to postinflammatory hyperpigmentation, which usually resolves within a few months.[12]
Differential Diagnosis
Differential diagnoses include but are not limited to lichen planus, keratosis pilaris, follicular eczema, lichen sclerosus et atrophicus, lichen spinulosus, pigmented purpuric dermatosis.[1][4][6][9]
Prognosis
Lichen nitidus is a self-limiting dermatosis that is usually asymptomatic and not necessary to treat. It usually resolves within months to a year.[3] If lichen nitidus becomes symptomatic or is cosmetically disturbing, then the above treatment options are available.[2]
Complications
Lichen nitidus is usually asymptomatic. On occasion, lesions can be mildly pruritic or affect the nails, palms, soles, and mucosa. It usually is not necessary to treat and will resolve within months to a year.[3]
Consultations
A dermatologist consult is an option for further evaluation and management of patients with lichen nitidus.
Deterrence and Patient Education
Patients require education on the benign nature of lichen nitidus and how lesions will most likely spontaneously resolve. If patients become symptomatic or have cosmetic concerns, they should also understand the available treatment options.
Enhancing Healthcare Team Outcomes
Health care providers should communicate the benign nature of lichen nitidus with patients and be aware that lesions will most likely spontaneously resolve on their own. This explanation will avoid treatment that is not required and decrease the risk of side effects of the treatment modalities used for lichen nitidus. If lesions persist, become symptomatic, or cosmetically disturbing, the clinician should discuss appropriate treatment options with patients. Referring to a specialist for management when needed and having open communication between all health care providers will overall improve patient care.
When initiating treatment, it is wise for the clinician to consult a pharmacist, especially given the side effect profile of retinoid drugs. The pharmacist can verify dosing and help educate the patient on dosing and adverse effects. This counsel should be reiterated by a dermatology specialty nurse who is familiar with these medications and can assist the clinicians in implementing any treatment plan. This interprofessional team approach will improve treatment outcomes for patients with lichen nitidus. [Level 5]