Continuing Education Activity
The Leopold maneuvers are used to palpate the gravid uterus systematically. This method of abdominal palpation is of low cost, easy to perform, and non-invasive. It is used to determine the position, presentation, and engagement of the fetus in utero. This activity describes the four Leopold maneuvers and explains the method of systematic abdominal palpation used to assess fetal presentation and position in the third trimester of pregnancy.
Objectives:
- Describe the normal fetal presentation and position.
- Explain the four Leopold maneuvers.
- Summarize the clinical significance of abdominal palpation in the obstetric examination.
- Identify the importance of improving training in abdominal palpation to enhance the delivery of care for obstetric patients.
Introduction
The Leopold maneuvers, named after the German obstetrician and gynecologist Christian Gerhard Leopold (1846–1911), are part of the physical examination of pregnant women.[1][2] Four classical maneuvers are used to palpate the gravid uterus systematically. This method of abdominal palpation is of low cost, easy to perform, and non-invasive. It is used to determine the position, presentation, and engagement of the fetus in utero.
Fetal presentation refers to the fetal anatomic part proceeding first into the pelvic inlet. When the fetal head is approaching the pelvic inlet, it is referred to as a cephalic presentation. The commonest presentation is the vertex of the fetal head. Malpositions are abnormal positions of the vertex of the fetal head, using the occiput as the reference point, relative to the maternal pelvis. Malpresentations are all presentations of the fetus other than vertex, which includes the breech presentation, transverse and oblique lie. Spontaneous vaginal delivery is most common when a cephalic-presenting fetus is in the occiput anterior position.[3]
Malpresentation is estimated to occur in 5% of all deliveries and is an essential cause of the high cesarean delivery rate.[4] It is essential to detect non-cephalic presentations before the onset of labor to mitigate the maternal and neonatal risks associated with complicated vaginal delivery or cesarean section. Detection of malpresentation in late pregnancy allows for counseling on adequate care measures. The underutilized external cephalic version and intrapartum planning and consenting are choices that can be discussed.[5][6][7]
Accurate assessment of fetal presentation and position is crucial in guiding obstetric management. However, the accuracy of Leopold maneuvers varies depending on many factors, especially examiner experience. Therefore ultrasonographic examination remains the current gold standard investigation for ensuring the fetus is in the cephalic presentation during the third trimester of pregnancy. It is recommended for confirmation when any malpresentation is even slightly suspected.[8][9]
Indications
Palpation is the contact of the operator's fingers and hands with the body of the woman or child. It offers the possibility of collecting data on an area, structure, or function by touch. Uterine contractions, the size of the pregnant uterus, any uterine masses, and attitude, presentation, degree of commitment of the fetus, and any fetal-pelvic disproportions can be detected.
Abdominal palpation is accurate in identifying the presentation, mainly if performed by experienced healthcare professionals. If in doubt about the presentation part, obstetric ultrasound should be used to confirm the results of the palpation. Ultrasound can also rule out fetal abnormalities, low placenta, hyperextension of the baby's head, and the presence of the umbilical cord around the neck of the fetus. The palpation technique requires skill and delicacy. The entire palm and fingers are useful for detecting myometrial activity, fetal movements, or any neoformations (fibroids), or the degree of edema. Palpation can be superficial or deep (the superficial one must always precede the deep one since the latter can cause pain); avoid having long nails because they can cause discomfort or injury.
From a psychological point of view, palpation is to be considered a form of analog communication between the midwife and the woman. Therefore through this technique, the operator can transmit the feelings they have towards the patient.
Contraindications
While the benefits of abdominal palpation are challenging to quantify, the risks have not been identified. Evaluation of presentation by abdominal palpation before 36 weeks is not always accurate. Routine evaluation of the presentation with abdominal palpation should not be offered before 36 weeks, due to any inaccuracies and inconvenience to the woman. The fetal presentation should be evaluated with the abdominal palpation at 36 weeks or later when the presentation can affect plans for childbirth.
Leopold maneuvers are complicated maneuvers to perform on obese women and women who have polyhydramnios. Palpation can sometimes be uncomfortable for the patient if no precautions are taken to ensure that she is well-positioned and relaxed.
Preparation
The aim of Leopold maneuvers is to determine the fetal presentation and position by systematically palpating the gravid abdomen. The initial steps are described below:
- Wash hands
- Explain the steps of the examination to the patient as this reduces anxiety and enhances cooperation
- Obtain consent
- The patient should be advised to void as an empty bladder promotes comfort and allows for more productive examination, and the distended bladder can obscure fetal contour
- Provision of privacy
- Prepare the equipment, such as measuring tape, Pinard stethoscope or Doppler transducer, and ultrasound gel
- Position the patient supine with the head of the bed raised to 15 degrees, and a small pillow or rolled towel placed on her right side
- Adequate exposure of the gravid abdomen from the xiphisternum to the pubic symphysis
- Inspect the gravid abdomen
Technique or Treatment
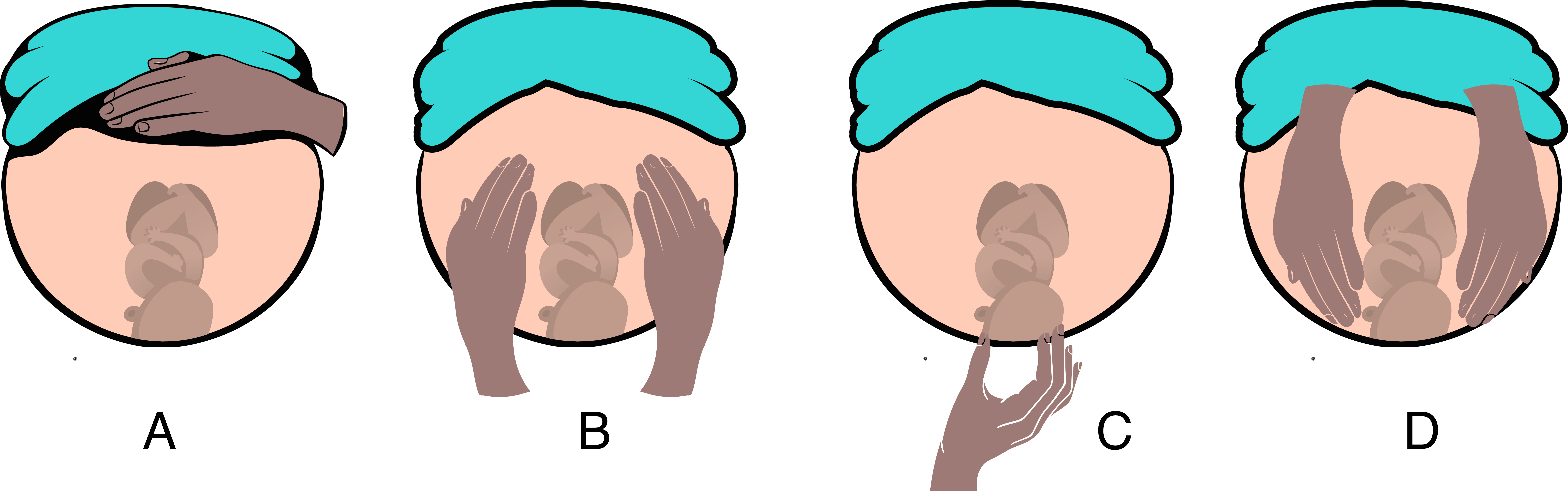
The First Maneuver
The first maneuver also called the fundal grip, assesses the uterine fundus to determine its height and which fetal pole—that is, cephalic or podalic—occupies the fundus. The uterine contour is outlined by the examiner, placing both of his or her hands on each upper quadrant of the patient's abdomen facing the maternal xiphoid cartilage. The ulnar border of each hand is in contact with the abdominal wall, and the opposite fingers are touching each other. Using the fingertips, the fundus is gently palpated to identify which fetal part is present in the upper pole (fundus) of the uterus. The breach gives the sensation of a large, nodular mass, and its surface is uneven, non-ballotable, and not very mobile whereas the head feels hard and round with a smooth surface of uniform consistency, is very mobile and ballotable.
The first maneuver aims to determine the gestational age and the fetal lie.
Gestational age can be evaluated using fundal height or McDonald's rule.[1] The uterine fundus reaches:
- The public symphysis at the 12th week
- A point midway between the pubic symphysis and the transverse and the transverse umbilical plane at the 16th week
- The transverse umbilical plane at the 20th week
- Having crossed this line, it is assumed each transverse finger breath corresponds to two weeks
The Second Maneuver
The second maneuver, sometimes called the umbilical grip, involves palpation of the lateral uterine surfaces. Still facing the maternal xiphoid cartilage, both hands slide down from the uterine fundus towards the lateral uterine walls. The clinician's hands are placed flat and parallel to each other along the abdominal wall at the level of the umbilicus. It allows establishing if the fetus is in a longitudinal, transverse, or oblique situation, and to determine the position of the back and small parts.The operator places the two flat hands sideways to the uterus and tries to bring them closer to the midline. In the approach maneuvers, the operator's hands are one on the back of the fetus and one on the small parts, which give different tactile sensations.The approach is possible when the fetus is in a longitudinal position regardless of the type of presentation, while it is not possible when the situation is transverse or oblique. Furthermore, it is possible to understand from which side the fetal back is located.
If the identification of the fetal back proves to be difficult, the provider can perform the following maneuvers. A simple adjustment involves alternating two hand palpation of lateral uterine surfaces. By placing the right hand steady on one side of the abdomen while using the palm of the left hand, the right side of the gravid uterus is palpated gently. This is then repeated using the opposite side. Otherwise, the Budin maneuver, named after French obstetrician and gynecologist Pierre-Constant Budin 1846–1907, can be performed for the precise determination of the position of the fetal back.[2] The uterine fundus is pressed with force using one hand, which accentuates the curvature of the fetal back, allowing for easier palpation with the other hand. The fetal heart can be auscultated at this time, which can also provide information on fetal orientation. The heart is well perceived when the stethoscope or the doppler transducer is placed on the back of the fetus.
The Third Maneuver
The third maneuver was modified by Karel Pawlík (1849–1914), a Czech gynecologist and obstetrician, and is referred to as the Pawlik grips. This maneuver aids in the confirmation of fetal presentation.
The first Pawlík grip, sometimes called the first pelvic grip, helps to define which presenting part of the fetus is situated in hypogastrium. Using the thumb and fingers of the right hand close above the pubic symphysis, the presenting part is grasped at the lower portion of the abdomen and draws the thumb and finger near to clasp the lower uterine segment including its contents.
In the second Pawlík grip, the clinician carries on by sliding the hand upward to determine the cervical groove: if the mass moves, the presenting part is not engaged. Then lateral movements and ballottement are performed. The differentiation between head and breech is made as in the first maneuver. This maneuver also allows for an assessment of the fetal weight and the volume of amniotic fluid.
The Fourth Maneuver
This fourth maneuver resembles the first maneuver; however, the examiner faces towards the maternal pelvis. This maneuver involves the examiner placing the palms of both hands on either side of the lower abdomen, with the tips of the fingers facing downward toward the pelvic inlet. The fingertips of each hand are used to apply deep pressure from the outside to the inside and in a craniocaudal direction along the lower contour of the uterus towards the birth canal. It is possible to identify the characteristics of the part presented and confirm the findings detected with the third Leopold maneuver. The fingers of both hands move gently along the sides of the uterus towards the pubis. The side where there is resistance to the descent of the fingers towards the pubis is larger is where the forehead is located. If the head of the fetus is well flexed, it should be on the opposite side from the back of the fetus. If the head of the fetus is extended, however, the occiput is perceived and is on the same side of the spine. It is possible to evaluate the degree of descent of the presented part and to realize if there are gross disproportions between this and the pelvic inlet.
This maneuver identifies which presenting part is in the lower uterine pole. To perceive how much of the cephalic extremity, which we recognized to be at the lower pole, descends into the birth canal: if it is entirely external, then it has not confronted itself, if it is confronting itself or if it has ultimately descended. The fingers travel the upper contour of the cephalic end, around the neck of the fetus.
Completing the fourth maneuver with the so-called "fifth maneuver" of Leopold, or maneuver of Zagenmeister, also can allow the approximate distance between the presenting part and the maternal pelvis. In the cephalic presentation, the hand is placed flat on the pubic symphysis, and the palpation could delineate the fetal head portion that can be reached above the pelvic inlet. Using the rule of fifths, the distance between the base and vertex of the fetal head is divided into five equal parts. Each fifth corresponding to 2 cm or approximately one transverse fingerbreadth. If the fetal head accommodates two fingerbreadths above the pelvic brim, it is said to be engaged.
Complications
A breech presentation occurs when the presenting part is either the buttocks and/or the feet. On examination, the head is felt in the upper uterine pole and the breech in the pelvic cavity. The fetal heart tones are auscultated higher than anticipated with a vertex presentation.
When the longest axis of the fetus is oriented transversely, the presenting part is typically the shoulder. In the transverse lie on palpation, neither the head nor the buttocks can be palpated in the lower uterine pole inlet, and the fetal head can be felt in the flank.
Occiput posterior position occurs when the fetal occiput is at or posterior to the sacroiliac joint. On examination, there is a lower abdomen flattened, fetal limbs are palpable anteriorly, and the fetal heart tones may be auscultated in the flank.
Brow presentation occurs with some extension of the fetal head. On palpation, the fetal occiput is higher than the sinciput, and more than half the fetal head is felt above the symphysis pubis.
Face presentation results from hyperextension of the fetal head. On palpation, the fold of the neck is felt as a deep indentation between the occiput and the back; however, in face presentation, this depression is limited.
Clinical Significance
Few studies have compared the gold standard ultrasonography with clinical examination to detect non-cephalic presentation in the third trimester of pregnancy. These investigators found that abdominal palpation fails to detect a significant percentage of mal-presenting fetuses.[3]
Clinical examination was relatively sensitive in multiparous women and those with lower body mass indices. The specificity of clinical examination increased significantly as gestational age increased, and body mass index decreased. When abdominal palpation was evaluated as a screening tool for identifying malpresentation, it was found that false-positive diagnoses were a more frequent error because of the low prevalence of malpresentation in low-risk populations.[4]
Leopold maneuvers have been reported to be difficult in obese pregnant women and pregnancies complicated with polyhydramnios, fibroids, or anterior placental location. In clinical practice, the use of repeated procedures by a second examiner, pelvic examination, and rescheduling a return visit with a sequential abdominal examination can serve to improve the accuracy of abdominal palpation findings.
Leopold maneuvers can help mothers to perceive and visualize fetuses. Thus abdominal palpations can develop the maternal-fetal relationship, which plays an important role in a child's psychological, cognitive, and social development.[5][6][7]
Enhancing Healthcare Team Outcomes
All healthcare providers should be competent with the methods to perform abdominal palpation of a gravid uterus and the significance of the findings. The findings observed should be documented and can be used to guide further obstetric management. Identifying pregnancies complicated by malpresentation and referral to appropriate facilities may lead to improved outcomes for both neonate and mother.[8]
Offering an external cephalic version (ECV) for breech presentation can contribute to the safe lowering of the primary cesarean delivery rate.[9] Training for existing or new staff who are moving to midwifery-obstetric care is necessary as experienced clinicians can be effective in using abdominal palpation as a screening tool for fetal malpresentation, particularly in settings where ultrasound may not be readily available.[4]