Continuing Education Activity
Emergency Department and primary care clinics are frequently called on to evaluate orthopedic complaints. It is essential for most providers to feel confident in the management of fundamental orthopedic problems. Fractures involving the distal radius (DR) of the forearm are common. The incidence of radial fractures is increasing as life expectancy grows, leading to a larger population of patients who are at risk for these injuries. Distal radial fractures are seen predominantly in children/adolescents and the elderly. Fracture patterns, management, and complications differ between these age groups. It is crucial for providers to review these distinctions, to know which fracture patterns are emergent, and to refer for further management in an appropriate time frame. This activity will review the epidemiology, management, and complications of distal radial fractures and highlight the role of the interprofessional team in their management.
Objectives:
- Review the causes of distal radius fracture
- Describe the presentation of a patient with distal radius fracture.
- Summarize the treatment options for distal radius fracture.
- Explain the importance of improving care coordination among interprofessional team members to improve outcomes for patients affected by distal radius fracture.
Introduction
Emergency Department and primary care clinics are frequently called on to evaluate orthopedic complaints. It is essential for most providers to feel confident in the management of fundamental orthopedic problems. Fractures involving the distal radius (DR) of the forearm are common. The incidence of radial fractures is increasing as life expectancy grows, leading to a larger population of patients who are at risk for these injuries. Distal radial fractures are seen predominantly in children/adolescents and the elderly. Fracture patterns, management, and complications differ between these age groups. It is crucial for providers to understand these distinctions, to know which fracture patterns are emergent, and to refer for further management in an appropriate time frame. Providers must have an understanding of forearm and wrist anatomy, and the recommendation here is that that readers review this topic in conjunction with this article. This chapter will review the epidemiology/etiology, as well as the eponymous fractures, management, and complications of distal radial fractures.
Etiology
Distal radial fractures can result from any trauma to the forearm. Isolated DR fractures typically include Smith’s, Colle’s, Torus/Buckle, Greenstick, Die-punch, and isolated radial shaft fractures. [1] These fractures most frequently occur as a result of fall on the outstretched hand (FOOSH) injuries. DR fractures in the elderly are often the result of low-energy falls from a standing or seated position. [2][3] They are often comminuted and intra-articular fractures that often fall outside of traditional eponymous classification. In children and adolescents, isolated DR fractures are more frequently the result of high energy falls sustained on the playground or during sporting events. [4] DR fractures can also present in more complicated injury patterns such as the Galeazzi fracture-dislocation, both bone fractures, radial styloid fractures, and Barton’s and Chauffeur’s fractures. The mechanism for these fractures is often more complex or atypical than that of isolated DR fractures.
Epidemiology
Distal radial fractures are very common either in isolation or in concert with other fractures and injuries. For example, in the United States, there is an incidence of around 67 upper extremity fractures per 10,000 people annually. Distal radial and ulnar fractures account for approximately 25% of these fractures. With the exception of the 18 to 34-year-old age group, DR fractures are the most common upper extremity fracture. The overall incidence of DR fractures occurring each year is increasing worldwide. For example, a 1998 study by Melton et al., from Rochester, Minnesota in the United States documented a 17% increase in DR fractures between 1945-1994. [5] Another 2017 study by Jerrhag et al., from Sweden showed a 2.0% increase in DR fractures per annum in men and a 3.4% increase in women aged 50-59 between 1999-2010. This study also showed statistically significant increases for the 17-64 year age group. [6]
It is difficult to attribute the growing incidence of DR fractures to any single cause. However, the general thinking is that increased childhood obesity and the overall potential for people to live more years with comorbidities such as osteoporosis have primarily contributed to this problem. Another theory advanced is that increased participation in organized sports has led to more childhood DR fractures. It is also possible that increased access to care has led to an apparent increase in fractures while the true incidence has remained stable.
DR fractures can occur at any age. However, there is largely a bimodal distribution of these injuries based on age and sex. The two most common age groups are children less than 18 years old, and adults greater than 50 years old. [6]
In children, the peak incidence of DR fractures is 12-14 years old in boys and 10-12 years old in girls. These peaks relate to the decreased level of skeletal mineralization and density that exist during pubertal growth spurts. During these times the rate of bone lengthening exceeds the rate of mineralization, which leaves these children more susceptible to fracture with even minor trauma. The majority (64%) of these fractures occur in males, primarily in the spring. “Fall” was listed as the primary mechanism in one large retrospective study by Ryan et al. Older adolescent athletes can also experience DR fractures. However, these patients have greater bone strength than younger, older, or more sedentary populations. There is usually a higher energy mechanism for these fractures that can lead to more severe injuries. Interestingly, the location of pediatric radial shaft fractures tends to occur more distally with increasing age. [4]
The second peak for DR fractures occurs in adults greater than 50 years old. After hip, they are the second most common fracture in the elderly. Peak incidence is in Caucasian women who are greater than 65 years of age. Osteoporosis is a common risk factor and occurs in 40% of postmenopausal women. The “T-score” is a measure of bone mineral density (BMD) that compares a patient’s BMD relative to that of a healthy 30-year old. The definition of osteoporosis is a T-score of less than -2.5. A T-score of less than -2.5 conveys a 10-year fragility fracture risk of around 15%. Other significant risk factors for DR fractures in patients older than 50 include prior falls, prior fragility fractures after 50 years of age, corticosteroid use, and advanced age. Dementia is also a risk factor in patients greater than 75 years of age. In older patients, each additional risk factor conveys increased probability of suffering a DR fracture. DR fractures extending into a joint space are twice as common in women with diabetes. [7]
Pathophysiology
The term “distal radial fracture” is a catch-all for any fracture of the radius that occurs close to the wrist. This label is deceiving as there are many types of DR fractures. They can all present differently, have different mechanisms of injury, and different management. It is important to be familiar with basic the management and emergent referral indications for each type of DR fracture. This section of the review will discuss the most common distal radial fractures. Treatment options are the topic in another section.
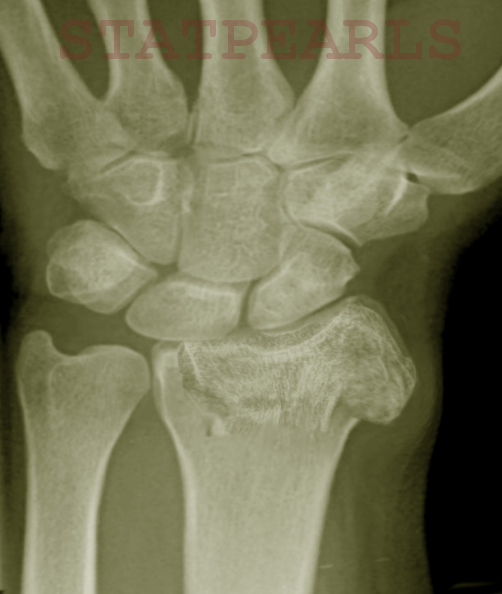
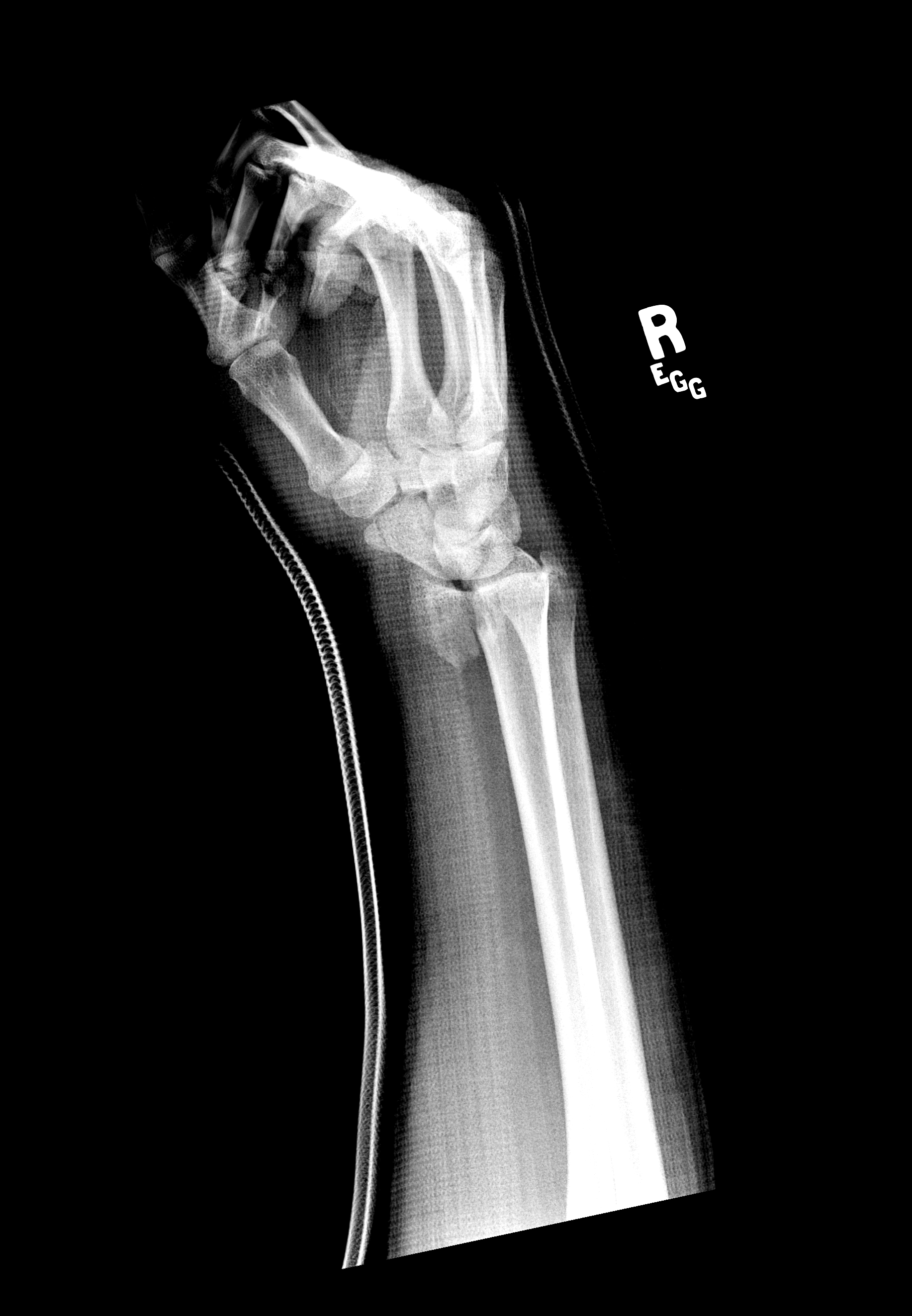
Colles’, Smith’s, Isolated Radial Shaft Fractures, Both Bone Fractures - The Colles’ fracture is the most common fracture of the distal radius in adults. It gets its name from Irish Surgeon, Dr. Abraham Colles, who first described this injury pattern in 1814. The mechanism of injury is classically a FOOSH. It is a metaphyseal fracture that occurs around 1.5 inches proximal to the carpal articulation. Characteristically it presents with dorsal angulation and displacement of the distal fragment of the radius. On X-Ray, the wrist will present with what is known as the “dinner-fork” deformity. The Smith’s fracture is essentially the opposite of the Colles’ fracture. It is often referred to as a “reverse Colles’,” and occurs with a fall onto or a direct blow or force to the dorsum of the hand.
In contrast to Colle’s, the Smith’s fracture will have a volar angulation of the distal fragment. This injury produces what is known as a “garden-spade” deformity on X-Ray. Colles’ and Smith’s fractures often occur in isolation but can have other associated injuries. Isolated radial shaft fractures can occur at any location along the bone. The mechanism of injury for isolated distal third radial shaft fractures is similar to Smith’s and Colles’ fractures, and the management is often identical. Both Bone forearm fractures are also common, especially in the pediatric population. They usually result from a “fall from height.” Both bone fractures involve the radius and ulna. However, the distal radius is frequently involved. There is a high rate of open fractures with this injury pattern.
Chauffeur’s/Radial Styloid Fracture - The Chauffeur’s fracture is an intra-articular fracture of the radius that includes the radial styloid. The fracture fragment can be variable in size. The injury is often the result of a FOOSH injury with a blow to the back of the wrist causing dorsiflexion and abduction causing the scaphoid to compress against the radial styloid. Patients may have small avulsions of the radial styloid that are not clinically significant, but these injuries are often associated with disruption of the radioscaphocapitate and other collateral ligaments; this can lead to lunate dislocation and scapholunate disruption. These fractures were historically suffered by drivers who would need to start their cars using a hand crank. Occasionally these cranks would backfire and forcefully strike drivers on the back of the wrist.
Die-Punch Fracture - A die punch fracture is an intra-articular fracture involving the lunate facet of the radius. The lunate facet is one of the three articular surfaces of the distal radius. It lies between the ulnar articulation and the scaphoid facet. It connects the distal radius to the lunate bone in the wrist. A die-punch fracture occurs with axial loading of the lunate, which causes an impaction fracture to the lunate facet of the radius. This fracture often occurs in isolation but can have associated injuries.
Galeazzi Fracture-Dislocation - The Galeazzi fracture-dislocation is a fracture of the distal third of the radius with an associated distal radioulnar joint (DRUJ) dislocation. These fractures are typically the result of FOOSH injuries. It is an uncommon injury pattern, and the DRUJ component is easi to miss for clinicians. They are labeled based on the direction of ulnar displacement. For example, if the DRUJ disruption causes volar deviation of the ulna, this is classified as a “Volar Galeazzi.”
Barton’s Fracture - A Barton’s fracture is an intra-articular rim fracture of the distal radius. It can be classified as either dorsal or volar. Dorsal rim fractures are more common and result from forced dorsiflexion and pronation. Volar rim fractures often occur with a fall onto a supinated hand/wrist. These forces disrupt the radiocarpal ligaments and subsequent avulsion fracture of the radial rim. In dorsal fractures, the avulsed fragment migrates dorsally. The opposite is true with volar fractures. These fractures are unstable and often present with a dislocation of the carpal bones. [1][2]
Greenstick and Buckle/Torus Fractures - Both Torus and greenstick fractures are incomplete fractures. Pediatric bones are poorly mineralized relative to adults and can bend without frankly breaking. These fractures can occur in any long bone but frequently occur in the metaphysis of the distal radius. Torus fractures occur with axial loading whereas Greenstick fractures result from bending forces. Torus fractures are characterized by buckling of the bony cortex and periosteum without any true fracture lines. There is generally minimal deformity with Torus fractures, and the periosteum and cortex are intact. Greenstick fractures will show bony bending. There will be a fracture of the convex surface with an intact concave surface. These fractures are extremely common in children, and unfortunately frequently missed.
Salter-Harris Type Fractures - A Salter-Harris fracture is a pediatric fracture that involves the epiphyseal plate. These fractures can occur in any bone that has a growth plate but frequently occur in the distal radius. The Salter-Harris scheme was first developed by Doctors William Harris and Robert Salter in 1963 and remains the most common classification system for epiphyseal fractures. Salter-Harris fractures are graded I through IX, with I through V being the most frequently used in clinical practice. Type I is a fracture that runs transversely through the growth plate. Type II runs through the growth plate and the metaphysis. Type III involves the growth plate and epiphysis. Type IV is a fracture of metaphysis, epiphysis, and growth plate. Type V is a complete direct compression fracture of the growth plate. Each of these has different prognosis and management. [4][8][9]
History and Physical
Patients with distal radial fractures will often complain of post-traumatic distal upper extremity pain. DR fractures can also be present as part of a larger multiple trauma presentation. In either case, it is vital not to fixate on an obvious DR injury, and to do a complete evaluation for other possible life-threatening injuries or problems. A systematic approach in trauma situations will prevent a provider from missing occult injuries. Children are also diagnostically difficult as their presentations are often subtle. Children can suffer unwitnessed falls or trauma, and they are often unable to verbalize their symptoms. They can appear well and favoring the uninjured arm may be the only sign of an underlying fracture. [10][8]
The history should focus on the mechanism of injury, duration, and quality of symptoms. Patient questioning should also include details such as their dominant hand, profession, and comorbid conditions. These are all factors that could affect management and potential surgical planning. The history should also serve to help uncover possible complications. Questions should focus on indicators of neurovascular compromise such as numbness, tingling, weakness, or discoloration of the limb. Of note, the median nerve is most commonly injured nerve in DR fractures and will present similarly to an acute carpal tunnel syndrome. [11][12] All pediatric patients with fracture should undergo evaluation for non-accidental trauma.
The focused physical exam should evaluate for gross deformity and general appearance of the distal extremity. Examination of the limb should look for any skin tenting or lacerations that could indicate an open fracture as this will quickly change injury management. There may be crepitus overlying the fracture site. The physical exam should also focus on ruling out complications such as compartment syndrome or other neurovascular issues. Forearm compartments should be soft. The radial pulse should be strong and equal between upper extremities. Capillary refill distal to the fracture should be less than 2-3 seconds. Test the motor function of the radial nerve by having the patient extend the metacarpophalangeal joints of the fingers against resistance. Palmar abduction of the thumb and holding the “A-OK sign” against resistance will test the motor function of the median nerve. Ulnar nerve strength testing is via abduction of the fingers against resistance. The sensation for the median and ulnar nerves should undergo evaluation by two-point discrimination on the pads of the 2nd and 5th fingers, respectively. The radial sensory function may be tested just proximal to the 2nd MCP. Normal two-point discrimination is less than 5mm, or 6mm in the elderly. It is important to document a thorough neurovascular exam as this will be used as a baseline for reexamination by orthopedists and other specialists. Finally, a thorough evaluation of the elbow, carpal bones, and hand should be part of the evaluation. Coexisting DRUJ instability, carpal instability, elbow dislocations, or proximal forearm fractures are easily missed in the evaluation of distal radial fractures. [13]
Evaluation
The essential elements in the evaluation of distal radial fractures are history and physical. These will guide a clinician in deciding what further imaging to obtain. X-rays are the standard imaging modality in the diagnosis of DR fractures. X-rays examination should look for radial height, radial inclination, radial shift, volar tilt, ulnar variance, ulnar styloid fracture, and DRUJ widening.
Computed tomography (CT) images may be necessary if X-rays are equivocal, but the history and physical are strongly suggestive of a fracture. CT imaging may also be useful in subsequent surgical planning for fractures that will go to the operating suite for fixation, especially intra-articular fractures. MRI adds little utility over X-ray and CT in the diagnosis of DR fracture. They may be useful if ligamentous disruption is highly suspected, but these studies are not necessary to perform in the Emergency Department. Advanced imaging such as MRI is more frequently performed in the outpatient setting by orthopedic specialists. [10]
There have been several classification systems devised to over the years to help grade distal radial fractures once diagnostically imaged. Eponyms, such as “Chauffeur’s Fracture,” are helpful in remembering the presentation and mechanism of injury. However, they are unhelpful in describing injury severity or the need for surgical treatment. The Frykman Classification is frequently used for grading these injuries and applies to all eponymous DR fractures. It grades DR fractures based on articular involvement, the degree of radiocarpal joint and DRUJ involvement, and presence or absence of ulnar styloid fractures. It does not account for the degree of comminution, displacement, or other factors that are important in predicting the need for surgical intervention. The Frykman Classification and other similar grading systems have received criticism for their lack of treatment guidance, inter-rater reliability, and poor ease of use. There is no consensus on the best classification system for DR fractures. [2]
When describing X-ray findings to an orthopedist, it is best to use the anatomic approach. A clear description of fracture location, open/closed status, neurovascular status, the degree of angulation, displacement, comminution, impaction, rotation, and presence of articular findings will provide more useful information for an orthopedic surgeon than attempting to grade the fracture using a traditional classification system.
Treatment / Management
The necessary treatment of all confirmed distal radial fractures involves pain management, immobilization, and evaluation for open fractures or neurovascular compromise. Patients with decreased sensation, motor deficit, neuropathy, or tense forearm compartments should receive immediate orthopedic consultation. A pulseless extremity should be seen immediately by an orthopedic surgeon, but may also warrant an additional evaluation by the vascular surgery service if available.
Open fractures are also an indication for emergent orthopedic evaluation. Open fractures grading is by the Gustillo-Anderson Scale, which rates fractures ranging from Grade I through Grade IIIc. Grade I represents a wound <1 cm with minimal contamination and soft tissue damage. Grade IIIc represents arterial injury and severe soft tissue damage. All open fractures graded II or higher will need surgical washout, but this decision is at the discretion of the surgeon. All open fractures should receive appropriate tetanus prophylaxis and antibiotic treatment. Gustillo Grades I-II may receive a first-generation cephalosporin such as intravenous cefazolin. Penicillin-allergic patients may receive IV clindamycin. Gustillo Grades 3 or greater will require the above plus the addition of an aminoglycoside such as gentamicin. [14]
Pain management should be tailored to meet the patient’s needs. Many patients initially require IV preparations such as morphine or fentanyl, although some can be treated adequately with oral medications. Advanced techniques such as hematoma blocks or ultrasound-guided nerve blocks may be a consideration for DR fractures that will require manipulation and reduction. Conscious sedation is also frequently utilized in these situations. Ketamine is a medication used frequently for this purpose, and intranasal fentanyl and midazolam are often a combination choice for pediatric patients. Regardless, the medication provided for conscious sedation should provide both analgesia, sedation, and amnesia. [15]
Closed reduction can often be performed on a case by case basis, and is the primary management for most extra-articular DR fractures. The basic mechanism underlying the closed reduction of DR fractures is traction/counter-traction. Finger traps are the best tool for placing a DR fracture under traction. Alternatively, the patient can be positioned on an exam table in the prone position with elbow supported and flexed. The forearm will dangle off the table. Weights may then be hung from the wrist to provide traction. If neither of these options is available, an assistant can hold the hand in traction while the physician provides counter-traction. To reduce an overlapping DR fracture, manually free the impacted bones by increasing the angulation of the fracture while providing simultaneous counter-traction. Once reduced, the arm should have stabilization with a formal 3-point molded short or long-arm cast or “sugar tong” type splint. Post reduction X-rays should be performed to ensure that the reduction has not fallen out of place.
In addition to the above general management, there are individual guidelines and criteria for each specific type of distal radial fracture. The remainder of this section will review the specific indications for surgery or conservative management in the most common distal radial fractures, as well as some additional pearls. Specific surgical techniques are generally outside the scope of this review and are not discussed here.
Colles’ and Isolated Radial Shaft Fractures -
Adults with closed extra-articular Colles’ fractures and dorsally angulated isolated radial fractures will generally heal well with closed reduction and casting. To be eligible for closed reduction as primary management these fractures should have no more than 5 mm of shortening, 5-degrees change in radial inclination, 2 mm of articular step-off, and 5 degrees of angulation. Successfully closed reductions may undergo splinting in a sugar tong splint until formal short or long arm casting can be performed.
A fracture that cannot have correction with closed reduction to the above parameters will probably require surgery. These patients should receive close follow up with an orthopedist as the fracture is at risk to fall back into the original deformity, even in a splint. Additional indications for urgent surgical referral are fractures with an intra-articular component, carpal ligamentous instability or suspected Triangular Fibrocartilage Complex (TFCC) injury, carpal dislocation, DRUJ instability, significant comminution, and fractures that do not maintain reduction once splinted. Younger patients are often treated more aggressively with surgical intervention than the elderly; this is especially true in young athletes or highly functioning patients who will have significant deterioration in their quality of life with any poor fracture union.
Most pediatric isolated distal radial fractures are more forgiving than in the adult population. The majority of these fractures will heal well without surgical intervention. The criteria for emergent and urgent surgical referral are similar to the adult population. Extra-articular fractures and Salter-Harris grades I and II can generally be managed conservatively, but should still receive close orthopedic follow up. There is an ongoing debate for the acceptable limits of radiographic angulation, malrotation, and bayonet apposition. Despite the controversy, the classically acceptable limitations are most commonly used today. The acceptable limitations for patients under 10 years old include less than 30 degrees of angulation, less than 45 degrees of malrotation, and less than 1 cm of bayonet apposition. In the absence of any emergent referral indications, pediatric patients with DR fractures can undergo closed reduction and close orthopedic follow-up.[10][16][17]
Complex Fractures Involving the Distal Radius -
Complex fractures of the distal radius include those with any associated articular involvement, ligamentous instability, TFCC damage, DRUJ injury, carpal fracture, carpal dislocation, volar displacement, significant comminution, significant angulation, or fracture-dislocation. The notion of “unstable” DR fracture is unfortunately defined primarily by expert opinion, and there is no overarching consensus definition seen in the literature. In general, if the fracture has to undergo reduction, that means it is out of the acceptable parameters for just placing a splint, and is unstable/at risk to fall back into deformity. Generally, these fractures include Barton’s fracture, Smith’s, Chauffeur’s fracture, Die-punch, and Galeazzi fracture-dislocation. Any DRUJ involvement will likely necessitate acute operative treatment unless there is only a minimal ligamentous instability without fracture. If seen in the Emergency Department, these complex fractures must at least be discussed with an orthopedist to determine the need for acute surgery or to arrange close follow up. Before outpatient follow-up, complex or unstable fractures should be reduced to the best degree possible and splinted for soft tissue rest and to prevent neurovascular compromise. [13]
Incomplete Pediatric Fractures of the Distal Radius -
Incomplete pediatric DR fractures include the Greenstick Fracture and the Torus Fracture. Torus fractures generally heal within 3 weeks without any intervention. These patients should follow up with their primary care within 10-14 days of injury. One study by Andrews et al., showed that Torus fractures might be manageable with soft bandaging. None of the patients involved in that study suffered any adverse events. However, it is still generally recommended at the time of this writing to place all Torus fractures in either a removable fiberglass or Velcro splint for 3 weeks. No consensus currently exists on the best splinting method for Torus fractures. [18]
DR Greenstick fractures generally receive conservative management. Minimally displaced or non-displaced fractures should be splinted and then subsequently placed in short arm casts. Children under 5 with DR greenstick fractures can tolerate up to 35 degrees of lateral angulation and 10 degrees of AP angulation. Children between 5 to 10 years of age can tolerate up to 25 degrees of lateral angulation and 10 degrees of AP angulation. Children older than ten should have reduction to less than 20 degrees of lateral angulation and 0 degrees of AP angulation. DR greenstick fractures should generally be left in a short arm cast for 4-6 weeks. [19][19][19]
Pediatric Growth Plate Fractures of the Distal Radius -
Salter-Harris fractures can occur in any pediatric bone with a growth plate. They frequently occur in the distal radius. As above, in the absence of neurovascular compromise or incomplete reduction, Salter-Harris grades I and II can be managed with closed reduction and casting. These fractures are not articular and have a good prognosis. Only one attempt should be made at closed reduction to prevent additional growth plate injury which can lead to growth arrest and permanent deformity.
Higher grade Salter-Harris fractures of the distal radius are usually unstable and require surgical fixation. Clinicians must maintain a high level of suspicion for Grade V Salter-Harris DR fractures, especially for high energy mechanism injuries, as they are easy to miss. If untreated, these patients can suffer growth plate arrest. In all cases, growth plate fractures must be at least evaluated by an orthopedist within 7 days. These fractures usually heal after 6 weeks and should be re-evaluated frequently for at a minimum one year to ensure that the growth plate has suffered no permanent damage. [20][9]
Differential Diagnosis
- Colles’ fracture
- Smith’s fracture
- Barton fracture
- Chauffeur’s fracture/radial styloid fracture
- Isolated distal radial fracture
- Both bone/radial and ulnar fracture
- Scaphoid/carpal bone fracture
- Scaphoid/carpal bone dislocation
- Distal radioulnar joint dislocation
- Carpal ligamentous disruption/TFCC injury
- Die-punch fracture
- Proximal metacarpal fracture
- Monteggia fracture
- Galeazzi fracture
- Greenstick fracture
- Torus/Buckle fracture
- Salter-Harris/growth plate fracture of radius (pediatric)
Prognosis
Simple distal radial fractures usually heal well and have no long-term complications. Complex fractures have variable prognoses that are multifactorial. Complex fractures have higher rates of malunion or nonunion, decreased joint function, neuropathic pain, complex regional pain syndrome, and post-traumatic arthritis. [13]Carpal tunnel syndrome and complex regional pain syndrome are the most common complications of DR fracture, followed by tendinitis. [12]Primary vascular disruption can occur in cases of significant trauma. Secondary or delayed vascular complications are uncommon. Children have the risk of permanent physeal disruption and are more prone to forearm contractures. [8]
Primary care and emergency clinicians can mitigate these complications by providing quality reduction and splinting, as well as referring for early orthopedic follow up in an appropriate time-frame. Additionally, most older adults who suffer distal radial fractures should undergo an evaluation for osteoporosis or osteopenia. In the elderly, these fractures may be an indicator of increased risk for osteoporosis, pathologic fractures, and overall increased morbidity and mortality. [21]
Deterrence and Patient Education
The radius is one of two long bones in the forearm. The radius lies under the thumb, between the wrist and elbow. The portion of the radius that is closest to the wrist is known as the “distal radius.” This part of the bone has the potential to fracture with a fall on an outstretched hand, but can also fracture with any fall or trauma to the upper extremity. The most frequent symptoms of a distal radius fracture are pain and decreased mobility of the wrist. Distal radius fractures are most frequently diagnosed with an X-ray, but sometimes other imaging is needed. Most patients with distal radius fractures can heal on their own after several weeks in a splint or cast. Some patients will require immediate or urgent surgery to correct the fracture. If you believe that you have a distal radius fracture, please go immediately to your nearest emergency room for evaluation.
Enhancing Healthcare Team Outcomes
Distal radial injuries are usually identified easily in the context of isolated trauma. "Front Line" providers in primary care and emergency medicine should familiarize themselves with the routine management of these injuries, and the indications for urgent surgical evaluation. Surgeons should educate local providers and emergency nurses and providers about how best to arrange follow-up for patients with distal radius injuries. Coordination between specialties, nursing support teams and clinicians will provide the best outcomes for patients and reduce long-term sequelae. In cases of significant debility or poly-trauma, inpatient teams should maintain a high index of suspicion for distal radius fractures during their tertiary surveys and have a low threshold to image upper extremities. (Level I)