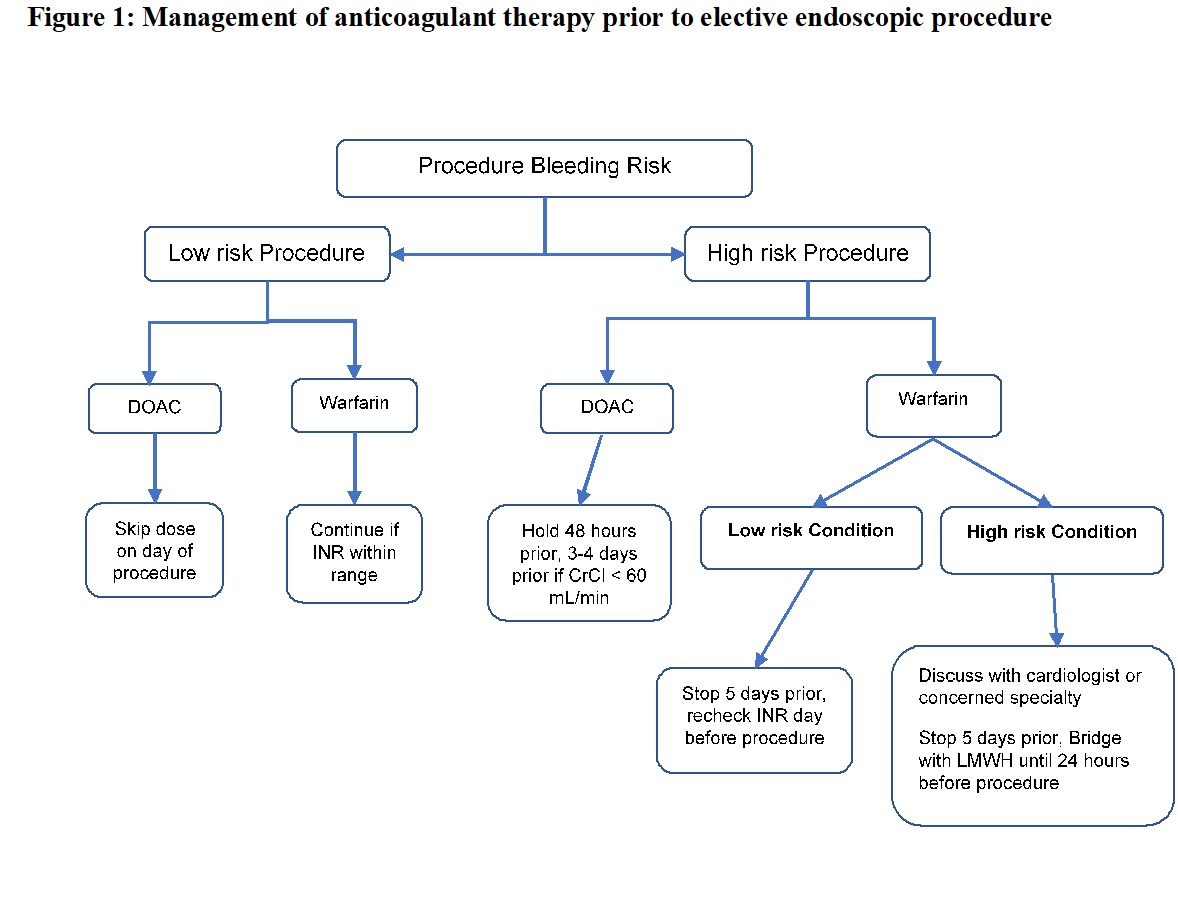
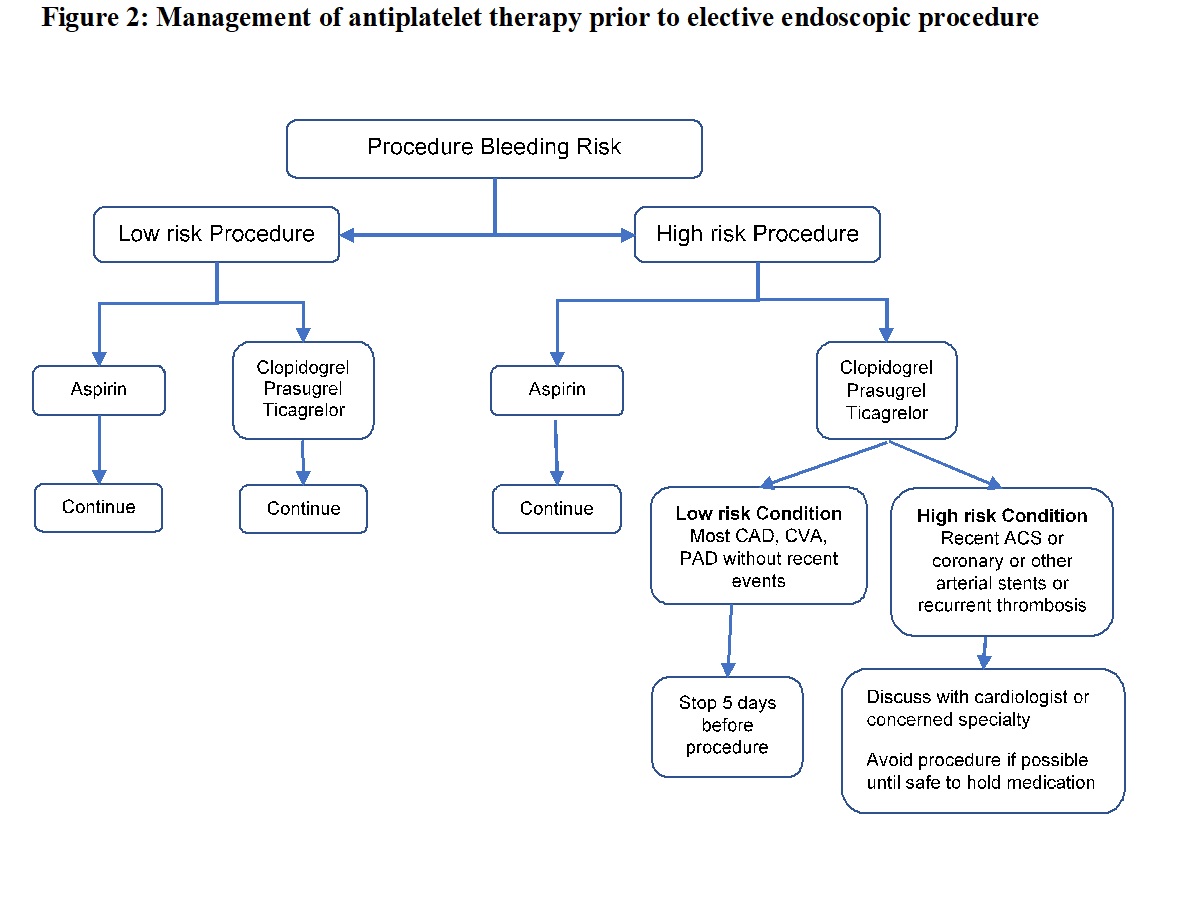
[1]
ASGE Standards of Practice Committee, Acosta RD, Abraham NS, Chandrasekhara V, Chathadi KV, Early DS, Eloubeidi MA, Evans JA, Faulx AL, Fisher DA, Fonkalsrud L, Hwang JH, Khashab MA, Lightdale JR, Muthusamy VR, Pasha SF, Saltzman JR, Shaukat A, Shergill AK, Wang A, Cash BD, DeWitt JM. The management of antithrombotic agents for patients undergoing GI endoscopy. Gastrointestinal endoscopy. 2016 Jan:83(1):3-16. doi: 10.1016/j.gie.2015.09.035. Epub 2015 Nov 24
[PubMed PMID: 26621548]
[2]
Veitch AM, Vanbiervliet G, Gershlick AH, Boustiere C, Baglin TP, Smith LA, Radaelli F, Knight E, Gralnek IM, Hassan C, Dumonceau JM. Endoscopy in patients on antiplatelet or anticoagulant therapy, including direct oral anticoagulants: British Society of Gastroenterology (BSG) and European Society of Gastrointestinal Endoscopy (ESGE) guidelines. Endoscopy. 2016 Apr:48(4):c1. doi: 10.1055/s-0042-122686. Epub 2017 Jan 23
[PubMed PMID: 28114689]
[3]
Chan FKL, Goh KL, Reddy N, Fujimoto K, Ho KY, Hokimoto S, Jeong YH, Kitazono T, Lee HS, Mahachai V, Tsoi KKF, Wu MS, Yan BP, Sugano K. Management of patients on antithrombotic agents undergoing emergency and elective endoscopy: joint Asian Pacific Association of Gastroenterology (APAGE) and Asian Pacific Society for Digestive Endoscopy (APSDE) practice guidelines. Gut. 2018 Mar:67(3):405-417. doi: 10.1136/gutjnl-2017-315131. Epub 2018 Jan 13
[PubMed PMID: 29331946]
Level 1 (high-level) evidence
[4]
Lip GY, Nieuwlaat R, Pisters R, Lane DA, Crijns HJ. Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: the euro heart survey on atrial fibrillation. Chest. 2010 Feb:137(2):263-72. doi: 10.1378/chest.09-1584. Epub 2009 Sep 17
[PubMed PMID: 19762550]
Level 3 (low-level) evidence
[5]
Douketis JD, Spyropoulos AC, Spencer FA, Mayr M, Jaffer AK, Eckman MH, Dunn AS, Kunz R. Perioperative management of antithrombotic therapy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012 Feb:141(2 Suppl):e326S-e350S. doi: 10.1378/chest.11-2298. Epub
[PubMed PMID: 22315266]
Level 1 (high-level) evidence
[6]
Kwok A, Faigel DO. Management of anticoagulation before and after gastrointestinal endoscopy. The American journal of gastroenterology. 2009 Dec:104(12):3085-97; quiz 3098. doi: 10.1038/ajg.2009.469. Epub 2009 Aug 11
[PubMed PMID: 19672250]
[7]
Schulman S, Elbazi R, Zondag M, O'Donnell M. Clinical factors influencing normalization of prothrombin time after stopping warfarin: a retrospective cohort study. Thrombosis journal. 2008 Oct 16:6():15. doi: 10.1186/1477-9560-6-15. Epub 2008 Oct 16
[PubMed PMID: 18925967]
Level 2 (mid-level) evidence
[8]
Garcia DA, Regan S, Henault LE, Upadhyay A, Baker J, Othman M, Hylek EM. Risk of thromboembolism with short-term interruption of warfarin therapy. Archives of internal medicine. 2008 Jan 14:168(1):63-9. doi: 10.1001/archinternmed.2007.23. Epub
[PubMed PMID: 18195197]
[9]
Douketis JD, Spyropoulos AC, Kaatz S, Becker RC, Caprini JA, Dunn AS, Garcia DA, Jacobson A, Jaffer AK, Kong DF, Schulman S, Turpie AG, Hasselblad V, Ortel TL, BRIDGE Investigators. Perioperative Bridging Anticoagulation in Patients with Atrial Fibrillation. The New England journal of medicine. 2015 Aug 27:373(9):823-33. doi: 10.1056/NEJMoa1501035. Epub 2015 Jun 22
[PubMed PMID: 26095867]
[10]
Dubois V, Dincq AS, Douxfils J, Ickx B, Samama CM, Dogné JM, Gourdin M, Chatelain B, Mullier F, Lessire S. Perioperative management of patients on direct oral anticoagulants. Thrombosis journal. 2017:15():14. doi: 10.1186/s12959-017-0137-1. Epub 2017 May 15
[PubMed PMID: 28515674]
[11]
Weitz JI, Quinlan DJ, Eikelboom JW. Periprocedural management and approach to bleeding in patients taking dabigatran. Circulation. 2012 Nov 13:126(20):2428-32. doi: 10.1161/CIRCULATIONAHA.112.123224. Epub
[PubMed PMID: 23147769]
[12]
Patrono C, Ciabattoni G, Patrignani P, Pugliese F, Filabozzi P, Catella F, Davì G, Forni L. Clinical pharmacology of platelet cyclooxygenase inhibition. Circulation. 1985 Dec:72(6):1177-84
[PubMed PMID: 3933848]
[13]
Gurbel PA, Bliden KP, Butler K, Tantry US, Gesheff T, Wei C, Teng R, Antonino MJ, Patil SB, Karunakaran A, Kereiakes DJ, Parris C, Purdy D, Wilson V, Ledley GS, Storey RF. Randomized double-blind assessment of the ONSET and OFFSET of the antiplatelet effects of ticagrelor versus clopidogrel in patients with stable coronary artery disease: the ONSET/OFFSET study. Circulation. 2009 Dec 22:120(25):2577-85. doi: 10.1161/CIRCULATIONAHA.109.912550. Epub 2009 Nov 18
[PubMed PMID: 19923168]
Level 1 (high-level) evidence
[14]
Eisenberg MJ, Richard PR, Libersan D, Filion KB. Safety of short-term discontinuation of antiplatelet therapy in patients with drug-eluting stents. Circulation. 2009 Mar 31:119(12):1634-42. doi: 10.1161/CIRCULATIONAHA.108.813667. Epub 2009 Mar 16
[PubMed PMID: 19289638]
[15]
Rubin TA, Murdoch M, Nelson DB. Acute GI bleeding in the setting of supratherapeutic international normalized ratio in patients taking warfarin: endoscopic diagnosis, clinical management, and outcomes. Gastrointestinal endoscopy. 2003 Sep:58(3):369-73
[PubMed PMID: 14528210]
[16]
Shingina A, Barkun AN, Razzaghi A, Martel M, Bardou M, Gralnek I, RUGBE Investigators. Systematic review: the presenting international normalised ratio (INR) as a predictor of outcome in patients with upper nonvariceal gastrointestinal bleeding. Alimentary pharmacology & therapeutics. 2011 May:33(9):1010-8. doi: 10.1111/j.1365-2036.2011.04618.x. Epub 2011 Mar 8
[PubMed PMID: 21385193]
Level 1 (high-level) evidence
[17]
Holbrook A, Schulman S, Witt DM, Vandvik PO, Fish J, Kovacs MJ, Svensson PJ, Veenstra DL, Crowther M, Guyatt GH. Evidence-based management of anticoagulant therapy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012 Feb:141(2 Suppl):e152S-e184S. doi: 10.1378/chest.11-2295. Epub
[PubMed PMID: 22315259]
Level 1 (high-level) evidence
[18]
Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP 3rd, Fleisher LA, Jneid H, Mack MJ, McLeod CJ, O'Gara PT, Rigolin VH, Sundt TM 3rd, Thompson A. 2017 AHA/ACC Focused Update of the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Journal of the American College of Cardiology. 2017 Jul 11:70(2):252-289. doi: 10.1016/j.jacc.2017.03.011. Epub 2017 Mar 15
[PubMed PMID: 28315732]
Level 1 (high-level) evidence
[19]
Pollack CV Jr, Reilly PA, Eikelboom J, Glund S, Verhamme P, Bernstein RA, Dubiel R, Huisman MV, Hylek EM, Kamphuisen PW, Kreuzer J, Levy JH, Sellke FW, Stangier J, Steiner T, Wang B, Kam CW, Weitz JI. Idarucizumab for Dabigatran Reversal. The New England journal of medicine. 2015 Aug 6:373(6):511-20. doi: 10.1056/NEJMoa1502000. Epub 2015 Jun 22
[PubMed PMID: 26095746]
[20]
Connolly SJ, Crowther M, Eikelboom JW, Gibson CM, Curnutte JT, Lawrence JH, Yue P, Bronson MD, Lu G, Conley PB, Verhamme P, Schmidt J, Middeldorp S, Cohen AT, Beyer-Westendorf J, Albaladejo P, Lopez-Sendon J, Demchuk AM, Pallin DJ, Concha M, Goodman S, Leeds J, Souza S, Siegal DM, Zotova E, Meeks B, Ahmad S, Nakamya J, Milling TJ Jr, ANNEXA-4 Investigators. Full Study Report of Andexanet Alfa for Bleeding Associated with Factor Xa Inhibitors. The New England journal of medicine. 2019 Apr 4:380(14):1326-1335. doi: 10.1056/NEJMoa1814051. Epub 2019 Feb 7
[PubMed PMID: 30730782]
[21]
Kato M, Uedo N, Hokimoto S, Ieko M, Higuchi K, Murakami K, Fujimoto K. Guidelines for Gastroenterological Endoscopy in Patients Undergoing Antithrombotic Treatment: 2017 Appendix on Anticoagulants Including Direct Oral Anticoagulants. Digestive endoscopy : official journal of the Japan Gastroenterological Endoscopy Society. 2018 Jul:30(4):433-440. doi: 10.1111/den.13184. Epub
[PubMed PMID: 29733468]
[22]
Douketis JD, Spyropoulos AC, Duncan J, Carrier M, Le Gal G, Tafur AJ, Vanassche T, Verhamme P, Shivakumar S, Gross PL, Lee AYY, Yeo E, Solymoss S, Kassis J, Le Templier G, Kowalski S, Blostein M, Shah V, MacKay E, Wu C, Clark NP, Bates SM, Spencer FA, Arnaoutoglou E, Coppens M, Arnold DM, Caprini JA, Li N, Moffat KA, Syed S, Schulman S. Perioperative Management of Patients With Atrial Fibrillation Receiving a Direct Oral Anticoagulant. JAMA internal medicine. 2019 Nov 1:179(11):1469-1478. doi: 10.1001/jamainternmed.2019.2431. Epub
[PubMed PMID: 31380891]