Continuing Education Activity
Blistering distal dactylitis (BDD) predominantly affects children and is characterized by the emergence of multiple fluid-filled lesions that specifically target the volar fat pad of the distal phalanx of the digits. BDD has also been reported in immunocompromised individuals. The pathogenesis of the disease remains unclear. A wound biopsy often demonstrates a superficial split with neutrophils and spongiosis. Systemic antibiotics are commonly recommended to avert the development of new lesions and the spread of infection to other sites. This activity reviews the comprehensive assessment and effective management strategies pertinent to BDD, underscoring the pivotal role of an interprofessional team in enhancing patient care. An emphasis is placed on the prevalent culture findings, predominantly detecting group A beta-hemolytic Streptococcus in the bacterial cultures derived from these fluid-filled lesions, aiding in diagnostic confirmation and tailored treatment plans for affected patients. The course discussion aims to equip healthcare professionals with the latest advancements and evidence-based practices to optimize patient outcomes.
Objectives:
Identify the role of group A beta-hemolytic Streptococcus in the etiology of blistering distal dactylitis.
Evaluate the typical presentation of bullae in blistering distal dactylitis.
Compare the use of incision and drainage, wet dressing, and systemic antibiotics in managing blistering distal dactylitis.
Communicate the importance of improving care coordination among the interprofessional team to enhance the delivery of care for patients affected by blistering distal dactylitis.
Introduction
Blistering distal dactylitis (BDD) is a localized bacterial infection manifesting as fluid-filled lesions over the fingers, especially in children.[1] Classically, BDD is localized to the volar fat pad of the distal phalanx of the digits, presenting as a medium-to-large nontender blister filled with a thin, white fluid. Bacterial cultures from this fluid most commonly grow Group A beta-hemolytic Streptococcus.
Etiology
Typically, BDD is caused by group A beta-hemolytic Streptococcus infection. Additionally, etiological agents such as Group B Streptococcus, Staphylococcus aureus, and methicillin-resistant S aureus (MRSA) have been reported.[2][3][4][5][4] The organisms tend to invade the skin through open wounds from insect bites, traumatic cuts, erosions, burns, or abnormalities of skin appendages such as nails. Additionally, there were recorded instances of combined bacterial and viral infections, namely involving β-haemolyticus Streptococcus and S aureus, β-haemolyticus Streptococcus and Staphylococcus epidermidis, and S aureus and herpes simplex virus.[6] Based on the clinical presentation and staphylococcal etiology, certain authors classify BDD as a clinical variant of bullous impetigo. The presence of several bullae is indicative that S aureus is the responsible pathogen.[7]
Epidemiology
Children aged 2 to 16 are most commonly affected. There have been case reports of BDD occurring in children younger than 1 and even in adults. BDD has also been reported in immunocompromised individuals, including HIV-positive cases, and in people with diabetes.
Pathophysiology
The actual pathogenesis of the blister is not very clear. Streptococcus does not seem to cause the development of bullae, either through a toxin-mediated or another indirect mechanism. S aureus, however, can produce an exfoliative toxin that cleaves desmoglein-1 in the superficial epidermis, leading to bulla formation. It should be noted that Streptococcus and S aureus–associated BDD are clinically indistinguishable, making the role of toxins in BDD uncertain.
Histopathology
A wound biopsy usually demonstrates spongiosis with neutrophils.[3] In some cases, the presence of erosions suggests that the epidermis split is superficial.[8][6] BDD has not been described to cause the severe necrosis that occurs in toxic shock syndrome and results in the formation of acral bullae.
History and Physical
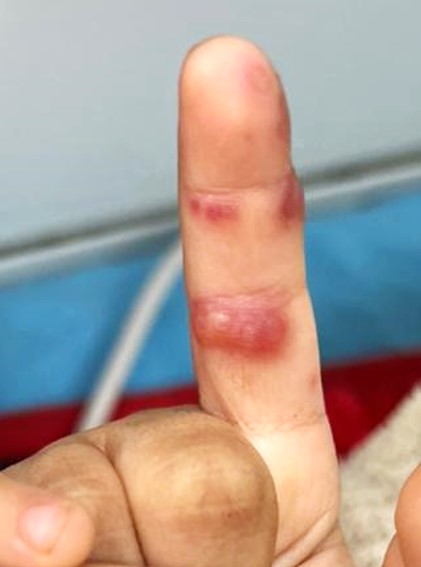
Dactylitis refers to inflammation of a digit and can be caused by inflammatory, infectious, or noninfectious factors. BDD may also affect the proximal phalangeal and palmar surfaces, as well as the toes. For these situations, the name "blistering dactylitis" is a more suitable description (see Image. Blistering Dactylitis).[9] This inflammatory process may affect only the bone (as in sickle cell dactylitis and syphilitic dactylitis), the bone, soft tissues, and skin (as in tuberculous dactylitis and sarcoid dactylitis), or only the skin (as in BDD). The presence of a thick stratum corneum and stratum lucidum over palms and soles could be the reason for the eruption of blisters in BDD.
A detailed history of thumb sucking, insect bites, or contact with chemicals or heat gives clues to differentiate these conditions from BDD. A single instance of BDD occurring after an animal bite was documented.[10] BDD presents as a single, or sometimes multiple, oval-shaped tense bullae containing seropurulent fluid on an erythematous base over the palmar aspect of the finger, which may extend dorsally to involve lateral nail folds. The lesions usually range in size from 10 mm to 30 mm. A darkening of the skin may be noticed a few days before the actual onset of the blisters. Typically, lymphangitis, lymphadenopathy, and fever are absent.[9] Nonetheless, some patients may complain of pain and tenderness in the area and may be febrile. The blisters progress to form bullae with central erosions or simple erosion with adherent layers of skin.[11][12] Bacterial infections of the eye, upper respiratory tract, and gastrointestinal or genitourinary tract may occasionally coexist, highlighting the need for systemic antibiotic therapy.
Evaluation
The fluid can be collected after puncturing or deroofing the blister. The fluid is then examined for Gram-stained smear bacterial culture and sensitivity to confirm the diagnosis and start the appropriate antibiotics.[13][14] Staphylococci and streptococci are grouped as gram-positive cocci. Staphylococci form clumps, whereas streptococci grow in chains. They can be discriminated against by the catalase test because staphylococci can produce catalase.
Treatment / Management
For tense and tender bullae, it is recommended to perform incision and drainage followed by wet dressing. Bullae may also be deflated with a sterile needle, leaving the blister roof intact. Wet compresses are helpful for rapid resolution of the bulla, followed by topical antibiotics. BDD can coexist with and may be secondary to clinically indiscernible bacterial infections of the upper and lower respiratory or gastrointestinal tract, which highlights the need for systemic antibiotic therapy.
Topical antibiotics alone are inadequate in most cases. Systemic antibiotics are commonly recommended to avert the development of new lesions and the spread of infection to other sites. Oral antibiotics also decrease the chances of spreading to other people. B-lactamase–resistant antibiotics (flucloxacillin, dicloxacillin, and cloxacillin) are the drug of choice because S aureus is often resistant to penicillin.
For cases that show MRSA positivity along with systemic signs, intravenous vancomycin is indicated. Improvement starts 24 to 48 hours after initiating antibiotics; however, treatment should be continued for 7 to 14 days, depending on the clinical response. Patients who do not improve after 48 hours, develop systemic signs, or have worsening local symptoms need to be reevaluated by sending specimens for culture and susceptibility testing.
Differential Diagnosis
Differential diagnoses for BDD include:
Herpetic whitlow: Herpes simplex virus (HSV) infection can resemble BDD with grouped vesicular lesions. Initial vesicles of BDD tend to be larger than those of herpetic whitlow. A Tzanck smear from the vesicle shows viral cytopathic effects. Polymerase chain reaction for HSV and antibodies to HSV-1 and HSV-2 can be sent for confirmation in suspected cases.
It has been suggested that BDD and herpetic whitlow could coexist at the distal phalanx. One hypothesis for this is autoinoculation due to thumb sucking in children. Infants can also be exposed to infection when using their fingers to explore the mouths of infected adults. Clinical response to antibiotics makes herpetic whitlow unlikely and can be used to differentiate from BDD.
Friction blisters: Friction blisters can resemble BDD, including those due to thumb sucking (and, in the case of toes, secondary to friction due to new shoes).
Paronychia: Nail fold swelling and nail dystrophy with irregular pitting and ridges are common in paronychia. The initial lesions of BDD are more distal than those of paronychia.
Burns: BDD can be distinguished from burns by the purulence of the vesicular fluid and Gram stain, whic reveal white blood cells and bacteria.
Insect bites: Insect bites tend to be itchy rather than painful, thus distinguishing them from BDD.
Contact dermatitis: A history of contact with common irritants can distinguish it from BDD. More diagnostic testing includes the patch test.
Pompholyx: Pompholyx presents as recurrent crops of deep-seated blisters on the palms and soles that cause intense itchiness or a burning sensation. The condition can occur secondary to inflammatory dermatophyte infections, palmoplantar hyperhidrosis, or contact with irritants.
Bullous impetigo: The vesicles of bullous impetigo are more superficial than those of BDD, although the etiology is the same. A bacterial culture more commonly grows Staphylococcus than Streptococcus.
Blistering disorders : Blistering disorders like epidermolysis bullosa simplex (EBS) and localized bullous pemphigoid (BP)-EBS commonly occur over exposed trauma-prone sites. Histopathology, including direct immunofluorescence, can confirm BP. Other tools, like antigen mapping, also help in diagnosis.
Prognosis
BDD usually resolves rapidly with the appropriate antibiotics and local dressing without complications or sequelae. However, digital amputation after BDD has been reported, necessitating the need to treat infections aggressively, especially in HIV-positive individuals. Typically, recurrence is rarely reported.[15]
Complications
BDD is rarely complicated and is generally known to subside with proper treatment. Recurrent BDD has been described in a case of ingrowing toenails.[16] Osteitis and auto-amputation have been described in an HIV-positive infant who had not received proper treatment until two months after the onset of symptoms.[17] Nonetheless, no cases of post-streptococcal glomerulonephritis have been reported in the literature.
Consultations
Medical professionals, particularly internists, should maintain a high level of suspicion for this disease in individuals of all age groups, rather than just children, and should be mindful of the possibility of it happening again.
Deterrence and Patient Education
Patients should promptly identify the tense blisters that specifically affect the volar fat pad of the distal phalanx of the digits, as they indicate an infection that requires treatment. Failure to promptly diagnose and treat this illness may lead to severe complications.
Pearls and Other Issues
Blistering distal dactylitis primarily affects children; however, it can occasionally occur in older individuals. Recurrent and remitting episodes of blistering distal dactylitis are infrequent. Lesions are not free from bacteria, and in the majority of cases, a culture will reveal the presence of Streptococcus pyogenes or Staphylococcus aureus. Infection typically occurs following trauma, such as an insect bite, abrasion, burn, or finger prick. The recommended treatment involves performing an incision and draining of the bullae, along with the administration of either topical antibiotics or a brief course of systemic medicines targeting staphylococcus and streptococcus bacteria.
Enhancing Healthcare Team Outcomes
The diagnosis and management of BDD can be challenging and are best done with an interprofessional team that includes a nurse practitioner, a primary care provider, an emergency department physician, and an infectious disease expert. The key is to drain and obtain fluid for culture from the bullae. However, it is important to know that BDD can coexist with, and may be secondary to, clinically indiscernible bacterial infections of the upper and lower respiratory or gastrointestinal tract, which underlines the need for systemic antibiotic therapy. The condition is always treated with oral antibiotics, and the pharmacist should ensure compliance with treatment. For those treated promptly, the outcomes are good, but when there is a lack of compliance with antibiotics, the infection can have an aggressive course.[18]