Continuing Education Activity
Paronychia is an infection of the proximal and lateral toenail and fingernail folds which may occur spontaneously or following trauma or manipulation. It is one of the most common infections of the hand, and it is essential to know how to treat it appropriately. This activity reviews the cause, presentation, and pathophysiology of paronychia and highlights the role of the interprofessional team in its management.
Objectives:
- Identify the etiology and pathophysiology of paronychia.
- Review the appropriate examination and evaluation of paronychia.
- Describe the appropriate treatment and management of paronychia.
- Summarize interprofessional team strategies for improving care coordination and communication to treat paronychia successfully and improve patient outcomes.
Introduction
Paronychia is an infection of the proximal and lateral fingernails and toenails folds, including the tissue that borders the root and sides of the nail. This condition can occur spontaneously or following trauma or manipulation. Paronychia is among the most common infections of the hand. Paronychia results from the disruption of the protective barrier between the nail and the nail fold, introducing bacteria and predisposing the area to infection. Acute paronychia is usually limited to one nail; however, if drug-induced, it can involve many nails.[1][2]
Etiology
The classification of paronychia is according to the clinical presentation:
- Acute paronychia - Lasting less than six weeks, painful and purulent condition; most frequently caused by a bacterial infection, especially staphylococci.
- Chronic paronychia - Usually caused by mechanical or chemical factors and sometimes infectious etiology like a fungal infection, especially Candida species. Risk factors include occupation (dishwasher, bartender, housekeeper), certain medications, and immunosuppression (diabetes, HIV, malignancy).
Classification can also be by etiology:
- Bacterial, commonly staphylococci
- Viral, commonly Herpes simplex virus
- Fungal, commonly Candida species
Noninfectious causes of paronychia can include contact irritants, excessive moisture, and medication reaction.[3]
Epidemiology
Paronychia is more common in women than in men, with a female-to-male ratio of 3 to 1. Usually, they affect manual labor workers or patients in occupations that require them to have their hands or feet submerged in water for prolonged periods (e.g., dishwashers). Middle-aged females are at the highest risk of infection.[4]
Pathophysiology
Paronychia results from the disruption of the protective barrier between the nail and the nail fold, which is the cuticle. Trauma (including manicures and pedicures), infections (including bacterial, viral, and fungal), structural abnormalities, and inflammatory diseases (ex. psoriasis) are predisposing factors. Organisms will enter the moist nail crevice, which leads to colonization of the area. The majority of acute paronychias are due to trauma, nail-biting, aggressive manicuring, artificial nails, and may involve a retained foreign body. Infections are most commonly the result of Staphylococcus aureus. Streptococci and Pseudomonas are more common in chronic infections. [5] Less common causative agents include gram-negative organisms, dermatophytes, herpes simplex virus, and yeast. Children are prone to acute infection due to habitual nail-biting and finger sucking, leading to direct inoculation of oral flora, which would include both aerobic bacteria (S. aureus, streptococci, Eikenella corrodens) and anaerobic bacteria (Fusobacterium, Peptostreptococcus, Prevotella, Porphyromonas spp.).[6]
History and Physical
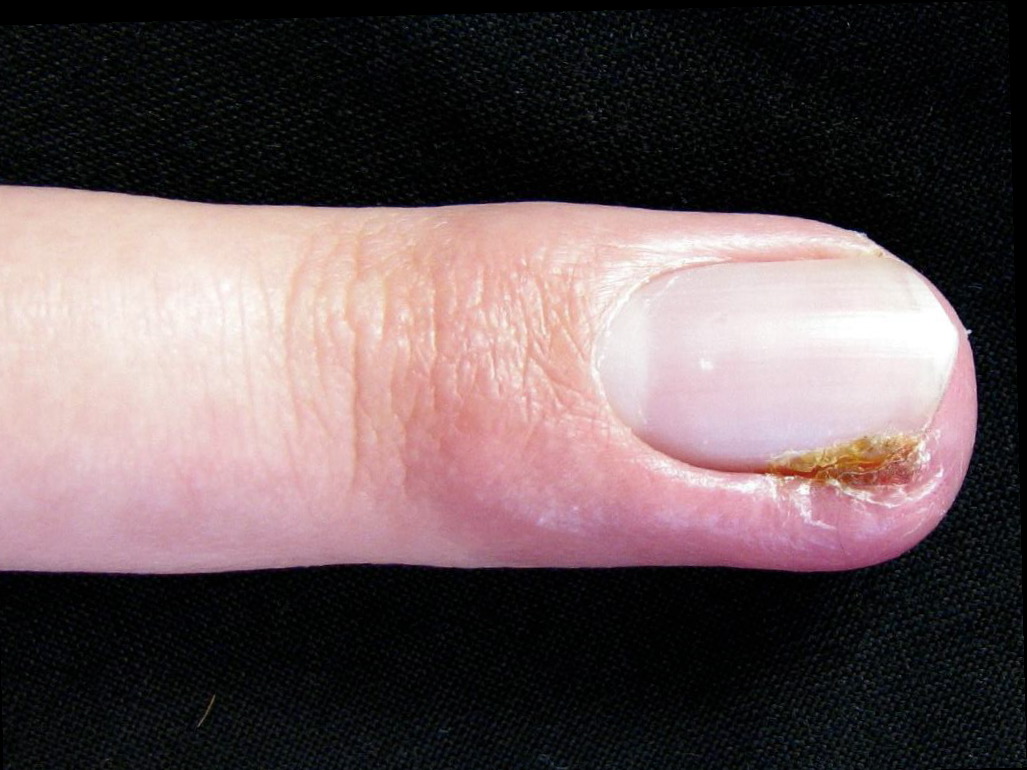
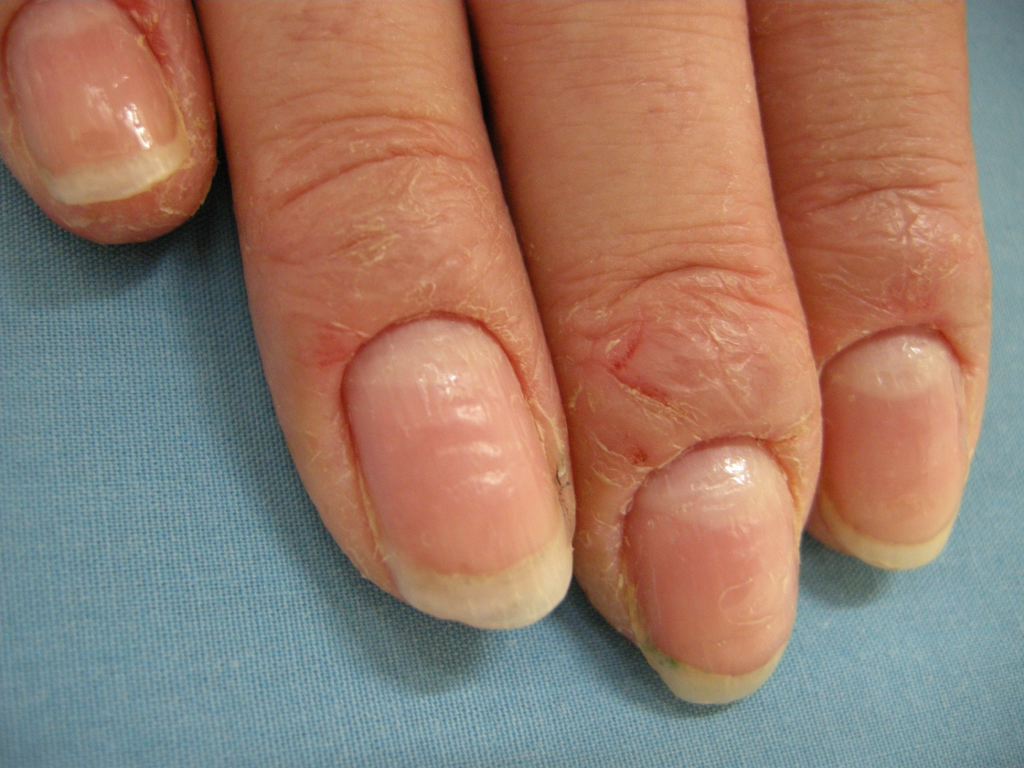
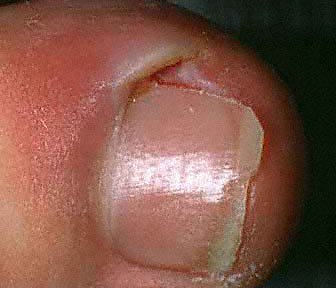
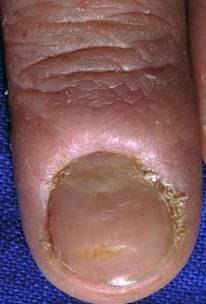
Paronychia is most commonly an acute inflammatory process causing painful redness and swelling to the lateral nail fold and is primarily diagnosed based on clinical presentation. The patient will usually present within the first few days of infection due to the pain. History may include recent trauma, infection, structural abnormalities, or inflammatory diseases. Occupation and working environment are critical historical findings; homemakers, bartenders, and dishwashers seem predisposed to developing chronic paronychia. Past medical history inquiry should include any debilitating illness like diabetes and HIV.[7] A list of medications the patient is currently taking may help determine the cause of chronic paronychia.[8]
Physical exam for acute paronychia will reveal an erythematous, swollen, and tender lateral nail fold. If an abscess is present, there may be an area of fluctuance. If there is an uncertainty of an abscess present, a digital pressure test may prove useful; the examiner can do this by applying pressure to the volar aspect of the involved digit. If an abscess is present, a larger than expected area of blanching will be visible at the paronychia and drainage will be needed. In chronic paronychia, the nail fold may be red and swollen, but fluctuance is rare. The nail fold may appear boggy, and the nail plate can become thickened and discolored. Other common findings of chronic paronychia may be a retraction of the proximal nail fold, nail dystrophy, and loss of the cuticle.[3]
Evaluation
To diagnose a paronychia, you will need to obtain a good history and physical, revealing a swollen and tender nail fold, as there is no laboratory testing or imaging that will lead to the diagnosis. The infection is usually straightforward; however, the presence of an abscess is not always evident, and the digital pressure test described above can be used to guide you.
Treatment / Management
Paronychias are usually either treated with incision and drainage or antibiotics. If there is inflammation with no definite abscess, treatment can include warm soaks with water or antiseptic solutions (chlorhexidine, povidone-iodine) and antibiotics. Warm soaks should be for 10 to 15 minutes, multiple times a day. There is not strong evidence recommending topical vs. oral antibiotics, and this may be physician-dependent based on experience. Antibiotic used should have staph aureus coverage. Topical antibiotics used may be a triple antibiotic ointment, bacitracin, or mupirocin. In patients failing topical treatment or more severe cases, oral antibiotics are an option; dicloxacillin (250mg four times a day) or cephalexin (500mg three to four times a day). Indications for antibiotics with anaerobic coverage include patients where there is a concern for oral inoculation; this would require the addition of clindamycin or amoxicillin-clavulanate. If the patient has risk factors for MRSA (including but not limited to: recent hospitalization, recent surgery, ESRD on hemodialysis, HIV/AIDS, IVDU, resident of long term care facility), chose an antibiotic with the appropriate coverage. Options include trimethoprim/sulfamethoxazole DS (1 to 2 tablets twice a day), clindamycin (300 to 450mg four times a day) or doxycycline (100mg twice a day).[3]
If an abscess is present, the infection will require drainage. Incision and drainage are usually with a #11 scalpel, and the blade is inserted under the eponychial fold (lateral nail fold) until pus begins to drain. Local or digital block anesthetic is generally helpful to allow comfort to ensure complete drainage. An abscess requires irrigation with normal saline, and if the abscess and incision site is large, the clinician can pack it with plain gauze for continued drainage. If the abscess extends to the nail bed or is associated with an ingrown nail, a partial nail plate removal may be needed. If an abscess is present and not drained, it can spread under the nail to the other side and result in a "run-around abscess." This scenario may require complete removal of the nail to allow adequate drainage and treatment. Warm soaks should be initiated after incision and drainage to encourage continued drainage by keeping the wound open and prevent secondary infection. The patient should follow up with a provider in the next 24 to 48 hours to ensure drainage and to look for signs of worsening infection. Usually, incision and drainage is the adequate treatment of acute paronychia; however, if there is a significant extension of cellulitis, oral antibiotics may be prescribed as above.[9]
In chronic paronychia, the patient should be instructed to avoid trauma as to the hands as much as possible. Wearing gloves is advised for manual workers. Treatment in chronic paronychia should point toward fungal etiology. Topical and systemic antifungal agents such as itraconazole and terbinafine are options since the etiological factor in chronic type is mostly Candida species. Other inflammatory diseases of the digits like ingrown nails, psoriasis, etc. should have treatment as well. In difficult to treat chronic paronychia, other causes such as malignancy merit exploration.
Differential Diagnosis
Differential diagnosis of paronychia include:
1- Cellulitis - Cellulitis is a superficial infection and will present as erythema and swelling to the affected portion of the body with no area of fluctuance. Treatment is with oral antibiotics.
2 - Felon - A felon is a subcutaneous infection of the digital pulp space. The area becomes warm, red, tense, and very painful due to the confinement of the infection, creating pressure in the individual compartments created by the septa of the finger pad. These require excision and drainage, usually with a longitudinal incision and blunt dissection to ensure adequate drainage.
3 - Herpetic whitlow - This is a viral infection of the distal finger caused by HSV. Patients usually develop a burning, pruritic sensation before the infection erupts. A physical exam will show vesicles, vesicopustules, along with pain and erythema. It is important to not confuse this with a felon or a paronychia as incision and drainage of herpetic whitlow could result in a secondary bacterial infection and failure to heal.
4- Onychomycosis - This is a fungal infection of the nail that causes whitish-yellowish discoloration. Sometimes difficult to treat and requires oral antibiotics instead of topical.
5- Nail Psoriasis - psoriasis can also affect the fingernails and toenails. It may cause thickening of the nails with areas of pitting, ridges, irregular contour, and even raising of the nail from the nail bed.
6- Squamous cell carcinoma - Squamous cell carcinoma is mainly cancer of the skin but can also affect the nail bed. It is a rare malignant subungual tumor subject to misdiagnosis as chronic paronychia.[1][10]
Prognosis
Paronychia usually has a good prognosis. Acute paronychia usually resolves within a few days and will rarely recur in healthy individuals. Chronic paronychia may persist for several months or longer and may recur in predisposed patients.
Complications
Acute paronychia can cause a severe infection of the hand and may spread to involve underlying tendons, which is why appropriate treatment on initial presentation is essential. This status may require evaluation and treatment by a hand surgeon as it often involves debridement, washout, or amputation, based on the severity of the infection. The major complication of chronic paronychia is nail dystrophy. It is often associated with brittle, distorted nail plates. Nail discoloration is not an uncommon complication of chronic paronychia.[11]
Consultations
A dermatologist can manage paronychia in the majority of cases, but on rare occasions where there is involvement of the deep structure and or the bones, then hand orthopedic consultation may become necessary.
Deterrence and Patient Education
Patients should keep their hands dry and warm. Recommendations include wearing gloves for any contact with water, chemicals, and irritants. Avoid nail-biting, manicuring nail folds, using nail varnish, application of false nails until complete recovery.
Pearls and Other Issues
Manicurist should stop the habit of removing cuticles from fingernails and toenails because it will create a port of entry for a variety of organisms and ultimately leads to colonization. Surgical intervention may be necessary for more severe cases. In patients with frequent recurrences, permanent nail ablation can be beneficial.
Enhancing Healthcare Team Outcomes
Assessment of any patients with a paronychia requires full, detailed history and proper physical examination. The patient history is essential, and it might give a clue for the triggering factors. Appropriate treatment is crucial as this can prevent worsening infections and complications.
Paronychia requires an interprofessional team approach, including physicians, specialists, specialty-trained nurses, and pharmacists, all collaborating across disciplines to achieve optimal patient results. [Level V] In most cases, the clinician (physician, NP, PA) will diagnose and prescribe treatment. Pharmacists can recommend antimicrobial therapy, whether fungal or bacterial and report back to the nurse or clinician if they have any concerns. Pharmacists can also check for drug-drug interactions, and let the nurse or physician know if they are present. Nurses and pharmacists can both verify patient compliance and counsel patients on their medications or the dosing/administration of the same, and report any issues back to the prescribing clinician, who can make changes to the patient's drug regimen based on patient needs.