Continuing Education Activity
Cradle cap, or pityriasis capitis, is a subset of infantile seborrheic dermatitis (ISD). It is a very common, mostly self-limiting, chronic non-inflammatory scaling skin condition that presents between the third week and first couple months of life. The peak incidence is at 3 months of life. The skin manifestations are marked by erythematous plaques with greasy-appearing yellowish scale. Cradle cap's name is analogous to its anatomical location. It can be found in areas dense in sebaceous gland activity, such as the scalp, T line of the face and external ears. Parents should be educated properly on the management and the benign nature of this condition. This activity reviews the evaluation, treatment, and complications of cradle cap and underscores the importance of an interprofessional team approach to its management.
Objectives:
- Summarize the hypothesized etiologies of cradle cap in infants.
- Outline counseling points for parents of an infant presenting with cradle cap.
- Review management strategies for symptomatic care of cradle cap.
- Explain the importance of improving coordination amongst the interprofessional team to enhance care for patients affected by cradle cap.
Introduction
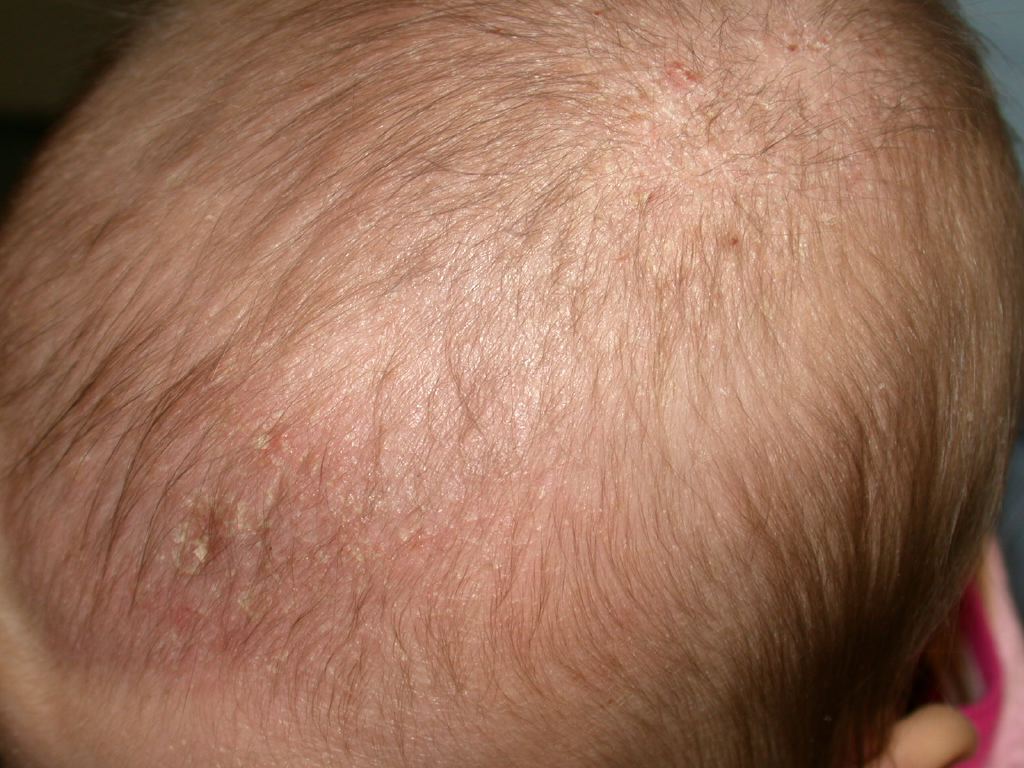
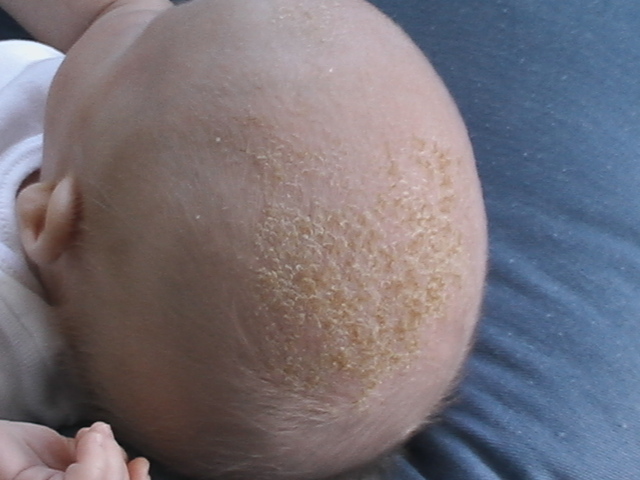
Cradle cap, or pityriasis capitis, is a subset of infantile seborrheic dermatitis (ISD). It is a very common, mostly self-limiting, chronic non-inflammatory scaling skin condition that presents between the third week and first couple months of life. The peak incidence is at 3 months of life.[1] The skin manifestations are marked by erythematous plaques with greasy-appearing yellowish scale. Cradle cap's name is analogous to its anatomical location. It can be found in areas dense in sebaceous gland activity, such as the scalp, T line of the face and external ears. Parents should be educated properly on the management and benign nature of this condition.
Etiology
Currently, there is no known cause for cradle crap. However, there are many factors that have been hypothesized to influence the condition. One hypothesis is the secondary influence of maternal circulating hormones resulting in overactive sebaceous gland activity.[2] Sebaceous glands produce sebum, which is an oil-like substance. Overproduction of sebum causes the dead corneocytes (scale) to remain adherant instead of undergoing normal desquamation. Furthermore, the increase in frequency of seborrheic dermatitis during infancy and adolescence supports a hormonal influence on the condition. Malassezia, a yeast, has been implicated in many cases of cradle cap. The yeast breaks down sebum, consuming the saturated fatty acids, and subsequently leaves the unsaturated fatty acids behind. M. globosa and M. restricta have been found in over 80% of all age cases in an outpatient dermatology setting.[3] The response from anti-fungals further strengthens this causal relationship. However, the yeast is also seen in a large quantity of normal patients, suggesting an independent susceptibility to the yeast.
Epidemiology
Seborrheic dermatitis is common in early infancy with no race predilection observed. The prevalence is 10% for both sexes in the first three months of life. Foley et al. reported a prevalence of 10.4% in boys and 9.5% in girls, suggesting no gender predilection. Furthermore, the condition peaks at three months of age with a prevalence of 70%, then decrease steadily as the infant approaches one year of life. The condition affects about 7% of children between during the second year of life, and most cases are characterized as mild, with a further decrease in prevalence through the fourth year of life. [4]
Pathophysiology
Cradle cap classically presents as greasy, non-inflammatory plaques with overlying yellowish scale, on the vertex and frontal regions of the scalp. Cradle cap is usually asymptomatic; neither painful nor pruritic. Most infants generally have no side effects from the condition with feeding and sleep not being interrupted.[5] Studies have shown that infants with cradle crap commonly have a family member with either atopic dermatitis and/or asthma.[6]
History and Physical
On history, the caregivers will report an asymptomatic, scaly eruption on the scalp, and sometimes face, usually by the thrid year of life, that is resistant to at-home remedies. The patient may have a family member with eczema and/or asthma. On physical exam, notable findings include accumulation of greasy yellow scale on the vertex and forehead of the scalp. The face may also be involved, presenting as erythematous scaly plaques on the forehead, eyebrows/eyelids, nasolabial folds, cheeks, and post-auricular areas. Nonetheless, other areas may be implicated such as the umbilical area, diaper zone, and intertriginous areas. The areas affected away from the scalp tend to have less scale with more erythema. In rare cases, the condition can present as an erythrodermic eruption. In this situation, immunodeficiencies and vitamin deficiencies should be considered by the clinician.
Evaluation
Cradle cap does not require biopsy or laboratory studies.
Treatment / Management
Cradle cap is generally a self-limiting skin condition. Prevention of cradle cap is difficult, secondary to the unknown cause of the condition, yet many believe hormones play a strong role.[3] Moreover, the treatment for mild and localized cradle cap should remain conservative. The infant should be washed daily with a gentle baby shampoo along with an emollient (white petrolatum, mineral oil, baby oil) prior to the shampoo use. The emollient may prove more effective if remaining in contact with the skin for a prolonged period of time, overnight if necessary, to break up the scale. Afterward, there should be the gentle removal of scale with a soft toothbrush or cradle crap comb. The oil will help soften the scale making it easier for removal. Once the scale is removed, parents should continue daily shampooing of their infant's affected areas to prevent recurrence. Cradle cap that does not improve after conservative measures or that is extensive in nature can be treated with an antifungal cream such as ketoconazole 2% or a topical steroid cream such as hydrocortisone 1% for approximately 1-2 weeks. In intertriginous areas, ketoconazole 2% cream is the preferred treatment option. Wannanukul et al. reported no superiority between ketoconazole 2% and hydrocortisone 1% for ISD, suggesting the primary mechanism to be emollient care. Nonetheless, the efficacy between 2% ketoconazole cream and 1% hydrocortisone cream showed no statistical significance in the better treatment option. Selenium sulfide, zinc pyrithione, and salicylic acid are used in adults with seborrheic dermatitis, yet the efficacy and safety are not known in the infant population. Parents should also be educated on the chronicity of this condition during the early infant years and reminded of its self-limiting nature. [7][8]
Differential Diagnosis
A condition commonly confused with cradle crap is atopic dermatitis. Atopic dermatitis presents with moderate to severe pruritus that interferes with sleeping and feeding in the infant, as well as erythematous, scaly and sometimes crusted lesions that are poorly demarcated on the cheek, scalp and extensor surfaces. Impetigo can be confused with cradle cap. However, impetigo starts out as vesicles with a thin, fragile roof. Tinea capitis presents similarly although with possible hair loss, and confirmed with KOH examination and the presence of lymphadenopathy. Diaper dermatitis normally spares the innermost skin folds. Psoriasis is uncommon in this age group, but would present as sharply defined, bright red, silvery scale papules that coalesce into plaques. Lastly, Langerhans cell histiocytosis should be considered in refractory cases of ISD that present with ulceration and erosion along with brownish-red to purpuric nodules in similar areas, ultimately confirmed by biopsy.
Prognosis
Cradle cap is generally self-limiting and benign. Yet, if the condition persists after 12 months of age, alternative diagnoses should be further investigated.
Complications
Bacterial co-infection could be a possible, but rarely seen complication, likely due to repeated scratching if irritated.
Deterrence and Patient Education
It is important to educate the parents on the chronicity and the self-limiting and benign nature of the condition.
Pearls and Other Issues
- Benign condition of the scalp
- If the condition does not improve with management, consider alternate diagnoses.
Enhancing Healthcare Team Outcomes
Education is imperative between the doctor-parent to establish proper management of cradle cap. This is a condition that can be managed conservatively. Therefore, the pediatrician and nurse should make sure the parent understands this, as well as other conservative measures such as the proper shampoo's and frequency to help quicken the resolution of scale.