Continuing Education Activity
Tenosynovitis is an inflammatory condition affecting the tendon sheath has a wide variety of causes and treatment considerations. Infectious forms of tenosynovitis can be rapid and progressive, resulting in damage to the tendon and surrounding structures, and in addition to antibiotics, may require surgical debridement and washout and sometimes necessitate amputation. Treatment of non-infectious tenosynovitis revolves around the underlying etiology but may result in long-term pain and disability if untreated. This activity reviews the evaluation and treatment of tenosynovitis and highlights the role of the interprofessional team in managing patients with this condition.
Objectives:
- Outline the typical presentation of a patient with infectious and non-infectious tenosynovitis.
- Describe the typical imaging findings of tenosynovitis.
- Review the treatment considerations for patients with tenosynovitis.
- Summarize the importance of collaboration and communication amongst the interprofessional team to improve outcomes for patients affected by tenosynovitis.
Introduction
Tenosynovitis is a broad term describing the inflammation of the fluid-filled synovium within the tendon sheath. It commonly manifests as pain, swelling, and contractures, depending on the etiology. The condition can affect any tendon in the body surrounded by a sheath but has a predilection for the hand, wrist, and foot. A basic understanding of the tendon anatomy allows the clinician to appreciate the pathophysiology, treatment, and complications. The tendon anatomy and relationship to the tendon sheath are well illustrated in the hand.
The tendons' intricate arrangement in the hand permits the gripping, grasping, and precise motor function of the hand. Shortly after exiting the carpal tunnel at the wrist, the tendons of flexor digitorium superficialis and profundus muscles cross the palm and enter tunnels formed by the fibrous sheaths on the palmar aspect of each digit. Within each tunnel, the tendons are surrounded by a synovial sheath or bursa. Together, the fibrous tunnel and synovial covering form the tendon sheath.
The tendon sheath has the following functions:
- The synovial fluid nourishes the tendon and provides a low-friction environment, allowing the smooth gliding of the tendon and reducing wear and tear of the tendons from excessive friction.
- The fibrous sheath provides anchor points for the tendon to prevent 'bowstringing.' For example, in the hand, they help anchor the tendons to the bony plane of the phalanges and interphalangeal joints to prevent the tendons from bowing when the digits are flexed.
Etiology
Tenosynovitis can be divided into infective and non-infective causes. Non-infective causes include autoimmune, overuse, and idiopathic.
Autoimmune
There is a strong link between rheumatoid arthritis and tenosynovitis, and up to 87% of rheumatoid arthritis patients have radiological features of tenosynovitis on MRI [1]. Rheumatoid arthritis has a predilection for synovial linings. As the tendon sheath has a sizeable synovial component, there may be an essential role of the tendon sheath in the disease process and the patient's symptoms. This has been shown in an experimental mouse model [2] but has yet to be proven in humans. Psoriatic is also a commonly associated autoimmune condition[3]
Overuse
Frequent repetitive movements can cause inflammation of the synovial sheath; this is often referred to as repetitive strain injury or overuse syndrome. A typical example is the prolonged periods working on a computer that strain the fingers, wrist, and forearm. Any prolonged repetitive movements increase the risk of tendon irritation and, thus, tenosynovitis.
Idiopathic
Tenosynovitis can be idiopathic; these patients have no established cause for their condition.
Infective
Infective tenosynovitis is caused by infective pathogens proliferating within the tendon sheaths. They reach the sheaths either by direct inoculation from injury or can spread from local or distant infections. Common organism found in infective tenosynovitis includes Staphylococcus aureus (40 to 75%) and MRSA (29%), other common skin commensals such as Staphylococcus epidermidis, beta-hemolytic Streptococcus, Pseudomonas aeruginosa, Eikinella in human bites, and Pasturella multocida in animal bites.[4]
Epidemiology
Tenosynovitis remains a common condition, with its incidence, prevalence, and distribution remaining variable depending on the etiology. For the general population taken as a whole, the incidence is between 1.7 to 2.6% for the stenosing form of tenosynovitis.[5] This number is much higher for persons with diabetes mellitus, ranging from 10 to 20%.[6] Of those who develop infections of the hand, only 2.5 to 9.4% of patients will go on to develop infectious tenosynovitis.[7] Individuals with rheumatoid arthritis are significantly at risk of tenosynovitis, with 55% of patients reporting symptoms averaging 3.1 tendons.[8]
Pathophysiology
Regardless of the etiology, the mechanism of tenosynovitis remains similar to the hallmark findings of inflammation within the tendon sheath. Purulence, autoimmune complexes, crystalline deposit, overuse, and other etiologies as above often affect the tendon synovium (the fluid around the tendon) or the tendon itself, resulting in inflammation and thickening.[9] The natural gliding properties of the tendon sheath complex become compromised as a result. While most tendons are at least partially contained by a tendon sheath and are therefore prone to tenosynovitis, some tendons are not contained in a tendon sheath, such as the Achilles tendon. Of important note, infectious tenosynovitis progresses over a series of surgically significant stages. The first stage demonstrates exudative distension of the tendon sheath apparatus; the second stage involves purulent filling, and the third stage 3 results in necrosis and destruction of the sheath, tendon, and adjacent structures.[10]
History and Physical
A detailed history focusing on possible etiologies is essential, as the cause actively directs treatment of tenosynovitis.[11][7][9] A history of injury, fever, ulceration, or purulence with acute digit contracture or pain upon flexion/extension would suggest an infectious etiology, whereas a history of longstanding arthritis or autoimmune disorder with slowly progressing symptoms would suggest a chronic systemic process.
Physical exam findings vary based on cause and extent; however, in general, they demonstrate swelling, pain, erythema, and difficulty moving the affected joint. For infectious flexor tenosynovitis, the “Kanavel signs” are important to recognize:[12]
- Tenderness of the flexor sheath
- Enlargement of the affected tendon in a symmetric pattern
- Baseline contracture of the affected tendon
- Pain with passive straightening of the tendon
These signs are 91 to 97% sensitive for pyogenic flexor tenosynovitis, however, with a reduced specificity of 51 to 69%.[13] Other etiologies of tenosynovitis present with a variety of physical manifestations. In rheumatoid arthritis, rheumatoid nodules or hand deformities may be helpful, while crystalline causes can sometimes be elucidated based on the finding of tophi or evidence of deposition on the exam. Other times, the physical exam may be non-elucidative such as in chronic overuse injury. Progression of tenosynovitis can result in visible contracture deformities and an inability to relax the tendon.
Stenosing tenosynovitis, a phenomenon resulting from enlargement of the flexor tendon relative to the flexor retinaculum pulley (A1 pulley), results in “catching” or “locking” of the joint.[14] In the fingers, this is known as trigger finger, resulting in flexion contractures at the PIP joints.[14] Stenosing tenosynovitis of the extensor pollicis brevis (EBL) and abductor pollicis longus (APL) results in PIP contractures of the thumb, often with a positive Finklestein test (adduction of the hand and wrist together) and is known as de Quervain tenosynovitis.
Evaluation
Laboratory evaluation can help evaluate and differentiate between the causes of tenosynovitis. However, it is not always necessary. When suspecting infectious causes of tenosynovitis, findings of elevated WBC, bacteremia, and culture may be helpful. Autoinflammatory diseases may demonstrate specific markers to assist in the diagnosis. Microscopic evaluation can further help in distinguishing crystalline pathology from infection or inflammation when suspected.[15]
Imaging evaluation is helpful yet not always necessary when diagnosing tenosynovitis. Plain film radiographs often show calcifications of the synovial membrane or, at times, periosteal reaction, suggesting inflammation; however, they may be negative altogether. Computed tomography can be useful for detecting bony abnormalities such as bony erosions or structural anomalies, but its soft tissue sensitivity for synovitis and tenosynovitis remains low.[16]
Ultrasound can often add diagnostic benefits, particularly in the hands where it can show echotexture changes in 15% of tendons and blurring of the tendon margins in 62%.[17] Additionally, tendon thickening could be visible in 44% of fingers, with an additional 6% demonstrating sheath cysts and 4% with further abnormalities of the metacarpophalangeal joints.[17]
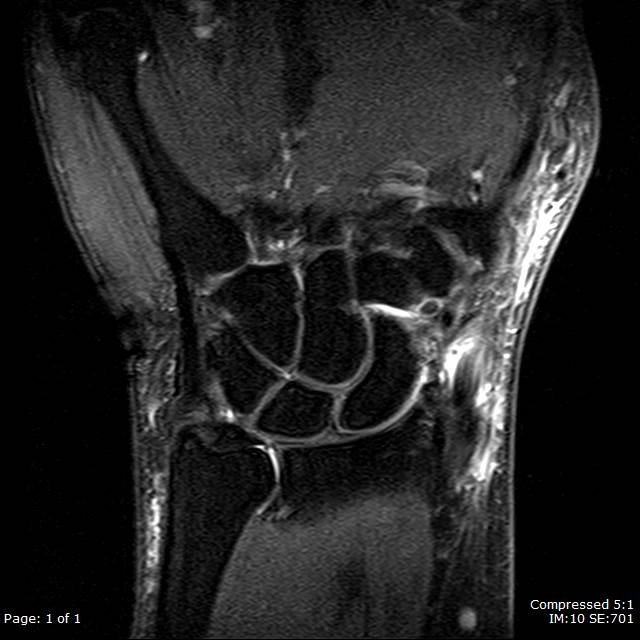
When ultrasound is limited or additional fine detail evaluation is required, further evaluation with MRI is an option. Contrast should be a consideration in cases concerning for infectious etiologies for abscess visualization. MRI features of tenosynovitis can vary based on etiology; however, they commonly demonstrate peritendinous edema and increased thickening of the extensor brevis longus (EBL) and abductor pollicis longus (APL) tendons in cases of de Quervain tenosynovitis.[18] In rheumatoid arthritis, bone marrow signal may increase even before symptoms of tenosynovitis.[16] Fluid collections demonstrating enhancement are suspicious for abscess formation.
Treatment / Management
Infectious tenosynovitis treatment can vary based on the offending agent when known; however, when empiric treatment is necessary, broad-spectrum antibiotics such as vancomycin at 15 to 20 mg/kg/dose every 8 to 12 hours with a third-generation cephalosporin at 1 to 2 g IV every 24 hours are considered and may improve outcomes.[7] Duration depends on clinical findings and the presence or absence of bacteremia, as well as the source of the infection. Sheath irrigation is a possibility in patients with stage 1 infection, with catheter-directed therapy resulting in improved outcomes compared to open irrigation.[7] Patients with stage 2 or 3 infections will likely require debridement.[18][19]
Noninfectious causes of tenosynovitis vary in their treatment based on etiology; however, many are treated conservatively with non-steroidal anti-inflammatory drugs such as naproxen.[20] Additional first-line treatment may consist of activity modification, splinting, and glucocorticoid injections.[20][21][22] Disease-modifying antirheumatic drugs (DMARDs) such as glucocorticoids may be additionally helpful in patients in patients who fail a trial of NSAIDs.[23] Surgical intervention may become necessary after 3 to 6 months of progression despite conservative therapy.[20] Surgical intervention may involve the decompression of affected tendons as well as debridement of inflammatory tissues.[20][24]
Differential Diagnosis
A variety of diseases may mimic or contribute to tenosynovitis; common examples appear below.
- Cellulitis/soft tissue infection may mimic symptoms of tenosynovitis, resulting in difficulty moving the affected joint from edema and pain.
- Joint-related diseases such as osteoarthritis, rheumatoid arthritis, pseudogout, psoriatic arthritis, and gout
- Recent or old trauma, including osseous or tendinous pathology, can often present similar to stenosing tenosynovitis.
- Dupuytren contractures can also appear as a case of stenosing tenosynovitis and are secondary to nodularity of the fascia causing chronic locking of the digits.
Prognosis
In cases of infectious tenosynovitis, the best outcomes are related to early empiric antimicrobial therapy and early irrigation or debridement when necessary.[7] Poor prognostic factors of infectious tenosynovitis include infection by Streptococcus pyogenes or multiple agents, delayed antibiotics and surgical intervention, purulence of the tissue, diabetes mellitus, renal failure, and peripheral vascular disease.[19][12] Stage 3 disease involving necrosis and destruction offers the worst outcomes, with a 59% amputation rate.[7]
The prognosis for non-infectious tenosynovitis is highly variable dependent on the etiology. However, those suffering from the stenosing form have a relatively good prognosis, with 93% finding improvement in finger-based symptoms within 6 to 10 weeks of wearing a thermoplastic splint, 54% with complete resolution.[21] Those who fail more conservative therapy and require glucocorticoids can expect persistent relief greater than one year in about 50% of patients.[22] Surgical patients also experience a good prognosis with recurrence of symptoms in only 4.6% of patients.[25] Patients with diabetes mellitus are a special group that does not respond as well to either corticosteroid or surgical therapy.[26]
Complications
The rate of complications for infectious/pyogenic tenosynovitis is high at 38% and includes long-term finger stiffness, boney/tendinous deformation, further infection into the deep spaces of the hand, necrosis of the tendon, adhesions, and eventual need for amputation.[7]
Patients suffering from the non-infectious form of tenosynovitis may progress into the stenosing form of tenosynovitis resulting in chronic contractures and flexion deformities requiring surgery. Treatment of non-infectious tenosynovitis carries additional complications, especially in those requiring surgery, such as infection, injury of the nerve, deformities of the flexor tendon, and scarring of the tissue.[27]
Deterrence and Patient Education
Avoidance of situations that increase the risk of infection to the hands is vital in preventing infectious tenosynovitis. Early detection of infectious signs such as tenderness, pain, contracture, and enlargement of a digit by the patient is important in determining good outcomes.[7] Patients suffering from non-infectious tenosynovitis should identify and avoid activities that worsen symptoms and take preventative care by addressing a systemic disease that may influence tenosynovitis.
Pearls and Other Issues
- Early recognition of infectious tenosynovitis by history and physical with prompt therapy, including empiric antibiotic therapy and possible surgery, is critical in preventing serious complications.
- Ultrasound is a valuable imaging tool when radiographs are unhelpful. Further characterization with MRI is preferable to CT.
- Conservative therapy with NSAIDs and splinting is the first line for non-infectious tenosynovitis and is often highly effective. Further treatment with steroid injections, DMARDs, and surgery may be warranted.
- Non-infectious tenosynovitis has many causes which may necessitate different treatment modalities. A detailed history and physical in conjunction with patient-directed laboratory and imaging studies can impact management dramatically.
Enhancing Healthcare Team Outcomes
Refractory non-infectious tenosynovitis and any form of infectious tenosynovitis may warrant consultation of an orthopedic surgeon for further evaluation and treatment, including surgery. The consultation of an infectious disease specialist may also be beneficial in patients suffering from infectious tenosynovitis where narrowing or broadening of antibiotic coverage and determining the length of treatment is necessary; this can include a consult with a board-certified infectious disease pharmacist. Rheumatology may be able to further assist in the causes and treatment of the non-infectious etiologies of tenosynovitis. The inclusion of radiology in the assessment of the tenosynovitis can additionally support the interprofessional team by providing the imaging findings and their associated interpretations. Orthopedic nursing staff can serve as a coordination point for all these various disciplines, ensuring all providers are informed and on the same page.
In summary, tenosynovitis requires an interprofessional team approach, including physicians, specialists, specialty-trained nurses, and pharmacists, all collaborating across disciplines to achieve optimal patient results. [Level 5]