Continuing Education Activity
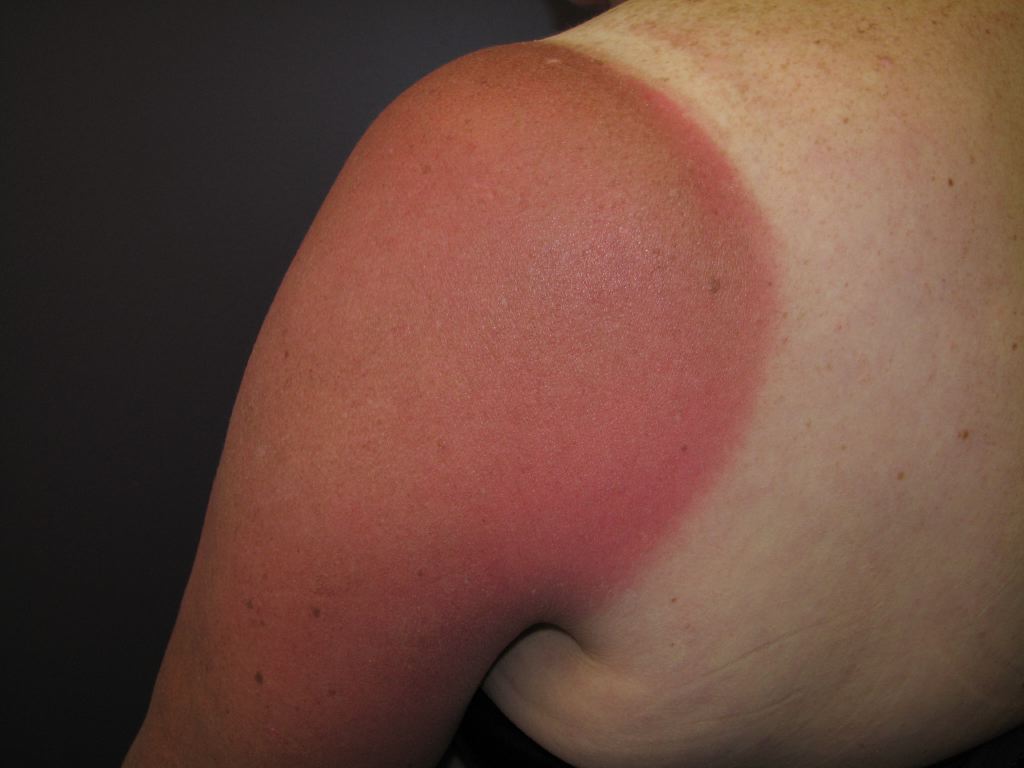
Sunburn is an acute inflammatory skin reaction occurring due to extended exposure to ultraviolet (UV) rays from the sun or artificial sources such as tanning beds. Sunburns can be quite painful, and in most cases, conservative treatment is all that is necessary. However, seeking hospital evaluation and treatment may be necessary in severe cases. Every year, over a third of the population experiences sunburn, which can have lasting consequences. The severity of sunburn depends primarily on the duration and intensity of exposure to UV rays. Overall, the number of sunburns experienced in individuals correlates with an increased risk of skin cancer. Therefore, it is crucial to educate individuals, particularly those in high-risk groups, about preventive measures for sunburn. This activity reviews the etiology, pathophysiology, and risk factors of sunburns, emphasizing the role of the interprofessional team in preventing and managing this condition.
Objectives:
Identify the signs, degrees, and potential complications of sunburn in patients during physical examinations.
Implement evidence-based sunburn prevention measures, including counseling on sun safety measures and sunscreen use.
Apply appropriate first-aid measures for sunburn management, including topical treatments, fluid replacement, and analgesia.
Collaborate with other healthcare professionals to provide comprehensive sunburn prevention and management, especially for patients with a history of sunburn or skin cancer risk factors.
Introduction
Sunburn is an acute inflammatory skin reaction occurring due to extended exposure to ultraviolet (UV) rays from the sun or artificial sources such as tanning beds. The intensity and duration of UV exposure, along with factors such as medication usage, time of day, ozone depletion, high altitude, clear skies, and skin phototype, primarily influence the risk of sunburn. To decrease the risk of skin cancer and enhance the quality of life, patients should be aware of the causes, treatments, and prevention methods for sunburn. They should adopt measures to prevent sunburn as repeated sunburns increase the risk of skin cancer and can cause visible signs of aging due to solar damage, thereby leading to worse cosmetic results. This activity covers the pathophysiology, management, and prevention of sunburn, aiming to reduce the risk of skin cancer and lower patient morbidity and mortality.
Etiology
Sunburn occurs when the skin is exposed to prolonged UV radiation from the sun or artificial sources.[1] The severity of sunburn can vary depending on several factors, some of which are mentioned below.
Medications
The risk of sunburn is elevated by the usage of certain medications, including thiazide diuretics, sulfonamides, fluoroquinolones, nonsteroidal anti-inflammatory drugs (NSAIDs), retinoids, tetracyclines antibiotics such as doxycycline, and St John's wort, among other photosensitizing medications.[2]
Increased UV Index
Understanding environmental factors contributing to sunburn risk is crucial for adequate sun protection and prevention. Here are some key considerations:
- The sun's rays are strongest between 10 AM and 4 PM.
- Reduced cloud coverage leads to greater exposure to intense UV rays.
- Higher altitudes correlate with an elevated risk of sunburn due to a thinner layer of the Earth's atmospheric protection.
- Closer proximity to the equator results in more direct exposure to UV rays.
Ozone Depletion
In some areas of the world, the ozone layer is depleted, resulting in ozone holes that allow for increased penetration of the sun's UV rays on the Earth.
Fitzpatrick Skin Phototype
Individuals with lighter skin tones are more prone to experiencing sunburns. In 1975, a physician named Thomas Fitzpatrick developed the Fitzpatrick skin phototypes classification system, as provided below, to categorize different skin complexions and their reactions to UV radiation.[3][4]
- Type I: Pale white skin that burns easily and does not tan.
- Type II: White skin that burns easily and tans with difficulty.
- Type III: White skin that may burn but tans easily.
- Type IV: Light brown or olive skin that hardly burns and tans easily.
- Type V: Brown skin that usually does not burn and tans easily.
- Type VI: Black skin that is very unlikely to burn and becomes darker with UV radiation exposure.
Individuals with Fitzpatrick skin phototypes I to III are more prone to sunburn because their skin contains less melanin pigment, which is crucial in shielding against UV radiation.
Individuals with lower Fitzpatrick skin phototypes also exhibit a lower minimal erythema dose, which denotes the minimum amount of UV radiation that results in non-diseased skin turning red within 24 hours of UV exposure.[5][6] However, skin classification is a multifactorial and subjective process, especially if self-reported. For instance, studies have demonstrated that individuals categorized as type IV and V according to the defined criteria may exhibit skin characteristics that fall within the range of type I through IV criteria.[3] The Fitzpatrick skin phototypes classification system was initially developed for individuals with white skin to determine the dose of UV light required during phototherapy. Ongoing research further highlights that the Fitzpatrick scale may not be the most suitable assessment tool for evaluating skin complexion in individuals with darker skin tones.[7][8]
Tanning
Basking in the sun for extended periods to attain a tanned appearance has been popular for years. However, this habit can heighten the risk of skin cancers and accelerate skin aging. Moreover, excessive tanning can lead to painful sunburn.
Inadequate Preventative Measures
Inadequate sun protection can result from not applying sunscreen frequently enough, using sunscreen with a low sun protection factor (SPF), and not wearing protective clothing in the sun.
Epidemiology
A study conducted on a representative sample of 31,162 adults from the 2015 National Health Interview Survey revealed that 34% of the participants had encountered at least one sunburn during that year. Individuals with Fitzpatrick skin types I to III with lighter skin tones, those aged 18 to 29, and non-Hispanic White individuals exhibited a higher likelihood of experiencing sunburn. Furthermore, using tanning lotions, engaging in physical activity, binge drinking, and being overweight increased the likelihood of sunburn.[9] Frequent outdoor activities on vacation can increase a patient's annual UV radiation exposure by 30% to 50%.[9]
Although sunburn can affect individuals of all skin types, people residing in Australia and New Zealand annually report the highest incidence of melanoma, often attributable to preventable sunburns.[9] Among studies involving individuals of Black African or Black Caribbean heritage residing in the United Kingdom, 50% reported a history of sunburn at some point in their lives. The prevalence of sunburn within 1 year was 13% in Black Americans and 30% in Hispanic Americans.[9]
Pathophysiology
Exposure to UVA rays, between 320 and 400 nm wavelengths, and UVB rays, between 295 and 320 nm wavelengths, can cause sunburn and DNA damage. UVA rays cause oxidative DNA damage, whereas UVB rays are absorbed directly by DNA and induce the formation of thymine-thymine cyclobutane dimers.[10][11][12] These dimers trigger the body to initiate a DNA repair response, which includes inducing cell apoptosis and releasing inflammatory markers such as prostaglandins, reactive oxygen species, and bradykinin.[13] As a result, this leads to vasodilation, edema, and pain, which manifest as the characteristic red and painful skin associated with sunburn. Furthermore, UVB ray exposure to the skin can elevate chemokines, such as C-X-C motif chemokine 5 (CXCL5), and activate peripheral nociceptors, ultimately resulting in overactivation of the skin's pain receptors.[14][15]
Histopathology
Prolonged exposure to the sun can cause sunburn, which significantly impacts all layers of the skin, with the epidermis and dermis being particularly affected. Examination of sunburned skin cells reveals the loss of Langerhans cells and the vacuolation of keratinocytes. Moreover, the dermis exhibits vascular changes, including the enlargement of endothelial cells and edema caused by mast cell degranulation—a process that initiates within 30 minutes of radiation exposure. Histamine and prostaglandin E2 levels increase 4-fold after UV radiation exposure, signifying the role of histamine in the skin's sunburn reaction. However, these changes are reversed after 24 hours.[16]
History and Physical
Sunburn primarily occurs due to excessive sun exposure without proper sun protection. Many patients acknowledge forgetting to use sunscreen, not applying it regularly enough, underestimating their sun exposure duration, or neglecting to wear protective clothing. A physical examination will unveil varying degrees of erythema and edema, contingent upon the extent of sun exposure severity.
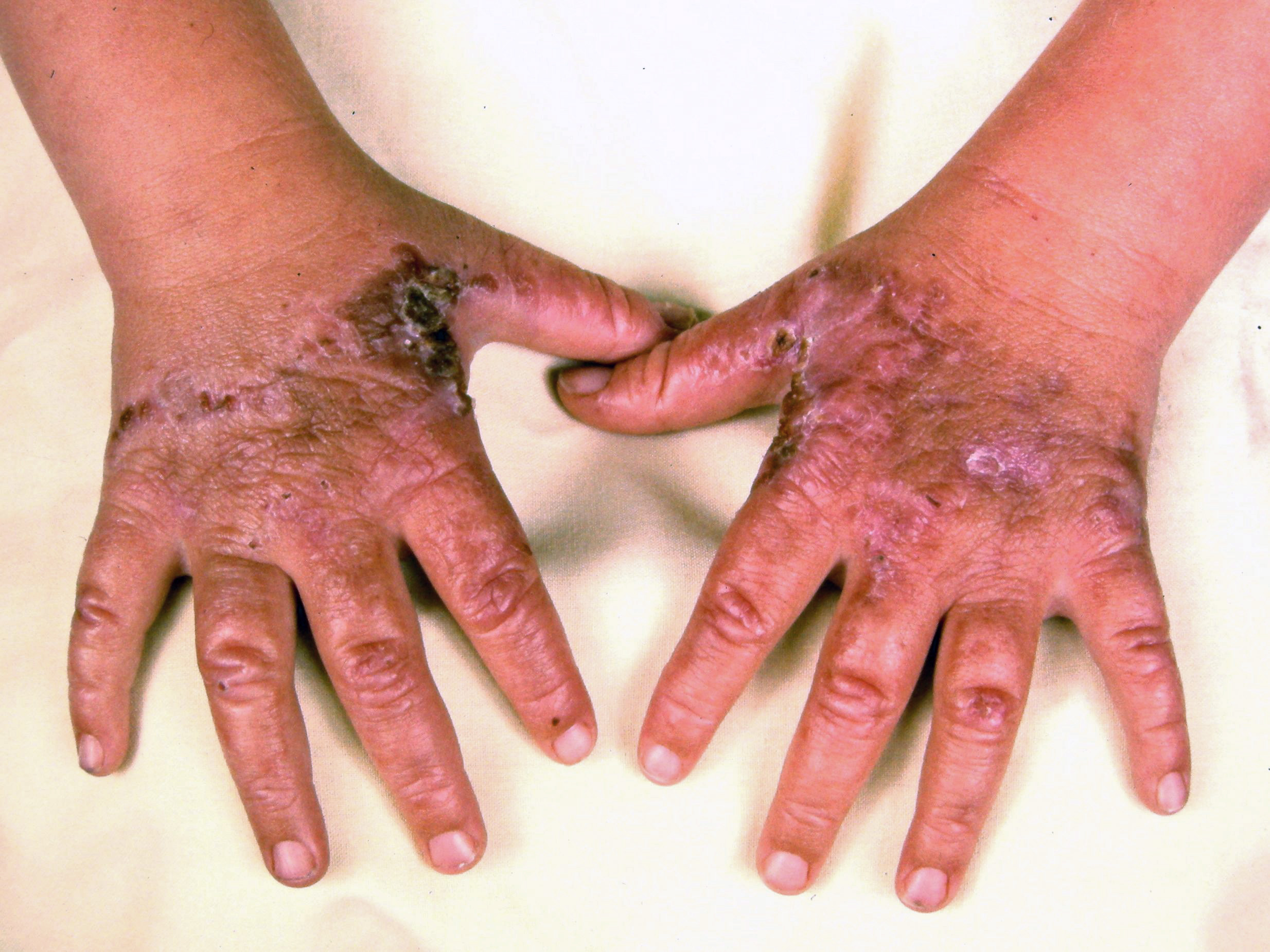
The sun's rays may leave certain areas of the skin undamaged if they are covered by clothing. However, blisters may suggest a more severe, partial-thickness burn requiring additional care. The affected sunburned skin may feel warm and painful to the touch, and, in severe cases, sunburn can cause systemic symptoms such as nausea, fever, and chills.
Erythema usually develops within 3 to 5 hours of sun exposure, reaching its peak within 12 to 24 hours. Erythema typically subsides in 3 to 7 days, whereas blisters should heal within 7 to 10 days. Skin peeling may continue for 7 to 10 days after sun exposure. Individuals with fair skin may develop solar lentigines, pale brown macules that remain after their symptoms have resolved.
Evaluation
A sunburn can be diagnosed through clinical examination alone and does not necessitate additional laboratory or radiographic testing.
Treatment / Management
Most sunburns can heal without requiring further medical intervention. Some practical ways to manage symptoms of sunburn at home are listed below.
- Individuals should avoid exposing the affected area to the sun to prevent further skin damage. In addition, it is advisable always to use sunscreen and wear sun-protective clothing.
- Individuals should consider taking over-the-counter NSAIDs to reduce pain.
- Individuals should stay hydrated by drinking plenty of water.
- Individuals should apply cool compresses, aloe vera gel, or lotion to moisten the skin and alleviate pain, and avoid local anesthetic creams.
- Individuals can soothe their skin with cool colloidal oatmeal baths or calamine lotion.
- Individuals should avoid using topical and oral corticosteroids because they do not offer benefits in treating sunburns.
- Individuals should wash the blisters with soap and water and cover them with moist gauze if they rupture. However, intact blisters should not be unroofed.
People suffering from severe sunburns that result in extensive blistering may risk losing fluids and electrolytes. In such cases, resuscitation with a crystalloid solution may be necessary if the total body surface area (TBSA) exceeds 20% in adults. The formula for resuscitation may differ depending on the healthcare facility. A burn center may be the most appropriate location for sunburn treatment.
The 2 standard formulas for fluid resuscitation in burn patients are listed below.
- Parkland formula: 4 mL x %TBSA x weight (in kg)
- Modified Brooke formula: 2 mL x %TBSA x weight (in kg)
Both formulas recommend administering half of the calculated crystalloid solution within the first 8 hours after the injury, with the remaining half given over the subsequent 16 hours. Notably, the resuscitation process should commence immediately after the injury, regardless of when the patient arrives at the emergency department.
Preventing sunburn is the cornerstone of effective sunburn management. A genetic predisposition to a higher risk of sunburn serves as a genetic marker for an elevated risk of developing skin cancer. Patients should receive counseling on sun avoidance, wearing protective clothing, using broad-spectrum sunscreen, and avoiding direct sunlight between 10 AM and 4 PM during the summertime. Individuals should apply sunscreen with an SPF of 30 or more 15 to 30 minutes before sun exposure and reapply it at least every 2 hours. Parents or caregivers should avoid exposing infants younger than 6 months to direct sunlight and use protective clothing and umbrellas for added sun protection. When inadequate shade or protection is available, the American Academy of Pediatrics recommends that parents or caregivers apply a small amount of sunscreen to infants' hands, faces, and heads. Individuals should be aware that using tanning beds with only UVA light is not safer than tanning outside in the sun.
Differential Diagnosis
The differential diagnosis for sunburn includes:
- Autoimmune diseases, such as systemic lupus erythematosus and dermatomyositis.
- Infections, including staphylococcal scalded skin syndrome, cellulitis, and erysipelas.
- Idiopathic conditions, such as pityriasis rubra pilaris.
- Malignancies, such as Sézary syndrome, cutaneous lymphomas, or a cutaneous manifestation of an internal malignancy.
- Common dermatological diseases, including rosacea, acne, stasis dermatitis, and seborrheic dermatitis.
- Solar reactions, including solar urticaria, phytophotodermatitis, photoallergic type IV sensitivity reactions, and phototoxic reactions.
- Congenital conditions, such as xeroderma pigmentosum and erythropoietic protoporphyria.
Prognosis
Sunburn can generally be managed at home with conservative treatment, leading to a positive outlook.
Complications
Sunburns might appear inconsequential, but closely monitoring them during the acute period is essential. Although a sunburn initially affects only the epidermis layer of the skin, it can potentially advance into a deeper burn, necessitating prompt medical attention or evaluation at a certified burn center. Certain patients may necessitate hospital admission for fluid replacement and parenteral analgesia. UV exposure accelerates premature aging and heightens the risk of skin cancer. Although cumulative lifetime UV exposure is associated with both melanoma and non-melanoma skin cancers, it is noteworthy that melanoma shows a stronger link to short, intense exposures and sunburns than other skin cancers.
Deterrence and Patient Education
The number of skin cancer cases, including melanoma, rises annually by 3% to 8%. Chronic occupational exposure and occasional recreational sun exposure pose risks to individuals.[17] Skin cancer can arise from sunburns at any age. Numerous campaigns worldwide strive toward promoting proper sun protection to prevent adverse consequences of sunburns and minimize the risk of developing melanoma and other skin cancers.
Applying sunscreen consistently and appropriately with a higher SPF, wearing sun-protective clothing, and seeking shade can protect against sunburns and the associated skin damage. Although recent studies indicate that people in the United States are becoming increasingly aware of the significance of sun protection, tourist areas consistently report a higher incidence of sunburns. Therefore, there is a need to initiate more prevention campaigns to raise awareness about sunburn prevention.[18][17]
The American Academy of Dermatology suggests utilizing water-resistant, broad-spectrum sunscreens that protect against both UVA and UVB rays, featuring an SPF greater than 30. Some essential recommendations for effective sun protection and minimizing the risk of sunburn are as follows:
- Finding shade during the peak sun hours of 10 AM to 4 PM.
- Wearing sun-protective clothing when outdoors.
- Avoiding artificial sources of UV rays, such as tanning beds.
- Exercising extra caution in sun-reflective environments such as snow, water, and sand.[19]
Pearls and Other Issues
Preventing skin cancer begins with protecting the skin from sunburns and UV radiation exposure. Individuals can proactively protect their health and well-being by remaining vigilant regarding these factors.[20]
Individuals can easily protect themselves from sunburn by following the below-mentioned simple steps in their daily lives.
- Individuals should apply a broad-spectrum sunscreen with at least SPF 30, waiting 15 to 30 minutes for it to absorb into the skin, before going outside.
- Individuals should remember to reapply sunscreen every 2 hours and after vigorous activity.
- Individuals should choose water-resistant sunscreen for water activities.
- Individuals can also rely on sun-protective clothing for an additional layer of protection.
- Individuals should avoid direct exposure to the sun between 10 AM and 4 PM to prevent sunburns caused by exposure to UV rays.
Despite the education available, many individuals still seek sunburn treatment at their local emergency departments. Research indicates that this occurrence is most prevalent among younger men and women in the Southern United States region during the spring and summer seasons. Estimates indicate that emergency room visits due to sunburns in the United States exceed 11 million dollars annually.[21]
Enhancing Healthcare Team Outcomes
Although sunburns may seem harmless and can heal without medical intervention, they increase healthcare spending through emergency room visits and raise morbidity and mortality rates by elevating the risk of skin cancer. Healthcare professionals in all specialties play a role in educating patients on proper sun protection. In local pharmacies, pharmacists can offer proper resources and guidance on sunscreens and over-the-counter remedies. Primary care and dermatology clinicians are critical in ensuring patients receive adequate skin screening examinations and counseling on sun safety, as well as educating them about abnormalities to look for on their skin.
All healthcare professionals should be aware of the risks associated with excessive sun exposure and sunburns and counsel patients accordingly by providing evidence of excessive sun exposure. Any healthcare provider who identifies a concerning skin lesion on a patient should promptly inform the patient and arrange an appropriate referral to a primary care or dermatology clinician. Patients who have experienced multiple blistering sunburns should consider scheduling yearly skin examinations with a dermatologist, particularly if they have a history of skin cancer.