Continuing Education Activity
Lyme disease is an infectious disease caused by Borrelia burgdorferi, which is spread by ticks. Lyme disease is divided into three stages: early localized, early disseminated, and late. This activity illustrates the evaluation and management of Lyme disease and reviews the role of the interprofessional team in caring for patients with this condition.
Objectives:
Apply knowledge of the pathophysiology of Lyme disease to the evaluation.
Identify the appearance of the characteristic erythema migrans rash during the physical exam.
Implement evidence-based treatment strategies for the management of Lyme disease.
Develop a well-coordinated interprofessional team approach to provide effective care for patients with Lyme disease.
Introduction
Lyme disease, or Lyme borreliosis, is the most commonly transmitted tick-borne infection in the United States and among the most frequently diagnosed tick-borne infections worldwide. Lyme disease is divided into 3 stages: early localized, early disseminated, and late. The early localized disease is distinguished by the red ring-like expanding rash of Erythema migrans at the site of a recent tick bite. Other symptoms experienced at this stage may be flu-like symptoms, malaise, headache, fever, myalgia, and arthralgia. Most patients only experience the symptoms of early, localized disease. About 20% of patients develop the early disseminated disease, with the most common symptoms being multiple erythema migrans lesions. Other symptoms of the disseminated stage are flu-like symptoms, lymphadenopathy, arthralgia, myalgia, palsies of the cranial nerves (especially CN-VII), ophthalmic conditions, and lymphocytic meningitis. Additionally, cardiac manifestations such as conduction abnormalities, myocarditis, or pericarditis may occur. The most common manifestation of the late disease is arthritis which is usually pauciarticular and affects large joints, especially the knees.[1][2]
The diagnosis is not always easy, as many patients cannot recall a tick bite. However, in endemic areas, patients who have the typical rash can be started on treatment without waiting for serology.
Etiology
In the United States, Lyme disease is caused by the bacterial spirochete Borrelia burgdorferi and is transmitted by the bite of an Ixodes genus tick, most commonly Ixodes scapularis. In Eurasia, the predominant causes are Borrelia burgdorferi, Borrelia afzelii, and Borrelia garinii.[3][4]
B burgdoferi has a particular affinity for the joint. B garinii is exclusively found in Europe and has selectivity for causing white matter encephalitis. B afzelli has an affinity for the skin and is found at the site of the infection. Several Ixodes subspecies transmit Borrelia.
Epidemiology
Lyme disease is most commonly reported in the Northeastern and upper Midwestern United States. The primary states with endemic Lyme disease are Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. Sporadic cases have been reported in northern California, Oregon, and Washington.[5][6]
In states where Lyme disease is common, the incidence is about 40 per 100,000 people. The infection occurs during late spring, summer, and early fall.
For some unknown reason, Lyme disease is commonly reported in Caucasians but can infect all races. Perhaps the skin lesion may not always be obvious in dark-skinned individuals. Lyme disease affects people of all ages but appears slightly more common in females.
Pathophysiology
The most common and first presenting sign of Lyme disease is the erythema migrans rash, which is found in 70% to 80% of cases and appears at the site of the tick bite as an expanding, erythematous skin lesion, measuring 5 cm in diameter or larger. The lesion may present as homogeneous erythema or display a targetoid appearance. The rash appears 1 to 2 weeks after the initial tick bite. If untreated, disease progression may lead to other relatively common findings, including early arthritis in up to 30% in some series; neurologic manifestations, 10% to 15%; or cardiac involvement, 1% to 2%.[7]
Histopathology
Erythema migrans histologic findings are nonspecific, usually showing a perivascular cellular infiltrate which consists of histiocytes, lymphocytes, and plasma cells. Rarely mast cells and neutrophils are identified. A biopsy may show eosinophilic infiltrates, which consist of a local reaction to the bite. Spirochetes may be identified using antibody-labeled or silver stains. Usually, a paucity of spirochetes is found in the tissues of those infected with Lyme disease.
Acrodermatitis Chronica Atrophicans
In acrodermatitis chronica atrophicans, an early biopsy may show a lymphocytic dermal infiltrate, often perivascular in location, with some vascular lymphedema and telangiectasia. Plasma cells may be seen in the cellular infiltrate. Late lesions may demonstrate epidermal thinning with loss of skin appendages. In the later stages, plasma cells may be the only feature distinguishing morphea from acrodermatitis chronic atrophicans.
Fibrotic nodules may show fibrosis of the deeper dermis and hyalinization of collagen bundles. B burgdorferi can sometimes be cultivated from the lesions.
Borrelial Lymphocytoma
Histologic examination is performed in patients with suspected Borrelia lymphocytoma when the history is unclear enough to support a diagnosis. Borrelia lymphocytoma biopsy shows a dense dermal lymphocytic infiltrate with lymphoid follicles and pseudoterminal centers. Lymphocytes with both B- and T-cell markers, occasional macrophages, plasma cells, and eosinophils are seen.
History and Physical
Localized Lyme disease is characterized by erythema migrans occurring 1 to 2 weeks after tick exposure in an endemic area. The differential diagnosis for early Lyme disease with erythema migrans includes other skin conditions such as tinea and nummular eczema. Patients may develop early disseminated or late disease manifestations if not treated in the localized stage. Early neurologic Lyme disease manifestations include facial nerve (CN-VII) palsy, lymphocytic meningitis, or radiculopathy. Cardiac involvement includes myopericarditis and typically presents with heart block. Lyme arthritis is mono- or pauciarticular, generally involving large joints, most commonly the knee, and occurring months removed from the initial tick bite.
Because the symptoms are not specific, one should consider other infections transmitted by ticks, like coinfection with Babesia microti and Ehrlichia. Coinfection has been reported in about 10% of patients.
Like syphilis, Lyme disease is classified into 3 stages: localized, disseminated, and persistent. The first 2 stages are part of early infection, and the third stage is of persistent or chronic disease. Stage 3 usually occurs within 12 months of the infection.
Stage 1: Early localized disease that may present with erythema migrans and low-grade fever. This stage usually occurs within 1 to 28 days following the tick bite.
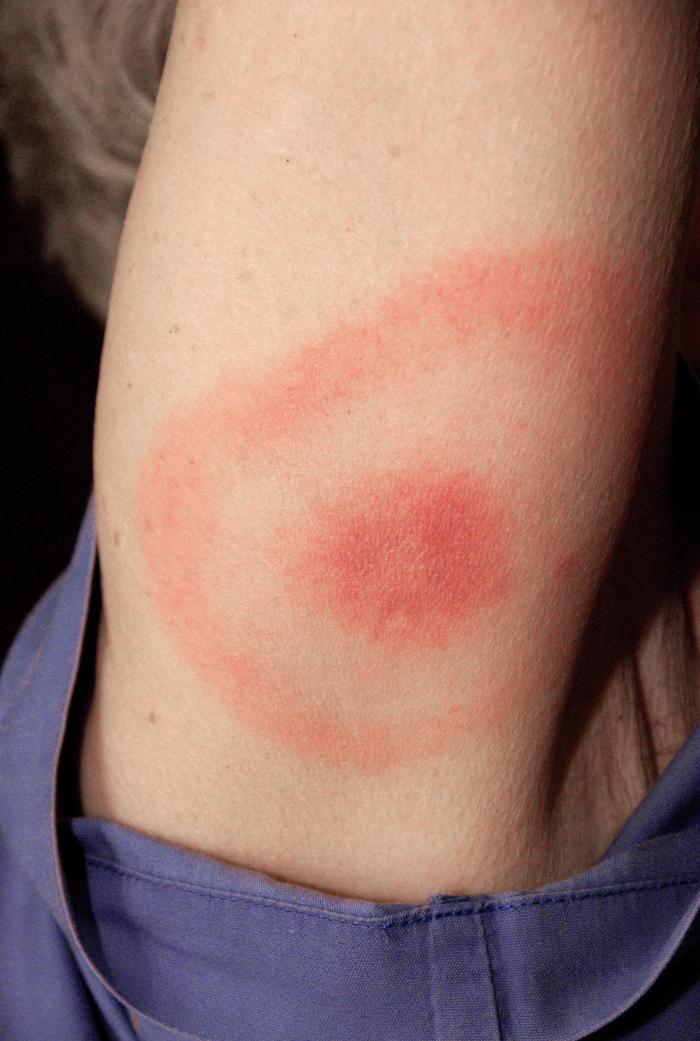
The classic rash is seen in 70% of patients and may develop between 5 to 7 days following the tick bite. The uniform rash usually occurs at the site of the tick bite and may burn, itch, or be asymptomatic. The rash tends to expand for a few days, and concentric rings may be visible (see Image. Lyme Disease "Bulls-Eye" Rash). If left untreated, the rash persists for 2 to 3 weeks. About 20% may have recurrent episodes of the rash, and multiple lesions are not uncommon. At the same time, flu-like symptoms may be present. The low-grade fever may be associated with myalgia, neck stiffness, and headache. Visual problems include eye redness and tearing. About 30% of patients with the rash have no further progression of symptoms.
Stage 2: Usually develops 3 to 12 weeks after the initial infection. Features may include general malaise, fever, neurological features (dizziness, headache), muscle pain, and cardiac symptoms (chest pain, palpitations, and dyspnea). Cranial neuropathy may present as diplopia. Eye pain and keratitis have also been reported. The knee, ankle, and wrist joints are often involved. These symptoms may last 12 to 20 weeks, but recurrence is rare. When a single joint is involved, it may be mistaken for septic arthritis. About 20% of patients have CNS involvement, including encephalopathy, meningitis, and cranial nerve neuropathy. Bell palsy is seen in about 5% of patients. When meningeal symptoms are present, lumbar puncture is warranted to rule out other causes. Encephalopathy presents with deficits in concentration, cognition, memory loss, and personality changes. Extreme irritability and depression are also common.
Borrelia lymphocytoma is a rare presentation of early Lyme disease reported in Europe. It presents as a nodular red-bluish swelling that usually occurs on the ear lobe or areola of the nipple. The lesions can be painful to touch.
Stage 3: Late Lyme disease may occur months or years after the initial infection. The typical features include neurological and rheumatological involvement. Many patients may not have a history of erythema migrans. However, these individuals may present with aseptic meningitis, Bell palsy, arthritis, or dysesthesias. Cognitive deficits are common. The key feature of late-stage Lyme is arthritis which tends to affect the knee. the neurological and psychiatric symptoms mimic fibromyalgia. Radicular pain is common. Borrelia encephalomyelitis is rare and can present with ataxia, seizures, hemiparesis, autonomic dysfunction, and hearing loss. Acrodermatitis chronica atrophicans is typically seen in older women and tends to occur on the dorsum of the hands and feet.
Cardiac involvement may present with arrhythmias or transient heart block. Conduction abnormalities are not uncommon, but most cases are isolated and rarely last more than a few days. Rarely does a patient require permanent pacing
Evaluation
In endemic areas with features of the classic rash and recent tick exposure, treatment can be started without waiting for blood work. However, the symptoms are vague in most patients, and testing is needed. Others may not recall a tick bite or develop the rash.
Serologic testing is insensitive during the first few weeks of infection, and patients presenting with erythema migrans rash and a history of residing in or traveling to an endemic region may be treated based on clinical findings. In later stages of the disease, a 2-step approach is recommended for the serologic diagnosis of Lyme disease. The first step is to perform a quantitative screening test for serum antibodies to B burgdorferi using a sensitive enzyme immunoassay (EIA) or immunofluorescent antibody assay (IFA). A Western blot should follow specimens with positive or equivocal results. Serologic diagnosis is sensitive (greater than 80%) for patients with neurologic or cardiac manifestations.[8][9][10]
Sequential serological testing is not recommended in the acute state because antibody titers often remain elevated for a long time. Testing the tick is not recommended either. And biopsy of the skin is rarely done.
Other blood work may reveal elevated ESR, leukopenia, and thrombocytopenia. Joint aspiration is only recommended if one suspects septic arthritis.
In children, Lyme meningitis is rare if:
- the headache is less than 7 days
- CSF has less than 70% mononuclear cells
- absence of the 7th or other cranial nerve palsy
The ECG may reveal an AV block. Brain imaging may show abnormality in 20% of patients with CNS symptoms. The most common are punctate lesions of the periventricular white matter. Borrelia species are had to culture and not routinely done.
Treatment / Management
Specific treatment is dependent upon the age of the patient and the stage of the disease. For patients older than 8 years of age with early, localized disease, doxycycline is recommended for 10 days. Patients under the age of 8 should receive amoxicillin or cefuroxime for 14 days to avoid the potential for tooth staining caused by tetracycline use in young children. Longer courses and parenteral antibiotics may be required for more severe manifestations such as arthritis, atrioventricular heart block, carditis, meningitis, or encephalitis. However, European data and newer studies demonstrate that oral treatment regimens or transitioning to oral therapy at hospital discharge may be appropriate for some patients.[11][12][13]
Doxycycline is used in most patients except in children and pregnant women. In children, amoxicillin remains the drug of choice. Pregnant women show a good response to ceftriaxone.
Patients with Lyme carditis should be admitted and monitored until the ECG features of a block subside. Lyme arthritis usually resolves in 6-8 weeks. CNS Lyme disease responds well to antibiotics, most commonly with ceftriaxone. Clinicians should monitor patients for the Jarisch-Herxheimer reaction when starting therapy. The ocular feature of Lyme disease does respond to topical steroids and IV ceftriaxone or penicillin. Some patients may experience posttreatment Lyme disease syndrome with nonspecific symptoms. These symptoms do not respond to antibiotics. The Jarisch-Herxheimer reaction is a cytokine-mediated reaction to the antibiotic-mediated destruction of spirochetes. With Lyme disease, the reaction is seen in 5% to 15% of patients and usually resolves within 1 day.
Differential Diagnosis
In patients with erythema migrans, a careful history and physical examination are all required to diagnose Lyme disease. However, many patients with Lyme disease present with erythema migrans or extracutaneous symptoms where diagnosis becomes a challenge. In those cases, erythema migrans may never have occurred, may not have been recognized, or may not have been correctly diagnosed by the clinician.
Other problems include the following:
- Acute memory disorders
- Ankylosing spondylitis and rheumatoid arthritis
- Atrioventricular nodal block
- Cellulitis
- Contact dermatitis
- Gout and pseudogout
- Granuloma annulare
- Prion-related diseases
Staging
Stages of Lyme disease
- Stage 1: Localized disease associated with erythema migrans and flu-like symptoms; duration 1 to 30 days
- Stage 2: Early disseminated disease with malaise, pain, and flu-like symptoms; may affect the neurological, ocular, and musculoskeletal organs; duration 3 to 10 weeks
- Stage 3: Late or chronic disease chiefly affects the joints, muscles, and nerves and may last months or years. Lyme arthritis is a hallmark of this stage.
- The occurrence of post-treatment Lyme syndrome is debatable.
Prognosis
For early cases, treatment is usually curative. However, treatment may be complicated due to late diagnosis, antibiotic treatment failure, and concomitant infection with other tick-borne diseases such as ehrlichiosis, babesiosis, and immune suppression.
Approximately 5% of patients have lingering symptoms of fatigue, pain, or joint and muscle aches after treatment. These symptoms can last for 6 or more months. This is called post-treatment Lyme disease syndrome. Chronic Lyme disease is generally managed similarly to fibromyalgia or chronic fatigue syndrome. Whether chronic disorder exists remains debatable. The reason is that many non-validated testing systems on the market are often falsely positive. In addition, there has been a public hysteria about chronic Lyme disease, with patients demanding treatment. The workup is usually negative in most cases of chronic Lyme disease. Further, there is no evidence that long-term antibiotic therapy helps. Most patients eventually recover without any residual sequelae.
Complications
The complications that can manifest with Lyme disease are as follows:
- Arthritis
- Carditis
- Neurological deficits
- Ocular manifestations
- Acrodermatitis chronica atrophicans
Consultations
Consultations that are typically requested for patients with this condition include the following:
- Infectious disease
- Dermatologist
- Neurologist
Pearls and Other Issues
Based on the geographic distribution of the shared vector Ixodes scapularis, coinfections with Lyme disease and human granulocytic anaplasmosis and/or babesiosis can occur. Co-infected patients may be more severely ill at presentation, have a persistent fever longer than 48 hours after initiating antibiotic therapy for Lyme disease, or present with anemia, leukopenia, and/or thrombocytopenia. When co-infection is suspected or confirmed, treatment with an appropriate antimicrobial regimen for each infection is necessary to resolve the illness.
Enhancing Healthcare Team Outcomes
The key to Lyme disease is prevention, requiring an interprofessional team approach. All healthcare workers should educate patients on preventing tick bites while hiking or working outdoors. In areas where ticks are common, cleaning up the environment by removing the underbrush and spraying an insecticide may reduce the tick burden in the area. The outdoors person should be told to wear appropriate garments and be familiar with the skin features of the tick bite. The nurse should educate the patient on how to remove the tick from the skin and when to seek medical assistance. The pharmacist should educate the patient on medication compliance for those confirmed to have acquired Lyme disease.
Healthcare professionals should educate parents on how to inspect their children for ticks at the end of an outdoor event in an endemic area. While many repellants are on the market, it is best to avoid them as the risk of harm is greater than any benefit. If one is going to use a repellant, DEET is the 1 product often used; however, it is not 100% effective. Finally, the pharmacist should educate the patient about the harms of taking prophylactic doxycycline; a better strategy is to remove the tick as soon as it is visualized.
Finally, pets can also develop Lyme disease and carry the tick. Hence, pet owners should examine their pets regularly and remove the tick. There is no risk of acquiring Lyme disease by removing the tick.
Patients need to be told that there are many unvalidated tests for Lyme disease which offer false-positive results. Even though there is a Lyme vaccine, the public should be educated that the effects of the vaccine are not consistent or long-lasting; hence one should not rely on the vaccine to prevent Lyme disease.[14][15]
Outcomes
The prognosis for patients treated for Lyme disease is excellent, with no residual deficits. However, a few individuals may develop a recurrent infection if an infected tick bites them. Individuals who receive late treatment may develop neurological and musculoskeletal symptoms. Lyme arthritis is not uncommon. Some patients may develop Lyme carditis which results in a heart block and requires temporary pacing of the heart. Despite the large number of people affected, Lyme disease is not fatal. There continues to be a debate about the existence of posttreatment Lyme disease. Still, this diagnosis has been promoted by the lay public and media, as there is no good evidence that such a condition exists.[16][17]