Continuing Education Activity
Calcaneus fractures are rare but potentially debilitating injuries. The calcaneus is one of seven tarsal bones and is part of the hind-foot which includes the calcaneus and the talus. The hindfoot articulates with the tibia and fibula creating the ankle joint. The subtalar or calcaneotalar joint accounts for at least some foot and ankle dorsal/plantar flexion. Historically a burst fracture of the calcaneus was coined a "lovers' fracture" as the injury would occur as a suitor jumped off a lover's balcony to avoid detection. This activity reviews the causes, presentation, and diagnosis of calcaneus fractures and highlights the role of the interprofessional team in their management.
Objectives:
- Describe the pathophysiology of calcaneus fractures.
- Review the evaluation of a patient with a calcaneus fracture.
- Summarize the treatment options for calcaneus fractures including surgical options and the risks and benefits associated with treatment.
- Explain the importance of improving care coordination among interprofessional team members to improve outcomes for patients affected by calcaneus fracture.
Etiology
Calcaneal fractures most commonly occur during high energy events leading to axial loading of the bone but can occur with any injury to the foot and ankle. [4][5] Falls from height and automobile accidents are the predominant mechanisms of injury, although jumping onto hard surfaces, blunt or penetrating trauma and twisting/shearing events may also cause injury. Most of the injuries cause the bone to flatten, widen, and shorten. Stress fractures may occur with overuse or repetitive use, such as running.
Pathophysiology
Falls from a height directly translate energy into the calcaneus on impact as the heel strikes a surface crushing the calcaneus against the talus. The talus acting as a wedge causes depression and the widening of the calcaneal body. [6][7]Similarly, a foot depressed against an accelerator, brake or floorboard translates a large amount of force through the calcaneus during high-speed automobile accidents. Fracture patterns are similar in either mechanism. Gunshot wounds and other ballistic injuries cause a more diffuse nonpredictable fracture pattern but remain uncommon. Avulsion fractures require a large amount of twisting or shearing force due to the strength of the ligamentous and tendinous attachments to the calcaneus. The tibial artery and nerve run along the medial aspect of the calcaneal body and are thought to be shielded by the sustentaculum tali thus neurovascular injuries are uncommon with calcaneal fractures.
Evaluation
Evaluation of a potential calcaneus fracture should include the following:
- Complete neurovascular examination as well as evaluation of all lower extremity tendon function. Loss of ipsilateral dorsalis pedis or posterior tibial pulse compared to contralateral limb should raise suspicion of arterial injury and prompt further investigation with angiography or Doppler scanning.
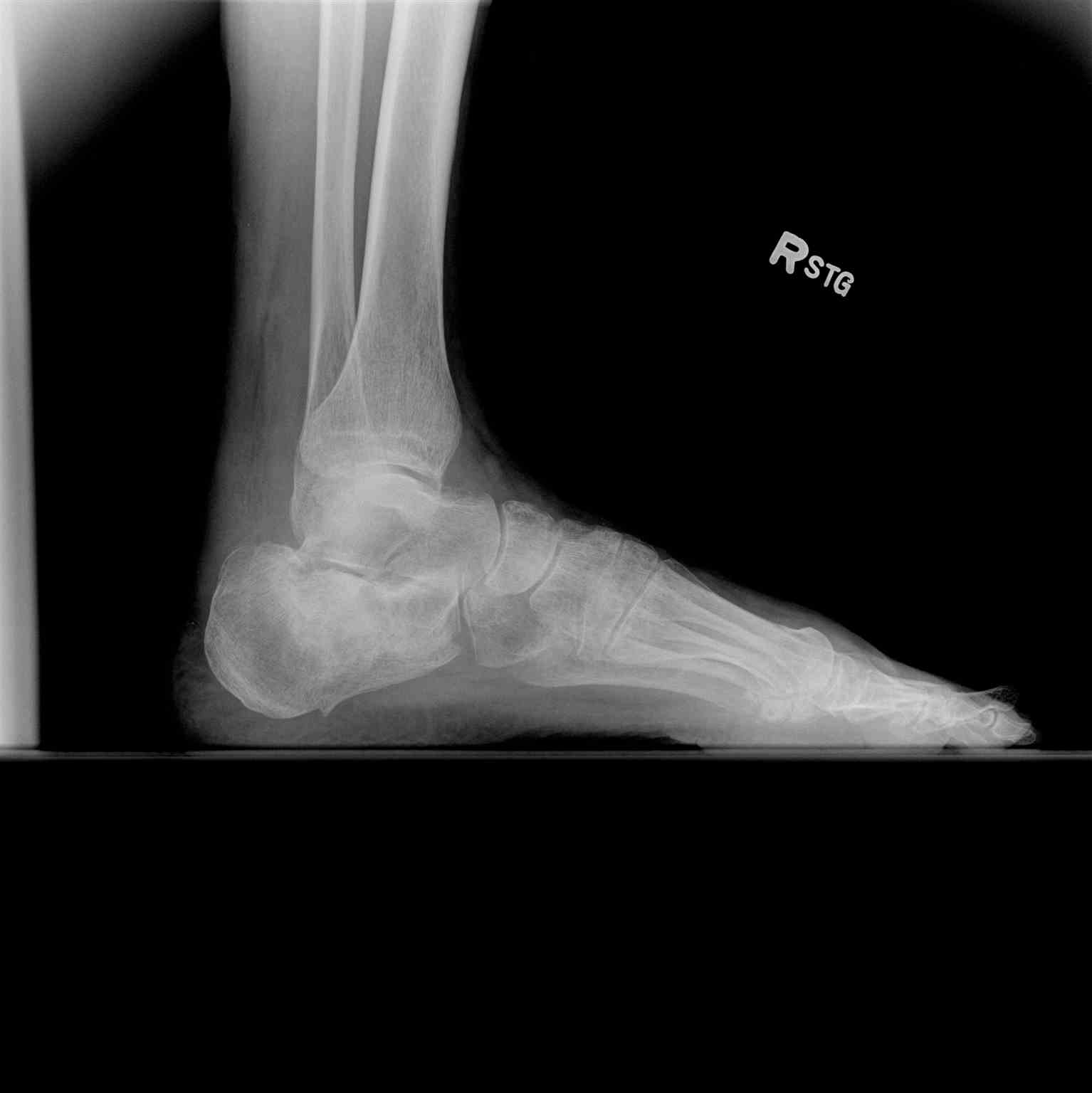
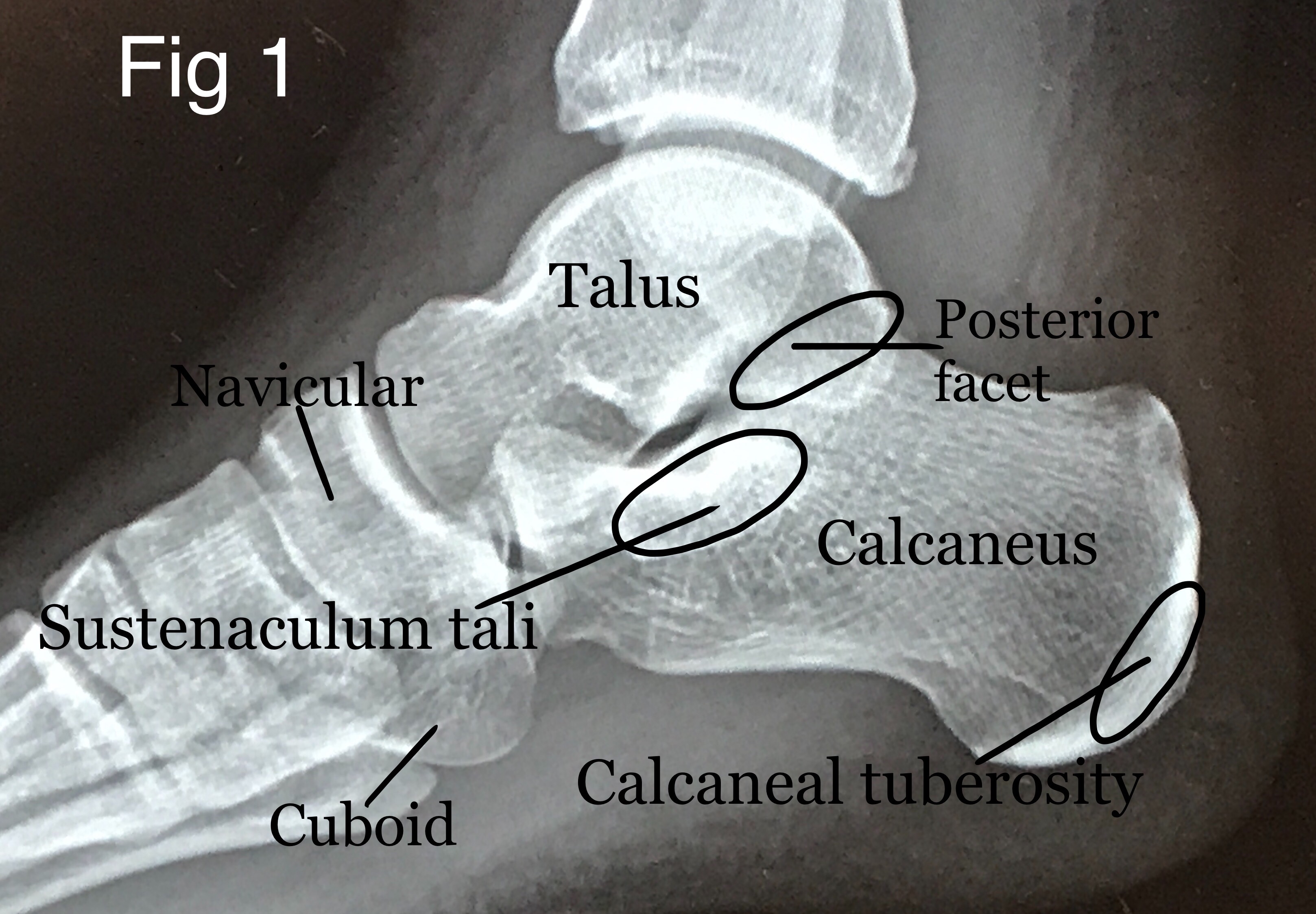
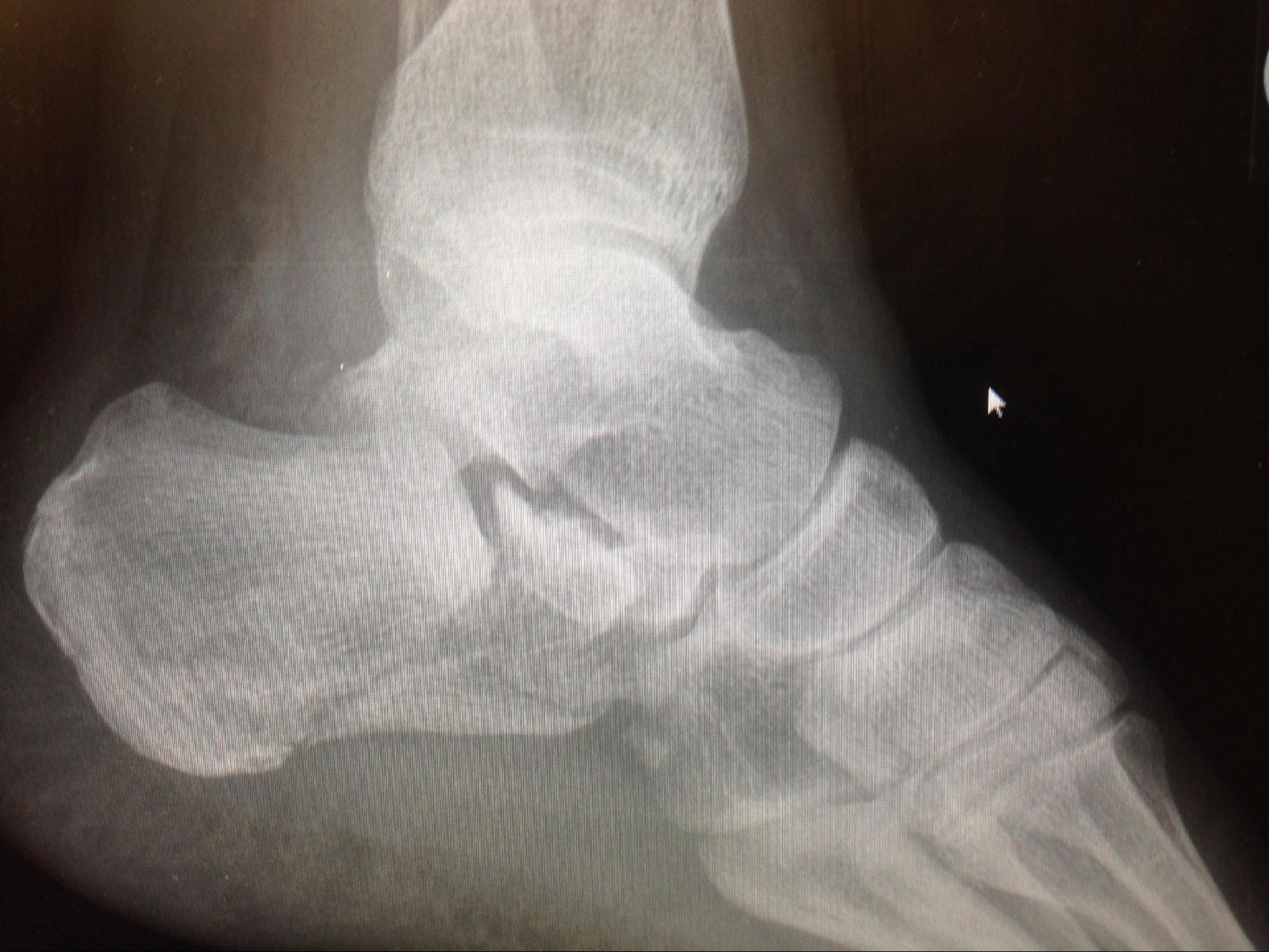
- Initial bony evaluation with AP, lateral, and oblique plain films of the foot and ankle is needed. A Harris View may be obtained which demonstrates the calcaneus in an axial orientation. [8]
- Noncontrast computed tomography remains the gold standard for traumatic calcaneal injuries. CT scan is used for preoperative planning, classification of fracture severity, and in instances where the index of suspicion for a calcaneal fracture is high despite negative initial plain radiographs (2 to 3-mm cuts are recommended).
- Mondor's Sign is a hematoma identified on CT that extends along the sole and is considered pathognomic for calcaneal fracture.
- Stress fractures such as those seen in runners would be best evaluated with a bone scan or MRI.
- Bohler's Angle may be depressed on plain radiographs. Defined as the angle between two lines drawn on plain film. The first line is between the highest point on the tuberosity and the highest point of posterior facet and the second is the highest point on the anterior process and the highest point on the posterior facet. The normal angle is between 20-40 degrees.
- The Critical Angle of Gissane may be increased. Defined as the angle between two lines drawn on plain film. The first along the anterior downward slope of the calcaneus and the second along the superior upward slope. A normal angle is 130-145 degrees.
- Normal Bohlers and Gissane angles do not rule out a fracture.
- Abnormalities of either of these findings should prompt a CT scan for further classification and evaluation of the fracture.
Calcaneal fractures can be classified into two general categories.[9][10]
- Extraarticular fractures account for 25 % of calcaneal fractures. These typically are avulsion injuries of either the calcaneal tuberosity from the Achilles tendon, the anterior process from the bifurcate ligament, or the sustentaculum tali.
- Intraarticular Fractures account for the remaining 75%. The talus acts as a hammer or wedge compressing the calcaneus at the angle of Gissane causing the fracture.
There are two main classification systems of extraarticular fractures.
Essex-Lopresti:
- Joint depression type with a single verticle fracture line through the angle of Gissane separating the anterior and posterior portions of the calcaneus.
- Tongue type which has the same verticle fracture line as a depression type with another horizontal fracture line running posteriorly, creating a superior posterior fragment. The tuberosity fragment may then rotate superiorly.
Sanders Classification: Based on reconstituted CT findings.
- Type I fractures: 1 nondisplaced or minimally displaced bony fragment
- Type II fractures: 2 bony fragments involving the posterior facet. Subdivided into types A, B, and C depending on the medial or lateral location of the fracture line.
- Type III fractures: 3 bony fragments including an additional depressed middle fragment. Subdivided into types AB, AC, and BC, depending on the position and location of the fracture lines.
- Type IV fractures: 4 comminuted bony fragments.
Treatment / Management
Initial treatment includes:
- Aggressive wound care and antibiotics as needed for contaminated wounds. [11]
- Analgesics.
- ICE and elevation.
- Immobilization with splinting, Bulky Jones type splints are commonly applied.
- All patients who are candidates for outpatient treatment are non-weight bearing at discharge.
Closed fractures
- All surgical treatment is aimed at restoration of heel height and width (i.e., reconstructing the anatomy to reapproximate Bohler and Gissane angles), repair and realignment of the subtalar joint, and returning the mechanical axis of the hindfoot to functionality.
- Most extraarticular fractures are treated conservatively with 10-12 weeks of casting (true extra-articular fractures only account for roughly 20% of all calcaneal fractures)
- Calcaneal tuberosity avulsion displaced sustentaculum tali, and large substantial calcaneal body fractures may require operative management.
- Some intraarticular injuries may be treated in a closed fashion depending upon severity. Many are treated with either open surgical reduction and internal fixation, percutaneous pinning, or sometimes arthrodesis.
- Nondisplaced Sanders type I fractures may be treated in a conservative, closed fashion.
A recent randomized controlled trial reviewed operative versus non-operative treatment for closed, displaced, intra-articular calcaneus fractures. It included a total of 151 patients with 73 in the operative arm and 78 in the non-operative arm. The operative group was treated as described below with the extensile lateral approach and the non-operative group was treated with initial immobilization followed by gentle mobilization as allowed by pain. The results of the trial included a higher complication rate including infection and a requirement to remove hardware in 11% of the operative group, but there were no differences between the group with regards to health outcomes, range of motion, heel width, walking speed, and gait. All participants of the study recovered very slowly from injury, most improvement plateaued at 18 months and most participants reported ongoing adverse effects from their injury at 2 years. This study concluded with recommendations against operative intervention for closed, displaced, intra-articular fractures of the calcaneus. [12]
A more recent meta-analysis from 2017 composed of 18 trials including 1467 patients found significantly improved anatomical improvements with operative intervention with regards to the restoration of Bohler's angle, calcaneal heights and widths as well as the likelihood of resuming former work. The meta-analysis did confirm the higher complication rate of operative intervention but concluded that operative treatment of displaced, intra-articular calcaneal fractures has better anatomic recovery, functional outcomes and return to work. [13]
Surgical Treatment:
When surgical management is recommended it is with the goal to restore calcaneal morphology and to restore articular congruency. The decision to move forward with surgery must be based on fully informed consent of the abundant risks and expected benefits of surgery and must involve the patient in shared decision making as the operative intervention for calcaneal fractures is fraught with complications.
Surgical treatment must be delayed until the so-called, "wrinkle sign," returns. This will usually occur five to ten days following the injury. Furthermore, all serous and hemorrhagic blisters must be epithelialized. [8] Sanders et all describe that the soft tissue swelling may take up to 21 days to resolve and that surgery should not proceed until this has occurred. [14]
Surgical intervention is typically recommended for the following indications: [15]
- Displaced tongue type Fractures
- Joint depression with articular comminution or anterior process involvement
- Bohler's angle of <5 degrees on initial presentation
- Fracture Dislocation
- Anterior process fractures with >25% of the calcaneocuboid articulation involved
- Calcaneal body fractures with significant varus or valgus malalignment, lateral impingement, loss of calcaneal height, or significant translation of the posterior tuberosity.
Open fractures
Open calcaneal fractures require emergent irrigation and debridement and careful wound management. Outcomes with open calcaneal fractures are generally poorer than closed fractures. An article by Aldridge et al in 2004 reviewed a case series of open calcaneal fractures and found that despite an increase in complications the quality of life metrics was higher than expected. They found that despite a higher complication rate than closed calcaneal fractures treated operatively the complication rate in their paper was not as high as had been previously reported in the literature. [16] Aldridge's group did recommend that definitive fixation not be performed at the time of initial irrigation and debridement.
Previous literature by Siebert et al included 36 open calcaneal fractures in which there were 23 cases with complications including need for soft tissue coverage, nine cases of osteomyelitis, five amputations and one arthrodesis. Their cohort of patients additionally had poor quality of life metrics post-operatively. The worst results with regards to patient-reported outcomes and complications were found in the Grade III open fractures. [17]
Surgical treatment tends to fall into one of two categories, the open extensile lateral approach, and minimally invasive techniques. Tourniquet use is recommended for both approaches.
The Extensile Lateral Approach:
The extensile lateral approach has been the primary approach for many years for operatively treating calcaneal fractures. It allows for adequate visualization intra-operatively and allows for manipulation of the fracture to restore alignment and articular surfaces. The extensile lateral approach is performed by creating full-thickness soft tissue and periosteal flaps as previously described by Gould and lateral modified by Benirschke and Sangeorzan. [18]The lateral calcaneus and joint surfaces can be well visualized and typically temporary retraction is created by the placement of Kirschner wires into the talus, fibula, and cuboid.
The fracture lines are opened at this time and may include temporary removal of the lateral wall. Manual traction is used to restore the high and length of the tuberosity (placement of a Steinmann pin into the tuberosity is helpful in restoring these parameters). The varus deformity must also be corrected at this time. A temporary reduction may be maintained by the placement of Kirschner wires through this tuberosity fragment into the "constant" fragment of the medial sustentaculum. The lateral posterior facet joint surface must be anatomically reduced under direct visualization and may be held with temporary fixation, typically lag screw fixation will allow for compression and healing across the articular surface as described by Sanders et al [14]. Care must be taken to ensure one does not over-penetrate the medial cortex. Over penetration of the medial cortex of the constant fragment may lead to entrapment of the flexor hallucis longus tendon and fixed great toe flexion. Reduction and alignment should be verified with fluoroscopy and exchanged for definitive fixation and the wound should be closed in layers with many recommending drain placement. [18][14]. The closure is typically recommended with an interrupted Allgöwer-Donati stitch to try to relieve tension on the incision itself. Level 1 evidence supports the Allgöwer-Donati stitch's use over the vertical mattress suture in lower extremity trauma as the Allgöwer-Donati yields improved tissue perfusion at the incision site. [19]
The Minimally Invasive Approach:
The goals of the minimally invasive technique (or sinus tarsi approach) are to minimize soft tissue injury while simultaneously allowing for fracture reduction and stabilization. The indication for this approach includes Sanders type II and III, patients with comorbidities that make soft tissue more vulnerable to complications include diabetes mellitus, smoking and/or obesity, peripheral vascular disease, and minimal posterior facet fragment comminution. The sinus tarsi approach is performed by creating a 2-4cm incision along a line from the tip of the fibula towards the base of the fourth metatarsal base. that allows for direct visualization of the posterior facet and the anterolateral fragment of the lateral wall. Typically a small, low-profile is plate is used after reduction of the joint surface and is placed along the joint-line. Adjunctive percutaneous screws are often placed to assist with the other parameters of calcaneal morphology including height, width and hindfoot alignment. A Shantz pin is still used through a percutaneous incision for manipulation of the calcaneal tuberosity. Alignment is still evaluated under fluoroscopy. However, because of the lack of elevation of the L-flap, there is a decreased risk of peroneal tendon irritation and sural nerve complications. Of note, this same incision may be used for subsequent subtalar arthrodesis should that be necessary. [20]
Some authors contend that anatomic reduction, fracture disimpaction, and repositioning is exceedingly difficult with limited exposures. Once the surgeon has committed to the minimal approach conversion to the extensile lateral approach is not recommended and thus great care must be taken in determining the correct approach for the correct patient. [14]. However, a recent meta-analysis was performing comparing minimally invasive techniques with the standard lateral extensile approach. In this analysis, there were 2179 participants followed for an average of 22.41 months. The results of the analysis showed no statistically significant difference in post-operative calcaneal width, length, deep infection or Gissane's angle between the two approaches. There was, however, a difference between wound complications, superficial infection, nerve injury, VAS pain scores, American Academy of Orthopedic Foot and Ankle Society (AOFAS) scores, calcaneal height and post-operative Bohler's angle in favor of minimally invasive techniques. This part of the growing body of evidence that the smaller incision techniques may be useful in certain groups. [21]Of note, there was no comparison of pre-operative fracture morphology and many authors contend that more severe patterns require the extensile approach and are also predisposed to a higher complication rate.
Kline et al retrospectively reviewed a cohort of 112 calcaneal fractures in which 79 underwent the traditional extensile lateral approach and 33 were treated using minimally invasive techniques. This allocation was based on surgeon preference. The group demographics were comparable. The extensile group's fracture composition was 53% Sanders II and 47% Sanders III. The minimally invasive group's fracture composition was 61% Sanders II and 39% Sanders III. Both groups had a 100% union rate and similar radiographic parameters with regards to Bohler's angle and the angle of Gissane. The wound complication rate was 29% in the extensile lateral group with 9% of the total treated cases requiring repeat surgery for those complications. Only 6% of the minimally invasive group had wound complications and none required additional surgery. Kline et al concluded that the minimally invasive technique was valuable and could lead to a lower complication rate and comparable results. [22]. Many other groups have similar findings in that the sinus tarsi approach seems to lead to similar radiographic and functional outcomes with fewer wound complications overall. [23]
Special Cases:
Medial External Fixator Placement:
Some authors have adopted a two-stage surgical approach for severely displaced closed calcaneal fractures to try to mitigate the issue of soft tissue compromise. The calcaneus assumes a shortened and widened position with heel varus as a result of the fracture displacement and loss of Bohler's angle. A small series was performed by Githens et al with the supposition that medial external fixator placement would allow for improved soft tissue healing, early restoration of calcaneal morphology, and reduction of wound-related complications by re-tensioning the incision during the operative intervention. Twenty-one fractures were included in this series and the authors found that calcaneal length, height, and axial alignment can be restored with an external fixator, Bohler's angle cannot be restored with external fixator and ligamentotaxis alone. The authors had no deep or superficial wound infections requiring surgical intervention, which is promising but the authors simultaneously cautioned against drawing conclusions from such a small and limited series without statistical power or a control group. [15]
Tongue Type Fractures:
Tongue-type fractures can lead to variable amounts of displacement of the tuberosity fragment, but due to the pull of the Achilles tendon, significant superior and dorsal displacement may occur leading to the potential to tent the posterior heel skin and place the soft tissue at significant risk of breakdown. Emergent reduction to relieve this tented skin is often recommended. A temporizing measure is typically to place a removable posterior splint in plantarflexion with close skin monitoring until definitive treatment. If not treated emergently skin breakdown may lead to disastrous sequelae. Urgent fracture reduction should proceed at the first sign of skin compromise. [24]One hundred and thirty-nine tongue type fractures were reviewed at a single institution over a 5 year period and found an overall rate of 21% soft tissue compromise, further finding that fractures with greater initial displacement were at a greater risk of skin compromise. In patients with identified threatened soft tissue upon presentation treated with emergent operative reduction and fixation none went on to further soft-tissue complications[24].
Extremely comminuted fractures:
Some surgeons will favor primary subtalar arthrodesis as it seems to reduce the need for subsequent procedures and the associated increased costs and lost time from work associated with those additional surgeries. [25] However, other studies have found that patients who develop post-traumatic arthritis who first undergo open reduction internal fixation of their fractures with the intraoperative restoration of calcaneal morphology do better than those who develop subtalar arthritis due to malunion following non-operative treatment. [26]
Prognosis
The Sanders classification has been found to have sustained prognostic value. One hundred and eight calcaneus fractures operatively treated (Type II and III) were evaluated at a minimum of 10 years with an average follow-up time of 15.22 years. CT scan was performed immediately postoperatively and 95% of the fractures have posterior facet reduction to the anatomic position (with no appreciable step-off of the articular surface) and with no reductions >5mm inaccurately reduced. The results of this cohort of verifiably well-reduced fractures demonstrated that the type III fractures were 4 times more likely to require eventual subtalar fusion compared to type II fractures. Long-term functional results in this cohort resulted in mild pain and some alterations in activities of daily living. [14]
Certain Populations tend to have better results a well [27]:
- Women
- Younger Adults
- Patients with a lighter workload (office work compared to heavy manual labor employment)
- Patients not receiving workers compensation
- Patients with a higher initial Bohler's angle. The amount of initial displacement based on Bohler's angle of <0 degrees is correlated with lower functional outcomes. When the initial Bohler's angle is greater than fifteen degrees upon presentation their functional results will be better regardless of operative versus non-operative treatment. [8]
Complications
Due to the severe nature and the force required to sustain calcaneal fractures concomitant injuries must be considered.[28][29] Studies have shown greater than 70% of patients with calcaneus fractures have additional injuries.
- A thorough evaluation of the entire spine should be performed anytime a calcaneal fracture is identified especially when a fall is a mechanism. The force from impacting the ground translates through the lower extremity and upward sometimes causing spinal compression fractures.
- Compartment syndrome of the foot is a rare but severely debilitating complication of calcaneal fractures and can occur in up to 10% of the injuries. A high index of suspicion is needed in considering patients presenting with increased pain either after treatment or during the initial evaluation.
- Osteomyelitis, postoperative wound infection, malunion, and subtalar arthritis are all potential complications of calcaneal fractures and repair.
Infections and wound breakdown are the most common and devastating complications of the extensile lateral approach. Wound complications and infections can be as high as 37% and 20% respectively with operative intervention. [20]
Subtalar osteoarthritis may result from surgical or nonsurgical treatment with an increasing number of patients with non-operatively treated displaced intra-articular calcaneus fractures requiring late subtalar fusion as a result of subtalar arthritis. [8] Another study found that non-operative measures were up to 6 times more likely to lead to a late subtalar fusion due to symptomatic subtalar arthritis. [30]This is considered post-traumatic arthritis. Loss of subtalar motion is very common as well.
Sural nerve injury may result in up to 15% of cases treated operatively (more often with the extensile lateral approach). The risk is reduced with a more inferiorly based L-incision. [31]
Chronic pain is also a common complication, in many cases owing to post-traumatic subtalar arthritis, malalignment or stiffness resulting from the injury.
Peroneal tendon instability may result from displaced, intra-articular calcaneus fractures. [32] This may result from direct damage to the tendons themselves as a result of the injury or fracture fragments that may impinge on the tendons. Up to a 40% displacement of the peroneal tendons has been appreciated on CT scans of calcaneus fractures. [33]. Furthermore, with significant height loss, calcaneal widening and hindfoot varus subfibular impingement may result from soft tissue or osseous abnormalities. Subfibular impingement may result in lateral heel pain, particularly with eversion of the hindfoot. Techniques have been described to perform percutaneous calcaneal osteotomy and peroneal tendon decompression to try to alleviate subfibular impingement after calcaneal malunion. [34]
Enhancing Healthcare Team Outcomes
Calcaneus fractures have enormous morbidity and are often associated with many other injuries. Thus, the condition is best managed by an interprofessional team that includes a trauma surgeon, emergency department physician, orthopedic nurses, orthopedic surgeon, internist, and physiotherapist. All open wounds need immediate surgery. After surgery complications are common and may include compartment syndrome, osteomyelitis, wound infection malunion and subtalar arthritis. Non displaced fractures are managed conservatively.
Overall the outlook for patients with calcaneus fractures is guarded. Those with an isolated fracture do recover with time but those with a concomitant injury to the pelvis, spine, neck or head often require prolonged rehabilitation and still have residual physical deficits.
Displaced Type III fractures have a higher likelihood of resulting in subtalar fusion than lower classification injuries and patients should be counseled that further procedures may be required, including possible subtalar fusion. [14](Level III)
Complete recovery from a calcaneus fracture may take months or even years. [35][36](Level V)