Continuing Education Activity
The earliest written description of a brachial plexus injury (BPI) is attributed to Homer circa 800 BC in his depiction of a battle during which Hector struck Teucer over the clavicle with a rock, rendering him incapable of wielding his bow in The Iliad. In the simplest terms, the brachial plexus can be thought of as 5 nerve roots (C5 through T1), which originate in the posterior triangle of the neck and extend into the axilla and terminate in five nerves: musculocutaneous, axillary, radial, median, and ulnar. This activity reviews the pathophysiology, causes, presentation and diagnosis of brachial plexus injuries and highlights the role of the interprofessional team in its management.
Objectives:
- Review the causes of brachial plexus injuries.
- Describe the presentation of a patient with brachial plexus injury.
- Summarize the evaluation of a patient with brachial plexus injury.
- Explain the importance of improving care coordination among interprofessional team members to improve outcomes for patients affected by brachial plexus injury
Introduction
The earliest written description of a brachial plexus injury (BPI) is attributed to Homer circa 800 BC in his depiction of a battle during which Hector struck Teucer over the clavicle with a rock, rendering him incapable of wielding his bow in The Iliad.[1] In the simplest terms, the brachial plexus can be thought of as 5 nerve roots (C5 through T1), which originate in the posterior triangle of the neck and extend into the axilla and terminate in five nerves: musculocutaneous, axillary, radial, median, and ulnar. The plexus occasionally receives contributions from the C4 and T2 nerve roots.[2] The levels of the brachial plexus are arranged as roots, trunks, divisions, cords, and branches from proximal to distal, with the roots and trunks more commonly injured than the divisions, cords, and branches.
Etiology
Obstetric injury; severe trauma caused by falls, direct, blunt blows, or high-speed motor vehicle collisions; penetrating injury; forceful traction injury; and compression injury can all result in damage to the brachial plexus. Upper trunk traction injuries occur when the head and neck are violently pulled caudally from the shoulder and torso. Similarly, lower trunk traction injuries occur when the arm is violently abducted above the head.[3] In the polytrauma patient, injuries to the brachial plexus are rare, but concomitant blunt trauma to the head, torso, extremities, and major blood vessels often takes precedence for treatment and further obscures the clinical picture.[4]
Epidemiology
BPI is most common in younger males between the ages of 15 and 25.[3] In Naraka’s analysis of BPI in over 1000 patients,[5] he described the law of 7 seventies:
Approximately 70% of traumatic BPIs result from traffic accidents, of which 70% involve motorcycles or bicycles; of these patients, approximately 70% sustain multiple injuries; 70% of patients sustain a lesion of the supraclavicular plexus, of which 70% will have one or several avulsion of the plexus roots; 70% of these patients will also sustain root avulsions of the lower plexus; 70% of patients with root avulsions of the lower plexus will experience chronic pain.
Ballistic trauma is the second most common mechanism of injury to the brachial plexus and typically produces neuropraxia.[6] Injuries to the brachial plexus cause substantial debility and long-lasting difficulties in activities of daily living. The burden to the patient and their caregivers can come from psychosocial and socioeconomic reasons.
Pathophysiology
The spinal nerves form when the ventral and dorsal rootlets from the spinal cord converge. The ventral rami of the C5 through T1 spinal nerves form the roots of the brachial plexus. A dorsal root ganglion is a group of neuronal cell bodies that lies proximal to the convergence of the spinal nerves. Injuries that occur proximal to the dorsal root ganglion are appropriately termed “preganglionic,” while injuries distal to the dorsal root ganglion are termed “postganglionic.” Distinguishing between preganglionic and postganglionic BPI has substantial implications for treatment and prognosis. The chance of spontaneous recovery after preganglionic injury is low and therefore requires early surgical intervention. Avulsions of the C8 and T1 nerve roots may concomitantly injure the sympathetic ganglion, resulting in Horner syndrome, which presents with the pathognomonic triad of miosis, ptosis, and anhydrosis.[3]
History and Physical
Obtaining a thorough history in a patient with possible BPI is necessary to identify the injury mechanism, associated fractures, and other concomitant trauma to the neck, shoulder, and chest cage. Careful inspection of the patient can provide important clues to the extent of the injury. Considerable bruising and swelling may indicate deep trauma with possible vascular injury, which can be confirmed by evaluating the radial, ulnar, and brachial pulses. A detailed neurologic examination is warranted to ascertain the location of the lesion. Paralysis of the paraspinal muscles may indicate injury at the cervical level of the foramen. Firing of the latissimus dorsi muscle (innervated by the thoracodorsal nerve, a branch of the posterior cord) and pectoralis major muscle (sternal and clavicular heads innervated by the medial and lateral pectoralis nerves, respectively from the medial and lateral cords) should be evaluated to determine whether the lesion is proximal or distal to the cord level.[3]
Evaluation
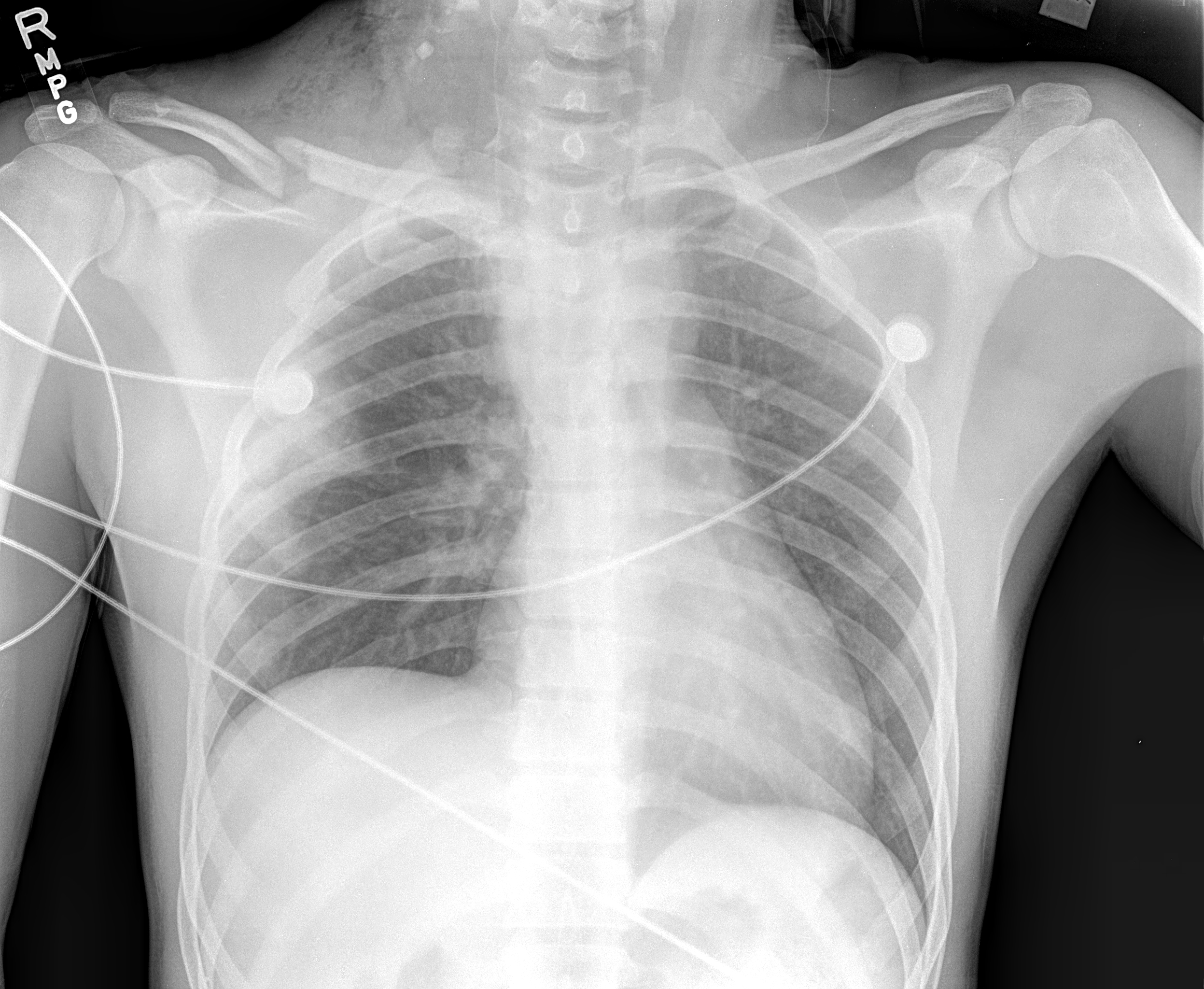
Plain radiographs must be evaluated for fractures of the cervical spine, transverse processes, clavicle, first rib, and scapula. Findings on initial examination are supplemented with advanced imaging and electrophysiological evaluation to determine the prognosis of neurologic recovery further. MRI and CT myelogram allow for identification of pseudomeningocele associated with root avulsions.[7] Hematoma at the site of the injury may distort the imaging; therefore, CT myelogram should not be performed earlier than 3 to 4 weeks from initial injury to allow for resorption. MRI of the cervical spine is less invasive than CT myelogram and also can provide information regarding inflammation and edema.[7]
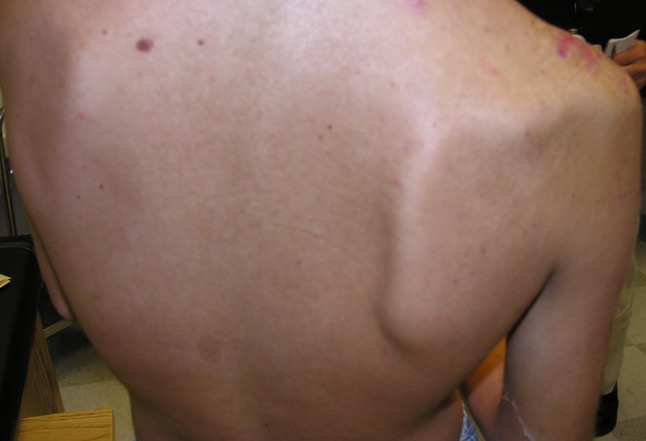
Recording of sensory nerve action potential (SNAP) in response to distal stimulation of the peripheral nerves helps to differentiate pre- and postganglionic lesions. If the patient exhibits a loss of sensation in a specific dermatomal distribution, a preserved SNAP is indicative of preganglionic injury due to the intact sensory cell bodies in the dorsal root ganglion.[8] Electromyography can also be utilized to differentiate pre- and postganglionic lesions by needle stimulation of proximal muscles innervated by nerves that branch off at the root level of the brachial plexus (paraspinal, rhomboid, and serratus anterior muscles).[3] The dorsal scapular nerve (C5) innervates the rhomboids. The long thoracic nerve (C5 through C7) innervates the serratus anterior muscle, and injury leads to medial scapular winging. The C5 contribution of the phrenic nerve may be injured with root avulsions, resulting in elevation of the ipsilateral hemidiaphragm on chest x-ray.
Treatment / Management
The surgical timing for the treatment of BPI remains a topic of controversy. Urgent surgical exploration of the plexus is indicated if a root avulsion or laceration injury to the plexus is suspected or in cases of open injury, retained foreign body, or vascular injury requiring vessel repair. Sharp transections of the brachial plexus allow for primary repair of the transected ends to optimize nerve regeneration. Prognosis for low-energy mechanism BPI is more favorable compared to root avulsions or preganglionic injuries and can be treated conservatively to allow for spontaneous recovery.[6] The patient should be closely followed with serial examinations, imaging studies, and electrophysiological testing. Delayed exploration may be indicated at three to six months after injury if the patient fails to regain neurologic function satisfactorily. There are few contraindications to brachial plexus surgery. In general, surgery should be avoided if the patient is not medically or psychologically cleared for surgery or if local wounds or infections obstruct the surgical approach. Adequate surgical exposure may be further obscured by edema and scar tissue in the cervical region. Other contraindications are determined on an individual basis. Chronic injuries to the brachial plexus that are more than 12 months old present a relative contraindication for surgical repair except in children who have greater regenerative potential. Low-demand patients and patients with underlying joint contractures may be poor candidates for surgery due to difficulty in achieving substantial functional improvements. Patients who may be noncompliant or unable to progress through the rigorous physical therapy regimen, which may continue for several years, are likely to have poor outcomes.[6]
Differential Diagnosis
Thoracic outlet syndrome - compression of the brachial plexus or subclavian vessels in the neck or axilla. Etiology may be soft tissue (scalene muscle hypertrophy) or bony (cervical rib) in nature. Vascular injuries and overuse in athletes may also results in TOS
Injuries of the shoulder joint (dislocation, AC joint injury, impingement, rotator cuff tear) - Traumatic injuries of the shoulder joint may be differentiated by plain radiography, MRI. Any neurologic deficits are often transient in nature.
Cervical spine pathology (cervical sprain, cervical radiculopathy) - Patients with cervical spine injury may present with neck pain, unilateral arm pain, weakness and paresthesias in a dermatomal distribution:
- C4 radiculopathy: scapular winging
- C5 radiculopathy: deltoid, biceps weakness
- C6 radiculopathy: brachialis, wrist extension weakness; numbness to thumb, index finger
- C7 radiculopathy: triceps, wrist flexion weakness; numbness to middle finger
- C8 radiculopathy: weakness in fine motor function of hand; numbness to ring, small fingers
Pearls and Other Issues
-
The brachial plexus originates from the ventral rami of spinal nerves C5, C6, C7, C8, and T1 but may occasionally receive contributions from C4 and T2.
-
Root avulsions may present with rhomboid/paraspinal muscle paralysis, medial scapular winging, Horner syndrome, and hemidiaphragm paralysis.
- Evaluation of latissimus dorsi and pectoralis major motor function helps to localize the lesion as supraclavicular or infraclavicular (proximal or distal to the cord level).
Enhancing Healthcare Team Outcomes
The diagnosis and management of BPI is extremely complicated and controversial. The injury is best managed by an interprofessional team that includes a neurologist, neurosurgeon, hand surgeon, physical therapist, internist, nurse practitioner and the primary care provider. After a diagnosis of BPI is made, the surgical timing for the treatment of BPI remains a topic of controversy.
There are few contraindications to brachial plexus surgery. In general, surgery should be avoided if the patient is not medically or psychologically cleared for surgery or if local wounds or infections obstruct the surgical approach. Adequate surgical exposure may be further obscured by edema and scar tissue in the cervical region. Other contraindications are determined on an individual basis. Chronic injuries to the brachial plexus that are more than 12 months old present a relative contraindication for surgical repair except in children who have greater regenerative potential.
Low-demand patients and patients with underlying joint contractures may be poor candidates for surgery due to difficulty in achieving substantial functional improvements. Patients who may be noncompliant or unable to progress through the rigorous physical therapy regimen, which may continue for several years, are likely to have poor outcomes.[6][9][10][11] Most patients do have residual neurological deficits and the quality of life is poor.[6]