Continuing Education Activity
Acrochordons (fibroepithelial polyps, skin tags, papillomas) are common benign neoplasms of the skin, often associated with obesity. These small pedunculated lesions are frequently a nuisance for patients, typically developing around the neck, axilla, and groin areas. They may bother patients because of associated symptoms such as itching, pain, and rubbing against clothes or simply because of their appearance. There may be a familial predisposition for developing these lesions, as well as the established association with obesity and insulin resistance. This activity reviews the diagnosis and management of these polyps, and highlights the role of the interprofessional team in caring for patients affected by these lesions.
Objectives:
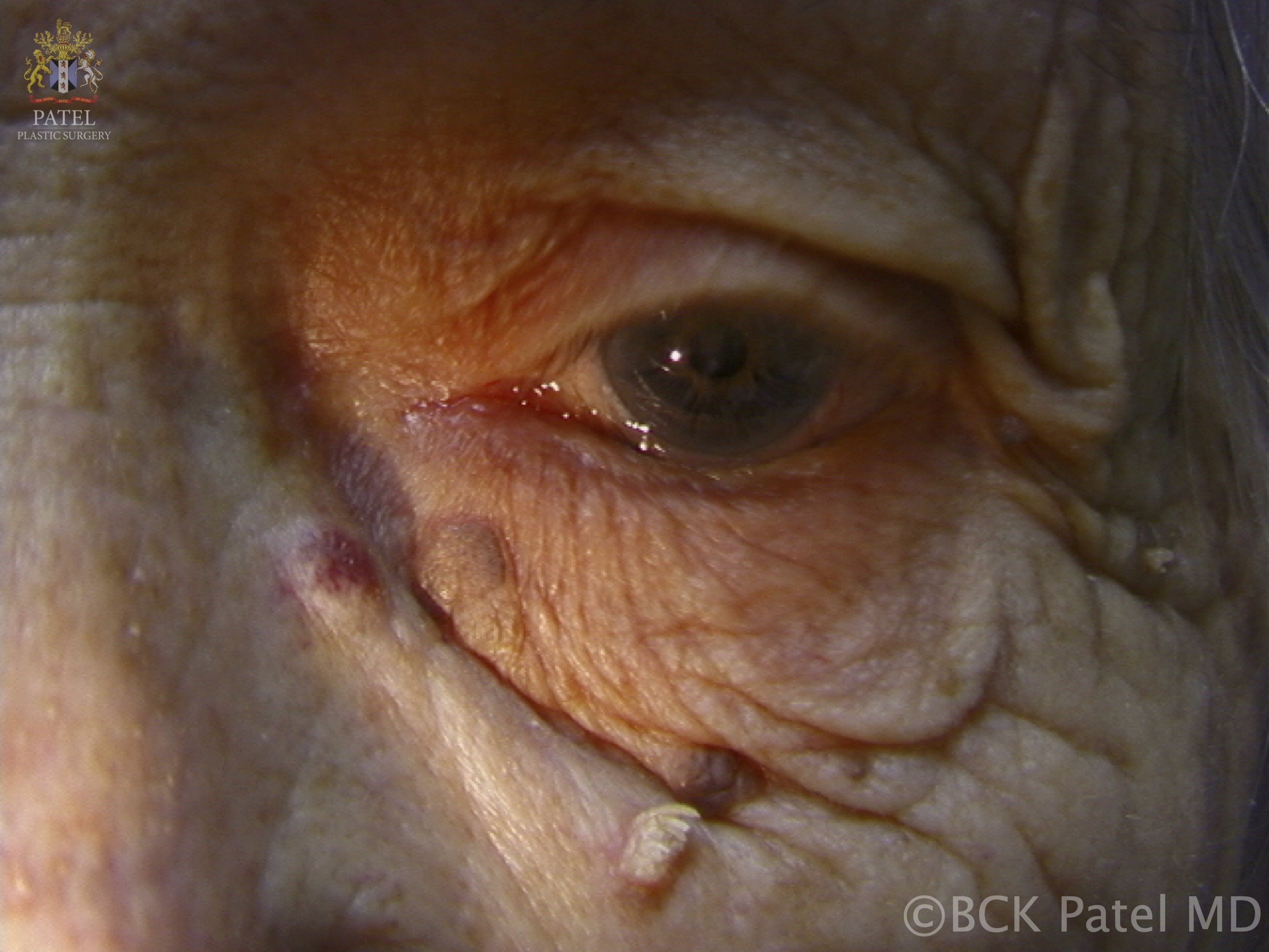
- Review the appearance and clinical features of an acrochordon.
- Histopathologic diagnosis is not routinely used to evaluate acrochordons. Identify cases where it should be considered.
- Identify the treatment options for patients presented with acrochordons.
- a collaborative, interprofessional team approach to caring with patients bothered by acrochordons.
Introduction
Acrochordons (fibroepithelial polyps, skin tags, papillomas) are common benign neoplasms of the skin, often associated with obesity. These small pedunculated polyps are frequently a nuisance for patients, typically developing around the neck, axilla, and groin areas. They can bother the patients due to associated symptoms like pain, itching and rubbing against clothes or sometime only because of their appearance. There is established association of acrochordons with insulin resistance and obesity along with a familial predisposition for developing such lesions. [1][2][3]
Etiology
Etiology of acrochordon is unknown, but it is hypothesized that they usually occur in localized areas with sparse elastic tissue that result in atrophic or sessile lesions. On the other hand, hormone imbalances also appear to be a cofactor for their development. Other factors promoting their growth are tissue growth factor, epidermal growth factor and infection. They mostly increase with age and sometime have a great cosmetic concern for the patients and their self-esteem decreases because of these skin lesions. [4][5]
Without histological confirmation, acrochordons cannot reliably be distinguished from benign melanocytic nevi and neurofibromas. However, since all of these likely possibilities in the differential diagnosis are benign, pathologic confirmation of such a diagnosis is not typically necessary since it will not impact management.
There is one inherited syndrome called Birt-Hogg-Dube syndrome, which is frequently discussed in the context of acrochordons. It is a rare autosomal dominant disorder characterized by multiple trichodiscomas along with fibrofolliculomas .These trichodiscomas are usually indistinguishable from acrochordons. On the other hand, a variant of basal cell carcinoma (BCC) may present with clinical overlap with acrochordons. The fibroepithelioma of Pinkus is another subtype of BCC that is classically reported as a pink acrochordon-like lesion on the lower back.
Epidemiology
Acrochordons have a high prevalence, reportedly 46% of the general population, increasing in frequency with patient age. Given that so many patients may have acrochordons, patients should be reassured that these are common benign lesions that should not be concerning. [6]
Histopathology
Skin biopsy with histopathology is usually not indicated unless the diagnosis is not clear. The typical acrochordons usually do not need to be sent to pathology. Histopathology examination is characterized by acanthotic, flattened, or frond like epithelium. A papillary-like dermis is composed of loosely arranged collagen fibers along with dilated lymphatic vessels and capillaries. [7][8]
History and Physical
- Small, soft, usually pedunculated lesions.
- Most commonly located on the neck, axilla, and inguinal folds (typically in intertriginous areas), though they can appear in almost any part of the skin.
- They may range from skin-colored to hyper pigmented
- Most vary in size from 2 to 5 mm or sometime larger ones do occur.
- Usually asymptomatic, but can be pruritic or become painful and inflamed by catching on clothing or jewelry.
Evaluation
There are no laboratory, radiographic, or other tests typically necessary to investigate patients with acrochordons. However, in the case that a clinician deems it necessary when removing multiple acrochordons to refer these specimens for pathologic evaluation, it is strongly recommended that each lesion is separated and placed in individually labeled containers. In the unlikely event that a lesion did end up being diagnosed as a concerning neoplasm (for instance, malignant melanoma), if all the lesions were placed in the same formalin specimen container, it would not be clear from which location the lesion of concern occurred.
Treatment / Management
Patients should be reassured that acrochordons are benign growths. There are various treatment options available:
- Snip excision: Small lesions can be snipped with small sharp iris scissor. This method usually works immediately and is very effective. It is not necessary to use anesthesia for the smallest skin tags.
- Cryotherapy: Liquid nitrogen can be applied directly to the skin tag with forceps or Cryo Tweezers or in the form of a spray from a cryogun. The Cryo Tweezers are usually very efficient and less painful. It is a very effective way to treat multiple skin tags.
- Shave Excision: Larger acrochordons may be removed with a shave or snip excision after injecting the base of the lesion with local anesthesia.
- Electrodesiccation: It works for very tiny lesions, too small to grab with forceps.[7][8][9]
- Follow-up is not usually necessary.
If a patient is suspected to have concurrent acanthosis nigricans, patients should be advised of the potential risk for diabetes. Such patients should be referred back to primary care and engage in discussions around the modification of diet and exercise. Even when acrochordons are present on the exam in isolation, since these patients often do have comorbidities including obesity, diabetes, or prediabetes, it is reasonable for any physician to encourage healthy eating habits, exercise, and other behavior modification to encourage benefits beyond the skin examination.
Differential Diagnosis
- Warts : Filiform warts usually resemble skin tags.The distribution of warts usually help to differentiate them from acrochordons.[1][2]
- Neurofibromas : These are benign soft pedunculated growth.
- Naevi : Different small pedunculated nevus usually resemble a skin tag. The size, pigmented pattern and location of naevi can differentiate these from acrochordons
- Seborrheic keratoses. For instance, some seborrheic keratosis, specifically the variant termed dermatosis papulosis nigra (DPN), may overlap clinically with acrochordons on the face. Dermatosis papulosa nigra typically present in a pattern of small, typically pigmented, pedunculated or simply raised papules on the face and adjacent structures. These are most common in patients of African-American descent.
Prognosis
It is a benigh skin condition usually do not need any treatment unless got irritated and also for cosmetic purposes.Reassuramce about the benign nature of disease usually decrease the anxiety of the patient.
Deterrence and Patient Education
- Advise patients that these growths are harmless and benign .These can be removed only if there is some discomfort ,irritation or for cosmetic concerns.
- If Patients are overweight, they should encouraged to lose weight. It would help to avoid new skin tags formation and improve the general health .
Enhancing Healthcare Team Outcomes
The primary caregiver and nurse practitioner should be aware that acrochordons are benign lesions and they usually require no treatment. Multiple lesions may be treated at one visit, although some patients may prefer to have one individual lesion treated first as a test spot.