Continuing Education Activity
Cheilitis is an inflammation of the lips. It may be acute or chronic, involving the vermilion and/or surrounding skin of one or both lips. It is a frequent reason for consultation. This activity describes the causes, pathophysiology, and presentation of cheilitis and highlights the role of the interprofessional team in its management.
Objectives:
- Identify the etiology of cheilitis.
- Review the presentation of a patient with cheilitis.
- Outline the treatment and management options available for cheilitis.
- Explain interprofessional team strategies for improving care coordination and outcomes in patients with cheilitis.
Introduction
Cheilitis is an inflammation of the lips, which could be acute or chronic. The inflammation primarily arises in the vermilion zone but may extend to surrounding skin and less commonly, to the oral mucosa. It may be caused by a multitude of factors, including contact irritants or allergens, chronic sun exposure, and nutritional deficiencies, as well as by various cutaneous and systemic illnesses.[1]
Etiology
Eczematous cheilitis could be a result of exogenous factors (irritant contact cheilitis, allergic cheilitis) or endogenous factors (atopic cheilitis).
Dry, chapped lips: Frequent exposure to hot or dry winds can cause loss of plasticity of keratin in vermillion, leading to sores and dry, scaly lips. The patient might get into the habit of chronic licking of lips to pick up scales, which further aggravates the problem.[2] It is also referred to as irritant contact cheilitis.
Allergic Contact Cheilitis: A delayed-type hypersensitivity reaction to allergens that come in contact with the lips can cause inflammation of the lips. It is also known as lipstick cheilitis since several ingredients found in lipsticks may act as irritants. The most common cosmetic sensitizers identified by patch testing include fragrances, Myroxylon pereirae, and nickel. However, some ingredients unique to lipsticks may also cause lip dermatitis. For example, castor oil, colophony, shellac, azo dyes, sesame oil, preservatives, ozonated olive oil, propolis, and copolymers. Apart from lipsticks, allergic contact cheilitis can be caused by a variety of other substances that come into contact with lips. They could be found in mouthwashes, toothpastes, and even food.[3] Lipstick cheilitis may present as persistent irritation and scaling, sometimes associated with edema and vascularization, confined to vermillion or extending beyond in some cases. Cheilitis caused by food may involve the skin around the mouth.[4]
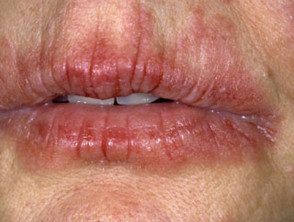
Atopic Cheilitis: Patients with a history of atopy or atopic dermatitis commonly have associated atopic cheilitis. It presents with dryness, erythema, scaling, and fissuring of lips.[5]
Angular Cheilitis: Angular cheilitis, also known as angular stomatitis or perlèche, is an acute or chronic inflammation of the skin and adjacent labial mucosa at the angles of the mouth. It manifests as a roughly triangulararea of erythema and edema at one, or more frequently both,angles of the mouth. [6]The most common cause of angular cheilitis in adults is a fungal infection, Candida albicans, and less commonly, Staphylococcus aureus. Poor oral hygiene, ill-fitting dentures, or absence of teeth as in the elderly can lead to excessive moisture and maceration from saliva leading to these infections. Less commonly, the nutritional deficiencies, particularly those of riboflavin (B2), niacin (B3), pyridoxine (B6), folate (B9), iron, and general protein malnutrition, may produce smooth, shiny, red lips associated with angular stomatitis, collectively known as cheilosis. [7]
Infective cheilitis:
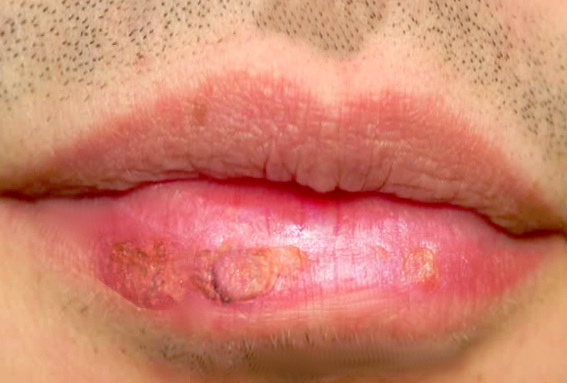
Viral cheilitis: It is mainly due to the herpes simplex virus, especially type 1. The primary herpes infection (herpetic gingivostomatitis) combines post-vesicular erosive and crusted cheilitis with diffuse stomatitis leading to dysphagia, perioral vesicles, fever, and cervical lymphadenopathy. Recurrence of oral herpes affects the lips in most cases. It manifests as a cluster of blisters accompanied by a burning sensation. Next, the vesicles erode to leave behind crusted erosions that resolve in a week.[2]
Bacterial Cheilitis: The most common cause of bacterial cheilitis is infection with group A Streptococcus or Staphylococcus.[6]
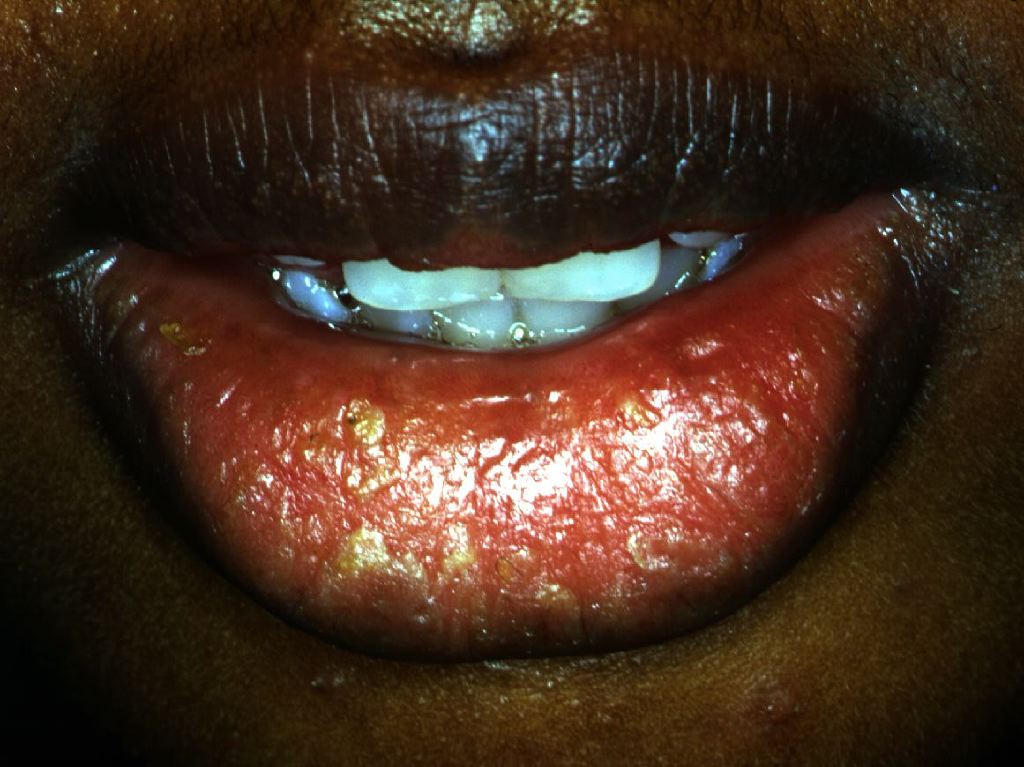
Mycotic cheilitis: Cheilitis caused by candida manifests with erythema and painful edema of the lips, sometimes with fissures, and it is usually accompanied by acute (pseudomembranous candidiasis) or chronic stomatitis, and/or angular cheilitis. The diagnosis is confirmed by taking a specimen for mycological examination.[8]
Parasitic cheilitis: Leishmaniasis is a possible cause of cheilitis in endemic regions. It gives the appearance of an erythematous papule or plaque that gradually enlarges and then ulcerates or a permanent lip enlargement (macrocheilia).[9]
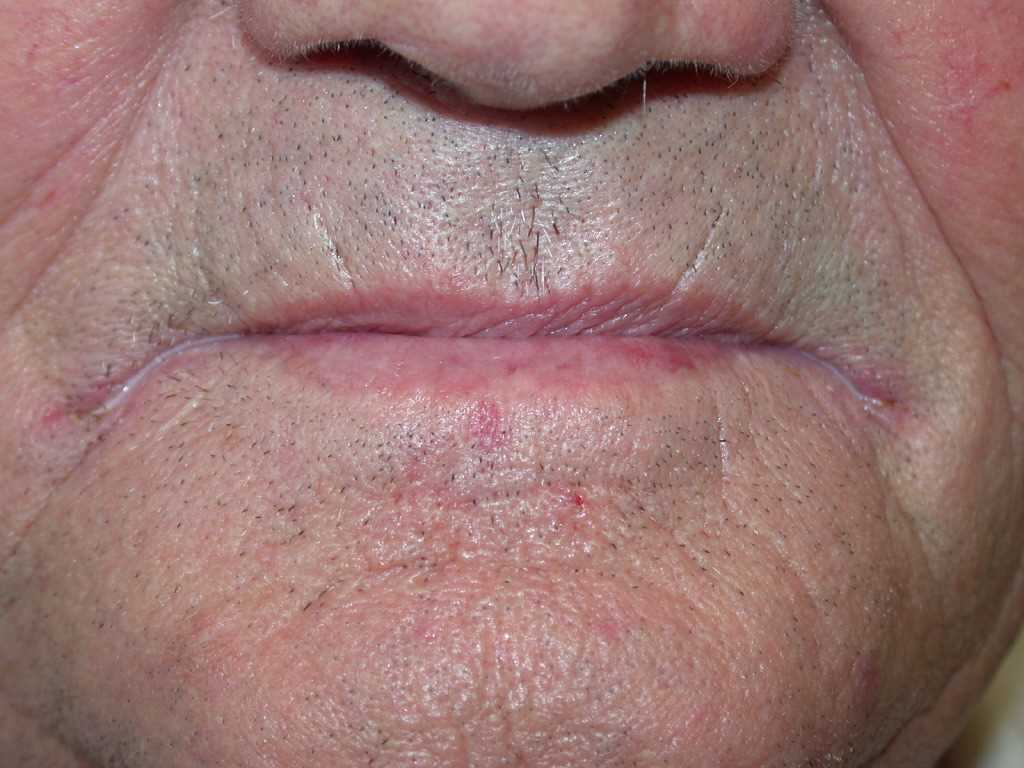
Actinic Cheilitis: Actinic Cheilitis (also known as solar keratosis of the lip or actinic keratosis) originates from the proliferation of atypical epidermal keratinocytes due to chronic sun exposure. It is a premalignant condition and occasionally progresses to squamous cell carcinoma.[10][11] Most cases are observed in outdoor workers, fair-skinned individuals, and during the fourth to eighth decades of life. The lower lip border receives the highest ultraviolet radiation, being at right angle to the midday sun rays and poorly protected by melanocytes. Clinical symptoms are varied, depending upon the stage of the disease, and may include erythema, edema, plaques, and nodules and later develop into ulceration as the lesion becomes malignant. Notably, the lesions have a characteristic "sandpapery" feel to touch.[12]
Drug-induced cheilitis: Systemic retinoids such as etretinate and isotretinoin cause dryness, erythema, scaling, and cracking of the lips (may include angles of mouth) in almost all the patients. Less frequently, it may also be caused by any other drugs that cause dryness of mouth and lip.[2]
Glandular cheilitis: It is a rare, chronic inflammation with tumefaction and sometimes suppuration of salivary glands at the lower lip. The most common clinical form is the simple cheilitis glandularis, which manifests as a moderate thickening of the lower lip with inflammatory dilated gland duct orifices, from which mucous saliva can be squeezed easily. [13][14]Older males are most commonly affected, but can also be seen in young individuals and women. In the more severe suppurative form (Volkmann’s cheilitis), the lip is enlarged considerably and persistently (macrocheilia) and is associated with pain and tenderness. Crusts and scales cover the surface, beneath which the salivary duct openings may be found. Eventually, it results in a deep-seated infection that may cause the formation of abscess and fistulous tracts.[13]
Cheilitis granulomatosis: Cheilitis granulomatosis is a persistent, idiopathic, nontender granulomatous inflammation of one or both lips. The initial manifestation is sudden diffuse or nodular swellings involving the upper lip, the lower lip, and one or both cheeks in decreasing incidence. Early attacks cause edema of lips that usually subsides in days to hours; however, recurrent attacks may lead to a persistent increase in swelling, leading to firm, rubber-like consistency of lips. [15]Cheilitis granulomatosis can be isolated, idiopathic (Miescher cheilitis granulomatosis), or associated with various systemic conditions (sarcoidosis, Crohn’s disease, tuberculosis). The complete form of Melkersson Rosenthal syndrome combines cheilitis granulomatosis, peripheral facial paralysis, and a fissured tongue with loss of taste sensation.[15][16]
Epidemiology
Eczematous cheilitis most common form of cheilitis and is more prevalent in people with a history of allergies. [5]
Angular cheilitis/infective cheilitis may present at any age with an equal male to female ratio but is especially likely in older individuals wearing dentures. Children suffering from these forms have a history of recurrent infections or immune defects.[17]
Actinic cheilitis is more prevalent in geographic areas with high ultraviolet (UV) irradiation, and in fair-skinned men who work outdoors (e.g., fishermen, farmers) in their fourth to the eighth decade of life. Certain genetic conditions associated with increased susceptibility to solar damage may predispose individuals to acquire actinic cheilitis at an early age (e.g., xeroderma pigmentosum, oculocutaneous albinism).[18][19]
Glandular cheilitis is a rare form of cheilitis, more prevalent in older males, but individuals in younger age and women also may be affected. The cause is unknown, but several factors have been identified, including atopy, infection, chronic exposure to the sun, repeated licking, and use of tobacco.[20][21]
Cheilitis granulomatosis is rare. It primarily affects young adults but can occur at any age, with equal ration in male to female. It is idiopathic. However, there are several predisposing factors, including food allergy, genetics, infection, and atopy.[22]
Pathophysiology
Eczematous cheilitis could be due to loss of plasticity, delayed-type hypersensitivity or atopy, depending upon the type.[2]
Angular cheilitis is a result of by softening of tissue from excessive moisture from saliva and secondary infection with Candida albicans or, less frequently, Staphylococcus aureus.[6]
Actinic Cheilitis originates from the proliferation of atypical epidermal keratinocytes due to chronic sun exposure.[10][11]
Drug-induced cheilitis is mainly caused by excessive dryness of mouth and lips.[2]
Glandular cheilitis results from fibrosis surrounding the salivary glands. Dense chronic inflammatory infiltrates may be found in severe cases.[13]
Cheilitis granulomatosis results from long-standing edema and perivascular inflammation of lip and facial tissue. As the infiltrates become more dense, pleomorphic and small focal granulomas are formed, indistinguishablefrom systemic granulomatosis.[15][16]
Evaluation
The diagnosis of most cheilitis is based on clinical signs and a careful anamnesis. The diagnosis of allergic contact cheilitis is confirmed by history of allergy and a relevant patch test reaction. Patients with negative patch testing are diagnosed with irritant contact cheilitis or atopic cheilitis. A biopsy is required in cheilitis granulomatosa to confirm the diagnosis. Once the diagnosis of granulomatous cheilitis is made, a thorough etiological assessment is necessary. A biopsy is also important in chronic actinic cheilitis if there is suspicion of malignant transformation. Finally, in the case of allergic cheilitis, an allergy survey is required. It includes a careful history and appropriate allergy tests.[2][23][24][25]
Treatment / Management
The therapeutic management of cheilitis is symptomatic and etiological:
Dry, chapped lips: Avoidance of lip sucking, lip balms, or any other causative agent, and the local application of petroleum jelly is helpful.[26]
Allergic contact cheilitis and atopic cheilitis: Excluding the allergen responsible and applying a low to medium intensity topical steroid and emollients. Sometimes a potent steroid (fludrocortisone) or off-label use of topical calcineurin inhibitors may be required.[4]
Angular cheilitis: The treatment is maintaining oral hygiene, using dentures with the proper fit, using barrier creams (eg, zinc oxide paste) or petrolatum and treatment of sicca symptoms. Vitamin supplements could be given in case of nutritional deficiency.[17] In case of cheilitis due to dentures, dentures must be removed before going to bed at night, brushed intensely, and then soaked in a solution of chlorhexidine gluconate or a dilute solution of bleach (10 drops of solution in a denture cup filled with water).[27]
Infective cheilitis: Maintaining proper oral hygiene, and treatment of the underlying cause of infection is indicated.[28] The most common infection is by Candida albicans which has different treatment approaches depending upon the associated HIV AIDS infection. Topical therapy with clotrimazole troches, miconazole mucoadhesive tablets, or nystatin swish and swallow is recommended as initial therapy in HIV seronegative patients and in HIV seropositive patients with mild thrush. Patients with recurrent infection, moderate to severe illness, or immunosuppression (CD4 <100 cells/microL) should be treated with systemic fluconazole ( an initial 200 mg loading dose, followed by 100 to 200 mg daily for up to 14 after clinical improvement).
Actinic cheilitis: A variety of treatments are used for the management of actinic cheilitis depending upon its severity. Simple observation with regular visits or treatment with liquid nitrogen is advised in case of focal mild or moderate actinic cheilitis. Patients with multifocal or diffuse symptoms may benefit from first-line therapy with topical medications (eg, topical fluorouracil, imiquimod). [19]5% fluorouracil cream is applied locally twice a day for two to four weeks. Discomfort associated with fluorouracil may lead to poor compliance and patient may be switched to imiquimod 5% cream ( three times per week for four to six weeks). Some may also require photodynamic or laser therapy. Patients with severe diffuse actinic cheilitis without evidence of high-grade dysplasia or cancer on biopsy should be treated with laser ablation with carbon dioxide (CO2) laser or erbium:yttrium-aluminum-garnet (Er: YAG). Surgical excision (vermilionectomy) ensures the histopathologic examination of the entire vermilion and is the treatment of choice for actinic cheilitis with high-grade dysplasia on biopsy.[18]
Drug-induced cheilitis: Lip moisturizers, emollients, and cessation of offending drugs lead to complete resolution of symptoms.[29]
Glandular cheilitis and cheilitis granulomatosis: Various therapies have been implicated for glandular cheilitis, including systemic antibiotics and corticosteroids (topical, intralesional, or systemic), and vermilionectomy (in case of severe symptoms).[20]
Differential Diagnosis
Differentials include lichen planus, sarcoidosis, angioedema, foreign body reaction, Crohn disease, Sjogren syndrome, and sarcoidosis.[2]
Consultations
Because of the many causes of cheilitis, the management is best done with an interprofessional team. The key is to make the diagnosis and the cause. For patients with chronic actinic cheilitis, referral to a plastic surgeon, dermatologist and oncologist is recommended as the treatment may vary from surgery, topical chemotherapy, laser or photodynamic therapy. Acute cheilitis can be managed by the primary care provider or nurse practitioner by offering the patient emollients. Patients with allergic cheilitis may require topical steroids and infectious causes may require antibiotics.[31]