Introduction
The pterygopalatine fossa (PPF) is a cone-shaped depression deep to the infratemporal fossa and posterior to the maxilla on both sides of the skull. The fossa is located between the pterygoid process and the maxillary tuberosity, close to the orbital apex. This space communicates with both the nasal and oral cavities, the infratemporal fossa, the orbit, the pharynx, and the middle cranial fossa through eight foramina. Three-dimensional understanding of this space is crucial for the rhinologist and skull-base surgeon for both the control of epistaxis and the removal of skull base lesions. The pterygopalatine space approach is used to treat lesions in the spaces posterior to the maxillary sinus, including the pterygopalatine space and lateral sphenoid recess. Pathologic processes in this space are rare, with the most common entities being juvenile nasopharyngeal angiofibroma, neurogenic tumors, a perineural extension of sinonasal malignancy, and meningoencephaloceles.[1][2]
Structure and Function
While not serving any specific functions, this space allows for the transit of several important structures through different foramina. The foramen rotundum connects the PPF to the middle cranial fossa. The pterygoid canal, also known as the vidian canal, connects the PPF to the middle cranial fossa. The palatovaginal canal connects the PPF with the nasal cavity and nasopharynx. Anteriorly, the inferior orbital fissure connects the PPF to the orbit. Medially, the sphenopalatine foramen provides access to the nasal cavity. Laterally, the pterygomaxillary fissure connects the PPF to the infratemporal fossa. Inferiorly, the greater palatine canal connects the PPF to the oral cavity.[3][4]
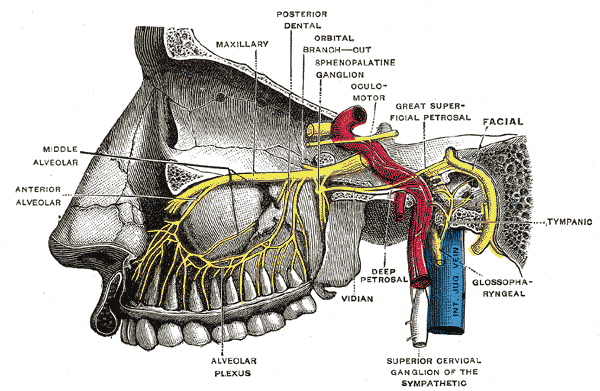
The pterygopalatine fossa also contains multiple important structures. This fossa contains the pterygopalatine ganglion. Nerve roots from the maxillary nerve suspend this ganglion. The PPF contains the terminal third segment of the maxillary artery. Furthermore, the maxillary division of the trigeminal nerve (CN V2) and the vidian nerve (the nerve of the pterygoid canal), which is a combination of the greater petrosal nerve and the deep petrosal nerve, traverse through the PPF as well.
The PPF is bounded by the maxillary, palatine, and sphenoid bones. The posterior wall of the maxillary sinus comprises the anterior border, and the palatine bone makes up its floor and anteromedial wall. The roof is made up of the sphenoid bone. More specifically, the sphenoid body and the orbital process of the palatine bone make up the superior boundary. The posterior wall of the maxillary antrum forms the anterior boundary. The pterygoid process and greater wing of the sphenoid constitute the posterior boundary. The medial boundary is made up of the palatine bone and nasal mucoperiosteum. Finally, the temporalis muscle via the pterygomaxillary fissure makes up the lateral boundary of the PPF.
The vascular and nervous structures are located anteroinferiorly and posterosuperiorly within the pterygopalatine fossa. The sphenopalatine artery, which is a branch of the internal maxillary artery, is found between the sphenoid and palatine bones and enters the nasal cavity at the sphenopalatine foramen. The maxillary division of the trigeminal nerve and the vidian nerve enter from the posterior wall of the PPF. The maxillary division of the trigeminal nerve moves through the foramen rotundum. The vidian nerve traverses through the pterygoid canal. They come together to form the pterygopalatine ganglion and then branch into the infraorbital nerve and the greater and lesser palatine nerves. The infraorbital nerve exits through the inferior orbital fissure and the greater and lesser palatine nerves pass through the greater and lesser palatine foramina respectively.
Posterior to the PPF, pneumatization of the lateral portion of the sphenoid bone results in the formation of a lateral sphenoid recess. This finding is observed in 25% to 48% of individuals. The roof of the lateral sphenoid recess can lie directly beneath the temporal lobe, and this is a common location for middle cranial fossa encephaloceles.
Surgical Considerations
When considering endoscopic resections of sinonasal cancer, the oncologic principle of adequate clearance of tumor margins must be the primary goal. Sinonasal tumors that originate within the maxillary sinus and the ethmoids/skull base can have both direct as well as perineural spread into the pterygopalatine and infratemporal fossas.[5][6]
The primary site of disease is managed first, and then the margins are cleared in the PPF. A medial maxillectomy is performed initially with the removal of the inferior and middle turbinates. This allows for complete visualization of the maxillary sinus. After creating the transmaxillary corridor, the trans-pterygopalatine fossa approach proceeds by stripping the mucosa that overlies the medial pterygoid wedge to expose the sphenopalatine artery. The sphenopalatine artery is then ligated, and the mucosa overlying the medial pterygoid plate is stripped down. The bone of the posterior maxillary wall is then removed, and the descending palatine artery either cauterized or ligated. It should be noted that the sacrifice of the palatine artery is not always necessary for liberal access and tumor removal within the PPF, but it can be undertaken for surgical access to the more lateral and deeper aspects of the infratemporal fossa. The Vidian nerve is then encountered and is often sacrificed. The orbital process of the palatine bone then drilled. The entire fossa is now mobile and can be resected or pushed laterally to gain access to the infratemporal fossa and pterygoid musculature.
Prior to undergoing surgical resection, it is important to obtain proper imaging of the paranasal sinuses and skull base. High-resolution CT images should be obtained using a stereotactic navigational protocol. Neurogenic tumors of the PPF usually enlarge the bony openings as they pass through the respective foramina. An MRI scan may also be beneficial in studying the anatomic outlines of the soft tissue structures, as well as assessing the perineural spread of a sinus or skull base neoplasms.
Clinical Significance
Several potential complications are specifically related to surgeries performed within the PPF. Damage to the Vidian nerve can result in chronic xerophthalmia. Removal of the pterygoid plates and associated muscles can lead to chronic trismus in the patient. CN V2 damage is possible while performing surgeries in either the PPF or infratemporal fossa. Finally, there can be an inadvertent injury to the carotid artery causing devastating consequences. While the carotid injury is unlikely when performing surgery within the PPF, stringent identification of the carotid artery is crucial while operating within the infratemporal fossa.[7][8]