Continuing Education Activity
There are over 470 species of sharks worldwide, and sharks generally prefer shallow waters in temperate and tropical regions. These regions are the most common sites for divers and surfers to become victims of shark-related injuries, though these injuries are rare. Nevertheless, when shark attacks occur, they cause an extreme degree of mutilation, even with a single bite. When shark bites do not result in death, massive blood loss, amputation, and vital organ puncture can occur. The frequency of shark attacks continues to increase due to an increased number of humans venturing into sharks' natural habitat. This activity describes the evaluation, diagnosis, and management of shark attack injuries and stresses the role of team-based interprofessional care for affected patients.
Objectives:
Identify the epidemiology of shark attack injuries.
Compare strategies for preventing shark attacks.
Determine the treatment options available for shark attack injuries.
Communicate interprofessional team strategies for improving coordination and communication to advance the management of shark attack victims and improve outcomes.
Introduction
There are over 470 species of sharks throughout the world. Their habitats include saltwater and freshwater alike. They generally prefer the shallows in temperate, tropical regions, which is usually where divers and surfers come into contact with them and potentially become the victims of shark trauma. While this is a genuine safety threat, it remains statistically unlikely. Nevertheless, for those shark attacks that do occur, they become increasingly more perpetuated secondary to the level of mutilation achieved from even a singular bite. The wounds sustained from a shark bite have not been shown to follow any singular disease course or bacterial growth pattern. Even when non-fatal, massive blood loss, amputation, and vital organ puncture can occur. Even though sharks have not become more aggressive over the years, the incidence of shark attacks is increasing, thought to be due to the rise of water activity by people within the sharks’ environment.
Etiology
Sharks may attack if they perceive humans as food; although, this is considered uncommon and generally a mistaken identity, for example, mistaking a thrashing limb or reflection from diving or snorkeling gear for a smaller fish. Attacks may be provoked if a human appears to be a threat or a competitor for food (and possibly mistaken as a mating competitor). Unnecessarily touching a shark is never recommended. Many bites occur when sharks are handled after being caught in nets or on fishing lines. Sharks may also attack to protect their territory. Although menstrual blood from a female swimmer could theoretically attract sharks, there is no evidence that this increases the incidence of shark attacks. However, some organizations still recommend that females avoid swimming in waters where a shark could potentially attack them during menstruation.[1]
Epidemiology
Worldwide, the International Shark Attack File notes 38 shark attacks on divers from 1990 through 1999. In the 10 years before this data, the number was 34, and only 20% of those attacks were fatal.[2]
Of the 470 shark species, only 30 have been found to have attacked humans, and only 4 of the 30 species make up most of the attacks. Sharks with the most documented attacks are the Great White shark, the Tiger shark, and the Bull shark, but the oceanic whitetip shark is believed to have the most attacks even though many of these are undocumented due to attacks occurring at sea, rather than in the coastal waters where attacks are more easily reported. Oceanic whitetip sharks are the sharks that quickly congregate around ship and airplane accidents.[3]
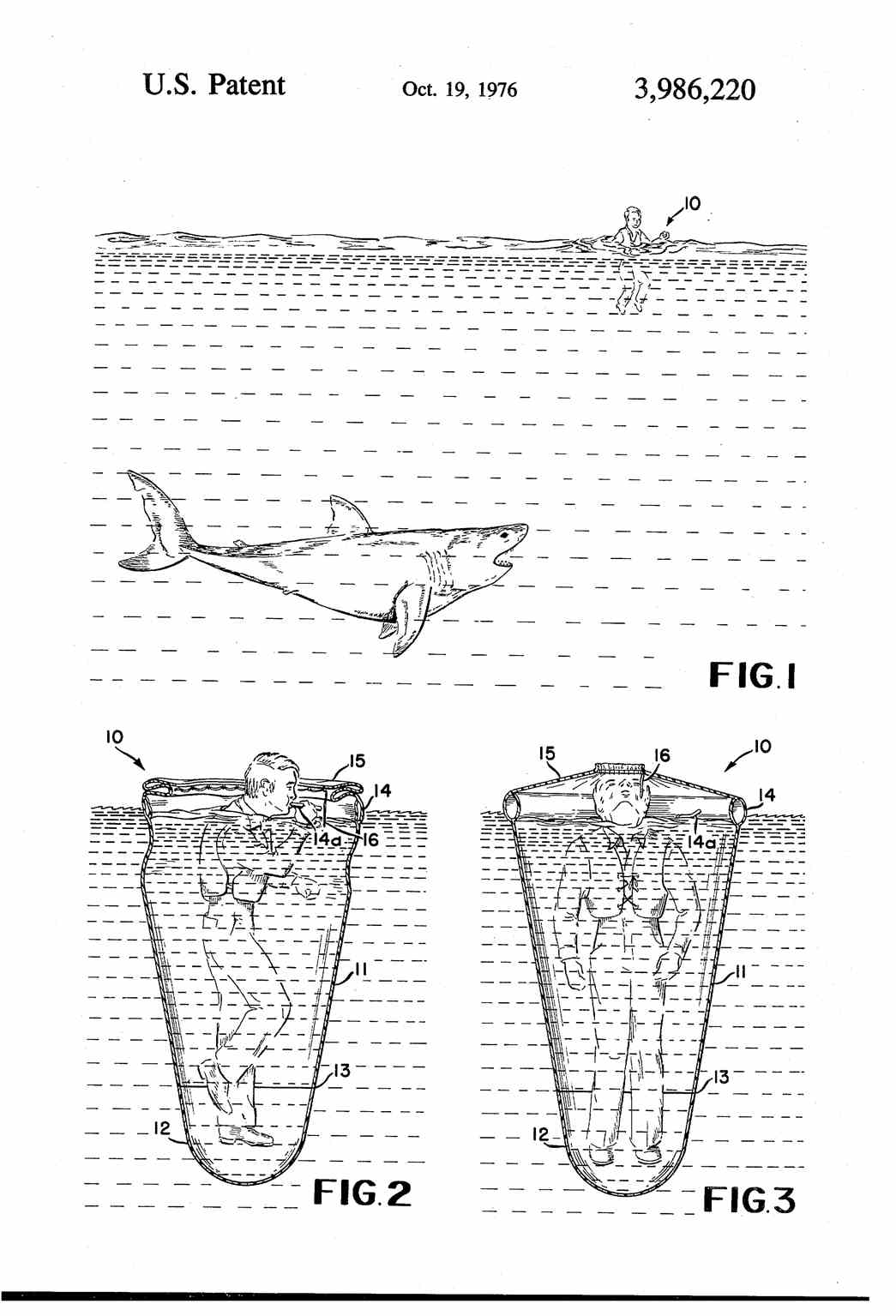
The scope of this problem is important. The United States is home to the world's overall shark attack capital (New Smyrna, Florida, although closely followed by South Africa and New South Wales) and the world's Great White shark attack capital (California). While shark attacks receive an inordinate amount of media coverage, the likelihood of being bitten by a shark in the United States in 2023 is less than 1 in 3.6 million. (See Image. Johnson Shark Screen). To put this in perspective, on average, 3,300 individuals drown each year in the United States, while shark attacks affect only around 91 people, and on average, only 1 of those cases is fatal. Knowledge about shark attacks can provide insight into areas and species to avoid. Almost half of all shark attacks are on surfers.[4]
Pathophysiology
Wounds sustained in marine environments are exposed to a multitude of bacterial species. Vibrio species are the predominant species found in seawater and on the teeth of great white sharks and are clinically significant to humans due to their pathogenic nature.[5][6] However, the actual profile of oral flora varies from species to species.[7] Other clinically relevant bacteria that are present include but are not limited to Staphylococcus, Streptococcus, Aeromonas, Clostridium, Erysipelothrix, Mycobacterium, Pseudomonas, Plesiomonas, and Shewanella.[5] Foreign bodies, including shark teeth fragments, can be introduced into these bites and serve as a nidus for infection. The tissue is often revitalized, making infection a very serious threat. Damage to the neurovascular bundles in bites may cause considerable long-term deficits.
History and Physical
Once stabilized, or if the patient is initially stable on presentation, obtain a thorough history of the events that led up to and occurred during the shark encounter. Any current medical co-morbidities, including those that may predispose to immunocompromised states such as diabetes, liver cirrhosis, alcohol use, or immunosuppressant medication, and any previously existing neurologic deficits, are important to know and document. The history should also include the patient’s tetanus vaccination status. Injuries should be examined carefully to determine their extent, the degree of devitalized tissue, neurologic and vascular integrity, bony injury, and foreign bodies.
Evaluation
Imaging should be performed to evaluate for retained pieces of shark teeth in wounds, fractures, and periosteal damage. An X-ray, ultrasound, or CT scan can identify such objects. CT angiography can be used if there is suspicion of vascular injury despite the patient being hemodynamically stable and if no “hard signs” (eg, pulsatile bleeding, rapidly expanding hematoma, etc.) of vascular injury should be observed.
Treatment / Management
The initial management of a patient who was the victim of a shark attack usually begins in the pre-hospital setting. It is important to assess the scene for safety and to remove the patient from any area likely to cause further harm to the patient or treating providers. Sometimes, this means moving the patient away from the water on a beach shore. Like all traumatic injuries, initial medical care should assess and stabilize the patient’s airway, breathing, and circulation, which can be performed by the Advanced Trauma Life Support (ATLS) Protocol. Hemorrhage control is a priority. Extremities are the most likely to be injured,[8] and if bleeding control is difficult to achieve, there should be no hesitation to use tourniquets to stop the bleeding as a temporary measure for other stabilizing interventions. Tourniquets should be left in place until the patient can be evaluated by a surgeon who can repair an injured blood vessel. Intravenous lines for fluids and/or blood transfusions should be started as soon as possible. A surgeon must clean or debride these areas in the operating room if there is extensive tissue loss. Hypothermia is often an issue due to time in the water, blood loss, and shock. Wet skin should be dried to avoid further heat loss, and rewarming measures should be initiated as soon as possible without delaying other resuscitative measures.
Isolated wounds can be treated in the emergency department or an outpatient clinic. These wounds need to be cleaned thoroughly to prevent infection. With any wound caused by an animal bite, foreign objects can be retained in the tissue and must be identified for removal.
Thorough wound cleaning plays a crucial role in preventing wound infections. This can begin at the scene using tap water to irrigate the wound. Further irrigation should be performed in the emergency department or the outpatient setting. Careful exploration to find foreign bodies is necessary. Devitalized tissue should undergo debridement and copious irrigation. Although most injuries are minor or superficial, some are more serious and require surgical debridement and repair.[8][9]
There is no consensus for minor wounds regarding the decision for wound closure. The decision on whether or not to close a wound inflicted by a shark should weigh the risk of infection against the potential of poor cosmetic healing. Shared decision-making with an informed, reliable patient can be performed to help make this decision. One documented case in the scientific literature involving a wound inflicted by the teeth of a shark utilized a loose wound closure 24 hours after the injury in conjunction with prophylactic oral antibiotics and scheduled re-evaluations. There was no documented infection related to the wound following this treatment.[10]
Prophylactic antibiotics should be given for all shark bites, even minor ones. The choice of antibiotics should cover for Vibrio species. Fluoroquinolones, third-generation cephalosporins, and doxycycline are highly active against V vulnificus. Staphylococcus and streptococcus coverage should also be considered due to their prevalence in wound infections.[10] As such, a combination regimen of cephalexin, doxycycline, and ciprofloxacin would be appropriate for prophylaxis. For more serious Vibrio infections requiring hospitalization, 1 antibiotic regimen recommended by the Center for Disease Control and Prevention (CDC) is a combination regimen including a 7-14 day course of doxycycline 100mg PO/IV BID and a third-generation cephalosporin (eg, ceftazidime 1–2g IV/IM q8 hours).[10] Antibiotic selection should be tailored based on wound or blood culture results.[11][12][4]
Differential Diagnosis
Due to a shark's large, conspicuous nature, there is rarely any diagnostic uncertainty regarding a shark bite. The patient, EMS personnel, or a bystander often communicates a history of an encounter with the animal. In the case of an unwitnessed shark trauma in which a patient is unable to provide any history due to barriers such as altered mental status, and if unable to obtain collateral history, one must consider trauma from other marine lifeforms. Additionally, a provider should consider the potential complications associated with such traumatic injuries. Though not comprehensive, a starting point is listed below:
- Acute respiratory distress syndrome (ARDS) from submersion/drowning
- Anaphylaxis
- Arterial injury
- Cellulitis
- Compartment syndrome
- Fracture
- Infectious organisms
- Aeromonas (freshwater)
- Chromobacterium
- Edwardsiella
- Erysipelothrix
- Escherichia coli
- Mycobacterium
- Mycoplasma
- Pseudomonas
- Shewanella
- Staphylococcus
- Streptococcus
- Vibrio (saltwater)
- Clostridium tetani (Tetanus)
- Necrotizing fasciitis or myonecrosis
- Nerve Injury
- Osteomyelitis
- Rhabdomyolysis
- Trauma from other marine animals
- Barracuda
- Crocodile
- Giant Groupers
- Octopus
- Jellyfish (Cnidaria)
- Moray eels
- Skates
- Stingray
Prognosis
Most injuries from shark attacks are non-fatal. In 1 review of 86 consecutive cases, the majority (81%) of patients had only minor injuries that required simple sutures. However, patients with more extensive wounds were associated with higher morbidity and rates of limb loss. In the fatal traumas, most deaths occurred as a result of exsanguinating hemorrhage from vascular injury.[2]
Complications
In the acute setting, similar to other penetrating trauma, neurovascular injuries and acute fractures are possible. Inadequate exploration or wound care can lead to a retained foreign body or retained devitalized tissue, leading to infection and further tissue loss and morbidity. Even with proper care and appropriate antibiotic selection, patients can still develop serious wound infections, leading to tissue necrosis, sepsis, and/or limb amputation.
Deterrence and Patient Education
Sharks may bite to eat, protect territory, or as a startle reaction. In general, shark attacks are rare. Recommendations from the Global Shark Attack File that can help decrease the likelihood of shark attacks include:
- Seek advice from local people before engaging in water activities where shark attacks have occurred.
- Remain aware of your surroundings.
- If you suddenly become uneasy while in the water, leave immediately.
- If you see a shark, do not harass or touch it, no matter its size
- If swimming or surfing, do not enter the water when sharks are present and leave the water the water slowly and quietly if they are sighted or if you are requested to do so by a lifeguard or other professional
- Do not swim, surf, or dive alone
- Do not stray far from the shore
- Do not swim at night.
- Avoid swimming in low visibility, such as murky or turbid water.
- Avoid swimming close to river mouths.
- Be cautious when swimming in the breakers.
- Do not swim close to sandbars.
- Be cautious crossing channels between sandbars or on the edge of steep drop-offs.
- Avoid swimming or surfing near jetties.
- Avoid swimming in areas where birds are diving into the water.
- If schools of fish are milling nearby, do not attempt to chase them from the area.
- If baitfish leap at or above the surface, leave the water immediately.
- If spearfishing or collecting shellfish, do not attach your catch to a stringer at your waist, and stay alert when removing a fish from your spear. If wade-fishing, do not carry bait on your person.
- If spearfishing, change locations frequently.
- Avoid areas where fishing occurs, or offal is dumped into the sea.
- The presence of porpoises and dolphins may indicate sharks are hunting in the area.
- Leave the water when pods of dolphin cluster or head inshore
- Avoid swimming, surfing, or diving near pinniped haul-outs or rookeries.
- Avoid high-contrast swimsuits
- Refrain from excess splashing or making quick, abrupt movements in the water.
- Do not swim with dogs or horses.
- If a shark approaches uncomfortably close, keep it at bay with your speargun or a shark billy. Do not attempt to spear the shark unless you think a bite is imminent.
Enhancing Healthcare Team Outcomes
Shark bites are managed with an interprofessional team that includes a general surgeon, vascular surgeon, infectious disease expert, emergency physician, and intensivist. Shark bites are not common, but when they do occur, they are either fatal at the site or the individual suffers serious injury, including amputation of the limb. The management of shark bites is more difficult as many encounters occur at sea away from expert medical assistance. Like any trauma, the priority is to resuscitate the patient with priorities on the airway, breathing, and circulation. Unfortunately, there is a paucity of evidence in the scientific literature to help guide the management of shark-related trauma. Most evidence comes from retrospective cohort studies, chart reviews, extrapolation from basic science studies, or expert opinion.