Continuing Education Activity
Scaphoid fractures are the most common carpal fractures and tend to occur in younger, active individuals. They account for 2% to 7% of all fractures and 60-70% of carpal bone fractures. Scaphoid fractures are not uncommonly missed initially on clinical and radiographic examination. These injuries can be misdiagnosed initially as simple wrist sprain. This misdiagnosis can lead to increased morbidity for the patient as the risks of non-union can be high (14-50% if displaced). If left untreated, arthritis, deformity, and instability invariably develop within five years, leading to a significant disability. As these injuries often happen in young, active patients, the associated morbidity and cost implications secondary to disability are significant. This activity describes the pathophysiology, evaluation, and management of scaphoid fractures and highlights the role of the interprofessional team in the care of affected patients.
Objectives:
- Identify the common mechanisms of injury that lead to scaphoid fractures.
- Summarize appropriate evaluation and examination procedures, including diagnostic imaging, for a suspected scaphoid fracture.
- Describe the appropriate management options for scaphoid fractures.
- Explain how careful planning and discussion among the interprofessional team members will improve outcomes for scaphoid fractures.
Introduction
Scaphoid fractures are the most common carpal fractures and tend to occur in younger, active individuals. They account for 2% to 7% of all fractures and 60% to 70% of carpal bone fractures.[1] Scaphoid fractures are not uncommonly missed initially on clinical and radiographic examination. These injuries can be misdiagnosed initially as a simple wrist sprain.
This misdiagnosis can lead to increased morbidity for the patient as the risks of non-union can be high (14% to 50% if displaced). If left untreated, arthritis, deformity, and instability invariably develop within five years which can lead to significant disability. As these injuries often happen in young, active patients, the associated morbidity and cost implications secondary to disability are significant.
Etiology
Patients typically present with wrist pain following a fall onto an outstretched hand. Axial loading of the wrist in forced hyperextension and radial deviation can cause the fracture as the scaphoid impacts on the dorsal rim of the radius. Contact sports and road traffic accidents are also common causes. Tumors and infections are uncommon causes of pathological scaphoid fractures.
Epidemiology
Scaphoid fractures predominantly affect young adults, with a mean age of 29 years.[2] There is a higher incidence in males. They are unusual in the pediatric population and the elderly population, where the physis or distal radius, respectively, are more likely to fracture first. Scaphoid fractures account for 15% of acute wrist injuries.
Pathophysiology
The scaphoid is the largest of the eight carpal bones.[3] Anatomically, the scaphoid has proximal and distal poles with a waist between the two. Blood supply to the scaphoid bone is predominantly from branches of the radial artery (dorsal carpal branch). These enter the dorsal ridge and supply 80% of the proximal pole via retrograde flow. The second source is from the superficial palmar arch, a branch of the volar radial artery, which enters the distal tubercle and supplies the distal pole. The retrograde nature of the blood supply means that fractures at the waist of the scaphoid leave the proximal pole at high risk of avascular necrosis.[4]
The majority of fractures (approximately 65%) occur at the waist, with a quarter at the proximal third and 10% at the distal third.
The incidence of avascular necrosis carries a strong association with the location of the fracture; the proximal segment has a 100% rate of AVN, reducing to 33% at the distal segment of the scaphoid.
History and Physical
Scaphoid fractures most commonly cause pain and swelling at the base of the thumb in the anatomic snuffbox.
Patients will typically present with wrist pain after a recent history of trauma. Often the patients present late as the injury gets missed on plain radiographs. Pain is often centered on the radial side of the wrist and is worse with movement. There may be associated swelling and a reduced range of wrist motion. It is important to ascertain if the patient is a smoker as this increases the risk of non-union by approximately 20%.[5]
Examination of the wrist should follow the “look, feel, move” pattern. The deformity is unlikely unless there is associated carpus dislocation, for example, perilunate dislocations. It is important to palpate over the distal radius and ulna and metacarpals to assess for any associated injury. Classically, there is tenderness in the anatomic snuffbox dorsally, especially with wrist fractures. The snuffbox is the area between the first and third extensor compartments with abductor pollicis longus and extensor pollicis brevis tendons lying radially, and the extensor pollicis longus tendon lying on the ulnar side. There may also be tenderness over the scaphoid tubercle on the volar aspect, which can be felt as the bony prominence radial to flexor carpi radialis at the level of the distal palmar crease. Tenderness usually presents in one of three locations:
- The volar prominence at the distal wrist for distal pole fractures
- Anatomic snuffbox for waist or mid-body fractures
- Distal to Lister's tubercle for proximal pole fractures
The scaphoid compression test is a more sensitive test and involves placing the examining index finger and thumb over each pole of the scaphoid and compressing. This maneuver is likely to elicit pain in the presence of a fracture. Pain in the anatomic snuffbox on ulnar deviation of the wrist also suggests scaphoid fracture.
Evaluation
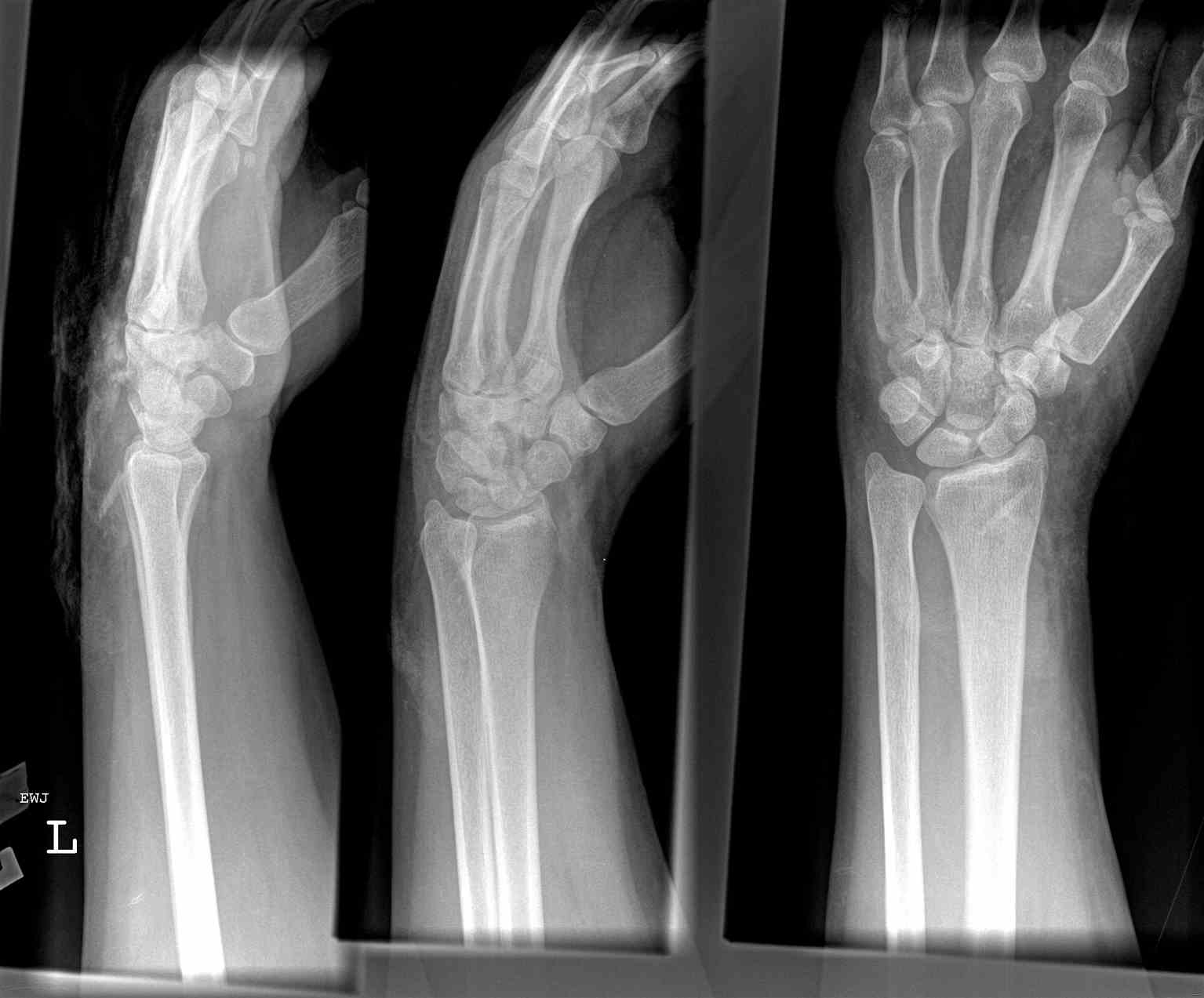
The evaluation begins with PA and lateral views of the wrist alongside scaphoid views, taken with the wrist at approximately 30 degrees of extension and 20 degrees of ulnar deviation. The estimates are that up to 25% of scaphoid fractures are not evident on initial plain radiographs. If high clinical suspicion exists, the wrist should undergo immobilization in a splint or cast for 7-14 days and plain radiographs repeated. If early confirmation is needed, bone scans can be done to diagnose occult fractures at 72 hours post-injury.
Persisting clinical suspicion after negative repeat radiographs warrants Magnetic Resonance Imaging (MRI) or Computed Tomography (CT).[6] MRI is the most sensitive means of diagnosis and can also identify any associated ligamentous injury or bone edema/contusions.[7] A recent meta-analysis estimated 97.7% sensitivity and 99.8% specificity for MRI.[8]
Although CT scan has also high sensitivity and specificity, fractures with less than 1 mm displacement can be missed.
There are no particular laboratory tests, but if surgery is to be done, then routine blood work, including full blood count, urea and electrolytes, clotting screen, and group and save are required.
Treatment / Management
Nonoperative Management
Fractures that are non-displaced and within the distal third of the bone can be managed non-operatively with immobilization in a cast.[9] There is active debate as to whether a long or short arm cast is optimal and whether a thumb spica should be included to immobilize the thumb. Still, there is no evidence currently to suggest whether one option is better than the other.[10]
The cast is usually needed for six weeks with repeat radiographs taken at this time to assess for union. The time to union varies depending on the location of the fracture. The distal third would be expected to heal within 6-8 weeks, the middle third within 8-12 weeks, and the proximal third within 12-24 weeks. The relative increase in time to healing while moving from distal to proximal is secondary to the tenuous blood supply and retrograde arterial flow.
Surgical Fixation
The indications for operative management include:
- Displacement greater than 1mm
- An intrascaphoid angle greater than 35 degrees (humpback deformity)
- A radiolunate angle of more than 15 degrees
- Transcaphoid perilunate dislocation
- Proximal pole fractures
- Comminuted fractures
- Undisplaced waist fractures in individuals that need to return quickly to work/sport
- Nonunion or avascular necrosis
The surgical fixation involves inserting screws or K-wires and can be done percutaneously or via an open procedure. The latter is preferable for non-unions and those fractures that exhibit gross displacement.
Technique
Positioning of the screw is crucial and should be in the middle third of the central axis of the scaphoid; this provides the most stability, reduces time to union, and improves alignment.
Access to the scaphoid can be via a dorsal or volar approach. The decision is made based on the surgeon's preference and the location of the fracture. The volar approach uses the interval between the flexor carpi radialis and the radial artery and is the optimal approach for waist and distal pole fractures. It has the benefits of allowing exposure of the entire scaphoid and radioscapholunate ligament and is least damaging to the vascular supply. The dorsal approach is preferred for proximal pole fractures but places the vascular supply at greater risk of injury.
Nonunion
Treatment of scaphoid non-union is approachable in a variety of ways.[10] Early on in its course, open reduction and internal fixation with bone grafting can be an option. A bone graft can be sourced from the distal radius or the iliac crest.
Alternative treatments include excision of the proximal fragment, total or partial arthrodesis (fusion), radial styloidectomy, or proximal row carpectomy. These are salvage procedures and are usually considered when there is evidence of arthritis of the radio-carpal joint.
Differential Diagnosis
- Distal radius fracture
- Other carpal bone fractures
- Scapholunate dissociation
- De Quervain tenosynovitis
- Osteoarthritis
- Tendonitis
Pertinent Studies and Ongoing Trials
There remains much debate within the literature regarding the management of undisplaced scaphoid waist fracture; whether an early operative intervention has better outcomes compared to conservative management in a cast. There have been numerous systemic reviews exploring this question, but insufficient evidence exists to inform the management of waist fractures adequately.[11][12][13][14][15] Several studies reported earlier return to function following surgery although there was a higher incidence of complications, albeit minor ones.
Toxicity and Adverse Effect Management
Pain can usually be managed according to the WHO pain ladder with paracetamol (acetaminophen), initially alongside non-steroidal anti-inflammatory drugs (NSAIDs), provided there are no contra-indications. If this fails to control the pain, then weak opioids such as codeine can be introduced before progressing to stronger opioids such as morphine. These may be indicated in the initial post-operative period.
Prognosis
Scaphoid fracture with displacement <1 mm has a union rate of 90%. The prognosis worsens if the fracture is displaced, with a missed diagnosis, or if the fracture is in the proximal pole. If left untreated, the risk of chronic pain with associated reduced range of motion and grip strength is more likely to occur.
Complications
Nonunion - This is the most likely complication arising from missed scaphoid fractures. The risk is higher in those that are very displaced or have associated carpal fractures. These will generally require operative intervention with screw fixation. There are three stages:
- Radioscaphoid arthritis
- Scaphocapitate arthritis
- Lunocapitate arthritis
Scaphoid nonunion advanced collapse (SNAC) is the end-stage and is managed with wrist fusion or proximal row carpectomy.
Avascular necrosis - The incidence of this is approximately 30-40%. This is most likely to affect the proximal pole.
Scapholunate Dissociation
Delayed union
Postoperative and Rehabilitation Care
Physiotherapy is a requirement whether the fracture undergoes operative or non-operative management. Physical therapy helps the patient to regain range of motion and wrist strength. In the early stages, swelling predominates, and it is important to keep the hand elevated with active finger, elbow, and shoulder movements encouraged to avoid stiffness. After immobilization (for conservatively managed fractures or post-operatively), the wrist stiffens, and physiotherapy is vital for safely increasing the range of movement. Active range of motion alongside pronation and supination exercises are encouraged once the cast comes off.
Post-operatively, the wrist is usually immobilized initially in a below elbow back-slab and then converted to a full cast at two weeks after wound review and repeating plain film radiographs. They remain in the full cast until six weeks postoperatively, when plain radiographs will be repeated and the cast removed if there are radiological signs of bone healing. A wrist splint for a further six weeks may be indicated to protect the wrist.
Return to sport and driving can usually safely take place from 3 months.
Deterrence and Patient Education
Wrist protection in the form of a removable splint may be of benefit if the patient takes part in high-risk activities where a fall on an outstretched hand may be more likely. Smoking cessation is recommended to optimize fracture healing both for those managed operatively and non-operatively.
Pearls and Other Issues
General practitioners and emergency medicine doctors should be vigilant to scaphoid fractures to ensure that they are not missed and referred appropriately to the orthopedic team. Neglect of injury for over four weeks increases nonunion rates almost tenfold.
Enhancing Healthcare Team Outcomes
Emergency department doctors and general practitioners should work in conjunction with radiologists and orthopedic doctors to minimize the chances of missing these fractures. An interprofessional team approach is vital in managing these fractures, and early physiotherapy and hand therapy involvement of PT/OT will help improve outcomes. The patient should have direct involvement at all stages of discussion and receive proper education regarding conservative versus operative management benefits.