Introduction
Deglutition or swallowing is an innate function. Swallowing sounds like a simple physiological human function, but it is a complex, multifaceted process involving a variety of muscles and nerves. It is the starting point for the peristaltic transport of food to the stomach. Deglutition in humans can be of three distinct phases: oral phase, pharyngeal phase, and esophageal phase, of which the first one is voluntary, and the other two are reflex actions. The oral phase further divides into an oral preparatory phase and an oral propulsive phase. The location of the food bolus defines each of these phases as it descends towards the stomach. The oral and pharyngeal stages of swallowing share anatomy with the respiratory tract, so protection of the airway is of utmost importance. The anatomy of the structures involved in deglutition will be discussed further in this article.[1]
Structure and Function
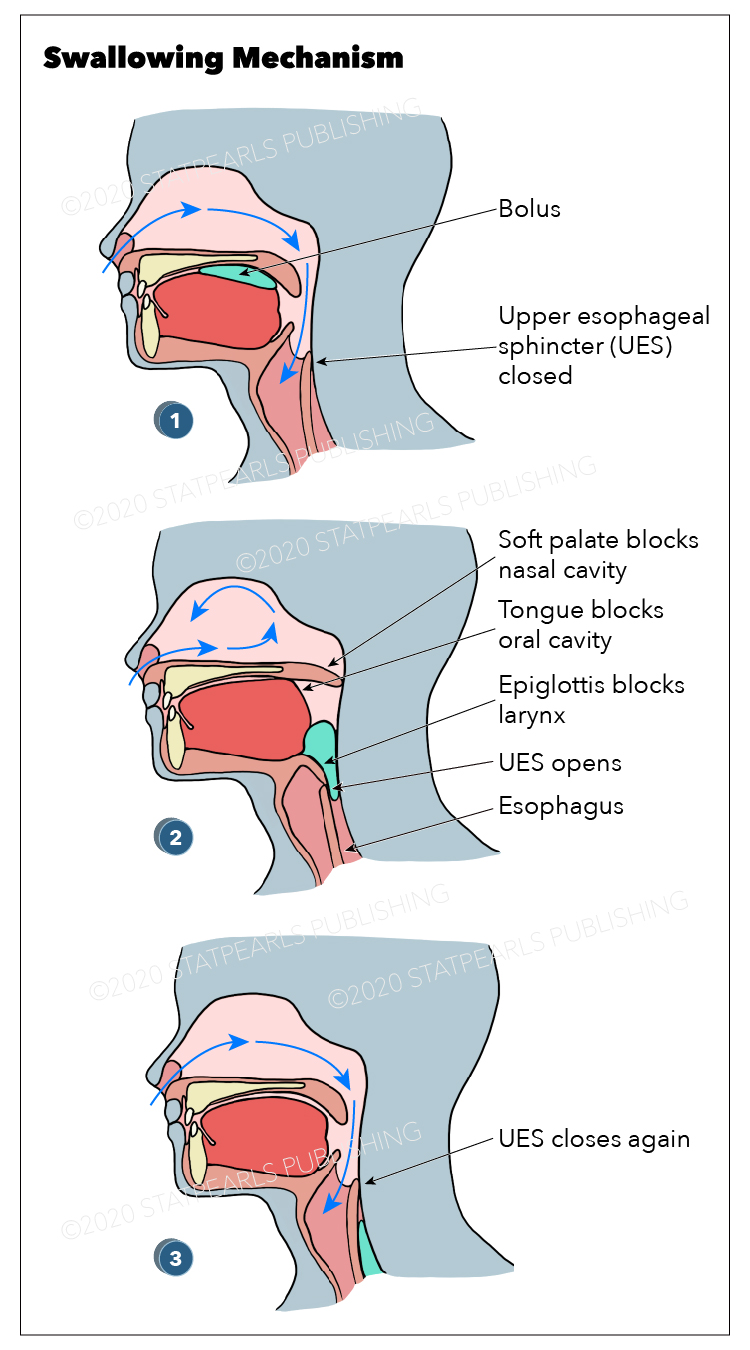
The function of each structure involved in the swallow summarizes into two main themes: propulsion of the bolus toward the stomach and protection of the airway. The oral preparatory stage begins when food or liquid is consumed through diet and enters the oral cavity. When drinking liquids, the posterior tongue rises to meet the soft palate to ensure a proper seal, preventing leakage of liquid oral cavity contents into the oropharynx before the swallow initiates voluntarily. This seal does not form between the palate and tongue during the mastication of solid foods, and therefore free communication between the oral cavity and oropharynx is preserved. Immediately before the initiation of a swallow, the anterior tongue rises to meet the hard palate as the posterior tongue drops and opens the oropharynx. The bolus is then propelled down the palate by the tongue toward the oropharynx; this is the oral propulsive stage. Contrast this with consuming liquids as the pharyngeal stage begins throughout the oral propulsive stage. The first irreversible step in swallowing, the pharyngeal stage, occurs next and is categorized by a rapid phase of muscle contraction to propel the bolus through the upper esophageal sphincter and into the esophagus. This stage starts when the consumed bolus makes its way to the palatoglossal arch.[2] The protection of the airway is essential to this stage and occurs by the induction of a swallowing apnea. This cessation in breathing usually occurs toward the end of expiration and helps prevent the aspiration of consumed material.[3] The vocal folds also adduct, and the glottis closes; the muscles and nerves involved in these steps will be discussed in greater detail later.
Embryology
The structures involved in the physiological act of swallowing develop early in fetal life, around the beginning of week four of embryological development. Around this time, the branchial or pharyngeal arches begin to form and will later give rise to the mature adult structures pertinent to swallowing. These adult structures form via involvements from all three primary germ cell layers and derive from one or more of the six pharyngeal arches, with arch five involuting early in development. The mucosal surfaces lining the pharynx derive from endoderm, the muscles, and bones pertinent to swallowing derive from mesoderm with coordination from the neural crest, and ectoderm gives rise to glands of the mouth, tooth enamel, and the nerves involved in the neural regulation of the sequence.[4][5][6][7]
Blood Supply and Lymphatics
Blood supply and lymphatic drainage of the head and neck is a very complex picture. Lymph node clusters primarily involved in the drainage of structures integral to swallowing are as follows.
The submental group of nodes primarily drain the floor of the oral cavity and the anterior part of the tongue. The submandibular group drains both the hard and soft palates, the mucosa of both cheeks, and contributes to drainage of the mouth and anterior tongue. The upper jugular cluster of nodes drains the parotid gland and receives secondary drainage from the submental and submandibular node clusters, as well as the pharynx and larynx. The middle jugular cluster of nodes directly drains the base of the tongue, hypopharynx, as well as receiving drainage from the upper jugular cluster. The lower jugular group of nodes primarily drains efferent lymphatics from the upper and middle jugular nodes as well as drainage from the hypopharynx. The medial supraclavicular cluster of nodes receives drainage from the lower jugular nodes, as well as the hypopharynx and esophagus. The posterior triangle group of nodes drains the nasopharynx and oropharynx. The anterior compartment of nodes drains the anterior floor of the mouth, the anterior-most part of the tongue, hypopharynx, and cervical esophagus. The retropharyngeal nodes drain the nasopharynx and the soft palate, while the retrostyloid nodes drain just efferent lymph via the nasopharynx.[8][9]
Blood supply to structures found in the head and neck that are integral to human swallowing can be summarized as follows. The tongue receives its blood supply via the lingual artery, which is a branch of the external carotid. The hard palate receives much of its blood supply via the superior alveolar artery as well as contributions from the greater palatine artery, while the soft palate is maintained by branches of the ascending palatine artery, which is a terminal branch of the maxillary artery.[10][11]
Pharyngeal muscles primarily receive their blood supply via the external carotid artery, with the ascending pharyngeal artery branch being of utmost importance. Pharyngeal constrictor muscles receive blood via the inferior thyroid artery and the tonsillar branch of the facial artery, while the salpingopharyngeus and palatopharyngeus muscles receive vascular supply from a branch of the facial artery and maxillary artery.[12][13]
The vascular supply of the esophagus divides segmentally. The inferior thyroid artery supplies the cervical esophagus. The proximal thoracic esophagus is supplied by branches of the bronchial arteries, while the distal thoracic esophagus receives its blood supply via branches directly stemming from the aorta.[14][15]
Nerves
Multiple nerves have been recognized as integral components of the physiological act of swallowing. Coordination by these nerves allows us to masticate, elevate our palate, and propel a food bolus toward and down the esophagus. The primary nerves involved include CN V3, IX, X, XII, the ansa cervicalis, and the recurrent laryngeal nerves. Pharyngeal sensation is achieved chiefly via CN IX. The upper esophagus is innervated by CN X, while the splanchnic plexus and CN X innervate the lower esophagus. The splanchnic plexus keeps the lower esophageal sphincter contracted, while the parasympathetic input via CN X relaxes the lower esophageal sphincter (LES).
Muscles
Swallowing is a highly regulated and coordinated physiological act. Starting in the oral cavity with the tongue, the genioglossus, hyoglossus, and styloglossus are supplied by CN XII while the palatoglossus muscle receives supply from the vagus nerve (CN X). The mylohyoid muscle is also involved and receives its innervation via CN V3. Each of these muscles helps the tongue carry out its wide range of potential movements involved in swallowing and are integral components to the oral stage of swallowing.
Before a food bolus can be propelled toward the pharynx signaling the start of the pharyngeal stage, the muscles of mastication must be recruited to help break down the ingested food. The masseter, temporalis, lateral and medial pterygoid muscles complete this task via innervation from CN V3.
The pharyngeal stage of swallowing utilizes the most muscles with coordination from multiple nerves and nerve plexuses. It starts with the tensor veli palatini (CN V3), which tenses the soft palate — tensing of the soft palate assists the levator veli palatini (CN IX, X, and the pharyngeal plexus) with the elevation of the soft palate to occlude and prevent the entry of ingested food particles into the nasopharynx. The palate must be tense to provide a steady base so that the pharynx may elevate during swallowing. The suprahyoid muscles assist with elevating the hyoid bone during swallowing and include the digastric (CN V3 and VII), stylohyoid (CN VII), geniohyoid (CN XII), and the mylohyoid (CN V3).[16] The infrahyoid muscles, commonly referred to as the strap muscles, function opposite to that of the suprahyoid muscles and act to depress the hyoid bone during swallowing. These muscles include the omohyoid, sternohyoid, and sternothyroid muscles (ansa cervicalis), and the thyrohyoid muscle (CN XII).[17] The longitudinal pharyngeal muscles function to condense and expand the pharynx as well as help elevate the pharynx and larynx during swallowing. These muscles include the stylopharyngeus (CN IX), salpingopharyngeus (CN X), and the palatopharyngeus (CN X).[18] The superior, medial, and inferior pharyngeal constrictor muscles do what their name implies, constrict the pharynx; this is done in a coordinated fashion to help propel the food bolus toward the upper esophageal sphincter (UES). These muscles are innervated by CN X, except for the cricopharyngeus muscle, which is innervated by the recurrent laryngeal nerve and is situated between the pharynx and the esophagus and functions to help with the transfer of the food bolus into the esophagus through the UES.[13] A few muscles of the larynx act to adduct the vocal cords to prevent aspiration and include the lateral, oblique, and transverse cricoarytenoid muscles, all of which are innervated by the recurrent laryngeal nerve. The aryepiglottic muscle, with help from the oblique arytenoid muscle, brings the arytenoid cartilages together and acts to close the epiglottis at the laryngeal inlet, thus preventing food from entering the larynx mitigating the potential for aspiration. The inferior laryngeal nerve innervates the aryepiglottic muscle.[19] The upper third of the esophagus contains striated muscle and the UES under voluntary control. The middle third of the esophagus is a mixture of striated and smooth muscle, while the lower third is made up of smooth muscle and contains the involuntary LES.
Physiologic Variants
Physiological and anatomical variants exist in the general population, and some can impair swallowing, while others do not affect the process at all. A congenital cleft lip and/or palate poses an issue early on in life and can impair the child’s ability to produce a good seal for suckling, as well as impairing velopharyngeal closure which allows the potential for regurgitation into the nasopharynx. Abnormal development of dentition and parts of the oral cavity can make mastication much more difficult for these select patients, and thus swallowing is impaired because the food bolus cannot be effectively broken down. A tracheoesophageal fistula is a condition that can present in many different anatomical variations and can severely disrupt the outcome of what would be normal swallowing if found to be present at birth. Most of these require surgical interventions to correct their defect.[1] Muscles of the mouth and pharynx can be variable regarding their origin and insertions, and this can sometimes cause difficulties swallowing.
Surgical Considerations
Surgical options vary depending on the condition. Patients with achalasia can benefit from a Heller myotomy, where muscle fibers of the overreactive lower esophageal sphincter are cut to help relieve the constant contraction that obstructs food from entering the stomach.[20] A large Zenker diverticulum can cause dysphagia and, when symptomatic, can be removed or treated via an open or laparoscopic approach.[21] Severe cleft lip and palate are normally surgically repaired early in the patient’s life. Strictures and webs of the pharynx or esophagus can be treated endoscopically with serial dilations of the area of narrowing.
Clinical Significance
Difficulty swallowing is a common problem encountered in clinical practice, especially when treating elderly patients. An uncommon acquired condition usually seen in older men is known as a Zenker diverticulum. This condition is considered a false diverticulum, as it only involves the mucosa and submucosa, and is caused by herniation of the esophagus through a muscular defect in the cricopharyngeus muscle. This diverticulum leaves the patient susceptible to dysphagia, halitosis, and aspiration. A Zenker diverticulum is assessable with a barium swallow study. Another condition that requires clinical intervention is esophageal or pharyngeal strictures or webs. These acquired conditions are often related to gastroesophageal reflux and can critically narrow the esophagus or UES, making swallowing difficult. Serial dilations are often necessary to alleviate these strictures. Cancer can also present with signs of dysphagia, and the dysphagia is usually for solid foods, like the dysphagia seen in strictures and webs. Cancer will also present with more severe signs such as blood and weight loss as the cancer is actively dividing. Esophageal motor dysfunctions can occur and include conditions like diffuse esophageal spasms and achalasia. Both of these conditions make it difficult to move food bolus through the esophagus and the stomach.[1] Tests routinely used to evaluate for dysphagia include esophageal manometry studies, barium swallow studies, and esophagogastroduodenoscopy.[22] Symptoms must be present while swallowing to diagnose dysphagia, but when a patient describes a fullness in their esophagus unrelated to swallowing, it confers a diagnosis of globus hystericus, which usually gives evidence toward a functional disorder but can also mean the issue resides within the muscles of the pharynx or upper esophagus.[23]
Other Issues
The act of swallowing can be impaired anywhere from the mouth to the opening of the stomach at the LES. Any pathological process that disrupts the structures involved in swallowing can pose significant clinical dysphagia. If prolonged and not managed early, dysphagia can lead to the consequences of malnutrition. Any lesion that presents near the esophagus and causes esophageal compression can mimic the usual symptoms of dysphagia. Some considerations include an enlarged thyroid gland, a cancer of the mediastinum, an enlarged left atrium, and previous surgery or radiation to that area.[23] Parkinson disease is also frequently associated with swallowing dysfunction due to the loss of dopaminergic neurons responsible for controlling the striated muscles in the oral cavity, pharynx, and esophagus.[24]