Continuing Education Activity
Injuries resulting in instability require immobilization to decrease the likelihood of further damage, protect soft tissues, alleviate pain, and accelerate healing. Instability may result from injury to the bones, joints, or soft tissues, such as fractures, dislocations, strains, or sprains. A splint may be the best initial treatment option for an unstable injury, and it may be the definitive treatment for some injuries. A splint may be loosely defined as an external device employed to immobilize an injury or joint. Splinting materials are most commonly plaster or padded fiberglass. Splinting is not a benign procedure, and care must be taken not to injure the patient further. This activity reviews the general indications, necessary equipment, procedural techniques, and common complications of splinting procedures while highlighting the role of the interprofessional team in caring for patients with unstable musculoskeletal injuries.
Objectives:
- Select patients with acute musculoskeletal injuries that will benefit from the application of an upper or lower extremity splint.
- Employ best practices when applying a splint to the upper or lower extremity.
- Identify and manage the common complications of splinting for musculoskeletal injuries.
- Develop and implement interprofessional team strategies to improve outcomes for patients with acute musculoskeletal injuries who have undergone a splinting procedure.
Introduction
Musculoskeletal injuries are prevalent, and injured patients may present to emergency departments or urgent care, primary care, or specialty clinics. The initial management of an acute traumatic limb injury includes obtaining a comprehensive medical history and performing a physical examination, paying particular attention to the neurovascular status of the affected limb.
Injuries resulting in instability require immobilization to decrease the likelihood of further damage, protect soft tissues, alleviate pain, and accelerate healing. Instability may result from injury to the bones, joints, or musculature. A splint may be the best immediate treatment option for an unstable injury; sometimes, a splint may be the definitive treatment option.[1][2]
A splint is loosely defined as an external device used to immobilize an injury or joint and is most often made out of plaster or fiberglass. Various splinting techniques may be employed, dictated by the location of the injury and the position of immobilization needed. Splinting aims to correct and restore the anatomic length, rotation, and angulation of a specific injury.[2][1][3]
Splinting is not a benign procedure; malpositioning can cause undue pain, malreduction, and skin breakdown. Improper splinting will necessitate replacement. Splint-related soft tissue complications are the second most common iatrogenic cause for referral to plastic surgery.[4] Poor splinting techniques are common, with one study demonstrating inappropriate splinting on 93% of patients.[5] A thorough understanding of the indications, contraindications, and approach to proper splint placement is essential for practitioners that treat patients with acute musculoskeletal injuries.
Anatomy and Physiology
Patient-specific anatomy must be accounted for when fashioning a splint. The splint should be fashioned to restore the anatomic resting joint position, minimizing adverse outcomes. The mainstays of acute immobilization are plaster or fiberglass splints. Prefabricated splints, such as foam splints or braces, may play a role in the immobilization of chronic injuries to provide structural support or pain control but are less commonly used in the acute fracture setting. Plaster is the preferred malleable splinting material to maintain a position-specific reduction, but it is limited by drying time, user experience, and provider-placed mold. Fiberglass splints are lighter, easier to apply, and more porous but are more expensive and provide a less-reliable mold.
The neurovascular status of the injured extremity must be assessed before and after splint placement. Additionally, excess pressure on the soft tissues may decrease the blood flow to the skin surface, causing irritation and necrosis; this is particularly important in areas with bony prominences, such as the elbow, knee, and calcaneus. Additional layers of protection applied during the splinting process are of great importance in these regions.
Upper extremity splints crossing the wrist should maintain neutral wrist dorsiflexion. In pediatric patients with supracondylar elbow fractures, the arm should be cast or splinted in a long arm cast with the elbow flexed between 60 and 90 degrees. The elbow should never be splinted while flexed more than 90 degrees due to the increased risk of Volkman ischemic contracture.[6][7]
Lower extremity splints crossing the ankle joint should maintain the ankle in a neutral resting position without excessive ankle plantarflexion to prevent resultant Achilles flexion contractures.
Excessive splint laxity may permit inappropriate movement of the injury, and, in cases of fractures, this may result in loss of bony reduction. If a splint is a definitive therapy, there must be a stable injury pattern. Fractures that are difficult to reduce, excessively shortened, or comminuted are not candidates for definitive splinting, as they usually require operative intervention. However, unstable injuries may benefit from temporary splinting if definitive operative fixation will be delayed. In these cases, temporary splinting is necessary to avoid further injuries, immobilize the fracture, and promote healing.[8]
Indications
The general indications for splint placement are immobilizing musculoskeletal injuries, supporting healing, and preventing further damage. Clinical situations that may benefit from splinting include but are not limited to:
- Temporary stabilization of acute fractures, sprains, or strains before further evaluation or definitive operative management
- Immobilization of a suspected occult fracture, such as a scaphoid fracture
- Severe soft tissue injuries requiring immobilization and protection from further injury
- Definitive management of specific stable fracture patterns
- Peripheral neuropathy requiring extremity protection
- Partial immobilization for minor soft tissue injuries
- Treatment of joint instability, including dislocation
Contraindications
While no specific contraindications to splinting exist, certain injuries and patient-specific comorbidities require special consideration.
The presence of open wounds or acute injuries that violate the skin requires soft tissue care, which may include tissue debridement or wound closure before splint application. Antibiotic administration should be considered for these patients depending on the severity of the lesion.[9]
Injuries resulting in neurosensory deficits may preclude splint application due to increased risks of compartment syndrome, pressure injuries, or malreduction. Surgical evaluation of these injuries is warranted as neurosensory deficits may indicate a surgical emergency. Patients with peripheral neuropathy may undergo lower extremity splinting on a case-by-case basis. Due to alterations in baseline sensation, patients with peripheral neuropathy have difficulty detecting splint-induced pressure injuries, skin irritation, and vascular compromise.
Acute vascular injuries require a specialized surgical evaluation and potentially emergent definitive treatment. Additionally, the vascular status of an affected limb must be assessed before and after fracture reduction and splint application; reduction maneuvers can result in acute arterial injury or obstruction if a vessel is trapped between bony fragments. Patients with chronic peripheral vascular disease may undergo lower extremity splinting on a case-by-case basis but are at increased risk of complications such as pressure injuries.
Equipment
Splinting may be performed using plaster or fiberglass splinting material. It is imperative that all supplies be assembled before the procedure begins to avoid premature hardening of the splinting material. Supplies required for splinting include:
- Sheet or towel to protect the patient's clothing
- Stockinette or fabric underpadding
- Undercast padding, typically cotton
- Plaster or padded fiberglass
- Wider material is appropriate for upper arm or lower extremity splints
- Narrower material is appropriate for forearm splints
- Water bucket filled with cool water.
- Elastic bandage
- Sling for upper extremity injuries
Personnel
Splints may be applied by any healthcare team member who has received proper training, including physicians, advanced practice providers, medical assistants, technicians, or first responders. Although a sole operator may fashion and place a splint, assistance does ease the process. A second practitioner can gather materials, aid in fracture reduction, and secure the injured limb in position during splint application and molding.
Preparation
All splinting materials should be assembled before splint application to avoid the premature setup of the plaster or fiberglass.
A motor, sensory, and neurovascular examination should be performed and documented before splint application.
Open wounds or soft tissue injuries should be addressed during the preparation phase and may require antibiotics, wound irrigation, debridement, or tissue closure.
The splinting materials should be measured to fit the desired area, precut, and laid out in the order of use. Stockinette should be sized 8 to 10 cm longer than necessary to cover the splinted area. The plaster or fiberglass should also be measured and cut to an appropriate length, spanning the injured area. Plaster should be stacked 8 to 10 sheets thick to ensure adequate strength. Additional layers may be necessary for larger joints or body habitus, and fewer layers may be required for pediatric patients.
Oral or intravenous analgesia may be required. Conscious sedation may be needed for certain patients, particularly children.
Technique or Treatment
Splinting Technique
- Ensure adequate analgesia before splint application to promote muscle relaxation and facilitate fracture reduction.
- Ensure that any soft tissue injuries are addressed before splint placement.
- Apply a stockinette circumferentially to the injured area extending proximal and distal of the splinted region.
- Pad bony prominences such as the elbow, knee, or calcaneus with at least 1 to 2 cm of soft cast padding, as dictated by body habitus.
- Circumferentially apply 2 to 3 layers of cast padding to the remaining area of immobilization.
- Reduce any fracture by restoring the bone length, rotation, and alignment utilizing radiographic confirmation as necessary.
- Activate the splinting material by saturating them in the water bucket. Press the sheets together to laminate them for increased strength and adhesion.
- Mold the splinting material around the injured area to resist any deforming angulation.
- Ensure the splinting material does not circumferentially encase the injured area; overlap should be addressed by cutting the splint once the splinting material has set up.
- Fold the stockinette back over the ends of the splinting material to protect the skin.
- Circumferentially apply an elastic bandage around the splint. This aids in molding the splint material to the injured area and holds the support material in place until it has hardened. Direct placement on the skin should be avoided and is a commonly observed mistake.[10] (see Image. Completed Volar Splint)
- Repeat the neurovascular assessment. Changes in neurovascular status should prompt the rapid removal of the splint and physical reassessment.
Types of Splints
Common upper extremity splints include the coaptation splint, sugar tong splint, posterior long arm elbow splint, ulnar or radial gutter splint, volar or dorsal short arm splint, and thumb spica splint.
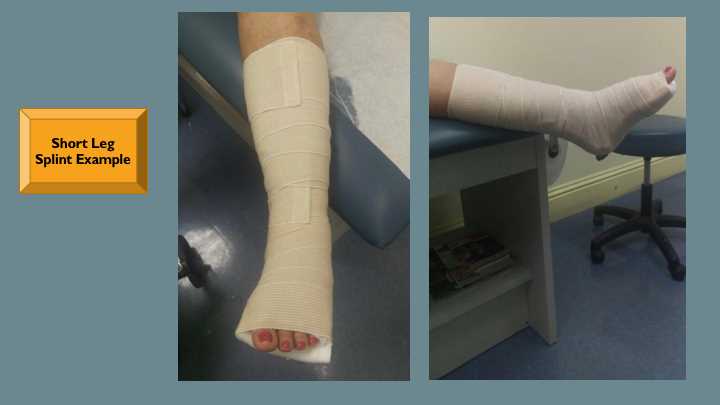
Common lower extremity splints include the posterior short or long leg splints and the posterior short leg splint with stirrups (see Image. Posterior Short Leg Splint).
These specific splinting approaches are well described elsewhere.[11]
Complications
Splints are commonly used but often applied improperly or inadequately.[12] Patients should be given a list of signs and symptoms that prompt a return to a medical professional. Complications of splinting acute musculoskeletal injuries include a loss of fracture reduction, skin irritation or breakdown, and joint stiffness. A properly fitting splint with appropriate underpadding immobilizing the fewest joints possible will minimize these complications.
Thermal injury secondary to the exothermic reactions of the splinting material is possible. Skin burns may be avoided by using cool or room-temperature water during splinting material activation, adequately protecting the skin with stockinette and underpadding, and careful assessment after splint application.
Compartment syndrome and neurovascular compromise are rare but severe complications of splinting. Compartment syndrome is more commonly induced by casting. However, if a splint is circumferential, compartment syndrome can occur. Examples of neurovascular compromise after splinting include acute carpal tunnel syndrome following the reduction and splinting of a wrist dislocation and the occlusion of the brachial artery following the reduction and splinting of a supracondylar humerus fracture. Both scenarios require prompt splint removal and reassessment of the affected extremity.
Clinical Significance
Splints may effectively immobilize injuries, including sprains, fractures, or soft tissue injuries. In specific scenarios, splints may be the definitive management of these injuries. Educating patients regarding splint care and return precautions aids in a successful outcome.
A splint must be differentiated from a cast when determining the best form of immobilization for each clinical scenario. A splint is the noncircumferential application of plaster or fiberglass with a supportive and forgiving structure that accommodates the physiologic swelling common to the acute inflammatory phase. In contrast, a cast is a circumferential application of plaster or fiberglass that rigidly immobilizes a particular joint or fracture. Because of the circumferential nature, casts are rarely placed in the acute setting.[1]
Splinting is not a benign procedure; improper splint application may result in adverse outcomes. One study found that up to 40% of patients splinted in the emergency department developed soft tissue complications, including skin ulceration in 6% of patients.[5] There is still debate whether casting or splinting has a lower complication rate in the immediate postoperative management of pediatric supracondylar fractures.[13][14]
Proper splint placement avoids unnecessary pain, complications, and excess healthcare costs. Careful monitoring for subsequent compartment syndrome, neurovascular compromise, and skin breakdown or necrosis should be performed. Patients who report numbness or tingling in the affected limb, pale skin, or increased pain and swelling should be evaluated immediately for potential complications.
Enhancing Healthcare Team Outcomes
A wide range of medical personnel may apply splints. Regardless of experience, basic knowledge about proper splint application and complications allows teams to work together to care for patients effectively. Articles and videos have been developed to help educate medical personnel about proper splinting techniques. Incorporating an interprofessional approach between orthopedic surgeons, emergency medicine practitioners, and primary care practitioners can significantly improve these skills.[11][15][16] Medical professionals may serve as the primary treating clinician or splinting assistants. Regardless of the role assumed, knowledge about the goals of immobilization and proper splinting techniques will improve patient care.
Following fracture splinting, follow-up care should be coordinated for the patient to ensure improving clinical status. For injuries that do not require specialty care or operative fixation, often this coordination occurs between emergency practitioners or first responders and primary care practitioners. This is particularly relevant in the case of pediatric forearm fractures, where most patients receive follow-up care with primary care practitioners and not orthopedic specialists.[17]
After splinting, patients should be instructed regarding proper splint care, including keeping the splint clean and dry and elevating the injured extremity to minimize swelling. Strict return precautions include getting the splint wet and changes in neurovascular status. Patients whose injuries will be managed exclusively with a splint require follow-up care 1 to 2 weeks after initial splint placement. Further evaluation may include radiographic imaging, a splint change, or conversion to a cast.
In the setting of multiple traumas, periarticular or open fractures, and any fracture with significant displacement, rotation, or malalignment requires coordination with an orthopedic surgeon, as these patients have an increased risk of adverse events.