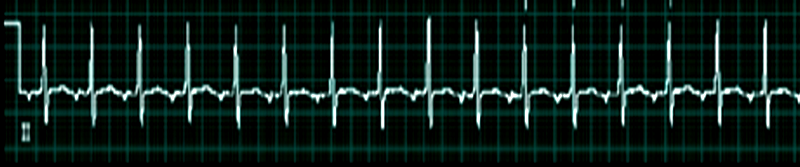
Continuing Education Activity
A focal atrial tachycardia is an arrhythmia with electrical impulses originating and confined within the atria. Focal tachycardia typically occurs in the setting of increased metabolic demand and stress, like infection, hypoxia, etc. Focal atrial tachycardia generally is a benign arrhythmia. In hemodynamically stable patients, management of this arrhythmia focuses on the treatment of underlying conditions. That said, focal atrial tachycardia requires differentiation from other atrial arrhythmias, like atrial fibrillation and atrial flutter. Appropriate diagnosis of focal atrial tachycardia must be made to guide proper management. This activity reviews the evaluation and treatment of focal atrial tachycardia and highlights the role of the interprofessional team in evaluating and treating patients with this condition.
Objectives:
- Identify the etiology of focal atrial tachycardias.
- Describe the evaluation of focal atrial tachycardias.
- Summarize the treatment and management options available for focal atrial tachycardias.
- Explain interprofessional team strategies for improving care coordination and communication to advance focal atrial tachycardia and improve outcomes.
Introduction
Atrial tachycardia is an arrhythmia with electrical impulses originating within the atria. Atrial tachycardia can be a result of one or a combination of the mechanisms leading to arrhythmia: automatic, triggered activity, or reentry. In some cases, the mechanism remains undetermined.[1] Electrophysiologic features may overlap if there is a small reentrant circuit, as in micro-reentry. It is useful to categorize atrial tachycardia in two broad groups: macroreentrant or focal.
The prototypic macroreentrant atrial tachycardia is an atrial flutter. Typical atrial flutter arises from the right atrium in a circuit bound anteriorly by the tricuspid annulus and posteriorly by the crista terminalis and Eustachian ridge.[2] The electrical activity can travel in a clockwise or counterclockwise direction in this circuit.
Atrial flutter is a complex arrhythmia with different management than focal atrial tachycardias. As such, the focus of this activity will be on focal atrial tachycardia (FAT).
Etiology
Atrial tachycardia tends to occur in individuals with structural heart disease, with or without heart failure, and ischemic coronary artery disease. However, focal atrial tachycardia often occurs in healthy individuals without structural heart disease. Other possible etiologies are listed below:
- Hypoxia
- Pulmonary disease
- Ischemic heart disease
- Stimulants: cocaine, caffeine, chocolate, ephedra
- Alcohol
- Metabolic disturbances
- Digoxin toxicity
- Heightened sympathetic tone
Epidemiology
The prevalence of focal atrial tachycardia is not well known. A European study of young males applying for pilot licenses demonstrated that 0.34% had symptomatic atrial tachycardia and 0.46% had symptomatic atrial tachycardia.[3] A study noted 10 to 15% of patients presenting for supraventricular tachycardia ablation had atrial tachycardia.[4]
Pathophysiology
Focal atrial tachycardias can arise from any or a combination of the three mechanisms causing tachyarrhythmias: enhanced automaticity, triggered, or reentry.[4] Reentry is typically the underlying mechanism in macro-reentrant atrial tachycardias like atrial flutter. If a reentrant mechanism is involved in a focal atrial tachycardia, it involves a micro-reentrant circuit which can be difficult to distinguish from an automatic focus on surface ECG.[5] Reentry involves adjacent substrate with different electrophysiologic properties. In a simplified version; tissue type A must have both different conduction velocity and rate of repolarization (electrical recovery) from tissue type B. As electricity propagates through types A and B at different rates, an early electrical stimulus may encounter type A recovered and type B refractory. The signal then transverses through type A and subsequently finds type B recovered, establishing a reentrant circuit. Reentry may be readily induced during an electrophysiology study.
Focal atrial tachycardia often occurs as a result of abnormal automaticity and are challenging to initiate during an electrophysiology study and require drug infusion to induce.[6] Abnormal automaticity arises from spontaneous phase 4 depolarization.
During phase 4, the cardiac myocyte membrane is polarized and at baseline. The inwardly rectifying potassium channel is responsible for maintaining baseline resting potential near potassium equilibrium.
Abnormal automaticity occurs as a result of accelerated phase 4 upslope, leading to spontaneously depolarizing cells. When the cell experiences further hyperpolarization, and more negative than -70 mV, automaticity may occur via the "funny" current, carried by sodium and potassium ions in sinoatrial, AV nodal, and His-Purkinje cells.[7]
The triggered activity has features seen with enhanced automaticity, though are felt to primarily involve calcium channels. Similar to reentry, triggered activity is inducible during an electrophysiology study.
History and Physical
A detailed history and physical are necessary for every patient, which should include home medications, as well as past medical and surgical history. Also, a social history which should consist of past or present tobacco use, alcohol use, and if the patient consumes caffeine, illicit drugs, or stimulants. A past medical history significant for chronic lung disease, pulmonary hypertension, or other conditions can predispose the patient to atrial tachycardia. Chronic alcohol use or withdrawal can also be associated with atrial tachycardia. Cardiac surgeries can lead to atrial tissue scarring that may be arrhythmogenic.
Patients can present with atrial tachycardias in various ways. Atrial tachycardia can present on telemetry of patients who may be asymptomatic or asleep. As focal atrial tachycardias tend to occur secondary to an underlying disease process, the patient presentation will reflect primary chief complaints.[8]
Patients with atrial tachycardia may complain of palpitations or sensations of fast heart rate, lightheadedness, chest pain or pressure, or shortness of breath. Symptom intensity will be related to the rate as well as the patient’s cardiovascular status. The patient may complain of irregular heart rate if the patient’s tachycardia is sufficient to produce an intermittent AV block.
Symptoms may occur in paroxysms or can be persistent. Symptoms may be related to the consumption of caffeinated products (including coffee, tea, energy drinks or chocolate) or stimulants like ephedrine. Symptoms can also be initiated or exacerbated by stress and exercise. Adenosine administration may cause transient AV block, but does not terminate focal atrial tachycardia.
Persistent focal atrial tachycardia can result in cardiomyopathy, which may lead to symptoms of dyspnea with exertion, increased lower extremity edema, and chest pain. Although the clinical course is typically benign, there is some risk of sudden cardiac death.[9]
The physical exam can demonstrate regular or irregular tachycardia with a heart rate greater than 100 BPM. If the patient’s atrial tachycardia includes a variable block, the intensity of S1 may vary from beat to beat. Excessive A waves may be present on observation of the jugular venous pulse.
Evaluation
EKG can aid the diagnosis of focal atrial tachycardia. EKG features may also inform the origin of focal atrial tachycardias.[10] Electrocardiographic features include:
- Atrial rate: 100 to 250 BPM
- Ventricular conduction can be variable
- Irregular or irregularly irregular in the setting of variable AV block
- Regular if 1 to 1, 2 to 1, or 4 to 1 AV block
- P wave morphology
- Unifocal, but similar in morphology to each other
- Might be inverted
- Differs from normal sinus P wave
- May exhibit either long RP or short PR intervals
- Rhythm may be paroxysmal or sustained
- May demonstrate an increase in the rate at initiation (i.e., “warm up,” or “rev up”)
- May demonstrate a decrease in the rate at termination (i.e., “cool down”)
Treatment / Management
Initial management of focal atrial tachycardia should focus on addressing underlying causes: treating acute illness, cessation of stimulants, stress reduction, appropriately managing digoxin toxicity, or chronic disease management. The ventricular rate is controllable with the use of beta blockers or calcium channel blockers. If atrial tachyarrhythmia persists and the patient is symptomatic, the patient may benefit from class IA, IC, or class III antiarrhythmics.[11] Of course, risks and benefits of using antiarrhythmic medications should be considered, especially in patients with ischemic or structural heart disease. Catheter ablation of focal atrial tachycardia may be appropriate in patients failing medical therapy.[12],[11]. As the driver of many focal atrial tachycardias is by enhanced automaticity, electrical cardioversion without concurrent medical therapy as listed previously will likely result in arrhythmia recurrence.
Differential Diagnosis
Focal atrial tachycardia may be challenging to distinguish from other regular, narrow complex tachycardias.[13] Furthermore, atrial tachycardias may demonstrate some irregularity during “warm-up” and “warm-down” phases, which may further prove difficult to differentiate. Atrial tachycardia is associated with a narrow complex QRS in the absence of aberrant conduction to the ventricles or bundle branch blocks.
As the management of focal atrial tachycardia differs from other narrow complex regular tachycardias, distinguishing focal atrial tachycardia from other supraventricular tachyarrhythmias is important. Below is a differential of similar appearing arrhythmias with their identifying features.
Narrow complex, regular tachycardias
- Sinus tachycardia
- P wave with superior axis
- Atrial flutter
- Biphasic, sawtooth appearing F wave
- Difficult to identify isoelectric, baseline PR segment
- Typical atrial flutter
- Involves circuit around the tricuspid annulus
- Counterclockwise flutter produces F waves that are negative in lead II and positive in lead V1
- Clockwise flutter produces F waves that are positive in lead II and negative in lead V1
- Atypical atrial flutter
- Involves circuit around the scar, left atrium, otherwise non-cavotricuspid isthmus dependent
- AVNRT
- Typical, slow-fast AVNRT
- Short RP interval
- P wave may be absent or within the S wave
- Atypical, fast-slow AVNRT
- Long RP interval
- P wave negative before QRS
- AVRT
- Baseline EKG may demonstrate pre-excitation
- P wave, PR interval, QRS are variable depending on accessory pathway location and conduction direction
- Orthodromic (propagation proceeds down AV node, His bundle, Purkinje fibers, retrograde through accessory pathway and back to AV node)
- QRS width: Narrow
- RP interval: Long
- Antidromic (propagation proceeds through the accessory pathway, and then retrogradely through the Purkinje system, to His bundle, through the AV node and back through accessory pathway)
- QRS width: Wide
- RP interval: Short
- Atrial tachycardia (Focal)
- Junctional tachycardia
- P wave may be absent or inverted
- If retrograde VA conduction, inverted P wave may occur just before or after the QRS complex
Narrow complex, irregular tachycardia
- Atrial fibrillation
- Irregularly irregular rhythm
- Atrial flutter, atrial tachycardia with variable AV block
- Has features of atrial flutter or atrial tachycardia, although variable block leads to irregular rhythm
- Multifocal atrial tachycardia
- P wave morphology with greater than or equal to 3 distinct morphologies
Prognosis
Focal atrial tachycardia is a benign rhythm. Overall prognosis depends on conditions precipitating this arrhythmia. However, if atrial tachycardia persists, it can lead to tachycardia-induced cardiomyopathies over time.[14] If there is a concern for a high burden of tachyarrhythmias, patients should undergo monitoring as an outpatient with a Holter monitor or outpatient/mobile telemetry. Medications should be adjusted as described above.
Deterrence and Patient Education
Risk factors for arrhythmia are similar to risk factors for developing heart disease. A heart-healthy lifestyle with a well-balanced diet, exercising and refraining from tobacco products is essential for prevention. Focal atrial tachycardia persistence can be mitigated by the avoidance of caffeinated products and other stimulant substances.[15]
Atrial tachycardia can produce symptoms such as palpitations, lightheadedness, and pre-syncope, which can understandably generate anxiety. It is therefore essential to convey to patients that although atrial tachycardia can be bothersome, it is not a lethal arrhythmia.
Pearls and Other Issues
- Overall, focal atrial tachycardia is a benign arrhythmia.
- Focal atrial tachycardia typically occurs secondary to an underlying disease process or acute illness.
- Focal atrial tachycardia is one form of atrial tachycardia. Atrial activation patterns in focal atrial tachycardia will be similar during the tachycardia, yet distinct from the normal sinus P wave. Focal atrial tachycardia can be regular or irregular if variable block exists. A “warm up” and “cool down” pattern can occur during initiation and termination, respectively.
- Patients can be asymptomatic or present with palpitations, chest pain, lightheadedness, dizziness, or presyncope. Focal atrial tachycardia often presents on telemetry on asymptomatic or sleeping patients.
- Ventricular rate control is achievable with calcium channel or beta blockers. If the patient remains persistently tachycardic or has uncontrolled symptoms, the patient may benefit from antiarrhythmic therapy with class IC or III antiarrhythmics.
- A possible significant cardiac sequella of prolonged atrial tachycardia (or any tachycardia) is tachycardia-induced cardiomyopathy. If there are concerns for high tachycardia burden, outpatient monitoring may be necessary.
Enhancing Healthcare Team Outcomes
Diagnosis of atrial arrhythmias is reliant on detection. Cardiac telemetry must be used judiciously and appropriately monitored. Healthcare professionals should understand the indications for initiating and discontinuing cardiac telemetry. Appropriate personnel should monitor telemetry and obtain 12-lead ECG’s to aid in the diagnosis of dysrhythmia when they occur.
Proper management of atrial tachycardia requires an interprofessional team approach, including physicians, specialists, specialty-trained nurses, and pharmacists, all collaborating across disciplines to achieve optimal patient results. [Level V]