Continuing Education Activity
A fetal echogenic bowel is defined as an increased echogenicity of the fetal bowel, which is noted on the prenatal ultrasound. In the third trimester, this can be a normal finding representing meconium in the bowel of the fetus. However, when fetal echogenic bowel is detected in the second trimester, it can be associated with several fetal disorders. This activity reviews the incidence, pathophysiology, and outcomes related to fetal echogenic bowel and highlights the role of the interprofessional team in the investigation and management of pregnancies with this finding in the second trimester.
Objectives:
- Describe the pathophysiology of fetal echogenic bowel.
- Review the diagnostic criteria for fetal echogenic bowel.
- Outline various perinatal conditions associated with fetal echogenic bowel.
- Summarize the prenatal and the postnatal management of fetal echogenic bowel.
Introduction
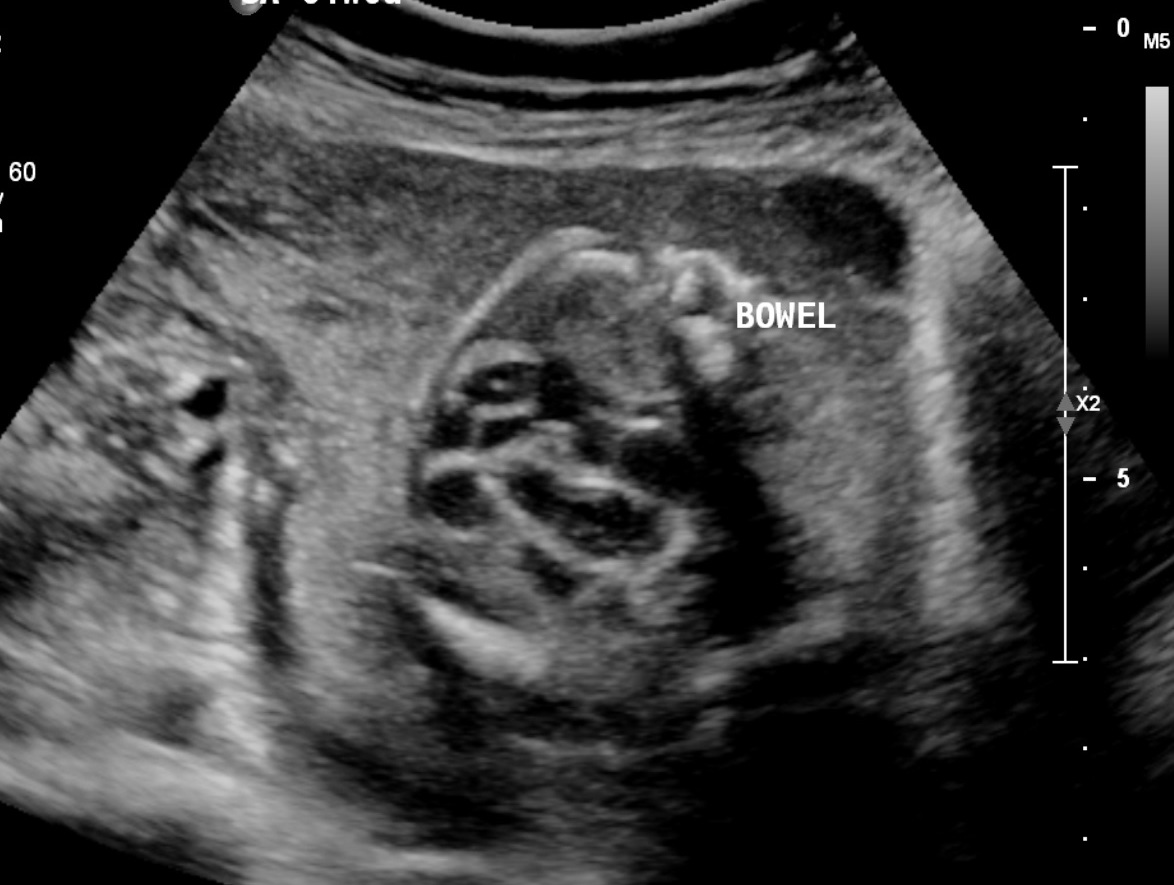
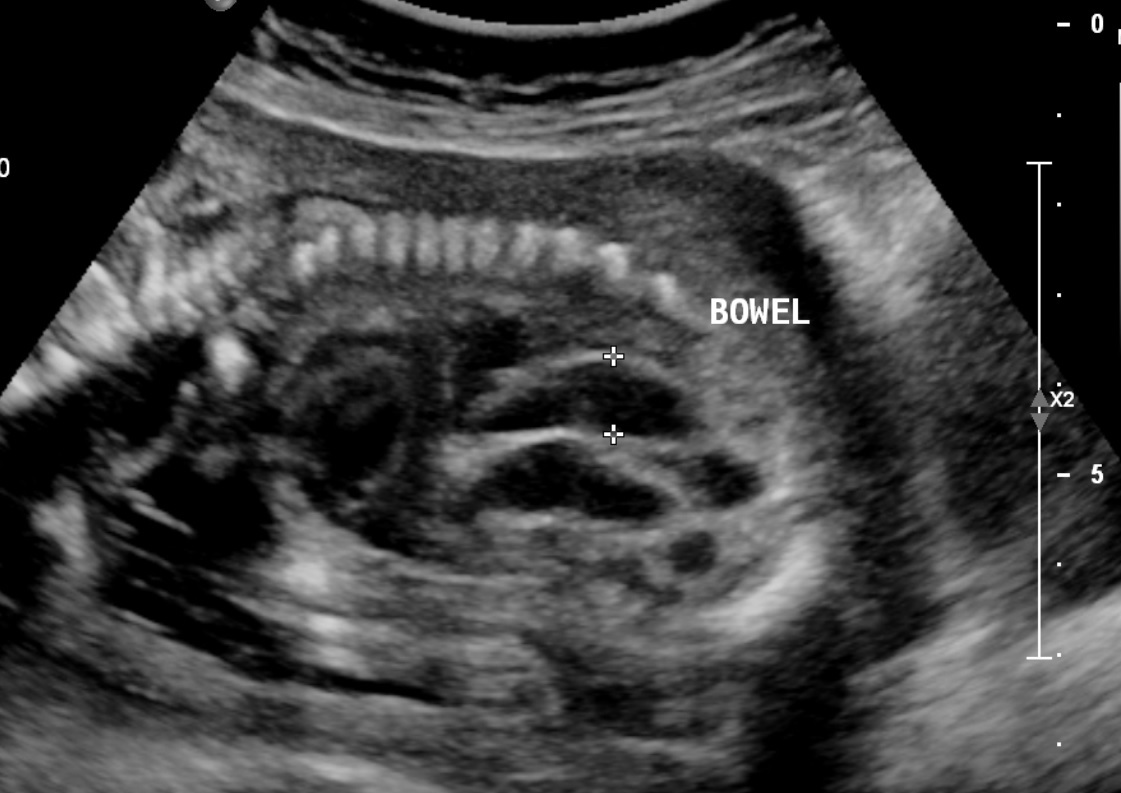
Fetal echogenic bowel is one of the soft markers detected on the prenatal ultrasound. Fetal echogenic bowel is defined as an increased echogenicity of the fetal bowel, which is noted on the prenatal ultrasound. It can be detected in the fetal ultrasound as a hyperechoic and well-defined area in the lower abdomen of the fetus. An associated focus of shadowing may suggest calcification. In the third trimester, this can be a normal finding representing meconium in the bowel of the fetus. However, when fetal echogenic bowel is detected in the second trimester, it can be associated with several fetal disorders.
Typically, the echogenicity is compared with the surrounding fetal iliac bone, although it can also be compared with the fetal lung or liver.[1][2] Fetal echogenic bowel can occur as focal, multifocal, or diffuse.
The most widely accepted grading system for fetal echogenic bowel compares the echogenicity of the fetal bowel with that of the fetal iliac crest. This classification was developed by Slotnick et al.[1] It is outlined as follows:
- Grade 1: mildly increased- less echogenic compared to the bone
- Grade 2: moderately increased- the same echogenicity as the bone
- Grade 3: pronounced increased- more echogenic than the bone.
The grading system is dependent on the subjective assessment of the sonologist and thus can be associated with significant inter and intra-observer variability. Furthermore, the transducer frequency and grading can affect this scoring. With the advancement of technology and the availability of high-frequency transducers, echogenic findings can be exaggerated, leading to an overdiagnosis of the fetal echogenic bowel.[3] Hence, the recommendation is to use a lower frequency transducer (<5 MHz) at a lower gain setting.[4]
Etiology
Fetal echogenic bowel was initially described as a normal variant and a transient fetal finding. The majority of fetuses with an isolated echogenic bowel have normal short-term and long-term neonatal outcomes.[5][6]
Later, fetal echogenic bowel was reported to be a perinatal ultrasonographic marker for conditions such as cystic fibrosis and trisomy 21. Currently, echogenic bowel has been found to be associated with chromosomal abnormalities (trisomy 21, 13, 18), cystic fibrosis, congenital infection (TORCH), intrauterine growth restriction (IUGR), gastrointestinal malformations (gastric obstruction, atresia, perforation, meconium ileus), placental insufficiency as well as intrauterine and neonatal death.[7][8] The incidence of these associations varies considerably among various studies.[9]
Epidemiology
The incidence of echogenic bowel varies from 0.2 to 1.8 % in the prenatal sonogram performed in the second trimester.[10] The variability in the incidence between different studies could be attributed to the high-risk population in some samples.
This variability could also be attributed to the fact that the detection of echogenic bowel is prone to significant inter-observer variability since the diagnostic criteria are based on a subjective assessment which is prone to over or underestimation of the finding based on the level of expertise of the sonographer as well as the frequency and the gain settings of the ultrasound machine.[11]
Pathophysiology
The pathophysiology of the echogenic bowel is speculative and has not yet been fully established. The fetus begins to swallow amniotic fluid by the end of the first trimester, which transits through the intestines. When this passage is slow or obstructed, contents in the bowel can become progressively thick and lead to a bright appearance in the ultrasound. The pathophysiology can vary depending on the underlying etiology. The primary mechanism may involve meconium stasis, or hypercellular meconium can occur for several reasons.[11] These include the following:
Meconium Stasis
- Hypoperistalsis
- Distal obstruction of the bowel
- Meconium ileus
- Fetal Intestinal ischemia
- Fetal Intestinal perforation
Hypercellular Meconium
- Abnormal enzyme secretion
- Proximal obstruction of the bowel
- Feto-placental bleeding into the amniotic fluid
- Intrauterine transfusions
Meconium Stasis
Infants with abnormal karyotypes can have decreased levels of microvillar enzymes leading to hypoperistalsis and further impeding the passage of meconium in utero. This meconium can be inspissated, especially in the second trimester when the bowel lumens are small. As the pregnancy progresses, the amount of fetal swallowing of amniotic fluid increases, as does the small bowel volume resulting in the resolution of meconium stasis and, in turn, leads to the resolution of the hyperechogenic appearance of the bowel.[12]
The pathophysiology of the association between the echogenic bowel and TORCH infection is also thought to be a result of the direct viral-induced cytotoxic effect and ischemia of the endothelial cells in the fetal bowel leading to hypoperistalsis, ileus, or fetal intestinal perforation.[13]
Proximal bowel obstruction can interfere with normal amniotic fluid swallowing and lead to decreased fluid content in meconium which subsequently leads to the formation of meconium plugs which can be identified as increased echogenicity.[14]
Hypercellular Meconium
Conditions such as cystic fibrosis can lead to abnormality in the enzyme secretion leading to abnormal consistency of the meconium, which is usually detected as diffusely increased echogenicity of the bowel along with bowel dilatation and calcification.[15]
Swallowed blood products due to maternal-fetal hemorrhage or intrauterine transfusions can also lead to hypercellular meconium and the finding of echogenic bowel.[14]
Other possibilities, such as compromised placental and fetal perfusion leading to the redistribution of blood flow and, subsequently, gut ischemia, have been postulated.[16]
History and Physical
History and physical exam can be useful in differentiating various pathologies associated with fetal echogenic bowel. Prenatal history should focus on additional pregnancy risk factors (advanced maternal age, gestational diabetes, fetal growth restriction, polyhydramnios), other major and minor fetal anomalies, results of prior imaging and screening tests, past medical history, and comorbidities.[10]
The postnatal examination should focus on detecting any congenital anomalies. A thorough abdominal exam can give clues such as palpable loops indicating bowel obstruction. The patency of the gastrointestinal tract should be confirmed.
Evaluation
A pragmatic approach should be adopted while investigating pregnancies with the finding of fetal echogenic bowel in the second trimester.[7] Risk stratification should be done based on grading and additional risk factors. Further evaluation should be offered, and an interdisciplinary team, including a genetic counselor, neonatologist, and maternal-fetal medicine, should be involved.
A detailed ultrasound evaluation should be performed to assess for additional markers or features suggesting chromosome abnormalities (e.g., nuchal translucency, cardiac anomalies). Further genetic screening, including cell-free fetal DNA testing or a quad screen, should be offered. In pregnancies with additional risk factors (high risk based on risk stratification, other soft markers, positive screening testing), amniocentesis and chromosomal microarray analysis may be offered.
Serological testing for infections such as toxoplasmosis and cytomegalovirus helps detect recent or past infections. Cystic fibrosis screening should be performed if not already done as a part of routine screening.
Serial sonographic monitoring is important even in pregnancies with normal screening test results to detect the progression as well as additional abnormalities. For example, in cases of intestinal obstruction, fetal echogenic bowel may be the initial sonographic finding. On serial sonographic screening, other markers such as dilated bowel loops and abnormal peristalsis will be detected.
Treatment / Management
Diagnosis of echogenic bowel in the second-trimester warrants thorough antenatal and postnatal follow-up due to the increased risk of fetal abnormalities.
Prenatal Management
A detailed sonographic assessment should be performed to assess for additional markers of aneuploidies. Even in the absence of additional markers, it is reasonable to offer cfDNA or quad screen.[17] In cases with additional markers, invasive diagnostic procedures such as amniocentesis should be offered.[18]
Assessment of amniotic fluid is also helpful in detecting maternal-fetal hemorrhage as a cause of the echogenic bowel. Screening for conditions such as cystic fibrosis using parental career screening and serological testing for TORCH infections should be considered.[4]
Serial sonographic screening throughout the pregnancy is recommended for reassessment and to monitor associated conditions such as IUGR, bowel dilatation, and polyhydramnios which are shown to be associated with adverse outcomes.[14]
Postnatal Management
The Association of gastrointestinal abnormalities and other comorbidities in infants with a diagnosis of fetal echogenic bowel highlights the need for these deliveries to be referred to a center with a higher neonatal intensive care unit with pediatric subspecialty services. Postnatally, a thorough clinical examination of the infant must be performed. Abdominal X-ray, UGI series, barium, or gastrograffin enema may be required to evaluate for intestinal obstruction.[19]
Passage of meconium and normal feeding pattern should be ensured. In certain cases, testing for congenital infection, CF screening, and karyotyping may be warranted.
Differential Diagnosis
Fetal echogenic bowel is considered a soft marker and, when detected in a prenatal ultrasound, should prompt further evaluation to detect additional abnormalities. As discussed above, multiple etiologies can lead to the finding of echogenic bowel.
The following differentials should be considered while evaluating fetal echogenic bowel:
- Increased cellularity or thick meconium (intestinal obstruction, cystic fibrosis, chromosomal abnormality)
- Fetal swallowing of blood (fetoplacental hemorrhage, bleeding into the amniotic fluid, placental abruption)
- Inflammation of the bowel (TORCH infection)
- Decreased blood flow in the bowel (fetal growth restriction, fetoplacental insufficiency)
- False-positive (frequency and gain settings of the ultrasound machine, expertise of the sonologist)
It may be possible to differentiate these based on additional clues to the underlying etiology. For example, additional abnormalities like a congenital heart defect or a thick nuchal cord may point towards aneuploidies, features of fetal ascites or hydrops may point towards an infective etiology, whereas thickened dilated bowel wall associated with obstruction or calcification may indicate cystic fibrosis.[19]
Prognosis
The prognosis of Echogenic bowel depends upon the underlying pathophysiology.[20] Isolated echogenic bowel can be a benign finding with normal neonatal outcomes. However, outcomes can be impacted when the fetal echogenic bowel is associated with other ultrasonographic markers or pregnancy complications.
Pregnancies complicated by fetal echogenic bowel and associated with other anomalies, fetal growth restriction, elevated alpha-fetoprotein (AFP), or progressive worsening in grading are associated with less favorable to poor outcomes.[10]
Complications
As the pathophysiology of fetal echogenic bowel is multifactorial, complications are mainly attributed to the underlying pathology. In pregnancies associated with IUGR or elevated AFP, complications may arise from underlying placental-fetal bleeding or congenital anomalies.
The association between echogenic bowel and Intrauterine fetal death (IUFD) may be related to underlying uteroplacental insufficiency.[21]
Consultations
Management of the echogenic bowel requires a multidisciplinary approach with the involvement of the following specialties:
- Maternal-fetal medicine
- Neonatology
- Pediatric surgery
- Clinical genetics
- Radiology
- Pediatric gastroenterology
- Pediatric infectious disease
Deterrence and Patient Education
Mothers diagnosed with fetal echogenic bowel should receive counseling regarding the importance of serial sonographic evaluations. In the presence of additional anomalies, genetic workup should be encouraged.
Enhancing Healthcare Team Outcomes
Fetal echogenic bowel is an uncommon but significant finding in second-trimester ultrasound and requires further sonographic screening. A well-structured grading system suggested by Slotnick et al. should be used while reporting the finding to reduce the diagnostic subjectivity.[1]
Pathophysiology of the fetal echogenic bowel is speculative and depends on the underlying etiology. Examination of the meconium and histologic evaluation of the small bowel from the terminated fetuses with fetal echogenic bowel may provide further answers to the underlying pathophysiology.
Given the broad differential diagnosis, further screening should be offered to identify the underlying etiology. Providers must counsel parents counseling should be done promptly to understand the implications of this finding. A shared decision-making framework between the medical team and the parent is necessary while considering further screening and diagnostic tests.[4]
In fetuses with normal screening, the finding of echogenic bowel may pose a significant dilemma for antenatal counseling. Fetal MRI may be a consideration in high-risk cases.