Continuing Education Activity
Body diaphragms are conventionally considered to be those anatomical structures that occupy a horizontal space. In reality, considering the three-dimensionality of the human body, it is preferable to consider them as areas in close anatomical continuity, able to influence each other: tentorium cerebelli, tongue, thoracic outlet, diaphragm, and pelvic floor. This activity covers the osteopathic manual approach to the 5 diaphragms and describes how to evaluate and then treat the tentorium cerebelli, the tongue, the thoracic outlet, the respiratory diaphragm, and the pelvic floor, using a non-binding sequence.
Objectives:
- Review the anatomical and neurological connections of the 5 diaphragms in the osteopathic field.
- Identify the best treatment strategy with 5 diaphragms.
- Summarize the clinical picture associated with the 5 diaphragms to allow the clinician a practical reflection to identify the correct treatment strategies.
- Outline some interprofessional strategies that can improve patient outcomes when using the osteopathic 5 diaphragms procedure.
Introduction
Assessment and treatment of the five diaphragms fit into the respiratory-circulatory model of osteopathic medicine (OM). Body diaphragms are conventionally considered to be those anatomical structures that occupy a horizontal space. In reality, considering the three-dimensionality of the human body, it is preferable to consider them as areas in close anatomical continuity, able to influence each other: tentorium cerebelli, tongue, thoracic outlet, diaphragm, and pelvic floor. This activity reviews the anatomical connections of these body areas, how they are evaluated, and how they should be manually treated, with a view to possible clinical pictures.
The osteopath's goal is to create space between the different anatomical structures (it is not possible to reshape the same structures manually), as space encloses the possibility of movement. To paraphrase Leonardo da Vinci; space is life.
Anatomy and Physiology
Osteopathic medicine (OM) was founded in America by the ideas and studies of Dr. A. T. Still in the late 1800s. The evaluation approach and manual treatment can be developed starting from the five osteopathic models: biomechanical-structural; respiratory-circulatory; neurological; metabolic-nutritional; behavioral-biopsychosocial. These models are not a constraint but a starting point; osteopathic models must always be integrated. The five diaphragms are part of the respiratory-circulatory model, where the focus is on improving the circulation of body fluids to improve the patient's health.[1] The first article that demonstrated the anatomical-physiological relationships of the 5 diaphragms by setting the clinical rationale for OM dates back to 2013: tentorium cerebelli; tongue; thoracic outlet; diaphragm; pelvic floor.[2]
- Tentorium cerebelli. This meningeal structure is located in the posterior cranial fossa area. It has a semi-circular transverse septum shape, with a concave front edge and convex posterior edge; it separates the cerebral lobes from the cerebellum. The falx cerebri merges with this septum, while below is the falx cerebelli. Its path involves the internal occipital protuberance, the occipital bone, the parietal bone, and the temporal bone; inside, we find the superior petrosal sinuses and the sinus rectus for the venous outflow and the glymphatic system for the lymphatic outflow.
- Innervation: The supratentorial portion is innervated by the nervus tentorii, which is a branch of the ophthalmic nerve, involving, in particular, the tentorial notch and the area of the straight sinus and transverse sinus. Parasympathetic fibers innervate the supratentorial area, probably originating from the sphenopalatine ganglion, together with fibers deriving from venous and arterial blood vessels that nourish the meninges; sympathetic fibers derive from the middle meningeal artery (which derive from the stellate ganglion), which terminate in the supratentorial area. The afferents of the tentorium deriving from the nervus tentorii end their path in the dorsal horns at the level of C2; the sympathetic and parasympathetic autonomic afferents derive from the dural vascular plexus and terminate in the medullary area of C1-C3. The subtentorial area is involved by the roots of C1-C4, by sympathetic fibers deriving from the sympathetic trunk, and by some cranial nerves such as X (vagus), IX (glossopharyngeal), XII (hypoglossal). The literature describes other possible innervations, such as some branches of cranial nerves VII (facial), together with parasympathetic fibers, and fibers of the IV (trochlear with the tentorial segment) coming from arterial vessels.
- Myofascial relationships: The subtentorial area is involved by 3 of the 4 suboccipital muscles (rectus capitis posterior minor, oblique capitis inferior, rectus capitis posterior major), forming a myodural bridge; we must remember that the suboccipital muscles are part of the thoracolumbar myofascial system. Through a fibrous structure known by the name of to be named ligament (TBNL), the nuchal ligament has relations with the tentorium cerebelli.[1][3][4][5]
- Tongue. The suprahyoid and sub-hyoid muscles influence the movements of the tongue and vice versa; equally, the intrinsic and extrinsic muscles of the tongue work in synergy: one can speak of the lingual complex. The lingual complex affects the occipitocervical area, the anterior area of the cervical tract, and is involved in chewing, breathing, and other bodily functions. Intrinsic muscles: transversus and verticalis linguae, inferior longitudinalis, superior longitudinalis; extrinsic muscles: genioglossus, styloglossus, hyoglossus, palatoglossus, glossopharyngeus, chondroglossus.
- Innervation: At the central level, the tongue musculature is represented in specific areas, such as the limbic area, the somatosensory cortex, the medulla oblongata, and the midbrain area. The innervation concerns the XII cranial nerve (hypoglossal), the V (the lingual nerve that derives from a mandibular branch), parasympathetic branches (deriving from the mandibular ganglion). The lingual nerve and the XII are anastomosed within the lingual musculature (and in other areas). Cranial nerve IX (glossopharyngeal) with parasympathetic branches innervates the tongue; the IX anastomoses with the parasympathetic branches, the XII, and the lingual nerve within the lingual musculature. Nerve VII (facial) provides afferent information of the tongue. Sympathetic-type fibers innervate the tongue, which fibers originate from the superior cervical ganglion—myofascial relationships. The lingual complex directly involves different muscles, such as the supra and sub-hyoid muscles, the masseter, the temporalis, the buccinator, the mylohyoid, the pterygoid, digastric, superior pharyngeal constrictor muscle; all the connective tissue of the craniocervical tract and up to the thoracic outlet is in communion with the lingual complex.[1][3][6][7]
- Thoracic outlet. This structure contains musculoskeletal components: sternum, first two ribs, clavicle, scapula, first two thoracic vertebrae, trapezius muscle, subclavian muscle, pectoralis major and minor muscles, intercostal and deep musculature of the dorso-cervical tract, and scalene muscles. We find three narrow passages for the brachial vascular-nerve package (C1-T1): anterior and middle scalene muscle, clavicle-first rib, and pectoralis minor muscle. This location also contains aspects of the sympathetic system, particularly the stellate ganglion and the vagus nerve with its parasympathetic component. The thoracic outlet region contains the fusion of the cervical bands with the thoracic bands and the passage of some visceral structures, including the pleural dome.[1][8]
- Diaphragm. The diaphragm muscle involves the terminal portion of the sternum (xiphoid process), the last six ribs, the vertebral bodies anteriorly of the dorsal-lumbar vertebrae (T11-L4), the transverse processes of L1. The vena cava, the esophagus, the aorta, the azygos, and hemizygous veins cross the muscle, as well as the lymphatic system (Quilo cistern). The innervation comes from the phrenic nerve and the vagus nerve, with components of the sympathetic system (subdiaphragmatic ganglia). The diaphragm directly involves the abdominal muscles, the psoas muscle, the quadratus lumborum muscle, as well as the entire fascial continuum of the thorax, abdomen, and back-lumbar area.[1][3]
- Pelvic floor. It is a muscle complex formed by the levator ani muscle, three muscle groups (puborectal, pubococcygeus, and iliococcygeus muscles), and the ischiococcygeus muscle. Furthermore, the gluteus maximus muscle is part of the levator ani muscle via a fascial septum at the level of the posterior ischioanal fossa. The pelvic floor area involves the abdominopelvic cavity, pubic symphysis, coccyx. The innervation of these muscles derives from S2-S4 (pudendal nerve) and the nucleus of Onuf (sacral spinal cord). The parasympathetic fibers derive from the S2-S4 area; sympathetic fibers derive from the lumbar chain. The pelvic floor is affected by different bands, such as the transversalis fascia, prevertebral fascia, iliac fascia, pectineal fascia, thoracolumbar fascia. Other contractile districts are involved via fascial connections, such as the adductor muscles, the tensor fascia lata, and the pyramidalis muscle. Below the pelvic floor, we find a triangular fascial formation, known as the urogenital diaphragm.[8][9]
During a quiet inhalation, a central pattern generator (CPG) comes into action, which components are found in the brainstem and spinal cord. The XII nerve is activated in the pre-inhalation and inspiratory phase to dilate the upper airways, undergoing a double movement: the hyoid portion is tractioned towards the front, while the posterior and upper portion is brought caudally and posteriorly. The sensation that the person feels is that of bringing the tongue back during the inhalation.
During the continuation of the inhalation phase, the phrenic nerve activates the diaphragm muscle; the vagus nerve manages the area of the esophageal hiatus (depending on whether there is a food bolus or not), the external intercostal muscles contract; tendentially, the abdominal muscles, the internal intercostal muscles, and the pelvic floor muscles are inhibited by the CPG, although the basic muscle tone remains in them.
The pelvic floor musculature descends, mirroring the movement of the diaphragm muscle. The opposite of the movements described happens during the exhale. When the diaphragm moves, all the myofascial systems of the five diaphragms are in tension (elongated and shortened), just as all bodily fluids are stimulated in their movements.[10][11][12]
Indications
Chronic diseases always show a recurrence of very similar related disorders and symptoms. To give examples, patients with diagnosed obstructive sleep apnea (OSA) present various related symptoms, such as headache, alterations in the neurophysiological behavior of the lingual complex, morphological and neurophysiological alterations of the diaphragm, alterations in the control of the pelvic floor muscles.[13][14][15][16][17]
In patients suffering from chronic obstructive pulmonary disease (COPD), one can encounter problems such as chronic headaches, OSA, alterations in the function and morphology of the diaphragm, and problems related to the pelvic floor muscles.[18][19]
Patients with chronic pain in the cervical tract may have common related symptoms, such as headache, functional changes in the lingual complex, respiratory dysfunctions, and postural changes in the pelvic area.[20][21][22][23]
Chronic kidney disease causes various comorbidities, such as chronic headache, OSA, impaired diaphragmatic function, and weakness of the pelvic floor muscles.[24][25][26]
The reasons are different and/or specific to the pathology in progress. The concept that emerges is the fact that the anatomical and neurological relationships of the five diaphragms have confirmation in the clinic. It is impossible to think and image the human body as a complex of discontinuous areas unable to influence each other.[27]
To understand the usefulness of the osteopathic approach with the 5 diaphragms, it is essential to know the anatomy-physiology of their connections. The osteopath not only looks at the symptom but, above all, at the causes of the symptom. Shoulder pain can be caused by diaphragmatic dysfunction. Like any other nerve structure, the phrenic nerve carries electrical and biochemical information in a bidirectional way. In its path, the phrenic nerve is mixed with the brachial plexus, like the axillary nerve (shoulder muscles).
A constant diaphragmatic dysfunction (due to trauma, emotions, and more) will induce the production of paracrine substances by the diaphragm muscle (cytokines and more), which will go retrograde towards the medulla, involving all the structures in connection with the phrenic nerve. As literature demonstrates, one of the symptoms of a functional alteration of the diaphragm muscle is a dysfunction of the shoulder arthrocinematics and/or pain (somato-somatic reflex). Another cause of dysfunctional reflexes from the diaphragm to the shoulder is the fascial continuum. When the diaphragm is lowered during inhalation, the connected fascial system is pulled downwards. It is easier, in fact, to raise the arm in flexion during an act of inhalation compared to the same movement during an act of exhalation. It can be useful to evaluate and treat the 5 diaphragms to resolve a shoulder disorder, as will be described later.
To give another example, abnormal traction of the suboccipital muscles (e.g., trauma to the sacrum area) will cause abnormal mechanical-metabolic tensions in the subtentorial dural area. As shown in the literature, the dural tissue will produce irritants that will affect the trigeminal system, with cranial pain. The mechanical dural receptors are found in particular near the vascular pathways; if stimulated for non-physiological causes, they can induce a chronic inflammatory situation, which will involve all the nervous structures of the area. Considering that the subtentorial area is innervated by the same cranial nerves that involve the lingual complex, we can strongly hypothesize the presence of a motor and/or sensory dysfunction. We must also consider the fascial relationships between the tentorium cerebelli and the lingual complex, the cervical tract, and the occipital area.
A dysfunction of a fascial tract can alter the dynamics of these relationships, both in the vicinity of the symptom and if the cause is distant, such as, for example, a sacral trauma. The thoracolumbar fascia includes the deep muscles of the spine, including the suboccipital musculature; abnormal traction of the sacrum will induce an abnormal tension of these cervical muscles.[28][29][30]
When there is a chronic, local or systemic problem, it is advisable to use the 5 diaphragm approach. In the acute phase, it is possible to use this approach, respecting the possibility or not of putting your hands on the tissue; in the event of a non-healed wound, the use of these techniques may not be effective, or the clinician's touch may cause discomfort to the patient.
Contraindications
No text in the relevant literature highlights contraindications for the use of the 5 diaphragms in osteopathic medicine. The only contraindications are the use of joint techniques, such as high-velocity low amplitude (HVLA). As we will see in the description, the proposed techniques are very gentle, without danger.
Equipment
The necessary equipment is a table (as well as all previous clinical data).
Personnel
The osteopathic approach can be performed by the clinician who has studied osteopathic medicine. The patient undergoing the treatment must always be aware of the clinician's procedure and only after prior clinical evaluation.
Preparation
Before proceeding with osteopathic manual treatment, the clinician must evaluate the districts that make up the five diaphragms. The evaluation is divided into two steps. The first is general, while the second is very thorough.
General Listening
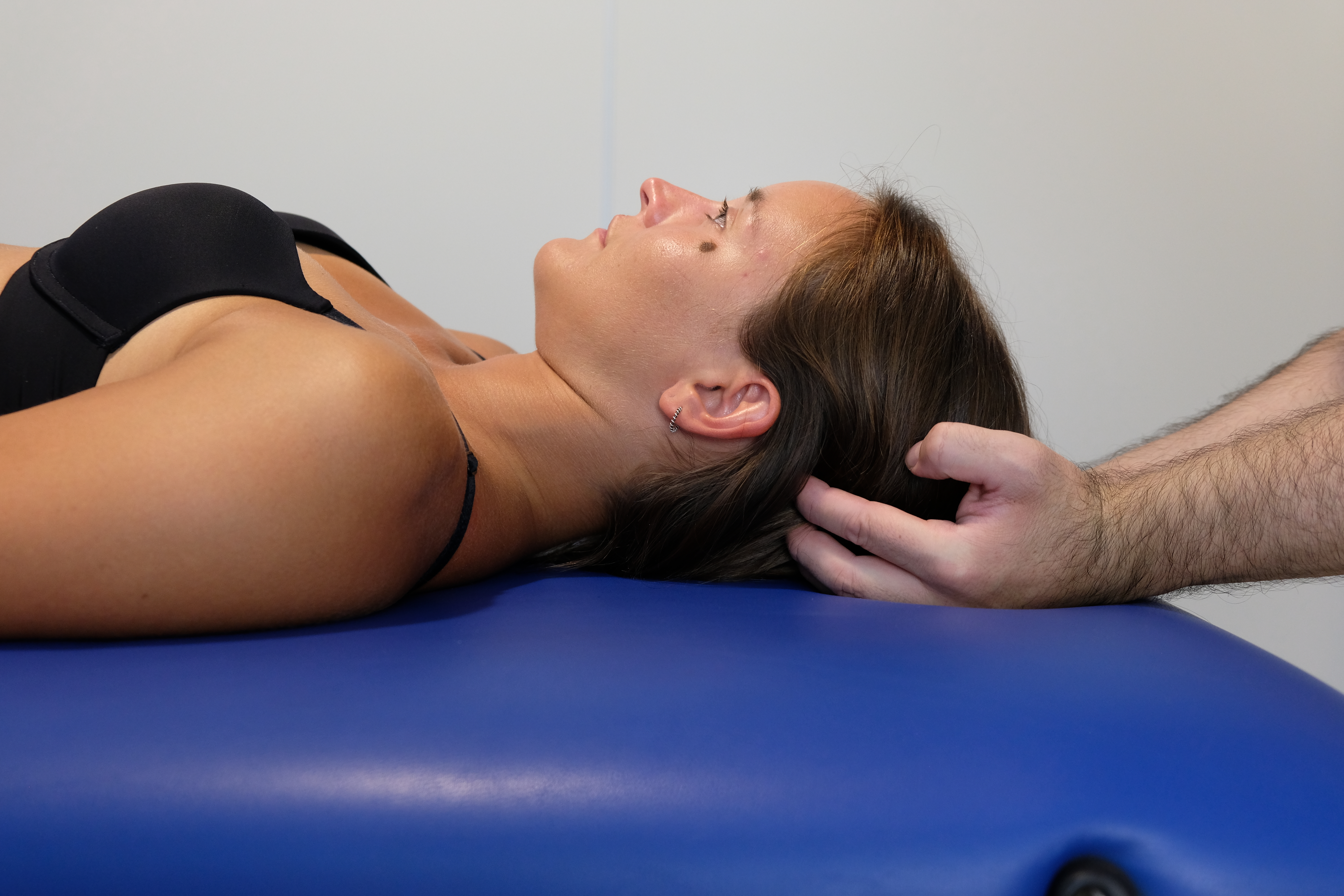
The patient is supine, while the operator is seated at the head of the table, starting to palpate the tentorium cerebelli. The little fingers are placed in contact with the inion or external occipital protuberance. In contrast, the other fingers form a semicircle, reflecting the tentorium's internal position until the index finger is placed on the asterion. This small bony depression is the union between the 'occipital, parietal and temporal bone. The tissue, the presence of pain, the temperature, and any tissue abnormalities or entrainments are assessed. In theory, one should "listen" to the movement of the tentorium with their fingers as an expansion and a return from the expansion. The movement does not match the heartbeat's rhythm or the breath; it is a slower movement.
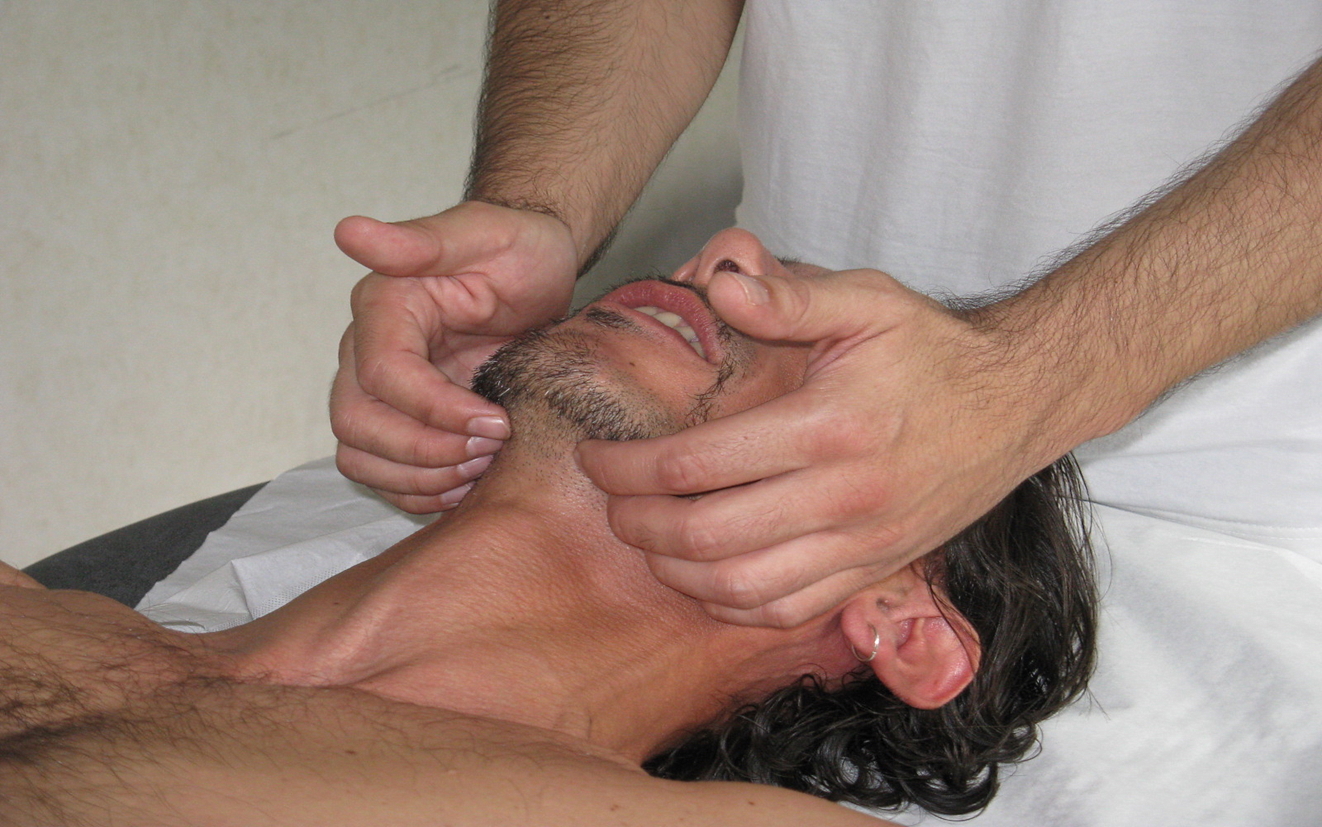
The clinician places the fingers of one hand under the buccal floor to assess any abnormal tensions of the lingual complex and listen to the small movements present; It is also possible to evaluate the tongue with one hand that takes the great horns of the hyoid bone, while the other is always placed under the buccal floor.
Always with the clinician sitting in the same position, the thoracic outlet is evaluated. The index finger is positioned above the clavicle, while the middle finger is placed under the same bone; the thumb should be placed near the transverse process of C7. The other two fingers rest on the chest. The tissue, the presence of pain, the tissue's temperature, and any tissue abnormalities or entrainments are assessed. The movement to be perceived through palpation is an opening and closing of the thoracic outlet. The movement does not correspond to the rhythm of the heartbeat or the breath; it is a slower movement.
To evaluate the diaphragm muscle in a general way, the clinician stands up and stands beside the patient. The hands are positioned posterolaterally, as the diaphragmatic displacement occurs to a greater extent precisely with the postero-lateral portion; the anterior portion displaces a few millimeters with calm breathing. The tissue, the presence of pain, the temperature, and any tissue abnormalities or entrainments are assessed. Any alterations in the perceived movement of the diaphragm should also be evaluated; we must remember that the diaphragm has a minor displacement with its right area due to the presence of the liver.
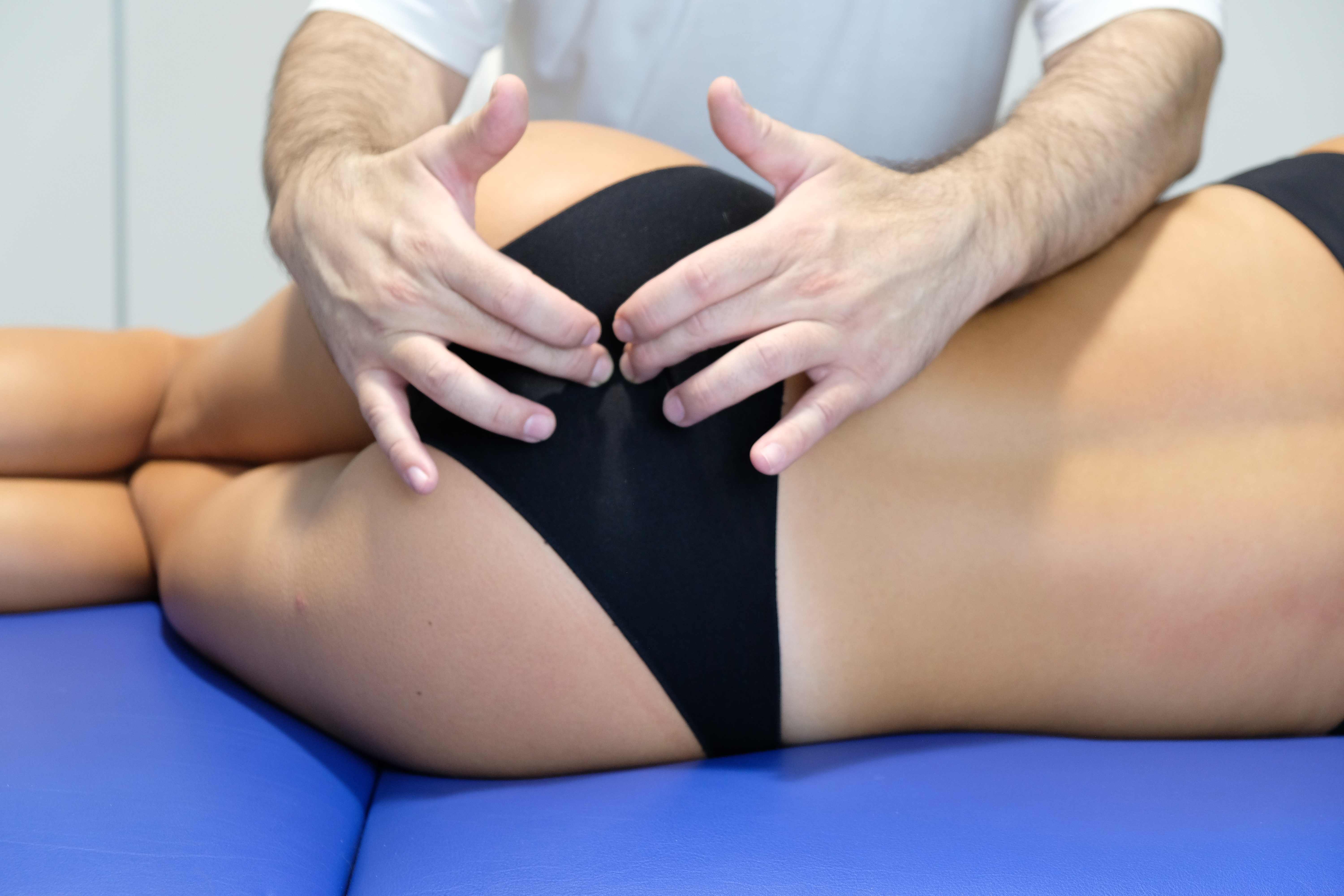
The last step of this general assessment is towards the pelvic floor, with the clinician standing. The palms of the hands are placed on the iliac wings, giving small oscillations towards the bed as if to want to "open" the pelvis. In this way, it is possible to identify movement or pain restrictions of the various components that make up the pelvic floor, muscles and joints, and any limits of visceral adaptation.
With this first approach, it is possible to highlight areas with difficulty in movement or symptoms such as pain or discomfort. To identify a more problematic area that requires osteopathic treatment, it will be necessary to carry out simple inhibitory tests. To give an example, the clinician finds dysfunctions in the respiratory diaphragm and the lingual complex. It places one hand on the diaphragmatic rib area, while the other hand is placed under the buccal floor; with the first-hand listening, he creates a pressure tension with the fingers of the second hand. In this way, the afferents of the lingual area are masked, highlighting any dysfunctions of the diaphragmatic area. The opposite action is performed, that is, the hand on the rib area presses against the ribs, while the cranial hand via palpation "listens" to what happens to the buccal floor. The anatomical area where the previously felt dysfunction does not change will most likely be the area that needs treatment.[31][32][33]
Manual Specific Evaluation
Tentorium cerebelli:
- The tone of the sub-occipital muscles
- The range of motion of the first cervical vertebrae, up to C4, and the dorsal nerve exits of the cervical plexus up to C3 (you can feel the presence of small buds under the finger)
- The presence of movement of the temporal bones and all sutures involving the temporal: occipitomastoid; sphenosquamosal; petrojugular; petroccipital; sphenopetrosal; temporozygomatic; parietomastoid; temporomandibular
- The tension of the tentorium of the cerebellum can be assessed by pulling the ear lobe in an anterior, oblique, and slightly caudal direction; the tension generated reaches the tentorium and the ear that responds to traction with greater brake, corresponds to the tentorial area in dysfunction.
- In evaluating the tentorium, it is necessary to listen via palpation to the other membranes and discern if the tentorial tension that appears is the cause or an effect from other membranous portions. Many texts deal with how to work and listen to membranes; it is not the technique that counts, but the palpatory quality.
Lingual complex:
- Visually observe the tongue and how the mouth is opened by the patient (if there are mandibular deviations and/or joint noises of the temporomandibular joint)
- Evaluate the behavior of the cervical spine when the mouth opens and the tongue is protruded/retruded.
- Observe the typology of the dental class to understand how the tongue interacts
- Evaluate how the tongue actively moves with the mouth open: forward or protruded; bringing the tip of the tongue up or in dorsiflexion; below or in ventroflexion; the whole tongue cranially or in elevation; inferiorly or in depression; lateral movements, right and left; backward or in retrusion.
- With a gloved finger, test the tongue's strength, with the movements just mentioned actively, but placing the finger in the opposite direction to the movement requested, creating minimal resistance.
- The tongue's movement is tested by asking the patient to rotate his head to the right and to protrude it, and the left side; the same protrusion is observed but with the cervical tract flexed and then extended. This observation is also important for the fascial and embryological correlations of the tongue and neck.
- The patient is subjected to a test to verify balance (Fukuda), with closed eyes and the tip of the tongue at the spot of the upper incisors, as we know that lingual afferents are important for postural management. The test is repeated with the tongue in the resting position. If the posture improves with the tongue in the spot, its afferents are correctly integrated into the body system; if, on the other hand, the result is indifferent or gets worse with the lingual spot, we could assume a tongue problem.
- With the tongue in dorsiflexion, the strength of the thigh is tested; the patient is asked to extend the knee, while the operator places his hand on the leg to create resistance. It is repeated with the other limb. If the strength increases, the lingual integration is preserved, while if it does not change or worsens with the tongue at the palatine spot, it could be a non-physiological lingual response. There is a parallelism between limb strength and lingual strength; a loss of limb strength corresponds to a decline in lingual contractility.
- The patient is asked to smile or pursue his lips, evaluating how the musculature behaves. In speech functions, the tongue has a neuromotor collaboration with the lip muscles, and any weakness of these muscles could detect a loss of strength and lingual coordination.
- Evaluate with the gloved hand, the tone of the chewing muscles
- Palpate the hyoid bone in different phases while the patient swallows, breathes, and opens the mouth and with a protrusion/retrusion movement of the tongue
It is possible to perform a non-instrumental test to get a preliminary indication on the function of the tongue, through the Performance Tongue Test (PTT). [34]
Thoracic outlet:
- Sternum
- Sternum-clavicle, sternum, and first rib joints; clavicle-scapula, C7-D1-D2, ribs-D1 and D2
- Observe how the scapula moves actively and passively
- Observe how the first rib moves
- Assess the scalene muscles, pectoral muscles (major and minor), subclavian muscle, trapezius muscle
- Shoulder mobility
- Pleural dome
- Fascial system of the pleural dome
Some tests can be carried out to understand if there is a neurological dysfunction:
- EAST (Elevated Arm Stress Test - Surrender)
- ULTT - (Upper Limb Tension Test of Elvey)
No test manual can assess the presence of vascular dysfunctions.
Diaphragm muscle:
- The patient is always supine. Put your hands sideways to the ribs in the diaphragmatic area; listen to how the ribs move actively and passively (giving small oscillations).
- Evaluate the xiphoid process (if it is painful); evaluate how the ribs and the xiphoid process behave.
- To evaluate the diaphragmatic domes, right and left, with the hand resting on the anterolateral ribs, the clinician applies a slight cranial thrust to evaluate the elasticity of the tissue. The forearm is parallel to the patient's abdomen.
- With the same position, but with the forearm positioned at 45 degrees with respect to the patient's abdomen, the clinician's hand carries out stresses towards the bed to assess the posterolateral muscle mass.
- Evaluate the medial and intermediate pillars, stimulating the movement of the vertebrae from D11 to L4 and the last rib.
- Evaluate the phrenic nerve in the passage of the thoracic outlet, near the anterior scalene muscle and laterally to the sternocleidomastoid muscle (the portion of the clavicle head); check if it is a painful area.
It is possible to use the manual evaluation of the diaphragm (MED Scale) and a test to understand if the diaphragm is correctly integrated into the body context from a neurological point of view. The patient performs a Fukuda test with a deep inhalation and repeats, but with normal breathing; if the diaphragm is not dysfunctional, the balance improves. If the test performed reveals a latent imbalance, the diaphragm may have dysfunction. Additional verification of the previous result is to evaluate the strength of the thigh during a flexion with the patient standing, placing a resistance (with the clinician's hand) over the thigh during the active movement, with a deep inhalation. If the strength improves, the diaphragm is properly integrated; if the strength does not improve or gets worse, the diaphragm may have functional dysfunction. The name of the test is the Bordoni diaphragmatic test (BDT) [35].
Pelvic Floor:
The patient is in a supine position.
- Symphysis pubis
- Suprapubic area for trigger points
- Ilioinguinal ligament
- Obturator nerve
- Adductor muscle strength
- Rotator muscles strength of the hip
- Pelvic floor muscles
- Pudendal nerve
- Sacral base-L5
- Sacroiliac joint
- External evaluation: bladder; uterus
The patient is in lateral decubitus.
- Pelvic floor muscles
- Iliolumbar ligament
- Iliac bone
- Coccyx
The patient is in the prone position.
- Spring test sacrum
- Trigger points thoracolumbar fascia
- Gluteal muscle
- Piriformis muscle
- Long dorsal sacroiliac ligament
- Pelvic floor muscles
- External evaluation: rectum
If the patient cannot position himself in certain positions, the osteopath will have to adapt to the patient and find different evaluation methods.[10][36][37]
Technique or Treatment
One of the most advanced techniques in manual osteopathic medicine is the unwinding approach, conceived by the American osteopath Dr. Frymann. It is a technique that can also be used in the pediatric sphere, as it exploits the principle of the patient's intrinsic force without inducing any manual force on the part of the operator.
The osteopath can perform a treatment on every single structure that makes up that particular diaphragm if the latter is considered dysfunctional, or the clinician can perform a treatment that involves more than one diaphragm simultaneously. Another choice is to treat all the diaphragms with general approaches. The technique used for each component, or a single component of a specific diaphragm, will depend on the clinician's choice.
When it is decided to work with more than one diaphragm, since the evaluation has brought the clinician's attention to two dysfunctional diaphragms, it is feasible to use the unwinding technique, the latter used in previous trials. Also, in this case, you can choose to work with a manual grip that reflects that of the evaluation and pass, once the technique is finished, on the second diaphragm, using the manual grip of the evaluation to perform the technique. Another possibility is to place a hand (the cranial hand) on one diaphragm and the caudal hand on the second diaphragm, using the Dr. Frymann technique. The manual grip will depend on the comfort of the osteopath, as it is a systemic technique. With this second possibility, the diaphragms may not necessarily be close (tentorium and tongue) but also distant (tentorium and pelvic floor). Finally, if the clinician considers that all diaphragms have to be worked, a manual grip can be used for each diaphragm and proceeded to the next. The time required to carry out the technique will depend on the skill of the operator, as well as the procedure's effectiveness on the patient.
When placing the hands on the patient's tissue, the osteopath must not add force or induce movement. The hands follow the inherent tissue movements. Initially, the perceived movement will be chaotic or unsymmetrical. The technique ends only when the clinician perceives the inherent movement of the patient's tissue with a symmetrical pattern in amplitude, entity, and duration. The hands will move but, in reality, they will always be still. This happens because the hands follow the various tissues and not vice versa. We have to imagine a seagull on the waves of the sea. Apparently, the seagull makes multiple movements, but, in reality, it is the sea that makes the seagull move.[38]
Complications
Current scientific literature demonstrates that there are no complications in performing unwinding techniques in patients. The technique can also be used on wounds not yet fully healed.[38]
Clinical Significance
Dysfunction of the lingual complex could be the source of dural pain. We know that tooth pulp inflammation causes a secondary symptom picture of pain in the tongue, through a retrograde behavior of the electrical and biological information from the gums, towards structures that innervate the lingual complex. From the electrophysiological and mechano-metabolic point of view, we cannot always predict where the symptom appears, precisely because of the networks of bodily innervations that communicate with each other. If the tongue has mechanical problems following a cervical trauma (whiplash), a situation could arise where the trigeminal system that innervates the lingual complex sends information in antidromic modalities to the Gasser ganglion. The latter contains neural cells and macrophages, and lymphocytes (and glial cells), which are responsible for making the trigeminal network more receptive to mechano-metabolic information, triggering trigeminal pain. At the dural level of the tentorium cerebelli, we can find mechanical receptors near the arterial routes. When these receptor areas are activated, they cause vasodilation and trigeminal pain. The tongue can be responsible for dural trigeminal pain, sending non-physiological information to the trigeminal ganglion in the Meckel's cavity, which will stimulate non-physiological behaviors in the dural area, with the final result of local dural pain or in other locations of the skull. (for example, to the eye for the important connection with the nervus tentorii).[39][40]
The manual treatment of the 5 diaphragms has several objectives, including improving the circulation of body fluids. The meningeal system encloses the venous vessels and the glymphatic system, which is drained, in particular, via the cribriform plate, to pass to the oral mucosa, tongue, and cervical tract, up to the thoracic outlet. Cranial dural tissue can change its tension state. This means that the passage in the fluids will be altered for different reasons. To give an example, a mechanical tension deriving from the suboccipital muscles can vary the tension of the tentorium and create an inflammatory environment where the arterial passages contribute to the extent of the inflammatory response as they alter their tone. We know that lighter fluids such as lymph and interstitial fluids are displaced, in particular, by the heartbeat, which is reflected in arterial vascular tone. A tensional alteration of the tentorium and arterial vessels can slow down the glymphatic flow and adversely affect immunoregulation. In the animal model, lymphatic vessels are found near the cranial nerves, including the branches that involve the functioning of the tongue. We can strongly assume that a non-physiological mechanical tension and an altered metabolic environment can produce inflammation and/or infections of the lingual complex, both due to altered nervous conductivity and the transport of biological substances to the tongue, as the literature suggests. Evaluating and treating the tentorium, in this case, to solve or help a lingual problem, has a clinical logic.[39][41][42][43]
Paresthesia in the fifth finger due to non-physiological pressure on the ulnar nerve could result from abnormal tension in the diaphragm muscle. Palpation could bring the osteopath's attention to the respiratory diaphragm, despite the suspected cause linked to the thoracic outlet syndrome. For an antidromic effect, the phrenic nerve (right or left) can carry inflammatory substances synthesized by contractile fibers or connective tissue in retrograde mode to the medulla, involving the motor neurons of the subclavian nerve. This last nerve is able to create non-physiological muscle tension in the subclavian muscle (hypertonus) and maintain the first rib in inspiratory attitude, which will compress the ulnar nerve resulting in a neuropathic picture. As demonstrated in the literature, a diaphragmatic herniation problem could be responsible for pain in the shoulder joint (involving the axillary nerve). In chronic pathologies, where the diaphragm muscle is involved, it is possible to find thoracic outlet syndromes, even if the nature of this combination is not always determined or illustrated by the authors. Myocardial infarction can alter the genetic transcription of some diaphragm proteins (such as in aging), inducing dysfunction in the breath, even sub-clinical. This can again lead to inflammatory substances being produced by the diaphragm and negatively affecting the function of the brachial nerves via transport by the phrenic nerve. If the diaphragm is in the inspiratory position, the phrenic nerve can undergo chronic non-physiological traction. As happens in traction neuropathies, the nerve tissue will produce biological substances that can reach the brachial medullary nerves.[2][44][45][46]
In some patients, the vagus nerve has a close relationship with the omohyoid muscle (infrahyoid muscle) and medial to the jugular vein; in some patients, this muscle may involve both clavicles or the mastoid process. The omohyoid muscle may be positioned above the superior transverse scapular ligament or laterally, under which the suprascapular nerve (C5-C6) passes. The omohyoid muscle is activated by the movements of the tongue and probably plays a proprioceptive role in the movements of the scapula. The suprascapular nerve and the phrenic nerve, as demonstrated with dye injection, are closely related. If the tongue's position tends to remain towards the hard palate, the omohyoid muscle will be more activated from an electromyographic point of view; this situation can alter the mechanical environment of the passage of the suprascapular nerve and negatively affect the phrenic nerve. Furthermore, the innervation of the omohyoid muscle (C1-C3) could alter the environment of neurological information that reaches the suboccipital muscles; the vagus nerve itself could undergo abnormal tension from the sub-hyoid musculature. Therefore, we could have a disturbance in a localized area (thoracic outlet) that spreads to other diaphragms. An altered scapular position, in the case of a hyperkyphotic attitude, could cause the same problems.[47][48][49][50]
Hypertonicity of the muscles that make up the pelvic floor could be a source of pain in this anatomical area, particularly during movements of the pelvis, during inhalation, or physical efforts (lifting or sneezing). The chronicity of the pain or the consequent (visceral) disorder could negatively alter the excursion of the diaphragm muscle, which could reduce its functional capacity during inhalation and create conditions that lead to chronic lower back pain. The osteopath must be aware of the anatomy of the 5 diaphragms and never dwell only on the symptom. In this example, the diaphragm should not be treated in the first instance but, rather, focus attention on the pelvic floor muscles.[51][52][53]
Previous cardiac surgery in median sternotomy can have iatrogenic repercussions on the phrenic nerve, such as a permanent partial injury. Or, if the lesion is complete and extensive, the patient may undergo another diaphragm plication to try to restore some of the main respiratory muscle function. One of the symptoms after cardiovascular surgery and in the presence of partial or total plegia of the phrenic nerve, particularly on the left and more rarely on the right, is an alteration of the movement of the ipsilateral shoulder (thoracic outlet). The main motivations concern an antidromic behavior of the nerve, which carries multiple biochemicals towards the medulla and involves the brachial plexus (axillary nerve). Furthermore, if the myofascial continuum undergoes a functional discontinuity due to a weaker anatomical area (hemidiaphragm), there will be an alteration in the distribution of mechanical tensions and, as in this specific case, the shoulder will undergo an alteration of its range of motion. The concept that must emerge from this clinical situation is that in the presence of a permanent phrenic lesion or the case of plication of the diaphragm, the osteopath can bring great relief to the patient without completely resolving the situation, as it is present. Structural damage (plegia and/or diaphragmatic scar). It is not a defeat, but it is a moment of maximum adaptability for the clinician, recognizing their limits and increasing the patient's maximum adaptability.
Enhancing Healthcare Team Outcomes
When a patient suffers from a disease, pain, or ailment, his entire personal sphere becomes involved. If the dysfunction is chronic, the psychic and emotional spheres will be involved. It may happen that, despite the osteopathic treatment, the results do not arrive; either the patient does not follow the clinician's directions, or the patient has an emotional wound deeper than the bodily disturbance. In both cases, the patient's involvement as the main actor in the treatment process is fundamental. We must understand not only the corporeal sphere but also the emotional and psychic one, making use of various health professionals, such as psychologists or psychiatrists, when necessary.
Turning to other health professionals is essential to obtain the maximum healing capacity of a patient, as the body is made up of different fields of scientific interest, not only osteopathy. Improving skills means interacting multidisciplinary level.
Not only do osteopathic outcomes improve with a multidisciplinary team, but results can be compared from different measurement sources.[54][55][56]
Another fundamental concept, not just limited to osteopathic medicine, is that science cannot always solve the patient's problem or that medical specialty is not always suitable for that specific pathology or dysfunction. It is mandatory to involve the patient (if not a minor) in the clinical situation, while, in the second case, collaboration on the part of the clinician is mandatory by sending the patient to another specialist.
Nursing, Allied Health, and Interprofessional Team Interventions
The five diaphragms involve distinct body districts, albeit in a relationship of absolute continuity. The presence of different healthcare professionals is a must.
Nursing, Allied Health, and Interprofessional Team Monitoring
To further confirm the results of the osteopathic manual treatment, we must send the patient to health professionals who reflect the anatomical area of competence or the pathology of competence or to constantly monitor the therapeutic path.