Continuing Education Activity
Hypertrophic scars are contained within the site of injury and may regress over time, while keloids spread beyond the borders of the initial injury and do not regress. On histological examination, hypertrophic scars tend to have collagen in a wavy, regular pattern, whereas keloids have no distinct pattern of collagen. This activity reviews the evaluation and management of hypertrophic scars/keloids and highlights the role of the interprofessional team in the recognition and management of this condition.
Objectives:
- Describe the recommended management of hypertrophic scars/keloids.
- Outline the typical presentation for a patient with hypertrophic scars/keloids.
- Review the pathophysiology of hypertrophic scars/keloids.
- Summarize the importance of enhancing care coordination among the interprofessional team to ensure proper evaluation and management of hypertrophic scars/keloids.
Introduction
Typically, wound healing occurs in a dynamic process of balanced regulation. When this regulation is unbalanced, less desirable scars such as hypertrophic scars and keloids can occur. Hypertrophic scars and keloids are both raised, firm scars formed from excess fibrinogen production and collagen during healing.[1] They can both be symptomatic, most commonly, pruritic but can also be painful and cause movement restrictions and cosmetic disfigurement.[2] Although these may often be confused, there are distinct differences between the two. Hypertrophic scars are contained within the site of injury and may regress over time, while keloids spread beyond the borders of the initial injury and do not regress. On histological examination, hypertrophic scars tend to have collagen in a wavy, regular pattern, whereas keloids have no distinct pattern of collagen.[1]
Etiology
Hypertrophic scars and keloids arise from some injury to the skin that goes deep enough to affect the dermal layer. They can occur after burns, surgery, insect bites, tattoos, acne or chickenpox, and piercings. Although the specific mechanisms remain unknown, several associations are thought to influence the formation of these abnormal scars. Systemic inflammation has been posited to increase the risks of hypertrophic scars and keloids, and conditions increasing systemic inflammatory markers have been hypothesized to increase the risk of both scar hypertrophy and keloid.[3] Some authors have suggested sex hormones may affect keloid risk by increasing inflammation leading to overproduction of collagen.[4] Others have described increases in the number and size of keloids in people with hypertension, though an etiologic role has yet to be demonstrated. Mechanical forces on the wound have been shown to be an important contributor, with increased wound tension and other increases in mechanical stress increase the risk of pathogenic scar formation.[5][6]
Epidemiology
Keloid formation seems to have a genetic predisposition. A classical association is increased incidence of keloid in people with darker skin complexion than individuals with a fairer complexion. The highest prevalence is seen in the African population, followed by the Asian and Hispanic population, and less frequently in Caucasians. Some studies have shown keloid formation in twins, suggesting a genetic predisposition, as well as several generations of families that are affected by keloid formation.[7]
Hypertrophic scars do not appear to have a genetic predisposition. Some studies suggest, however, that they are more common in populations with a darker complexion. Hypertrophic scars also appear on areas of skin subject to stretching due to the increased tension.[8] Reports show that the incidence of forming hypertrophic scars is 39% to 68% after a surgical procedure and 33% to 91% after burns. Although there have been reports stating an increase in hypertrophic scarring in women, other studies have shown no difference between men and women.[9]
Both keloids and hypertrophic scars tend to occur in younger populations, ages 11 to 30 years old, which is thought to result from the increased rate of epidermal turnover in this younger population and increased collagen production.[8] Younger populations are also thought to have more tension on their skin and a much more active immune system as opposed to older individuals with more elastic skin and decreased immune response.[9]
Pathophysiology
In normal wound healing, there are three phases: the inflammatory phase, the proliferative phase, and a remodeling phase. The first inflammatory stage of healing may be most important in determining the outcome of the scar. During this phase, inflammation regulation takes place through proinflammatory cytokines, IL-6 and IL-8, and an anti-inflammatory cytokine, IL-10. A change in expression in these pro-inflammatory and anti-inflammatory cytokines may lead to an increased incidence of hypertrophic scar and keloid formation.[1]
During the proliferative phase of healing, macrophages in the area of injury release growth factors, such as transforming growth factor-beta (TGF-beta), which activates fibroblasts to create collagen. In hypertrophic scars and keloids, the thinking is that the dysregulation of TGF-beta leads to the formation of these types of scars. TGF-beta 1 and 2 manage activation of fibroblasts, while TGF-beta 3 is a receptor antagonist and leads to decreased fibroblast activity. The belief is that overexpression of TGF-beta 1 and 2 and decreased expression of TGF-beta 3 leads to increased extracellular matrix production causing these abnormal scars. There is a 3-fold increase of collagen production in hypertrophic scars and a 20-fold increase in keloids, leading to a larger, abnormal appearing scar.[1]
Histopathology
In keloids, several histological findings can help to distinguish it from other types of scarring. For example, there can be increased numbers of mast cells are present in keloid scar tissue compared with normal scar tissue. An increase in keratinocytes in the epidermis may account for the thicker epidermal layer seen in keloids. In normal dermal tissue, there are two distinct layers: the papillary and reticular layers. In keloid tissue, there is no distinction seen between these two layers. There is also an abundance of collagen in keloid tissue, arranged in a haphazard pattern or whorls, as opposed to the parallel pattern seen in hypertrophic scars and normal scar tissue. There is an increased ratio of type I/III collagen in keloid cells compared with normal skin tissue, but both types are present in greater quantities in keloid scar tissue compared to normal tissue.[10]
Histologically, hypertrophic scars classify as having a flattened epidermis with increased collagen fibers organized in a pattern parallel to the dermis. Blood vessels orient vertically, and there is papillary and reticular dermal scarring.[2] Collagen fibers in hypertrophic scars are finer than in keloids, and there is a greater number of Type III collagen compared with type I collagen. As opposed to keloids, hypertrophic scars have myofibroblasts and alpha-smooth muscle actin.[11]
History and Physical
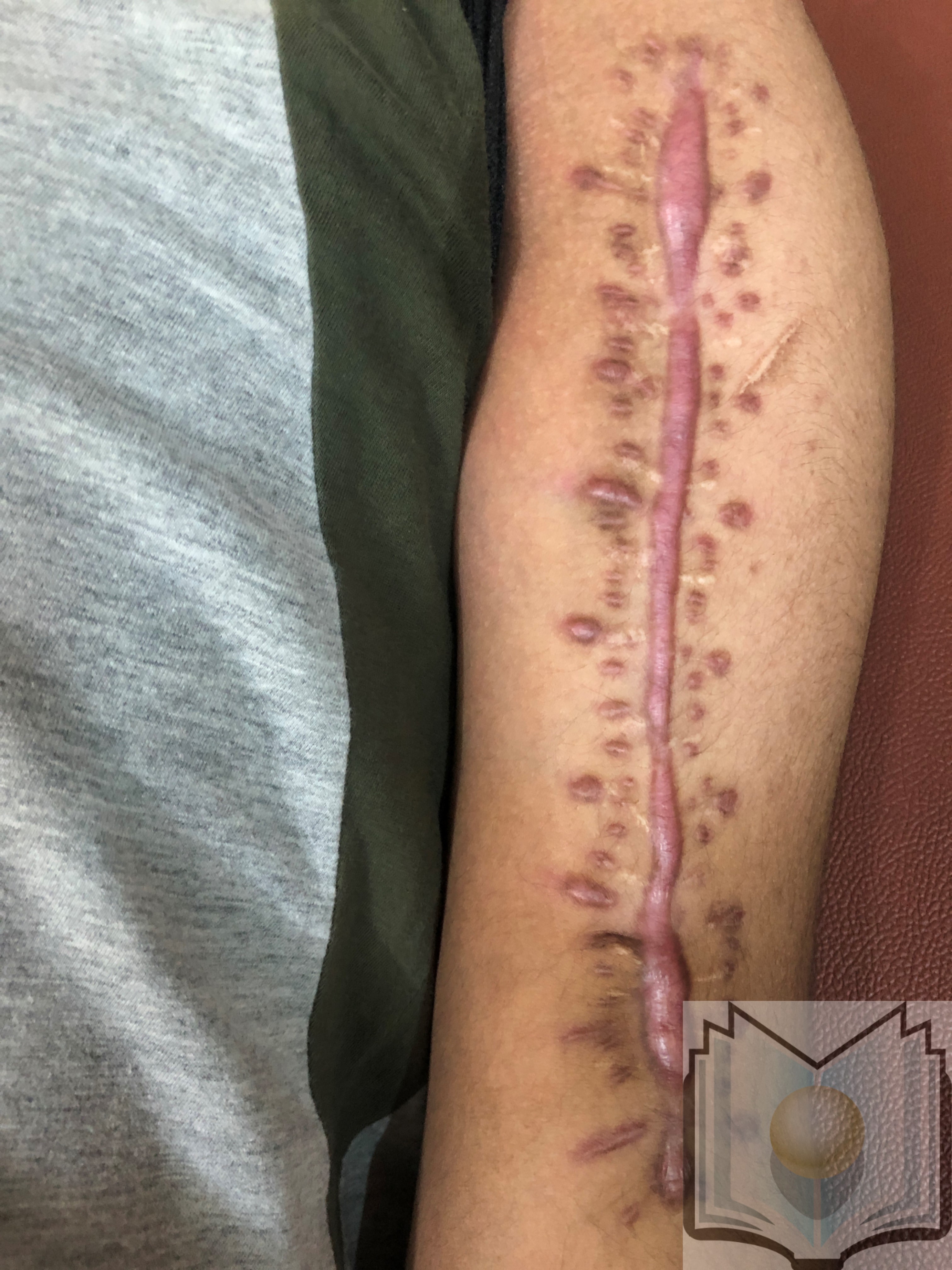
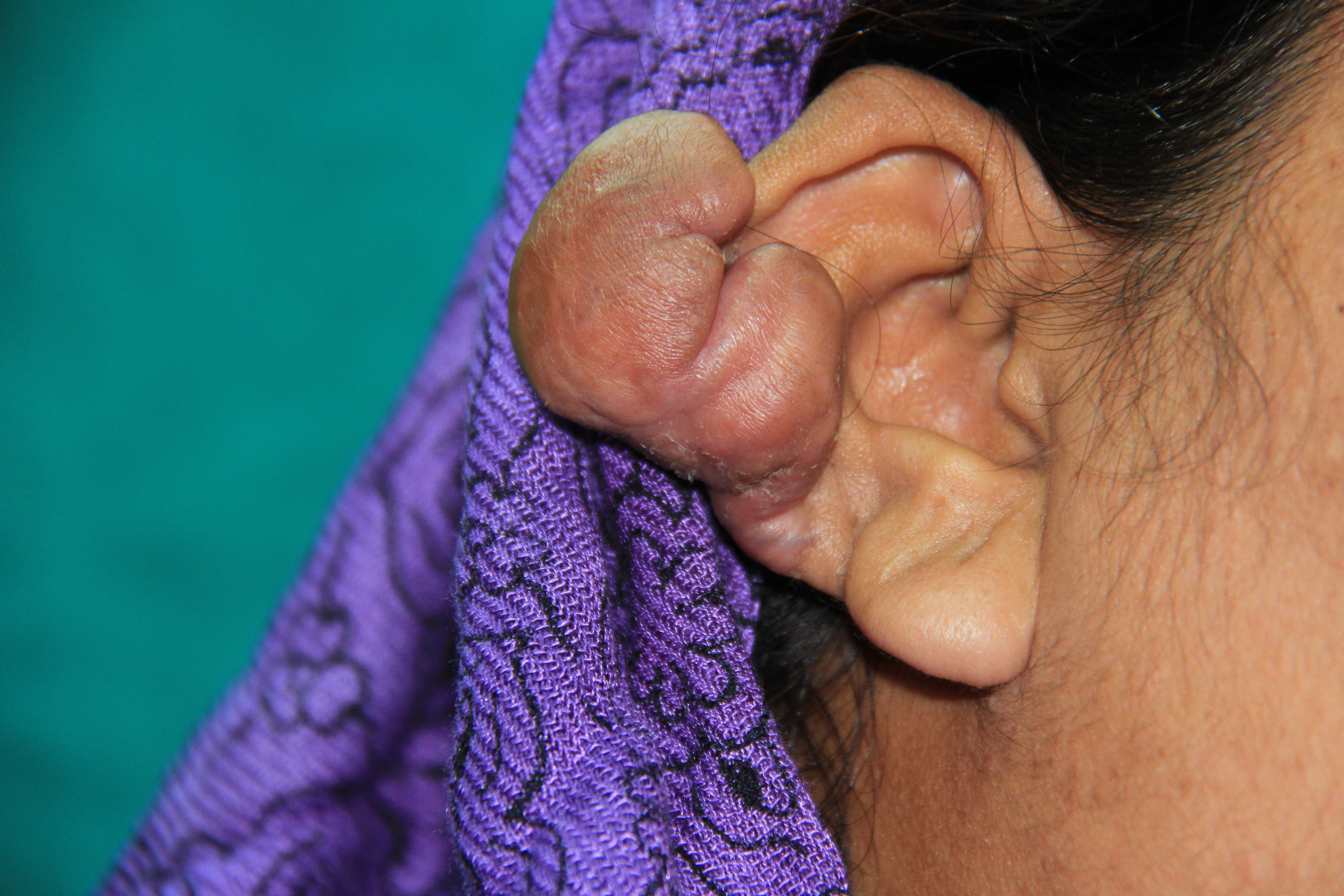
Both keloids and hypertrophic scars have a raised, thickened scar with increased cellularity and increased collagen nodules.[10] Keloids can appear after trauma or spontaneously and occur commonly in earlobes, shoulders, chest, back, cheeks, and knees. They most commonly appear in patients with darker skin tones, and there is a genetic predisposition. They can be painful and often are pruritic. They appear around 3 months after an injury but continue to proliferate with no improvement. There is a high recurrence rate for keloids after attempted excision, and they are harder to treat than hypertrophic scars. By definition, a keloid will extend beyond the borders of the original scar; if it remains entirely within the borders of the original scar, it is not a keloid.[11]
Hypertrophic scars have a higher incidence of occurrence compared with keloids and remain confined to the original wound border. There is not a strong genetic predisposition, and they can occur commonly in all skin tones. These frequently occur in extensor surfaces where there is increased tension. They can appear within one month of injury and begin to regress after six months. If excised, hypertrophic scars have a decreased incidence of recurrence, making treatment easier than that of keloids.[11]
Evaluation
The evaluation of a patient with a keloid or hypertrophic scar should begin with the patient's history. If there was no associated trauma, it is less likely a hypertrophic scar, as these are only posttraumatic. If there is a known injury, it may be either. Asking the patient if they experience pain or pruritus is an important determinant due to an increased incidence of pain and pruritus in keloids. Your history should also include a family history due to a strong genetic predisposition to keloid formation. Knowing how long a scar has been present and if there have been any changes in size can also help in your evaluation. If there is evidence that a scar is improving over time, it may indicate the patient has a hypertrophic scar as keloids do not regress.[11]
On physical exam, the location of the scar is essential, as keloids are typically present on earlobes, face, chest, and back, whereas hypertrophic scars are more common on extensor surfaces. The patient's skin tone is also crucial because keloids are more common in darker skin tones and hypertrophic scars are present in all skin types. Keloids will grow beyond the borders of the initial injury or occur spontaneously, and hypertrophic scars remain contained within the area of injury.[11]
Histological staining should also be used to evaluate the patient, as a more parallel pattern of collagen is characteristic of hypertrophic scars, and a random, whorl pattern of collagen is characteristic of keloids. Hypertrophic scars will contain thin collagen fibers with a greater ratio of collagen type III to type I, and keloids will be predominantly thick fibers of type I collagen. Hypertrophic scars will have myofibroblasts and alpha-smooth muscle actin, which will both be absent in keloids.[11]
Treatment / Management
Treatment of hypertrophic scars and keloids can be challenging, and there are several modalities available. The most important guideline for scarring is prevention by avoidance of trauma. When these procedures are unavoidable, it is important to add prophylactic therapies, such as topical therapies, during wound healing to prevent the formation of an abnormal scar. However, many patients already have an injury that has formed a keloid or hypertrophic scar. Management of these patients is important to aid in improving pain or pruritus and improving cosmetic outcomes.[1]
First-line therapy of keloids and hypertrophic scarring includes occlusive dressings, compression therapy, and steroids. Occlusive dressings are thought to work by reducing collagen synthesis by decreased delivery of blood, oxygen, and nutrients to the scar. Patients must wear these dressings twenty-three hours a day, and they work best immediately after injury or surgery.[11] Compression therapy is another treatment option that provides local pressure to the affected area; this has a thinning effect on the skin and reduces the cohesiveness of the collagen fibers. Examples of compression therapy include button compression for earlobe keloids, pressure earrings, ACE bandages, and spandex bandages. Steroids are also first-line and can be used alone or in conjunction with other therapies. Steroids decrease the synthesis of collagen and proinflammatory mediators. Intralesional triamcinolone injections are used every four to six weeks throughout several months as either monotherapy or as an adjuvant therapy to other treatments.[1]
Surgical treatment entails excision of the scar with primary closure, ensuring a tension-free closure to minimize the chance of recurrence. Although there is a high recurrence of keloids with excision, this may be reduced when performed in conjunction with steroids or more involved adjuvants such as radiotherapy and interferon therapy. Cryosurgery works by inducing cellular injury and necrosis to the affected area and reducing the area of the scar.[1] Cryotherapy works better on smaller scars and has a decreased recurrence rate when used on hypertrophic scars than keloids.[11]
Radiation therapy is an adjuvant treatment for keloids as an adjunct after surgical excision, especially in multiply-recurrent keloids. Standard external-beam radiation therapy is most commonly used (20-25 Gy total dose, often in three fractions) and is begun the day after surgical resection. Brachytherapy has also been employed but is not as common. Although the radiation dose is low, the risk of subsequent malignancy from radiation therapy exists and is one disadvantage.[11]
Newer adjuvant and emerging therapies include interferon, 5-fluorouracil, imiquimod, tacrolimus, bleomycin, retinoic acid, and botulinum toxin A. Interferon therapy works in vitro by reducing collagen synthesis. 5-Fluorouracil works as an antimetabolic agent by interrupting RNA, causing inhibition of fibroblast proliferation and TGF-beta expression to decrease Type I collagen in scar tissue. In keloidal tissue, imiquimod causes induction of apoptotic genes, causing cell death in these tissues. Tacrolimus is a topical treatment that leads to decreased fibroblast proliferation by downregulating TGF-beta receptors. Bleomycin is used in dermatology primarily to treat recalcitrant warts and keratoacanthomas, but in vitro administration to fibroblasts has been shown to decrease collagen synthesis. Retinoids are inhibitors of matrix metalloproteinases that overexpress in keloids and hypertrophic scars. Tretinoin and isotretinoin, both retinoids, cause a reduction in collagen synthesis, leading to improved scar appearance. Tension is thought to be a factor leading to the formation of keloids and hypertrophic scars. Botulinum toxin A is thought to reduce tension on the healing wound, leading to improvement in scarring.[1]
Differential Diagnosis
Some malignant mimickers of keloids and hypertrophic scarring can include malignant dermatofibrosarcoma protuberans. This condition can be distinguished from keloids and hypertrophic scars by microscopy, showing a storiform pattern of spindle cells with a honeycombed pattern of fibrous stroma.[10] On immunohistochemistry, they will contain vimentin, CD34, Bcl-2, HHF-35, and smooth muscle actin, which are not present in keloids and hypertrophic scars. Trichilemmal carcinoma is another rare cutaneous adnexal malignant tumor that can resemble keloids. These come from hair follicles and are diagnosed by large, polygonal keratinocytes with clear, glossy periodic acid-Schiff-positive cytoplasm. Keloidal basal cell carcinoma can be confused with keloids and contains prominent, keloidal type thick collagen bundles. In another case, they misdiagnosed a 9-year-old with having a keloid that turned out to be a giant cell fibroblastoma, another malignant tumor.[12] It is important to differentiate these malignancies from keloids or hypertrophic scars, especially before treatment, as steroids are contraindicated in malignant tumors, yet steroids are a common treatment for keloids and hypertrophic scars.[13]
Cutaneous scleroderma may be confused visually with keloids or hypertrophic scarring, and careful consideration should be taken to diagnose cutaneous scleroderma correctly so as not to miss a systemic disease. Cutaneous scleroderma presents with a thickened dermis and hyper-pigmented keloid-like lesions. If there is any question, a biopsy should be obtained. On microscopic exam, they find collagen bundles to lie parallel to the dermis with a decreased number of fibroblasts compared with other scar tissues.[10] Sclerotic neurofibroma may also be mistaken for a keloid; however, testing will reveal positive findings of protein S100. Infections such as hair folliculitis can be confused for a keloid. Folliculitis can be bacterial or fungal, and it is important to distinguish infection from a keloid or hypertrophic scar as steroids are contraindicated in an infection.[13]
Prognosis
Hypertrophic scarring has a good prognosis when compared with keloids. Hypertrophic scars typically develop soon after injury and may increase in size for a period before regressing on their own. They have a better response to treatment without recurrence and typically only require a single treatment modality.[14]
As opposed to hypertrophic scars, keloids have a worse prognosis. Keloids tend to have a genetic component, and at-risk patients can develop multiple keloids from surgeries or injuries. Keloids can continue to develop for up to one year and do not spontaneously regress. After treatment, especially surgical excision, keloids have a high rate of recurrence, making treatment difficult. Adjuvant therapies must be incorporated after surgery to aid in the prevention of recurrence.[14]
Complications
Keloids and hypertrophic scars can lead to prolonged pain and pruritus, are cosmetically disfiguring, and can be functionally debilitating, causing emotional and psychological distress to patients. There is an abundance of treatments available, but none are perfect, and they each have their own side effects. Pruritus is the most common complication of keloids and hypertrophic scarring, followed by pain. Depending on location and size, these scars can cause movement restrictions to patients, and there is significant evidence proving a psychosocial aspect of scarring.[2]
Treatments are also not without consequences. There is a risk of recurrence of keloids and hypertrophic scars with any therapy, with the highest recurrence rate following surgical excision of keloids. Steroids carry a risk of telangiectasias, atrophy, and changes in pigmentation around the treatment site. Cryosurgery frequently causes hypopigmentation to the treatment area and can cause blisters and pain. Radiation therapy has a risk of malignancy, although they have observed no cases of malignancy following radiation therapy for keloids and hypertrophic scarring.[1]
Deterrence and Patient Education
Patients should receive education on the risk factors of keloids and hypertrophic scars. They should counsel those at risk for forming these scars before any surgical procedure on prevention and alternative forms of management. Although any injury or surgery can lead to a scar, the increased incidence of pain and pruritus, as well as the potential for functional disability, is much higher in keloids and hypertrophic scarring. Although there are several modalities of treatment available, there is no therapy that is completely effective in preventing and treating these scars. Especially with keloids, there is a high incidence of recurrence despite the method of treatment used. Patients need to work closely with a dermatologist to appropriately treat and manage these scars to prevent further enlargement and disability associated with keloids and hypertrophic scars.[14]
Enhancing Healthcare Team Outcomes
Keloids and hypertrophic scars used to be diagnosed and managed by primary care clinicians. However, with such a vast array of treatments available, dermatologists and possibly a plastic surgeon should be incorporated into the interprofessional team that treats and manages these conditions. Correct diagnosis is vital so as not to miss a systemic disease or malignancy.[13] A necessary diagnostic measure in differentiating these scars from other diagnoses is a biopsy. It may be important for a pathologist to review biopsy findings to come to a definite diagnosis.
If performing a surgical excision, having a surgeon specializing in this area, such as a plastic surgeon, is vital to ensure the best outcome possible. There may also be a need for a wound nurse to manage pressure and occlusive dressings after surgery. Data proves that taking these measures after surgery leads to an improvement in size and decreased recurrence rates.[11] Treatments that involve radiation therapy may require a radiologist to aid in treatment, and pharmacists are important in the proper dosing and prescribing for newer treatments involving 5-fluorouracil, interferon, bleomycin, and other adjuvant therapies. With this interprofessional approach and early, aggressive treatment, keloid and hypertrophic scar formation may be prevented or significantly improved. [Level 5]

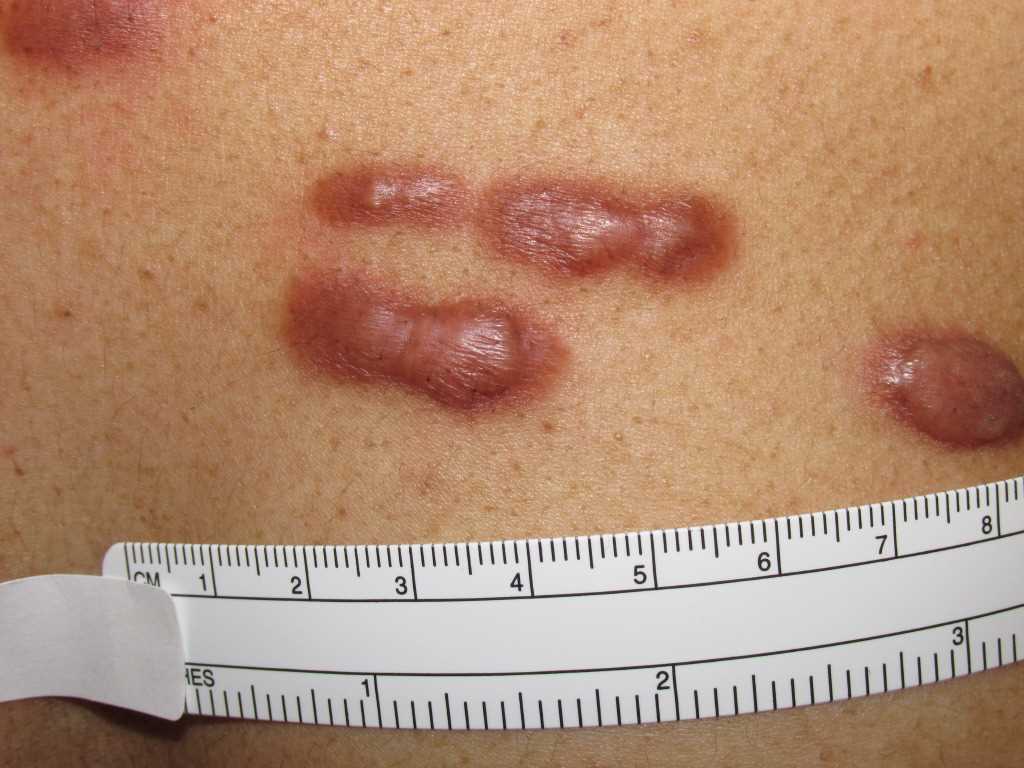
![Keloid, [SATA]](/pictures/getimagecontent//6496)