Continuing Education Activity
Pityriasis versicolor, or tinea versicolor, is a common, benign, superficial fungal skin infection. The causative organism, yeast from the genus Malassezia, is part of the normal skin flora. Clinical features of pityriasis versicolor include either hyperpigmented or hypopigmented scaly macules. The most frequently affected sites are the trunk, neck, and proximal extremities. This activity reviews the evaluation and management of pityriasis versicolor and highlights the role of interprofessional team members in collaborating to provide well-coordinated care and enhance patient outcomes.
Objectives:
Identify the clinical manifestations of tinea versicolor to make an accurate diagnosis.
Differentiate tinea versicolor from other dermatological conditions with similar presentations.
Implement evidence-based treatment modalities for tinea versicolor.
Apply effective strategies to improve care coordination among interprofessional team members to facilitate positive outcomes for patients undergoing treatment for tinea versicolor.
Introduction
Tinea versicolor, or pityriasis versicolor, is a common, benign, superficial fungal skin infection. Saprophytic, lipid-dependent yeast from the genus Malassezia, previously Pityrosporum, are the causative organisms and part of the normal skin flora.[1] Tinea versicolor is not a dermatophyte infection like other forms of tinea. Clinical features are either hyperpigmented or hypopigmented macules with fine overlying scales. The most frequently affected sites are the trunk, neck, and proximal extremities.[2][3][4] The diagnosis of pityriasis versicolor is typically clinical. When the diagnosis is uncertain, a Wood's lamp and microscopic examination of scales soaked in potassium hydroxide may be helpful. Medical treatment is effective for tinea versicolor; however, the condition often returns, so preventive medicine may be essential over a more extended period. This topic discusses the etiology, diagnosis, and management of tinea versicolor.
Etiology
Tinea versicolor is caused by Malassezia, a dimorphic lipophilic fungus previously known as Pityrosporum. Malassezia is a component of the normal skin flora. Clinical disease develops when Malassezia transforms from yeast into its mycelial form. Researchers have identified 14 species of Malassezia to date.[4] The primary species responsible for tinea versicolor are Malassezia furfur, Malassezia globosa, and Malassezia sympodialis, with M. globosa being the most prevalent.[5][6][7][8]
Epidemiology
Tinea versicolor is common worldwide but most prevalent in warm and humid regions. Tinea versicolor can reach a prevalence of up to 50% in tropical countries, while in colder climates such as Sweden, it can be as low as 1.1%. Adolescents and young adults experience the highest incidence, possibly because their sebaceous glands produce more sebum, which creates a lipid-rich environment that promotes the growth of Malassezia. However, there have been reported cases in infants and children.[9] Tinea versicolor affects men and women equally, without any specific ethnic predominance.[10][11]
Pathophysiology
Malassezia is normally present on healthy skin, primarily in oily regions like the face, scalp, and back. However, if it transforms into its pathogenic filamentous form, it can cause tinea versicolor. The precise elements in the host's environment that trigger tinea versicolor still need to be clarified. Although experimental inoculations using topical oils and occlusion have proven successful, tinea versicolor is not contagious.[12][13]
Poor hygiene is not a causative factor. Environmental factors like heat and humidity, pregnancy, oily skin, and applying oily lotions and creams increase the risk of tinea versicolor.[13] Genetic predisposition and a hereditary component may play a role.[14][15] A survey found that 21% of patients with tinea versicolor reported a positive family history. Immunocompromised individuals are at an increased risk of developing tinea versicolor, suggesting that an altered immune response in the host may play a role in the condition's etiology.[16] Malnutrition and the use of oral contraceptives may also act as risk factors.[17]
The word "versicolor" was coined to describe the condition because of the potential for alterations in cutaneous pigmentation. While the specific causes of pigmentary variation remain unknown, several hypotheses exist. The symptoms of hypopigmented tinea versicolor, in which the skin does not darken in response to sun exposure, are generally most noticeable in the summer. Azelaic acid, a dicarboxylic acid generated by Malassezia, may have a role in the etiology of hypopigmentation due to its inhibitory or harmful actions on melanocytes.[18][19] An inflammatory response to the yeast could cause hyperpigmented and erythematous lesions.[18]
Histopathology
A skin biopsy is not required to confirm the diagnosis. If the patient undergoes a skin biopsy, histological findings are hyperkeratosis, acanthosis, and a mild superficial, perivascular infiltrate in the dermis. Fungal elements primarily localize within the stratum corneum and are frequently observable in sections stained with hematoxylin-eosin.
Microscopically, using potassium hydroxide, short hyphae, and yeast cells are visualized in a pattern often likened to spaghetti and meatballs. Periodic acid-Schiff staining may improve recognition of the fungus. Hypopigmented lesions typically contain fewer hyphae and spores than their hyperpigmented counterparts. In hypopigmented lesions, the horny layer is typically mildly hyperkeratotic, and the stratum spinosum may contain fewer melanosomes.[20]
History and Physical
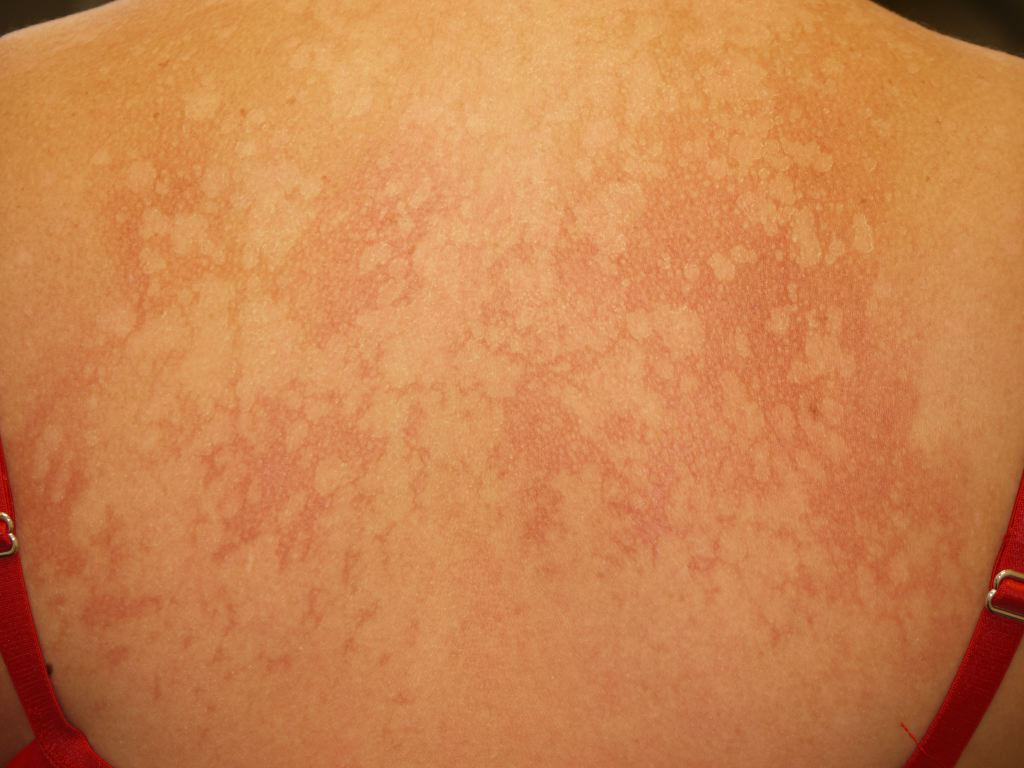
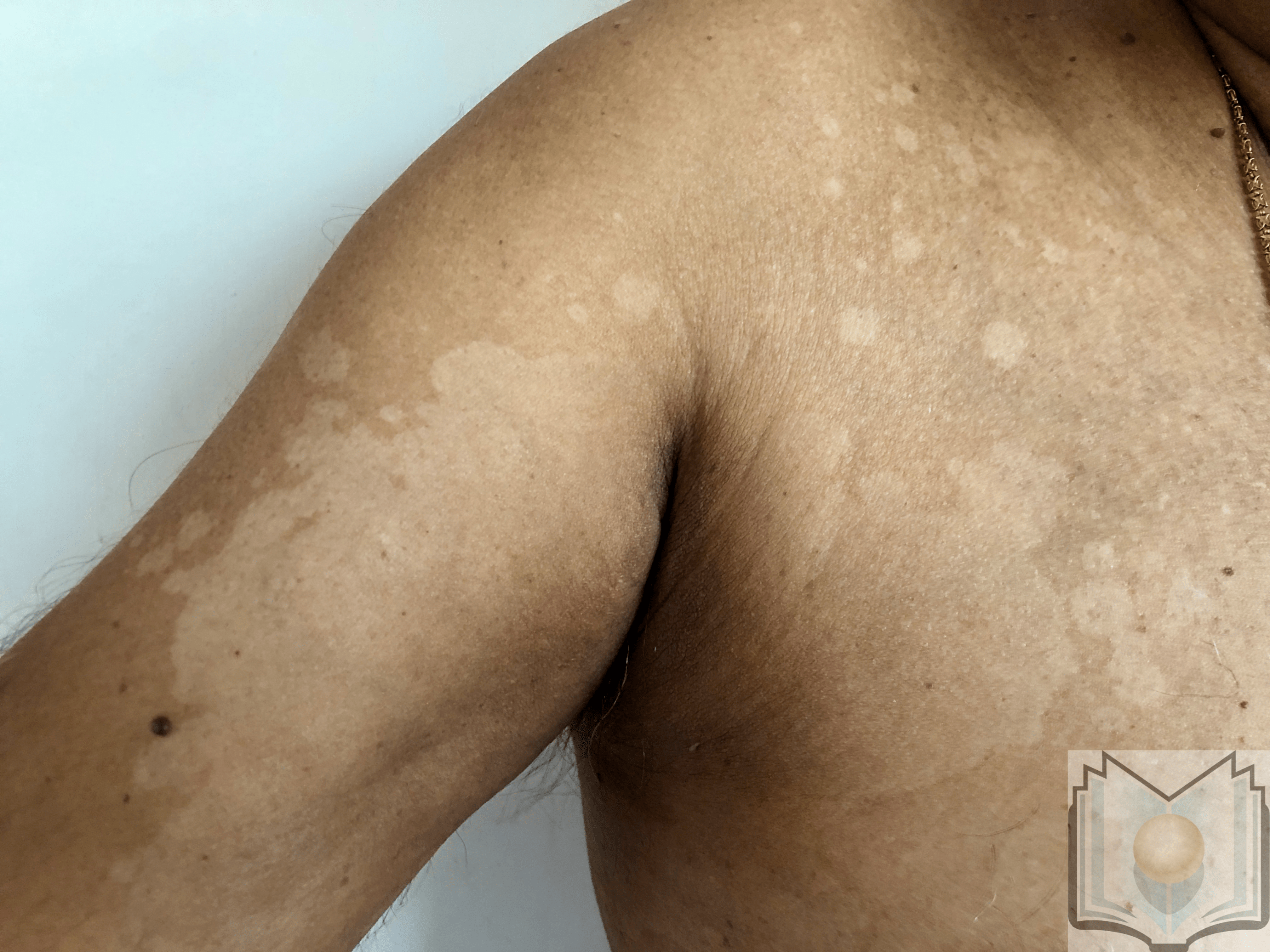
The characteristic feature of tinea versicolor is multiple, well-demarcated, oval, finely scaling patches or plaques. Skin lesions may be hypopigmented, hyperpigmented, or erythematous and occasionally become confluent and widespread. Hyperpigmented tinea versicolor is typically a light brown in those with a fair complexion. In patients with darkly pigmented skin, hyperpigmented tinea versicolor can manifest as macules and patches ranging from dark brown to grayish black. Affected areas can vary in hue on the same person and can differ for people of the same skin tone. The overlying scale may not be readily apparent on the lesions, but stretching or scraping the affected skin easily provokes it, known as the "evoked scale sign."
Lesions that have been burned out or treated often lack scale.[21] The distribution of affected skin reflects the lipophilic nature of the fungus since the upper trunk and proximal arms are predominantly involved. The face may also be affected, particularly in children. Tinea versicolor skin lesions are usually asymptomatic or slightly pruritic. However, severe pruritus can be present in hot and humid conditions.
Tinea versicolor can manifest in four distinct variants, plus a rare atrophic form.
Form 1
Form 1 presents as multiple oval-to-round macules with distinct, well-defined borders. These macules have fine scales and are primarily found on the upper trunk but may also extend to the lower trunk, neck, and proximal extremities. Over time, the macules tend to blend together, creating irregular patches of altered pigmentation. In the summer, the contrast in pigmentation between the affected and healthy skin becomes more noticeable. Light scratching with a scalpel or the edge of a glass slide easily produces a fine, powdery scale on the affected skin.
Form 2
Form 2 of tinea versicolor is an inverse variation that primarily affects areas with skin folds, the face, or isolated regions of the extremities. Form 2 is most common in individuals with compromised immune systems. The condition often involves the creases between skin folds. Form 2 can be mistaken for other skin conditions such as candidiasis, seborrheic dermatitis, psoriasis, and dermatophyte infections.
Form 3
Located primarily on the back, torso, and extremities, form 3 of tinea versicolor affects the hair follicles. This variation may result in lighter or darker skin around the hair follicles. Clinically, it can be challenging to differentiate from bacterial folliculitis. Folliculitis caused by Malassezia appears as red bumps or pustules around the hair follicles. Risk factors for Form 3 include diabetes, high humidity, using steroids or antibiotics, and immunosuppressive therapy.
Form 4
Form 4 of tinea versicolor appears as multiple small, solid, reddish-brown, and uniform inflammatory bumps measuring about 2 to 3 mm in diameter. These bumps may not have the characteristic fine, white scales seen in other forms. They are usually painless and found on the torso. Microscopic examination of the affected skin reveals not only fungal hyphae and spores in the outermost layer of the skin but also an interface dermatitis in the top layer of the deeper skin tissue.
Atrophying Tinea Versicolor
Atrophying tinea versicolor is an uncommon variant characterized by oval-to-round, reddish lesions that may occasionally appear ivory. These lesions typically have a wrinkled appearance and only affect the areas of the skin affected by tinea versicolor. When examined under a microscope, these lesions display epidermal atrophy, vascular ectasia, and decreased collagen and elastic fibers. Patients with a coexisting condition requiring prolonged use of topical corticosteroids often report these lesions. However, atrophying tinea versicolor has also been observed in patients who have never used topical corticosteroids.
Evaluation
The diagnosis of tinea versicolor can be made based on its characteristic clinical presentation of hyperpigmented or hypopigmented, finely scaling patches or plaques.[22][23][24]
If the symptoms are unclear diagnostically, dermoscopy and Wood's lamp examinations may be helpful. A Wood's lamp examination may help to demonstrate the gold-yellow, yellow-green, or coppery-orange fluorescence of tinea versicolor. Fluorescence is present in less than 50% of affected patients.[8][25] Common dermoscopic findings include a fine scale and a "contrast halo" sign, or ring of hypopigmentation surrounding the primary lesion of increased pigmentary network in a hyperpigmented lesion or a ring of increased pigmentation surrounding the primary lesion of decreased pigmentary network in a hypopigmented lesion.[26][27]
A microscopic examination of scales soaked in potassium hydroxide (KOH) provides a definitive diagnosis. The classic findings are grape-like clusters of yeast cells and long hyphae. Since the standard potassium-hydroxide mount lacks color contrast, methylene blue, ink blue, or Swartz-Medrik stain may be added for better visualization. Attempting to culture Malassezia species is known to be challenging, as they require fastidious culture conditions.
Treatment / Management
Prior to treatment, inform patients that the causative agent of tinea versicolor is a commensal fungal inhabitant of the normal skin flora, and the disease is not contagious.[28][29][30] Also, pigmentary alterations frequently persist following successful treatment. Restoration of normal pigmentation may take months following treatment.
Topical Medications
Topical medications are the first-line therapy for tinea versicolor. Ketoconazole, 2% shampoo, is highly effective. The shampoo is applied to the affected areas for five minutes before being rinsed. Typically, healthcare professionals use ketoconazole over 1 to 3 days. Three days are recommended, given the recurrence rate of tinea versicolor and the potentially difficult-to-reach affected areas. In a randomized study, a single application of 2% ketoconazole shampoo was compared to three consecutive days of treatment. Approximately 80% of patients treated with both regimens exhibited mycologic cure.[31] Other acceptable topical alternatives are:
- selenium sulfide 2.25% to 2.5% shampoo or lotion applied for 10 minutes daily for 1 week
- topical 1% terbinafine once or twice daily from 1 to 4 weeks
- ciclopirox 1% applied twice daily for 2 weeks
- zinc pyrithione 1% daily for 5 minutes for 2 weeks[32]
Oral Therapy
First-line treatment for limited tinea versicolor does not typically involve systemic therapy. Oral therapy is reserved for patients with tinea versicolor resistant to topical treatment or with widespread disease that makes topical drug application problematic. Before considering retreatment, confirmation of treatment failure is essential since pigmentary changes can persist for months after treatment. The preferred oral agents are itraconazole 200 mg daily for seven days and fluconazole 300 mg weekly for 2 weeks. Another effective therapy is oral itraconazole 200 mg for 5 to 7 days.
Oral terbinafine, in contrast to topical terbinafine, is ineffective. Likewise, griseofulvin is ineffective.[33] Systemic azole antifungals can cause abnormalities in liver function tests and significant drug interactions.
Although oral ketoconazole was effective for tinea versicolor in small randomized trials, life-threatening hepatotoxicity, adrenal insufficiency, and multiple potential drug-drug interactions have been reported with oral ketoconazole therapy, making it an unfavorable treatment option.[34][35]
Patients with recurrent tinea versicolor, particularly immunocompromised individuals, can prevent recurrences with topical or oral preventive therapy, especially during warm temperatures. Prophylaxis with topical selenium sulfide 2.5% or ketoconazole 2% shampoo applied to the entire body for ten minutes once per month is one such measure. Prophylactic doses of oral itraconazole 200 mg twice daily, once each month, are also employed. After 6 months of preventive treatment with itraconazole, a higher percentage of participants were symptom-free compared to placebo (88% vs. 57%).[36]
Alternative Therapies
A limited number of studies have demonstrated the efficacy of the 308-nm excimer laser, narrow-band ultraviolet UV-B phototherapy, 5-5-aminolevulinic acid- and methylene blue photodynamic therapy in treating tinea versicolor.[37] To confirm or refute these findings, well-designed, large-scale, multicenter, randomized, placebo-controlled trials are required.
Differential Diagnosis
Tinea versicolor may be confused with various conditions. A potassium hydroxide preparation can provide a definitive diagnosis and differentiate tinea versicolor from similar appearing conditions. The differential diagnosis includes:
Seborrheic Dermatitis
Seborrheic dermatitis of the trunk is frequently more erythematous and has thicker scales. Patients with seborrheic dermatitis frequently show involvement in additional locations, including the scalp, eyebrows, and nasolabial folds.
Pityriasis Rosea
Pityriasis rosea presents as inflammatory macules surrounded by a collarette of scales on the trunk in a "Christmas tree-like" pattern. Often, a bigger herald patch manifests before the general eruption.
Erythrasma
Erythrasma manifests as erythematous or hyperpigmented regions in the axillae or groin. Unlike tinea versicolor, the lesions of erythrasma emit a coral-red fluorescence when illuminated with a Wood's lamp.
Pityriasis Alba
Pityriasis alba is a mild form of eczematous dermatitis characterized by hypopigmented macules and tiny patches on the face and, to a lesser extent, the upper extremities. A fine scale may be visible. The lesions are accentuated but nonfluorescent on examination with a Wood's lamp. The disorder is most prevalent in children with a history of atopic dermatitis.
Secondary Syphilis
Secondary syphilis may exhibit erythematous to brown macules, papules, or small lesions with a generalized distribution. The palms and soles are frequently affected.
Tinea Corporis
Tinea corporis is a dermatophyte infection of the skin not involving the feet, groin, face, scalp hair, or beard hair.
Vitiligo
Completely depigmented macules and patches of the skin characterize vitiligo. Tinea versicolor only causes hypopigmentation.
Confluent reticulated papillomatosis of Gougerot and Carteaud
Confluent reticulated papillomatosis of Gougerot and Carteaud is an uncommon disorder of keratinization that typically affects young adults. Affected patients present with hyperpigmented, scaly macules that combine to form patches with a reticulated appearance. The neck, intermammary region of the chest, and upper back are affected.
Guttate Psoriasis
Guttate psoriasis presents as small, erythematous, scaling plaques affecting primarily the trunk and upper arms. The plaques often appear inflamed and in the shape of drops. Guttate psoriasis commonly follows a streptococcal infection.
Mycosis Fungoides
Mycosis fungoides may manifest as hypopigmented skin patches, with a preference for the trunk and extremities. This variant of the disorder is most prevalent among people with dark complexions. There may also be fine scales, erythema, or infiltrated plaques.
Terra Firma-Forme Dermatosis
Terra firma-forme dermatosis is a benign condition in which hyperkeratosis due to decreased normal desquamation results in the appearance of hyperpigmented papules or plaques that resemble dirty skin. Common sites include the neck area and the ankle. Unlike tinea versicolor, alcohol swabs remove the lesions.[38]
Prognosis
Oral and topical antifungal agents are effective; however, disease recurrence is common and may impact a patient's quality of life. Preventive therapies are likely beneficial. Also, patients must be reminded that despite successful eradication, pigmentary changes may take weeks or months to clear. Some cases of spontaneous resolution occur, but if left untreated, the disease can be chronic.
Complications
Hypopigmentation and hyperpigmentation can persist for months after successful treatment of tinea versicolor, leading patients to believe the treatment was unsuccessful inaccurately. The presence of scales and a positive KOH preparation indicate active infection. Drug resistance, disease recurrence, or disease dissemination should prompt the consideration of an immunodeficient state. There have been reports of hair thinning and loss within tinea versicolor lesions. Most commonly, hair thinning or loss occurs on men's forearms, abdomen, neck, and beard regions.[39]
Deterrence and Patient Education
The cause of tinea versicolor is a fungus usually present on the skin. Generally, this fungus does not cause any problems, but a rash can develop in people living in hot and humid climates. Tinea versicolor causes multiple small patches of the skin to have more or less color than usual. The colors vary from white to light brown, dark brown, gray-black, or pinkish red. The rash most often appears on the upper back, chest, and upper arms. Tinea versicolor is not contagious.
Treatment is usually topical with antifungal creams, lotions, or shampoos and may last from 1 day to 4 weeks, depending on the treatment suggested. Oral medications are available for more extensive infections or when topical treatments do not work. Tinea versicolor has a high recurrence rate, and many patients successfully prevent recurrence by using preventative treatment once a month for 6 months. The pigmentary changes that may have occurred due to the condition take longer to resolve than the actual infection. Most of the time, they resolve within 2 to 4 months of starting treatment.
Pearls and Other Issues
Pityriasis versicolor is a benign but commonly recurrent superficial fungal infection of the skin. Therefore, patients need effective follow-up care to implement a relapse prevention strategy.
Enhancing Healthcare Team Outcomes
Tinea versicolor is a relatively common skin disorder likely to be encountered across multiple medical specialties. Awareness of the etiology and presentation of tinea versicolor across specialties can prevent unnecessary isolation in group settings. Effective communication within the patient's healthcare team is necessary to ensure all clinicians know the treatment to avoid any possible medication interactions if oral therapy is elected. Proper patient education by the healthcare team can decrease patient anxiety regarding transmission, permanent skin color changes, and recurrence to provide the best patient outcome.[40][41]