Continuing Education Activity
Syndactyly is one of the most common congenital anomalies of the extremities. It fails to differentiate the digits, defined as a fusion of adjacent digits. Syndactyly can be seen in the upper and lower extremities, and up to 50% of cases are bilateral. To avoid the morbidity associated with this condition, it must be promptly diagnosed and treated. This activity reviews the evaluation and treatment of syndactyly and highlights the role of the interprofessional team in evaluating and treating patients with this condition.
Objectives:
Determine the etiology of syndactyly.
Interpret the evaluation of syndactyly.
Identify the surgical management of syndactyly.
Communicate interprofessional team strategies for improving care coordination and communication to treat syndactyly and improve outcomes adequately.
Introduction
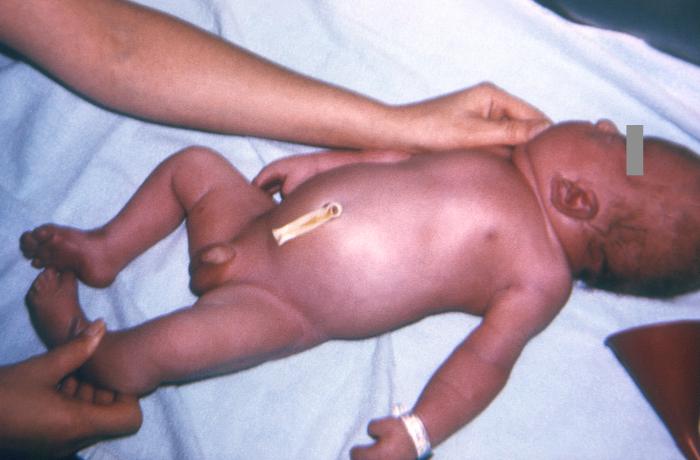
Syndactyly is 1 of the most common congenital anomalies of the extremities. Syndactyly refers to the soft tissue and/or osseous fusion of adjacent digits in the upper or lower extremity. This results in the appearance of "webbed" or "super" digits, depending on the extent of the anomaly. Syndactyly is described as simple or complex, depending on the bony fusion's presence (complex) or absence (simple). Complete syndactyly extends to the tip of the digits, including the nail folds, while incomplete syndactyly does not extend the full length of the digit. Complicated syndactyly is defined by interposed accessory phalanges or abnormal bones.[1] The most prevalent location is between the second and third toe in the feet and between the long and ring fingers in the hand. Syndactyly is most likely to present as an isolated phenomenon following autosomal dominant inheritance with incomplete penetrance but is also associated with multiple genetic syndromes such as Apert and Poland syndrome. Syndactyly is better tolerated in the feet than the hand, where independent digital motion is needed. Except for mild cases, surgical separation of the digits is often indicated to optimize hand function (See Image. Syndactyly, a Common Congenital Anomaly of the Extremities).[1][2][3][4][5]
Etiology
In the developing human, all digits are initially fused by a layer of loose mesenchymal tissue - syndactyly occurs as a failure to separate this fusion. Limb development begins in the fifth week of gestation, deep to a region of the ectoderm known as the apical ectodermal ridge (AER). The AER is responsible for the longitudinal growth of the limb. Development begins with the activation of mesenchymal cells in the somatic lateral mesoderm. The hands start developing during the sixth week when mesenchymal tissue of the hand plates begins to form the phalanges. The feet undergo a very similar process in the seventh week of development. Digits form due to signaling from the zone of polarizing activity (ZPA) through sonic hedgehog protein (SHH). Higher concentrations of SHH lead to the formation of the ulnar aspect of the limb, and lower concentrations are seen away from the ZPA, leading to radial-sided limb development. Finally, the dorsal and volar ectoderm are responsible for developing the dorsal and volar structures of the extremity. As development continues, “notches” form between the digits at the AER. These notches progress proximally as the previously fused mesenchymal tissue undergoes apoptosis, separating the digits via BMP-4 signaling pathways. The digits have formed by the end of the eighth week of development.
The failure of apoptosis separating the mesenchymal tissue or the failure of notch formation in the AER leads to syndactyly.[2][6][7] In the absence of an associated syndrome such as constrictive ring syndrome, Poland syndrome, Apert syndrome, and Carpenter syndrome, among others, syndactyly demonstrates an autosomal dominant inheritance pattern with variable penetrance. Inherited syndactyly has been linked to defects on the second chromosome.[1][2][3][4][5]
Epidemiology
Syndactyly is found in approximately 1 in 2000 live births.[1][2][3][4] It accounts for 20% of congenital hand malformations and is the most common congenital anomaly of the hand.[3] The condition affects the feet more often than the hands. It occurs bilaterally in 50% of cases. Syndactyly is most often an isolated autosomal dominant inherited condition. Penetrance is incomplete and also decreased in females compared to males. The frequency of syndactyly in males is nearly twice that of females. It is more likely to occur in Whites as compared to other races. Spontaneous isolated forms of syndactyly also exist. Syndromic syndactyly occurrences are associated with many genetic disorders, including Poland syndrome, Apert syndrome, Carpenter syndrome, and constrictive ring syndrome.[1][2][3][4]
History and Physical
A thorough history and physical exam should be performed on children presenting with syndactyly. Any family history of syndactyly should be noted. Incomplete penetrance may result in situations where syndactyly may "skip" a generation. It is important to ascertain if there were any pregnancy or birth complications. A thorough newborn orthopedic exam should be considered for patients presenting as neonates or infants to search for any suggestion of an underlying syndrome. It is important to note that isolated simple syndactyly is not typically associated with an underlying genetic syndrome.[3] Other examinations, such as testing for hip dysplasia, infantile reflexes, metatarsus adducts, sacral dimpling, and spine examination, should be considered in any newborn or infant presenting for evaluation. If there are physical exam findings concerning an undiagnosed genetic syndrome or complicated or complex syndactyly, referral to a geneticist would be warranted.
With specific attention to the syndactyly deformity, which digits are affected should be noted, whether the affected digits appear to be fused via soft tissue only or a combination of bony and soft tissue fusion. The distal extent of the interdigital connection should be noted. If there is a question of subtle incomplete syndactyly, a physical examination of the fingers in the sagittal plane is useful. Normally, the web spaces are angled at or near 45 degrees with 1 of the affected digits extended and the adjacent digit flexed. The presence of flexion and extension creases in the affected digits should be evaluated as they can give a clue to the underlying bony fusion and function of the digits.[3] The examiner should assess the ability of the affected digits to demonstrate independent motion. If independent motion of the digits is not demonstrated, complex or complicated syndactyly becomes more likely. Length differences between the adjacent affected digits should be observed and noted. The examiner should assess both hands and feet to ensure no other areas of syndactyly or accessory digits are present. Finally, it is important to discuss with the patient and family that there is, on average, a 30% skin shortage around the affected digits.[2] Hence when the affected digits are separated, skin grafting may be indicated for a tension-free closure.[2][3][4][5][8]
As some patients may have had previous treatment or surgery, history should also include previous records and operative reports. Photographs before surgery or demonstrating the progression of creep post-surgically may be useful. The skin should be examined for previous scars and skin donor sites to help plan future incisions. In a revision setting, thorough sensory and vascular examinations should be performed.
Evaluation
After assessing the patient’s extremity, multiplanar radiographs of the affected hand or foot are indicated. X-rays evaluate for osseous fusion of the phalanges and/or metacarpals. It is also valuable in assessing for possible supernumerary digits that may have not been noticed on physical examination. After the physical exam and imaging have been performed, the deformity can be classified. Classification can be descriptive, including terms such as incomplete or complete (involvement of the entire length of the digit), simple or complex (presence of bony fusion), and/or complicated (presence of accessory phalanges or abnormal bones).[1] Another classification commonly cited is the Tentamy and McKusick classification:
- Type I: Most common with involvement of the long and ring fingers in the upper extremity or second and third toe in the lower extremity. Follows an autosomal dominant pattern with incomplete penetrance
- Type II: Synpolydactyly with the involvement of the long and ring fingers in the upper extremity and/or fourth and fifth toes in the lower extremity with an accessory digit in the syndactyly web.
- Type III: Syndactyly involved in the ring and small finger.
- Type IV: Complete syndactyly of all fingers
- Type V: Metacarpal or metatarsal fusions of the ring and small finger in the upper extremity and third and fourth toes in the lower extremity.[9]
Advanced imaging is usually not necessary in cases of simple syndactyly. However, in cases of complex and/or complicated syndactyly, MRI imaging may be useful to assess the location of flexor tendons and neurovascular structures before planned surgery.
Treatment / Management
Syndactyly can be managed by operative and nonoperative means. Simple syndactyly of the toes is typically managed non-operatively if it is not affecting function. Surgery for cases of isolated syndactyly of the toes in this circumstance is of cosmetic benefit. It should only be performed after thoroughly discussing risks with the patient and family. Other indications to pursue nonoperative management include incomplete simple syndactyly and webs associated with super digits. Superdigits have been classified into 2 types: Type I involves 2 metacarpals that support 1 oversized digit, and type II involves a single metacarpal supporting multiple digits.[5][10] Surgery involving separating these digits often proves unsuccessful with unsatisfactory results. Other contraindications to surgical management include complex synpolydactyly, where the hand functions as a unit or hands with no active muscular control.[5] Essentially, nonoperative management is pursued if the surgeon does not believe the function of the affected hand/foot is not improved with surgery.
Operative management is common for syndactyly to produce a more functional hand (or foot). If operative management of syndactyly is warranted, the timing of the surgery is important to discuss. Typically, syndactyly releases are performed around 12 to 18 months of age. Delaying the surgery until the child is older than 18 months reduces the risk of scar contracture and webspace creep as the child grows. However, syndactyly of border digits (small finger and thumb webspace) and syndactyly with multiple fusions should prompt earlier release as the smaller digit tethers, the longer digit as the patient grows. Release occurs around 6 months of age to avoid angulation, rotary, or shortening of the adjacent digit and allow for early development of grip and coordination.[2][4][5][8]
Surgical Release
Multiple nuances exist in the surgical release of syndactyly, depending on the complexity of the involved digits. With this in mind, we discuss simple, complete syndactyly and describe modifications when more complexities are encountered. It is important to note that loupe magnification or using an intraoperative microscope is mandatory to achieve a successful outcome and limit the risk of neurovascular complications.
Achieving the optimal surgical outcome for patients with syndactyly is multifactorial and consists of multiple goals. Goals include (1) creating new paronychial nail folds, (2) developing the interdigital commissure (skin) of the digits to be separated, and (3) creating a new webspace.[2] Multiple techniques have been described to separate the digits, but the most described is the dorsal and volar-based zig-zag incision described by Cronin.[11]
The zig-zag approach to the commissure allows for triangular-based flaps to assist with the coverage of the digits. Planning the incision should start distally at the fingertips, where planning for the paronychial fold begins. The typical technique for developing these folds involves laterally based triangular flaps that, once released, are sutured into the respective digit, creating a new nail fold.[12] Next, the dorsal and palmar incisions are drawn proximally in a zig-zag fashion to create the previously described triangular flaps. It is important to draw the flaps so that the dorsal and volar flaps are not interdigitated.[8] As the incision is planned distally, the planned height of the web space is determined. Once determined, a dorsal rectangular flap is typically drawn with a volar triangular-based flap. Once the incisions are drawn, the case starts distally, starting with the paronychial folds and progressing about the dorsal incision. It is important to create full-thickness flaps as you proceed with your dissection. Careful dissection is carried out to identify the neurovascular bundles. Typically, these bifurcate proximally, but cases have been noted with a more distal bifurcation. If a distal bifurcation is noted, it is important to carefully dissect each neurovascular bundle so they can be incorporated into the correct digit. Once the dorsal dissection is completed, attention can be turned volar, and the separation can be completed. Next, tension-free closure is performed. If any areas of skin cannot be closed adequately with tension-free closure, full-thickness skin grafts from the hypothenar eminence, instep of the foot, wrist, cubital fossa, or groin can be obtained to fill the defects.[2][3][4][5][8][13] When selecting a skin graft, it is important to take from an area lacking hair growth, as this could lead to an undesirable cosmetic result. It is important to avoid split-thickness grafts as these are known to contract up to 50% and achieve an undesirable post-operative result.[3]
Other cases to consider include incomplete syndactyly, syndactyly of multiple digits, and complex syndactyly. In incomplete syndactyly, multiple flaps can be considered. The goal of the surgery for incomplete syndactyly depends on the length of the fusion of the affected digits. If one-third or less of the length of the digits is involved, a dorsal rectangular flap with volar-based triangular flaps can be utilized to reconstruct the webspace successfully.[2][3][5][14] A modified double reverse z-plasty has also been described to reconstruct the webspace.[2] The goal is to reduce the length of the webspace 1:1 as compared to the width of the webspace.[5] In cases of syndactyly involving the thumb, a 4-flap z-plasty or central V-Y advancement with laterally based z-plasty has been described.[5][15][16] The surgeon must release the patient’s syndactyly in stages when multiple digits are involved. Performing a syndactyly release on the radial and ulnar aspects of the digit simultaneously can risk vascular compromise to the digit.[2][3][5] It is recommended that, in this case, the patient’s surgery is performed in stages. For example, if all the digits in the hand, excluding the thumb, are involved, the first stage of the surgery could involve the release of the ulnar border of the index finger and the radial border of the small finger. A second stage, typically performed approximately 6 months later, would involve separating the ring and long finger.[3]
Finally, additional operative steps are required when bony fusion is involved (complex syndactyly). When planning on separating fused phalanges, preoperative planning is essential. Synostosis separation must be planned to retain as near normal anatomy as possible. In complex cases closing wedge, osteotomies may be indicated to correct for angulation differences. Collateral ligament integrity should be tested intraoperatively to determine if advancement or reconstruction is indicated. In complex and complicated syndactyly cases, the amputation of a nonfunctional ray may achieve a more functional hand than reconstruction and needs to be evaluated by the surgeon on a case-by-case basis.[5]
Differential Diagnosis
Syndactyly is typically easy to diagnose on physical exam; however, congenital hand deformities and syndromic conditions should be considered when evaluating a child for syndactyly.
- Poland syndrome
- Apert syndrome
- Ectrodactyly (cleft hand)
- Constriction band syndrome
- Synpolydactyly
- Carpenter syndrome
- Oculodentodigital dysplasia
Prognosis
The prognosis depends on the treatment strategy and complexity of the syndactyly. Complex and complicated syndactyly have less optimal outcomes and often require repeat surgical procedures.[8] In the case of simple syndactyly, good short and long-term outcomes have been reported.[8][17][18][19] However, it has been reported that up to 10% of patients undergoing syndactyly surgery require revision surgery at some point in the future.[20]
Complications
As with any surgical procedure, an infection can occur. Although infection is a relatively rare complication of syndactyly surgery, it has the potential to be devastating if not recognized and addressed promptly with surgical debridement or antibiotics. Recent data suggests a postoperative infection rate of 1.6%. Complications from the surgery are more likely to be present in patients with syndromic presentations and multiple preoperative medical diagnoses.[21] Another potential complication is scar formation and contracture.[5] This can be attributed to split-thickness skin graft use or growth of the surrounding bone. Full-thickness graft use is less associated with contracture and is preferred when possible for this reason.[22] Another common complication is web creep. Web creep is defined as the webspace migrating distally as the patient ages. This can lead to a progressive deformity in the hand. The patient's age during the operation may be an important factor concerning web creep. The patient should be followed at regular intervals after surgery to detect this complication at an early stage. Finally, devascularization of the digit or nerve injury can occur. Only 1 side of the digit must be operated on at a time to ensure that the digit retains a functional digital artery.[2][3][4][5] Devascularization may result in prolonged healing and recovery times or, in an extreme situation, create the potential need for amputation. In the setting of nerve injury, multiple techniques have been described to address digital nerve injury, including primary nerve repair, repair with nerve conduit, and nerve grafting. Digital nerve injury, even after repair, may result in loss of or diminished digital sensation.[23]
If nonoperative treatment is chosen, this may lead to diminished dexterity and function in the hands. Nonoperative treatment or observation of syndactyly between digits with length differences may result in increased deformity and growth disturbance. The shorter digit may create a tethering effect on the longer digit, pulling the longer digit into angular deformity toward the shorter digit and flexion.[5]
Postoperative and Rehabilitation Care
Postoperatively, patients are placed into a bulky soft dressing, splint, or cast depending on the complexity of the surgical procedure, surgeon preference, and patient factors that may affect compliance with post-operative care. Dressings are typically taken down at 2 weeks.[2][4] Once incisions have healed, the patient is started on an active range of motion and scar massage. Hand therapy can help the patient with scar massage techniques and assist in gaining range of motion.[4] In the growing patient, it is important to have continued follow-up to assess for complications of web creep. Richterman et al. described a reproducible technique measuring webspace height ratios on radiographs to monitor for this complication.[24]
Consultations
Syndactyly often requires an interprofessional healthcare team to achieve good outcomes. At a minimum, a hand surgeon or orthopedic specialist needs to be consulted for evaluation to assess surgical candidacy. If an underlying genetic syndrome is suspected, a referral to a pediatric geneticist or geneticist is warranted. Finally, physical therapy, occupational therapy, or hand therapy consultations may be indicated to assist with postoperative care, such as pain, scar, and edema control, as well as mobilization of the digits.
Deterrence and Patient Education
As mentioned in the previous sections, discussing with parents if and when surgery is necessary is important. Surgery is indicated for syndactyly if it is felt the function of the affected extremity can be improved. It is also important to educate parents that delaying the surgery until the patient is older improves outcomes unless specific situations, as previously discussed, are involved (border digit involvement and multiple fused digits). Although repeat surgery is relatively uncommon, it is important to discuss with the family complications such as scar formation and contracture, webspace creep, possible devascularization of the digit, and digital nerve injury.
Enhancing Healthcare Team Outcomes
An interprofessional team, including a pediatrician, hand or orthopedic surgeon, hand or physical therapist, and occupational therapist, best manage syndactyly. When a patient's presentation concerns a genetic syndrome, consultation with a geneticist to provide recommendations for further workup and treatment of associated findings is essential. In patients who form hypertrophic scars or in postoperative patients where excessive scar formation is a concern, the involvement of a therapist early may improve the postoperative cosmesis and function and limit contracture.[4] Patients tend to recover well from this operation; however, evidence has demonstrated that some patients require repeat surgery. It is important to understand the patient's financial situation and support system. The involvement of a social worker or case manager may be useful for the patient and aide's decision-making and timing of care. Coordinated interprofessional team dynamics and optimized communication can improve patient outcomes.