Continuing Education Activity
Sever disease, or calcaneal apophysitis, is a common cause of heel pain in children or young athletes aged 8 to 15 with immature skeletons. Sever disease results from repetitive microtrauma to the secondary ossification center by traction of the Achilles tendon insertion on the calcaneus. This overuse injury manifests as traction apophysitis at the heel, directly associated with the insertion site of the Achilles tendon. Children and adolescents experiencing a rapid growth spurt or engaging in sports that entail running and jumping may develop heel pain, which subsides with rest or inactivity. Sever disease follows a self-limited course, and its management involves activity modification or relative rest guided by pain levels. Symptom control incorporates the use of anti-inflammatory medications, ice, heel cups or heel lifts, and, in severe instances, immobilization. This activity delves into the etiology and pathophysiology of Sever disease and explores its evaluation and management while highlighting the crucial role of the interprofessional healthcare team in enhancing care for individuals affected by this condition.
Objectives:
Identify the characteristic signs and symptoms of Sever disease, including heel pain in skeletally immature individuals aged 8 to 15, and distinguish them from other causes of pediatric heel pain.
Screen pediatric patients, especially those undergoing rapid growth spurts or participating in running and jumping sports, for Sever disease through a comprehensive clinical evaluation.
Implement evidence-based conservative management strategies for Sever disease, including activity modification, relative rest, and proper footwear recommendations.
Collaborate with physical therapists, athletic trainers, and other interprofessional healthcare professionals to optimize the interprofessional care approach for patients with Sever disease.
Introduction
Sever disease, or calcaneal apophysitis, is a common cause of heel pain in children or young athletes aged 8 to 15 with immature skeletons.[1] Sever disease results from repetitive microtrauma to the secondary ossification center by traction of the Achilles tendon insertion on the calcaneus.[2] The condition frequently coincides with triceps surae shortening, which stems from the difference in growth rates between bone and muscle.[2] Sever disease is common among children and adolescents who engage in sports that involve running and jumping. The pain occurs due to a sudden increase in sports activities, especially during a rapid growth spurt. However, the pain subsides with rest or when the activity is stopped.[3] Sever disease may also develop in less active adolescents who wear flat shoes.
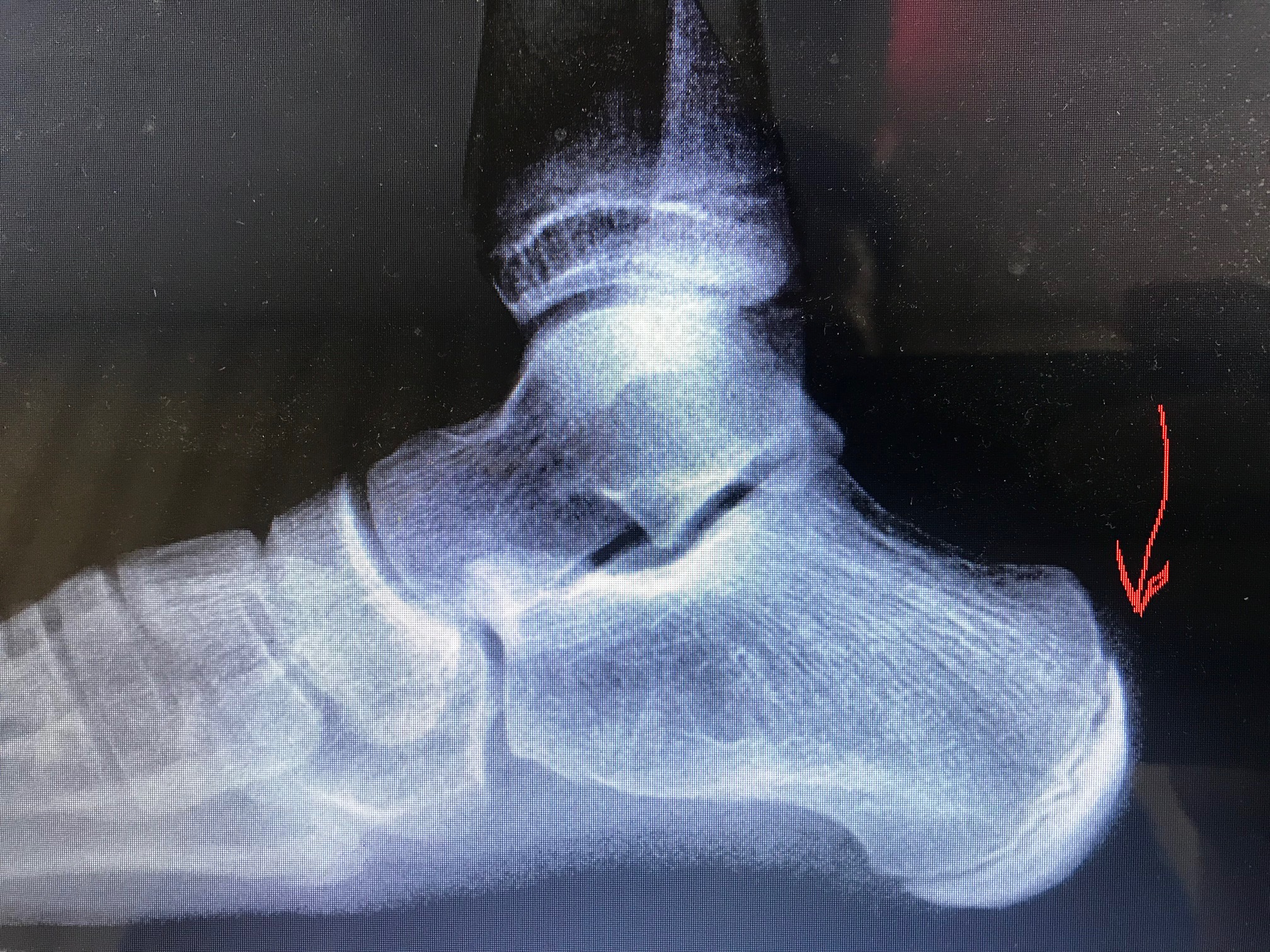
Patients affected by Sever disease usually report pain resolution during periods of rest or when the growth plate fully closes.[4] Clinical examination demonstrates tenderness over the calcaneal insertion point of the Achilles tendon and a positive squeeze test involving manual medial and lateral compression of the posterior calcaneus.[5] The diagnosis of Sever disease is primarily clinical and does not necessitate imaging studies. However, plain radiographs can assist in ruling out bone fractures, whereas magnetic resonance imaging (MRI) is valuable in differentiating Sever disease from infections and tumors.[4]
Sever disease typically follows a self-limited course, and its management involves activity modification or relative rest in response to pain. Symptom control incorporates the use of anti-inflammatory medications, ice, heel cups or heel lifts, and, in severe instances, immobilization.[6] A rehabilitation regimen emphasizing heel cord stretching and strengthening should be integrated into the care plan to alleviate symptoms and address underlying biomechanical factors that may predispose the individual to the condition.
Etiology
Sever disease is an overuse injury due to repetitive strain and microtrauma caused by the force of the strong Achilles tendon on the relatively soft calcaneal apophysis. The calcaneal bone can outpace muscle growth, and a shortened triceps surae directly correlates to the irritation of the apophysis.[7] After periods of rapid growth and increased activity, the force exerted by the Achilles tendon intensifies.
Factors contributing to the risk of Sever disease include a high BMI, increased or excessive sports activity, limited ankle range of motion, poorly cushioned or worn-out athletic shoes, cleated athletic shoes, running on hard surfaces, and biomechanical factors such as genu varum, forefoot varus, overpronation, pes cavus, or pes planus.[8][9] The most prevalent sports associated with this condition involve repetitive running and jumping, including basketball, soccer, track, cross-country, and gymnastics.[2]
Sever disease is not generally associated with traumatic events; however, in rare cases, trauma may lead to a complete avulsion fracture.[10]
Epidemiology
Sever disease predominantly manifests during the rapid growth phase in active children and adolescents aged 8 to 15.[4][10][11] As one of the leading causes of heel pain in adolescents, Sever disease contributes to 2% to 16% of all musculoskeletal complaints in children.[8] Notably, it is common for symptoms of Sever disease to appear on one foot, but up to 60% of patients experience pain in both feet. Males are more likely to develop this condition, with a frequency of occurrence 2 to 3 times higher than in females. The typical age of onset is around 12 for males and 11 for females.[2][10][12]
Pathophysiology
The posterior calcaneus develops as a secondary ossification center that provides the attachment point for the Achilles tendon. During the early adolescent growth spurt, bone growth exceeds the ability of the muscle-tendon unit to stretch sufficiently to maintain previous flexibility. Consequently, increased tension is exerted across the unossified or incompletely ossified apophysis. The apophysis represents the most vulnerable point in the muscle-tendon-bone attachment, unlike the tendon in an adult. Therefore, the apophysis is susceptible to overuse injuries resulting from repetitive stress.
Repetitive and excessive traction exerted by the strong Achilles tendon leads to microtrauma and chronic irritation, resulting in thickening and pain at the apophysis.[12] Thus, the leading theory that attempts to explain the mechanism behind Sever disease relies on the ongoing shear stress and repetitive impact on the open calcaneal apophysis. A study aiming to quantify this mechanism reveals that peak plantar pressure reaches 880 kPa in patients with Sever disease compared to 88 kPa in healthy controls during walking.[10] Intuitively, the peak plantar pressure would further exacerbate during running and jumping, explaining the pain experienced by patients with Sever disease.
History and Physical
The classic presentation of Sever disease involves an active child or adolescent aged 8 to 15 with unilateral or bilateral heel pain that intensifies during and after activity, particularly during running and jumping. The patient will often not recall a specific injury. However, the onset of pain will coincide with a recent growth spurt, a new sport or training, or the beginning of a sports season.[10] Pain typically alleviates with rest and is usually absent in the morning. With time, the pain may intensify, potentially leading to limitations in activity.
The physical examination should reveal no signs of erythema or ecchymosis, but there may be tenderness and mild swelling at the Achilles insertion on the heel. In addition, the physical examination may indicate pain with passive ankle dorsiflexion. Pain can be reproduced with manual medial and lateral compression of the posterior calcaneus and aggravated by standing on tiptoes—a phenomenon known as the Sever sign. Poor heel cord flexibility or dorsiflexion weakness may be observed as predisposing risk factors.[5][13] Upon gait examination, the patient may exhibit a limp or walk on their toes to avoid putting pressure on the affected heel.[1]
Evaluation
Sever disease is primarily a clinical diagnosis; hence, the history and physical examination outlined above are typically adequate for diagnosis.
If the presentation is atypical, severe, or persists after 4 to 8 weeks of conservative management, it is advisable to consider obtaining advanced imaging to rule out infection, neoplasm, or occult fracture. Plain radiographs often reveal sclerosis and widening of the growth plate. However, these changes can also be observed in normal variants.[14] When ordering radiographs, it is recommended to consider bilateral imaging to distinguish osseous abnormalities from normal variants in the individual patient.[5][13] MRI is more effective in differentiating between Sever disease, tumors, and infection.[4]
Laboratory findings typically fall within normal limits. Elevated inflammatory markers such as erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) may suggest osteomyelitis. In less than 50% of cases of calcaneal osteomyelitis, there is an elevated white blood cell count. However, CRP and ESR levels are elevated in up to 77% and 95% of cases, respectively.[15]
Treatment / Management
Sever disease is a self-limiting condition that resolves with maturation and closure of the apophysis.[11] The primary objective of the therapy is pain relief,[4] and there is no indication for operative management in Sever disease.
Limiting Participation in Painful Activities
Individuals should limit strenuous activity, especially running and jumping, and gradually resume participation when their symptoms resolve.[4] In some cases, patients may need to abstain from sports until symptoms subside temporarily.
Ice Application
Individuals should apply ice to the painful area for 20 minutes daily. Ice acts as a vasoconstrictor and reduces the flow of inflammatory cells to the affected area. When used with rest periods, ice aids in diminishing the inflammatory process.
Orthotic Use
Heel lifts, heel cups, and heel pads can reduce traction forces on the apophysis, thereby alleviating pain.[4] These are particularly beneficial in cleated shoes that may exacerbate symptoms by concentrating the impact force on the heel. Custom orthotics also represent a viable option.
Immobilization
Immobilization may be necessary if there is no improvement after 4 to 8 weeks, which involves periods of casting or using a CAM boot.[1][11]
Nonsteroidal Anti-Inflammatory Drugs
In the acute stage, oral non-steroidal anti-inflammatory drugs (NSAIDs) can be utilized to reduce inflammation. However, it is advised not to use anti-inflammatory medications before physical activity to prolong the child's playtime with reduced or no pain. Although topical ketoprofen is effective, it is not recommended for children under 12.[11]
Braces
Braces can be beneficial for barefoot athletes, such as gymnasts and dancers, who cannot wear orthoses. Barefoot athletes with Sever disease using the Cheetah heel cup and X-brace exhibit significantly decreased visual analog scores (VAS) and sports improvement at 2 and 3 months.[8]
Kinesiotherapy and Taping
Limited evidence supports kinesiology taping; however, affected patients report immediate relief. The taping technique regulates blood flow, eliminates inflammatory cytokines, and reduces tension and stress in the affected area.[10]
Stretching and Exercises
Calf stretches can alleviate the discomfort of the Achilles tendon pulling on the posterior calcaneus.[1] Exercising to strengthen adjacent muscles can also reduce the workload on the Achilles tendon.[1]
Physical Therapy
Physical therapy includes calf-muscle stretching, strengthening exercises, ultrasound, and possibly electrical stimulation.[10] In cases where a patient does not show improvement with a home stretching program, the involvement of a physical therapist becomes necessary.
A study comparing rest, orthoses, and physical therapy in treating Sever disease demonstrated a significant decrease in pain with all modalities, with no statistically significant difference between them for pain reduction.
The primary treatment for Sever disease typically involves heel cups, rest, ice, calf stretching and strengthening, and NSAIDs. Severe cases or those unresponsive to physical therapy and other conservative measures may require immobilization using a CAM boot or casting. Orthoses are beneficial when biomechanical factors, such as overpronation, are present. Furthermore, it is essential to maintain well-fitted and up-to-date footwear. Braces can be advantageous for individuals engaged in barefoot activities.
Symptoms typically resolve within a few weeks to months, and Sever disease is generally self-limited. Although recurrence may occur, particularly during periods of increased activity, it will not persist after apophyseal closure. Injection therapy or surgical intervention does not play a role in the management of Sever disease.
Differential Diagnosis
Several conditions may present similarly to Sever disease. Therefore, to properly distinguish between these conditions, it is crucial to conduct a complete medical history and a detailed physical examination.[6] As mentioned earlier, advanced imaging should be ordered for atypical, severe, or persistent presentations. Although most conditions are easily identifiable through MRI, calcaneal fractures and tarsal coalitions can be excluded with plain radiographs.[4][14]
The various conditions that share clinical features with Sever disease and necessitate a careful evaluation for accurate diagnosis include Achilles tendon rupture, Achilles tendonitis, retrocalcaneal bursitis, calcaneus fractures, calcaneal cysts, osteomyelitis, tarsal coalition, plantar fasciitis, heel contusion, posterior ankle impingement, and bone tumors.
Prognosis
Although the recurrence of Sever disease is relatively common, symptoms are typically anticipated to resolve after the closure of the apophysis. Symptoms should not be expected to persist after the patient reaches skeletal maturity.
Complications
Individuals with Sever disease may concurrently experience Achilles tendonitis and plantar fasciitis. The sole documented complication associated with Sever disease is osteomyelitis, as evidenced by a limited number of case reports in the literature. In cases where osteomyelitis is suspected, an MRI should be promptly ordered for a thorough assessment. The recommended course of treatment involves a 6-week antibiotic regimen, leading to the resolution of the infection and subsequent improvement in symptoms.[15][16]
Postoperative and Rehabilitation Care
Rehabilitation care involves the application of ice and adherence to stretching and strengthening protocols, which can be performed independently at home or with the guidance of a physical therapist. Physical therapists may also incorporate specialized therapies such as ultrasound and electrical stimulation. Specific exercises outlined in the protocols include stretching the gastrocnemius muscle and engaging in eccentric strengthening through heel raises.[10]
Consultations
In the comprehensive management of Sever disease, consultations play a pivotal role, involving collaborative efforts across various healthcare professionals and support personnel. Essential consultations may include podiatry, orthopedic surgery, primary care clinician, physical therapist, sports medicine clinician, caregivers, coaching staff, and athletic trainers.
Deterrence and Patient Education
Sever disease, also known as calcaneal apophysitis, is characterized by inflammation of the growth plate in the heel. This specific growth plate is the attachment point for the calf muscles in the back of the leg and the Achilles tendon to the foot. A growth plate is an actively developing part of the bone in children. The growth plate undergoes closure upon reaching full physical maturity, leading to the formation of solid bone. Before the closure of the growth plate, the surrounding tendons and ligaments exhibit greater strength than the growth plate itself.
During a growth spurt, the bone undergoes faster growth than the muscle and tendon, leading to increased tension exerted by the Achilles tendon on the growth plate. Factors such as a sudden surge in physical activity, participation in a new sport, obesity, or biomechanical issues such as flat feet can increase irritation in this area, ultimately resulting in Sever disease. Common symptoms include pain at the back of the heel after activity, especially upon squeezing both sides, limping, walking on toes, and difficulty running and jumping.
The diagnosis of Sever disease is primarily clinical, indicating that healthcare professionals do not necessarily require x-rays or specialized tests to confirm the disease. Additional diagnostic measures such as x-rays, MRIs, or laboratory tests may be ordered if symptoms are severe, unusual, or persist without improvement for 4 to 8 weeks to rule out more severe conditions.
Sever disease is a self-limiting condition, and the primary focus of therapy is on pain relief. Treatment is initiated with ice application, rest, and anti-inflammatory medications. Furthermore, heel cups or heel pads can provide pain relief. Custom orthotics effectively address biomechanical issues, while braces and cast immobilization may be considered for more severe cases. After the pain has subsided, exercises become essential for stretching the calf muscles and strengthening the leg muscles. Although Sever disease often experiences a recurrence, particularly with increased activity, it resolves entirely once the growth plate closes completely. Continued stretching and strengthening exercises and wearing shoes with adequate heel cushioning can be beneficial in preventing recurring pain.
Pearls and Other Issues
Various considerations and practical insights play a vital role in addressing the holistic care of patients with Sever disease.
- Patients should be reminded to maintain adequate hydration, a balanced diet, and sufficient sleep and to avoid increasing their activity levels by more than 10% per week. Preventing obesity remains of utmost importance.
- To guarantee safety and success, utilizing suitable equipment and techniques while carrying out tasks is crucial. Promoting stretching to sustain flexibility is advised, and consideration should be given to discouraging early specialization in a single sport.
- Sports that involve the use of cleated athletic shoes should be avoided.
- The decision to limit or abstain from physical activity should be made collaboratively by the healthcare professional, patient, and caregiver. This decision should involve a discussion of both short-term and long-term goals, with the primary consideration being the level of pain experienced. Importantly, all parties involved communicate effectively to ensure the best possible outcome for patients.
- Patients are frequently highly active across multiple domains, such as participation in various sports or on multiple teams within the same sport, especially during the same season. Therefore, it may be more effective to contemplate discontinuing one team or sport rather than a complete cessation of activity, as achieving patient buy-in from the individual can be challenging.[2]
Enhancing Healthcare Team Outcomes
Sever disease is prevalent among children and adolescents, yet it may not always attract attention due to its self-limited nature. Patients may present in various clinical settings, including the emergency department, urgent care clinics, athletic trainers, physical therapy, coaching staff, and primary care clinicians. Each individual must be familiar with this condition, which is occasionally misidentified as plantar fasciitis. Sever disease is typically managed conservatively, and most individuals experience symptom relief upon discontinuing overactivity.[13][17] A clear understanding of the etiology and pathophysiology of Sever disease, coupled with effective communication among healthcare professionals, caregivers, patients, coaching staff, and athletic trainers, will improve overall patient outcomes.
Patients, parents, caregivers, and coaching staff should rely on patient-reported symptoms to guide treatment and a possible return to play. Additionally, patients and caregivers need to be aware of the relatively high incidence of recurrence until skeletal maturation and closure of the apophysis occur. The growth plate typically begins to close between the ages of 8 and 14.[2]