Continuing Education Activity
Pityriasis alba is a prevalent and benign dermatological condition that predominantly affects children and adolescents. This skin disorder is often considered a minor manifestation of atopic dermatitis and is typically associated with a history of atopy. The name "pityriasis alba" derives from its appearance, where "pityriasis" denotes the fine scales and "alba" signifies the pale color (hyperpigmentation). Pityriasis alba is characterized by ill-defined macules and patches (or thin plaques), typically circular or oval, often with mild scaling and occasional pruritus.
The lesions are usually found on the face, especially the cheeks, arms, and upper trunk, and are more prominent in individuals with darker skin types. Initially, the lesions may exhibit mild erythema and gradually transition to a hypopigmented state over time. Sun exposure can accentuate the appearance of these lesions, which may often raise concerns regarding their cosmetic impact on patients or parents of children. However, pityriasis alba follows a spontaneous, self-resolving course, gradually restoring normal skin pigmentation. The resolution period for pityriasis alba varies from several months to a few years, although most cases typically resolve within 1 year. Treatment for this condition involves reassurance, low-potency topical corticosteroids, and mild emollients as the mainstay. This activity reviews the evaluation and management of pityriasis alba, highlighting the collaborative role of the interprofessional healthcare team in treating patients with this condition.
Objectives:
Identify and accurately diagnose pityriasis alba based on clinical presentation, considering characteristic ill-defined hypopigmented lesions with fine scales in children and adolescents.
Implement evidence-based management strategies tailored to the patient's needs, including reassurance, low-potency topical corticosteroids, and mild emollients.
Select appropriate therapeutic interventions, considering patient age, severity of symptoms, and potential impact on quality of life, while emphasizing the benign nature of the condition.
Coordinate with allied healthcare professionals to facilitate ongoing patient education and support, promoting a holistic approach to managing pityriasis alba.
Introduction
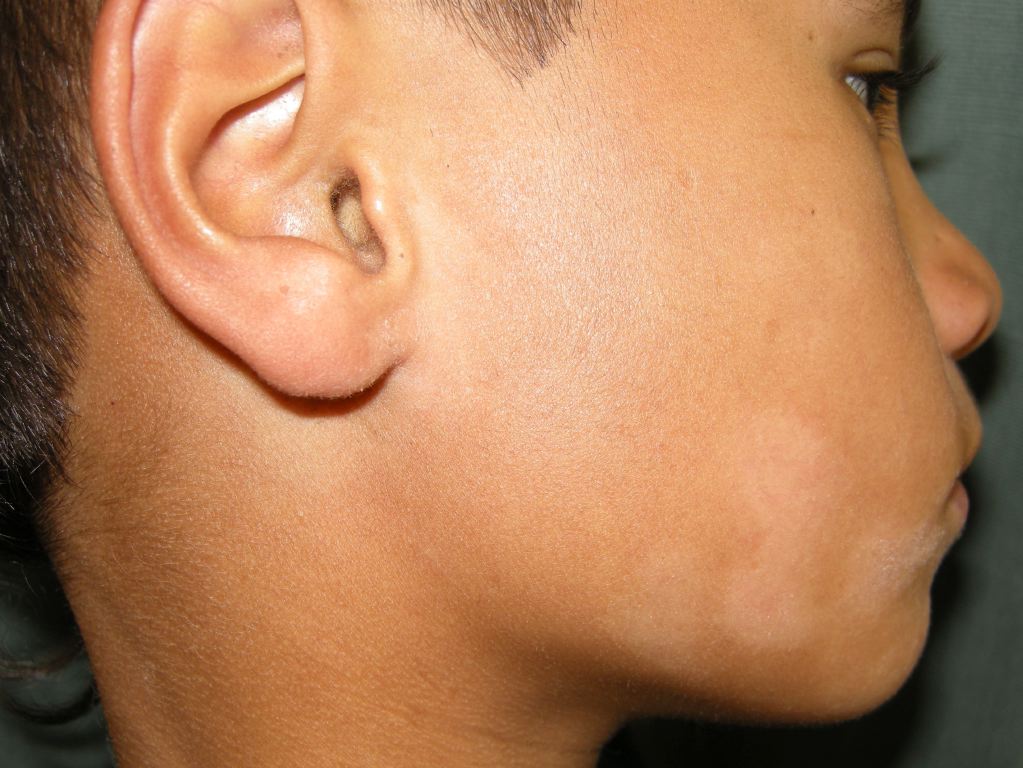
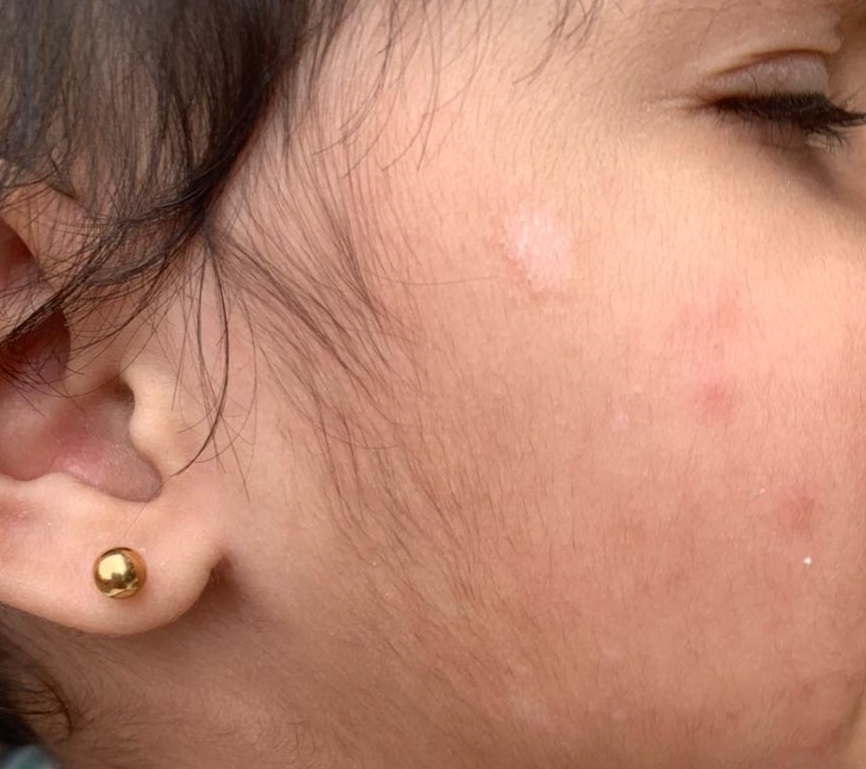
Pityriasis alba is a prevalent and benign dermatological condition predominantly affecting children and adolescents (see Image. Pityriasis Alba). The name "pityriasis alba" derives from its appearance, where "pityriasis" denotes the fine scales and "alba" signifies the pale color (hyperpigmentation). This skin disorder is often considered a minor manifestation of atopic dermatitis and is typically associated with a history of atopy in most individuals. Pityriasis alba is characterized by ill-defined macules and patches (or thin plaques), generally circular or oval, often with mild scaling and occasional pruritus (see Image. Macules or Patches Observed in Pityriasis Alba).
The lesions are usually found on the face, especially the cheeks, arms, and upper trunk, and are more prominent in individuals with darker skin types. Initially, the lesions may exhibit mild erythema and gradually transition to a hypopigmented state over time. Sun exposure can accentuate the appearance of these lesions, which may often raise concerns regarding their cosmetic impact on patients or parents of children. However, pityriasis alba follows a spontaneous, self-resolving course, gradually restoring normal skin pigmentation. The resolution period for pityriasis alba varies from several months to a few years, although most cases typically resolve within 1 year. Treatment for this condition involves reassurance, low-potency topical corticosteroids, and mild emollients as the mainstay.[1][2]
Etiology
The exact cause of pityriasis alba is unidentified. The disorder is not contagious, and no infectious etiology has been reported. Although a history of atopy may preclude this condition, it may also occur in nonatopic individuals. In many cases, it is considered a minor manifestation of atopic dermatitis. The most similar comparison is nonspecific dermatitis with residual postinflammatory hyperpigmentation.
Histopathology shows decreased melanin production in the affected areas. Associated findings in some studies include atrophic sebaceous glands, iron-deficiency anemia, and low levels of serum copper. Other theories of origin include hypopigmentation related to pityriacitrin, which filters sun rays by Malassezia yeasts. The significance of these findings and their relationship to pityriasis alba is uncertain.[3]
Epidemiology
Pityriasis alba is predominantly found in children aged 3 to 16, with 90% of cases occurring in those younger than 12. An estimated 5% of children in the United States may be affected. Studies have demonstrated a higher prevalence in Egypt (18%) and Mali (20%). Pityriasis alba is more common in individuals with a history of atopy, and a slight male predominance is noted. A clear racial predominance is not evident, although the lesions are more noticeable in individuals with darker skin types.
Pityriasis alba is a skin condition that is not influenced by seasons. However, in the winter, the dry air in homes may worsen scaling, and sun exposure during spring and summer may make lesions appear more visible and cause the surrounding skin to darken. Normal skin pigmentation typically returns spontaneously, usually within 1 year.[2]
Pathophysiology
Ultrastructural studies in individuals with pityriasis alba have shown no difference in melanocytes between the affected lesional and unaffected non-lesional skin of the same patient. Nonetheless, degenerative changes and fewer melanosomes within keratinocytes have also been noted.[4] In the extensive variant of pityriasis alba, hypopigmentation may be associated with a reduction in the number of active melanocytes, leading to a subsequent decrease in the size and number of melanosomes in the affected skin.[5]
Histopathology
The microscopic features of pityriasis alba include mild, chronic, nonspecific dermatitis with decreased melanin production. Various nonspecific histopathological features are noted, which include hyperkeratosis, parakeratosis, acanthosis, spongiosis, and perivascular infiltrates. Although no specific diagnostic criteria have been identified for this skin condition, a biopsy of a skin lesion can provide helpful information in diagnosis. Certain features in a biopsy specimen that may suggest the diagnosis include irregular or reduced melanin in the basal layer, an insignificant decrease in melanocyte count, and a reduced number of active melanocytes with a decreased number and size of melanosomes.[6][4]
History and Physical
Although the initial lesions of pityriasis alba may exhibit mild erythema, this erythematous stage may go unnoticed. The most common presentation is asymptomatic (or mildly pruritic) hypopigmented lesions, frequently found on the face. The patient or family history may include atopic dermatitis, allergic rhinitis, or asthma. The lesions may be incidentally discovered during a physical examination. However, patient or parental concern about the cosmetic appearance of the lesions often prompts consultation with a clinician. Hypopigmentation becomes more apparent with sun exposure, leading to darkening of the surrounding skin during the spring and summer.
On physical examination, multiple round or oval-shaped hypopigmented macules or patches (or thin papules and plaques) with indistinct margins are observed. Mild erythema and/or scaling may be present. The lesions typically range in number from 4 to 20, measuring between 0.5 and 5 cm in size. They are predominantly distributed on the face, neck, upper arms, and upper trunk.[1][7]
Careful examination of the patient is crucial as the scaly lesions may resemble psoriasis or eczema, as skin irritation by various causes may heal with postinflammatory hypopigmentation. Inquiring patients about their prior therapy with potent topical steroids is important, as it may contribute to hypopigmentation. Furthermore, exploring other topical creams or lotions is advisable, as they may develop irritant or allergic contact dermatitis with subsequent development of postinflammatory hypopigmentation, often confusing with the hypopigmented lesions of pityriasis alba.
Inspection for keratotic lesions on the elbows and knees and small pits in the nails is necessary, as these may indicate a diagnosis of psoriasis. Potential signs of atopic dermatitis should be explored in the patients, including Dennie-Morgan infraorbital folds, anterior neck folds, white dermographism, cheilitis, nipple eczema, infra-auricular fissuring, and eczema in the flexures.
Uncommon Variants of Pityriasis Alba
Pigmenting pityriasis: This condition is characterized by lesions with a central zone of bluish hyperpigmentation surrounded by a hypopigmented scaly halo. These lesions are often confined to the face and are associated with dermatophyte infection.[8] This variant is commonly observed in individuals with darker skin types from the Middle East and South Africa.[7]
Extensive pityriasis alba: This condition is characterized by symmetrical and widespread skin involvement. Compared to the classic variant, the lesions of this entity are less erythematous, less scaly, more persistent, asymptomatic, and more frequently seen on the trunk than the face. Furthermore, histopathology reveals the absence of spongiosis.
Evaluation
Based on the clinical appearance and distribution of skin lesions in a child or adolescent, the diagnosis of pityriasis alba is typically straightforward. Several diagnostic procedures can be helpful in cases of uncertainty, some of which are mentioned below.
- When exposed to a Wood's lamp, the lesions of pityriasis alba may be accentuated but remain nonfluorescent. This finding differs from vitiligo, which fluoresces brighter and exhibits edges with sharper demarcation.
- A potassium hydroxide preparation of skin scraping yields negative results for fungal elements. This result distinguishes it from conditions such as tinea versicolor or tinea corporis, where fungal elements are typically positive.
- A skin biopsy is generally unnecessary, but when performed, the procedure can differentiate between pityriasis alba and mycosis fungoides.[2][9]
- Dermoscopy of pityriasis alba reveals dull white areas with ill-defined margins, corresponding to melanosome loss in the basal layer of the epidermis histologically. In addition, white scaling, attributed to hyperkeratosis, typically exhibits a polygonal appearance or follows a distribution in the skin furrows. A subtle light-brownish pigment network is observed in the background, specifically in dark skin phototypes. Furthermore, perieccrine semicircles are considered a distinctive finding of pityriasis alba in the skin of color, representing pigmentation arranged in a semicircular pattern around the perieccrine openings. This particular feature is associated with partial resistance to the exfoliation of melanin around the eccrine sweat glands. In addition, dark phototypes may exhibit satellite white areas and brown dots.[10]
Treatment / Management
Patients and their parents can be reassured about the benign and self-limited nature of pityriasis alba. However, they should also be aware that the gradual resolution of the condition may extend over several months to a few years, although most cases resolve within 1 year.
Various treatment options are available for managing pityriasis alba, and each option aims to address specific aspects of the condition, offering diverse approaches to achieve relief and repigmentation.
- The affected areas should be protected from sun exposure to prevent the worsening of the cosmetic appearance due to the darkening of the surrounding skin. The use of sunscreen may aid in preventing sunburn on the lesions and reducing the darkening of the surrounding skin.
- Low-potency topical steroids, such as 1% hydrocortisone cream or ointment, may help alleviate erythema and pruritus while promoting the acceleration of repigmentation.
- Mild emollients, such as petroleum jelly and creams, may effectively reduce scaling.
- Topical calcineurin inhibitors, such as 0.1% tacrolimus ointment and 1% pimecrolimus cream, can effectively treat pityriasis alba. However, their utilization is infrequent due to the associated high cost.
- Calcitriol, a topical vitamin D analog, demonstrated efficacy comparable to tacrolimus.
- Additional treatment options, typically reserved for extensive cases, include psoralen plus ultraviolet-A (PUVA) photochemotherapy and targeted phototherapy using a 308-nm excimer laser.[1]
Differential Diagnosis
As various skin conditions share similarities with pityriasis alba, making a precise diagnosis is crucial. The distinctive features of potential differentials are listed below.
Nevus depigmentosus: This condition is characterized by a segmental distribution, typically occurring on the trunk, with no change in size or number over time.
Psoriasis: The early erythematous lesions may resemble pityriasis alba, but the sparing of elbows, knees, and scalp, along with the absence of salmon-colored scales, helps exclude this diagnosis.
Tinea versicolor: Potassium hydroxide examination can reveal hyphal and yeast forms of Malassezia furfur.
Vitiligo: This condition is characterized by complete loss of pigmentation. Lesions tend to favor periocular and perioral sites.
Mycosis fungoides: This condition is considered in persistent and symptomatic lesions exhibiting progressive changes in shape or color.
Pityriasis lichenoides chronica: This condition presents a widespread distribution involving the trunk and extremities. After the resolution of this condition, it often results in postinflammatory hypopigmentation, resembling the hypopigmented lesions similar to pityriasis alba.
Delusional tinea: Delusional changes may result in chronic postinflammatory hyperpigmentation, resembling pityriasis alba.
Leprosy: This condition should be considered in areas where there is exposure to armadillos.
Nummular eczema: This condition is characterized by intense pruritus, unlike pityriasis alba.
Other conditions include postinflammatory hypopigmentation from any cause, ash-leaf macules of tuberous sclerosis, hypopigmentation secondary to topical medications such as retinoic acid, benzoyl peroxide, and corticosteroids, pityriasis rosea, seborrhea, atopic dermatitis, contact dermatitis, nevus anemicus, discoid eczema, and tinea corporis.
Prognosis
Pityriasis alba is a self-limiting skin condition with a favorable prognosis, and complete repigmentation is the norm in most individuals. The primary concern is the cosmetic deficit for which patients often seek medical help. In addition, the risk of sunburn necessitates protection for areas of hypopigmentation. Although the duration of the skin disorder can vary from a few days to a few years, in some cases, treatment may help shorten its duration.
Pearls and Other Issues
Pityriasis alba is a prevalent skin disorder that is best managed by an interprofessional healthcare team due to the extensive range of potential differential diagnoses. Patients are advised to avoid sun exposure and wear protective clothing, such as a wide-brimmed hat and long-sleeved garments, as UV light can exacerbate scaling. Although outcomes are generally excellent, recovery may take months or even years.
Enhancing Healthcare Team Outcomes
Pityriasis alba, a common skin disorder, is typically managed by primary care clinicians, nurse practitioners, dermatologists, and specially trained nurses. The key focus is to educate the patient about the benign nature of the disorder. Usually, treatment is unnecessary, as the condition tends to regress spontaneously within 12 to 24 months. A referral to a dermatologist is advisable for individuals seeking treatment for cosmesis. Although various treatment options are available, there is no conclusive evidence suggesting the superiority of one over another. Moreover, some treatments are more likely to cause harm than provide benefits.[1] The use of a moisturizer may be beneficial for some patients.
In an interprofessional healthcare team, dermatology nurses play a crucial role in patient education, coordinating follow-up, and facilitating communication within the team. Pharmacists can also contribute by aiding in the selection of emollient creams and sunscreens, as well as participating in patient education.