Continuing Education Activity
Clubbing of the nails is soft tissue swelling of the terminal phalanx, resulting in flattening the angle between the nail bed and the nail. Clubbing typically occurs with other dermatologic and skeletal findings but can also less commonly occur in isolation. Although clubbing can present in many pathologic conditions, it can be idiopathic or familial. This activity reviews how to properly evaluate nail clubbing when patients with nail clubbing should receive additional evaluations, and the role of the interprofessional team in caring for patients with nail clubbing.
Objectives:
Identify the causes of nail clubbing.
Determine when a patient with nail clubbing should undergo additional evaluations.
Determine additional evaluations should be reviewed in select patients with nail clubbing.
Communicate the role of collaboration among interprofessional team members to improve care coordination and treatment outcomes for patients with diseases that may manifest with nail clubbing.
Introduction
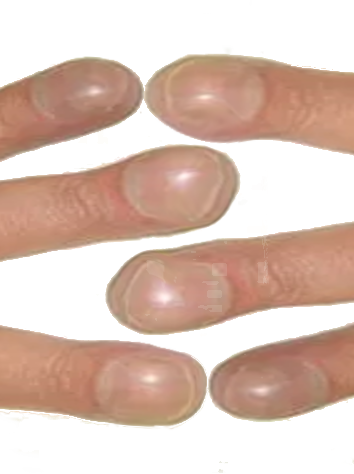
Clubbing of the nails is soft tissue swelling of the terminal phalanx, resulting in the straightening of the angle between the nail bed and the nail.[1] The association of clubbing of the fingers with an underlying disease has been known since Hippocrates. Clubbing is combined with other dermatologic and skeletal findings but can also less commonly occur in isolation. Although clubbing can present in many diverse conditions, it can be idiopathic or familial; the familial form frequently transmits as a dominant trait (see Image. Clubbing of Digits).
Etiology
Acquired nail clubbing has several causes, including infectious, neoplastic, inflammatory, and vascular diseases.[2] Isolated nail clubbing can be a benign hereditary condition, but given the multiple associated conditions, the underlying etiology should be ruled out.
Epidemiology
The incidence of nail clubbing can be difficult to estimate, given the numerous underlying etiologies. Further, not all patients with an underlying disease have the clinical manifestation of nail clubbing. In general, clubbing is seen in roughly 1% of all internal medicine admissions and is associated with serious underlying disease in 40% of those patients.[3]
Of the etiologies in adults, the most common pulmonary cause of clubbing is lung malignancy.[4] Of the several different types of thoracic malignancy, 80% of these cases of clubbing are caused by lung cancer. In comparison, pleural tumors contribute to roughly 10%, and other intrathoracic and mediastinal growth account for 5% of cases.[4] Despite being such a predominant cause of clubbing, clubbing is prevalent in only 5% to 15% of lung cancer patients.[4] The prevalence of clubbing in other conditions like interstitial lung disease, cardiovascular disease, gastrointestinal disease, infectious disease, and other cancers has been reported but shows significant variation.
Patients with clubbing may also have hypertrophic osteoarthropathy. This condition characteristically presents with the subperiosteal formation of new cancellous bone at the distal ends of long bones, particularly the radius, ulna, tibia, and fibula. Hypertrophic osteoarthropathy is almost always associated with clubbing, particularly in patients with bronchogenic carcinoma, other intrathoracic malignancies, and cystic fibrosis.
Pathophysiology
Multiple hypotheses have been proposed over the years to describe the pathophysiology of clubbing. The initial hypothesis suggests that clubbing results from peripheral deposition of clumped platelets and megakaryocytes, which are otherwise sequestered by pulmonary vasculature.[5] The main pathologic finding in clubbing is increased capillary density. The increased release of platelet-derived growth factor (PDGF) and vascular endothelial growth factor (VEGF) from peripheral megakaryocytes leads to increased vascularity, permeability, and connective tissue changes. The release of both PDGF and VEGF is thought to be enhanced by hypoxia.[6][7]
Numerous other signaling proteins are thought to be associated with nail.. clubbing, including prostaglandins, bradykinin, ferritin, adenosine nucleotides, interleukin-6, von Willebrand factor, serum transforming growth factor-beta1 (TGF-beta1), tumor necrosis factor-a, growth hormone, epidermal growth factor.[1] Shunting of blood past the capillary bed of either the lung or the liver suggests a lack of metabolism of angiogenic factors that bypass a critical organ may also be involved.
History and Physical
A proper history and physical exam are key to evaluating nail clubbing, especially given the numerous etiologies of this physical exam finding. While conducting the patient interview, it is crucial to identify the patient's symptoms, which will guide and narrow your differential diagnosis. It is important to remember that not all patients with clubbing have an underlying pathological disease, and not all with a disease will have the manifestation of nail clubbing. Equally, it is important to note that clubbing has much variation. The assessment of clubbing by physical exam is subjective and unreliable, especially if the clubbing is minimal and not severe.
Lovibond Angle
The most widely known physical exam sign of clubbing is the profile sign, also known as the Lovibond angle. The Lovibond angle is the angle found between the proximal nail fold and the nail at the location at the exit of the nail from the nail fold. Normally, this angle is less than 180 degrees; therefore, true digit clubbing can be differentiated from simple nail curving when the angle is greater than 180 degrees.
Hyponychial Angle
The hyponychial angle is also used as an objective criterion to assess clubbing. It is where a line is drawn from the cuticle to the distal digital crease, and a second line is drawn from the hyponychium to the cuticle.[4] An angle of fewer than 192 degrees is normal.
Phalangeal Depth Ratio
The phalangeal depth ratio, the ratio of the digit’s depth measured at the nail and the distal interphalangeal joint, is another objective criterion used to assess clubbing. The depth at the distal interphalangeal joint is normally greater than the nail's. Therefore, a ratio of greater than 1 supports clubbing.
Schamroth sign
In 1976, Schamroth reported a clinical sign associated with clubbing: obliteration in clubbed fingers of the diamond-shaped window normally produced when the dorsal surfaces of the corresponding finger of each hand are opposed. This sign is now called the Schamroth sign.
The nail cuticle angle straightening appears to be the most sensitive measurement of these features.[2] A noteworthy feature of clubbing is the speed with which it can develop, about 2 weeks in patients with new-onset empyema, and how quickly it can reverse, also about 2 weeks in patients after corrective cardiac surgery.
Evaluation
Nail clubbing is primarily evaluated during the initial patient evaluation. A thoroughly taken history, including attention to characteristic features of the many possible etiologies of clubbing, should be taken into account. The history is followed by the physical exam, where nail clubbing is assessed based on the above-mentioned features and measurements. Acquired clubbing is most often associated with pulmonary or cardiovascular diseases, so obtaining chest radiography is very reasonable during the initial workup. If plain films demonstrate no abnormality, a CT scan is the next step to look for a pulmonary neoplasm or other lesions that may still be localized and curable.
Treatment / Management
Treatment and management of nail clubbing are not focused on the clubbing finding itself but rather on the underlying etiology behind clubbing if it exists. Response to treatment will have a significant degree of variation depending on the underlying disease process. Data for the reversibility of clubbing is sparse. Clubbing reversibility has been reported, in particular in patients undergoing prostaglandin therapy for liver disease who developed clubbing, which reversed with the cessation of therapy.[1]
Differential Diagnosis
The differential diagnoses for nail clubbing include the following:
- Neoplastic intrathoracic diseases: Bronchogenic carcinoma, malignant and benign pleural tumors, metastatic cancers, Hodgkin lymphoma, thymoma, pulmonary artery sarcoma, nasopharyngeal carcinoma, rhabdomyosarcoma, primary lymphosarcoma of the lung, and esophageal cancer.
- Suppurative intrathoracic diseases: Lung abscess, bronchiectasis, cystic fibrosis, empyema, and chronic lung cavitary mycobacterial or fungal infection
- Diffuse pulmonary diseases: Idiopathic pulmonary fibrosis, asbestosis, Langerhans cell histiocytosis, lipoid pneumonia, and pulmonary arteriovenous malformations.
- Cardiovascular diseases: Cyanotic congenital heart disease, infective endocarditis, arterial graft sepsis, brachial arteriovenous fistula, aortic aneurysm, atrial myxoma, and hemiplegic stroke
- Gastrointestinal diseases: Inflammatory bowel disease, celiac disease, amoebiasis, ascariasis, and lymphoma of the gastrointestinal tract
- Hepatobiliary disease: Biliary cirrhosis and juvenile cirrhosis
- Metabolic diseases: Thyroid acropathy and severe secondary hyperparathyroidism
- Medication-induced cases: Laxative overuse, interferon alfa-2A, and prostaglandin infusion [4][8]
Prognosis
As with treating and managing nail clubbing, the prognosis highly depends on the underlying etiology. If the etiology is reversible, then clubbing will reverse. But if the condition is chronic or associated with a malignancy, clubbing is long-term.
Complications
Clubbing as an individual entity results in aesthetic changes, which can lead to complications, especially surrounding the psychosocial aspects of everyday life. Although the data is sparse, reports indicate that acquired clubbing is reversible with successful treatment of the underlying condition.[9] Furthermore, it is vital to establish the etiology of clubbing as the underlying condition responsible may result in further complications if left untreated.
Deterrence and Patient Education
Patients, in general, benefit greatly from adequate information provided to them by healthcare workers, especially regarding a condition they may have. As with other medical conditions, information on clubbing should be given to patients, and they should be encouraged to ask questions to further their insight into their situation. When acceptable, patients should receive reassurance, especially if the cause of their clubbing is not due to the underlying pathology.
Enhancing Healthcare Team Outcomes
Nail clubbing is a physical exam finding that often correlates with a serious underlying disease. Proper recognition of clubbing, therefore, plays a vital outcome in the progression of the disease. The initial physical exam in the case of clubbing may be at either an inpatient or outpatient setting, depending on the underlying cause. Clubbing is identified by anyone conducting the physical exam, including medical students, nurses, nurse practitioners, physician assistants, and physicians. Regardless of who recognizes clubbing first, an interprofessional team approach is the ideal way to evaluate and manage a patient with clubbing.
Depending on the underlying cause of the clubbing, evaluation by specialists may be required, including pulmonologists, oncologists, infectious disease specialists, cardiologists, gastroenterologists, endocrinologists, or radiologists. Cases where clubbing results in increased stress due to impaired physical appearance may warrant intervention from a behavioral therapist. Only through such a team approach can the diagnosis be confirmed.