Continuing Education Activity
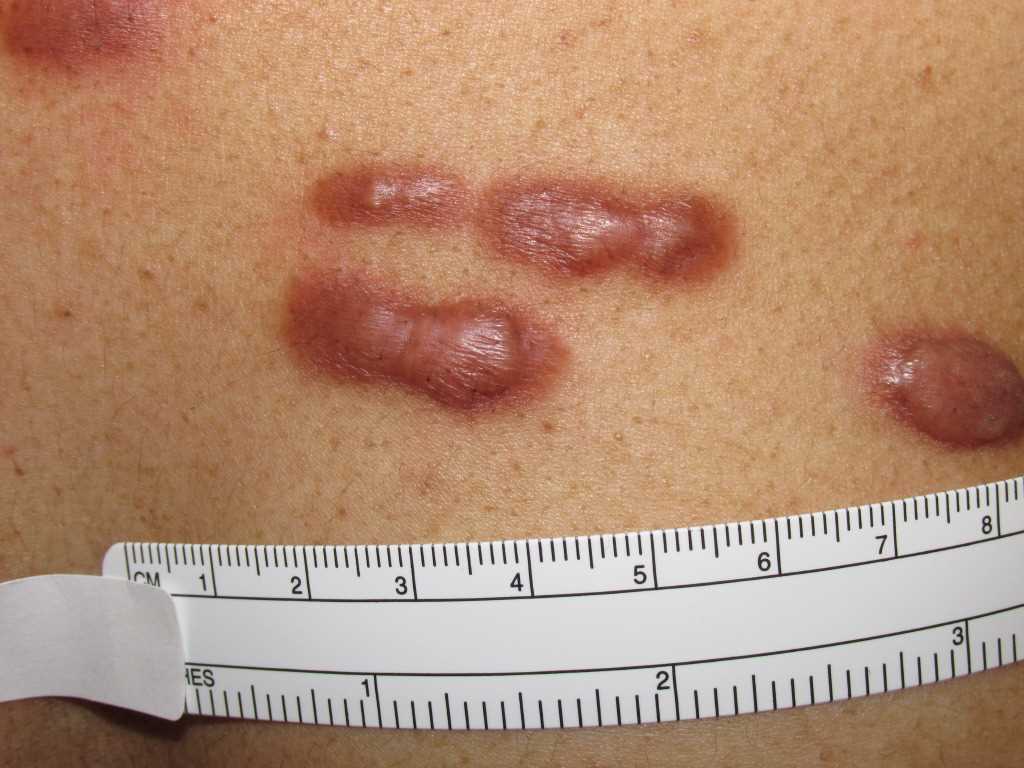
Keloids result from abnormal wound healing in response to skin trauma or inflammation. Keloid development rests on genetic and environmental factors. Higher incidences are seen in darker skinned individuals of African, Asian, and Hispanic descent. Overactive fibroblasts producing high amounts of collagen and growth factors are implicated in the pathogenesis of keloids. As a result, classic histologic findings demonstrate large, abnormal, hyalinized bundles of collagen referred to as keloidal collagen and numerous fibroblasts. Keloids present clinically as firm, rubbery nodules in an area of prior injury to the skin. In contrast to normal or hypertrophic scars, keloidal tissue extends beyond the initial site of trauma. Patients may complain of pain, itching, or burning. Multiple treatment modalities exist although none are uniformly successful. The most common treatments include intralesional or topical steroids, cryotherapy, surgical excision, radiotherapy, and laser therapy. This activity reviews the evaluation and treatment of keloids and the role of the interprofessional team in managing and educating patients with this condition.
Objectives:
- Explain the causes of keloid formation.
- Describe the most common populations that develop keloid formation.
- Review the signs and symptoms of keloids.
- Outline the evaluation and treatment of keloids and the role of the interprofessional team in managing and educating patients with this condition.
Introduction
Keloids result from abnormal wound healing in response to skin trauma or inflammation. Keloid development rests on genetic and environmental factors. Higher incidences are seen in darker skinned individuals of African, Asian, and Hispanic descent. Overactive fibroblasts producing high amounts of collagen and growth factors are implicated in the pathogenesis of keloids. As a result, classic histologic findings demonstrate large, abnormal, hyalinized bundles of collagen referred to as keloidal collagen and numerous fibroblasts. Keloids present clinically as firm, rubbery nodules in an area of prior injury to the skin. In contrast to normal or hypertrophic scars, keloidal tissue extends beyond the initial site of trauma. Patients may complain of pain, itching, or burning. Multiple treatment modalities exist although none are uniformly successful. The most common treatments include intralesional or topical steroids, cryotherapy, surgical excision, radiotherapy, and laser therapy.[1][2][3]
Etiology
Both genetic and environmental factors play a role in keloid development. Predisposed individuals may develop a keloid following any level of skin trauma including surgery, piercings, acne, tattooing, insect bites, burns, lacerations, abrasions, vaccinations, and any other process resulting in cutaneous inflammation. Increased tension in a wound also may contribute to keloid formation.[1][4][5]
Epidemiology
Dark-skinned individuals of African, Asian, and Hispanic descent have higher rates of keloid development compared to Caucasians. The incidence in these darker-pigmented populations ranges from 4.5% to 16%. The incidence is notably higher during pregnancy and puberty. A positive family history increases the risk for the development of keloids although no specific gene has been identified. Rare genetic syndromes can also confer increased risk for the development of keloids including Rubinstein-Taybi and Goeminne syndrome.[1]
Pathophysiology
Keloids are a result of aberrant wound healing. Standard wound healing consists of three phases: (1) inflammatory, (2) fibroblastic, and (3) maturation. In keloids, the fibroblastic phase continues, unchecked, resulting in the clinical and histopathological findings.
Keloidal fibroblasts have increased proliferative activity, persist for longer, and have lower rates of apoptosis compared to typical wound healing. This results in an overproduction of collagen and cytokines. Collagen synthesis in keloids is 20 times greater than that of healthy skin and three times greater than a hypertrophic scar.
Transforming growth factor-beta and platelet-derived growth factor are thought to be the primary drivers of this process. Transforming growth factor-beta, an integral part of wound healing, promotes chemotaxis of fibroblasts to the site of inflammation and produces collagen. Dysregulation of this pathway leads to fibrosis and abnormal scar response.[6][7][8]
Histopathology
The histologic hallmark of a keloid is increased whorls of thickened, hyalinized collagen bundles widely known as keloidal collagen. This feature is found in up to 55% of specimens. However, experts have determined the following four other diagnostic criteria when keloidal collagen is absent:
- Standard epidermis and papillary dermis
- “Tongue-like” advancing edge below the papillary dermis
- Horizontal fibrous band in the upper reticular dermis
- Prominent fascia like a band in the deep dermis
Important clinical and histopathologic differential includes hypertrophic scar. An increased number of fibroblasts and thickened collagen bundles arranged parallel to the skin surface characterizes these lesions. Another common finding includes vertically oriented blood vessels, which are rare in keloids. Hypertrophic scars do not exhibit keloidal collagen. Contrary to previous belief, smooth muscle actin expression is not a reliable way to differentiate hypertrophic scar from keloid.
History and Physical
Keloids are benign, dermal growths related to previous skin trauma or inflammation. Lesions may develop as early as 1 to 3 months or as late as one year after injury. Spontaneous lesions have been reported. However, it is more likely that the injury was not recalled due to its insignificance or that the keloid development was delayed by months or even years. Keloids may develop anywhere, but the most commonly affected locations include deltoid, pre-sternal chest, upper back, and ear. Unusual locations for these growths include eyelids, genitalia, palms, and soles. Keloids present as firm, rubbery nodules and frequently project above the underlying skin. They may have a narrow base, resulting in pedunculated lesions, or develop into a more a broad-based plaque. As stated above, an important differential diagnosis includes hypertrophic scar which will not project above underlying skin further than 4 millimeters and, as a rule, will never extend beyond the initial area of injury. In contrast, keloids always extend beyond the area of original trauma. Color ranges from erythematous, flesh-colored, or hyperpigmented and may change with the evolution of the lesion. Although these lesions are benign, they are frequently symptomatic. In one study, 86% of patients complained of pruritus while 46% experienced pain. Other reported symptoms include tenderness and burning. Finally, keloids may have significant cosmetic implications for affected patients as they can grow to be large and disfiguring.[1][9]
Evaluation
Evaluation is primarily clinical. A biopsy is not required unless the diagnosis is in question. In that case, a biopsy is diagnostic. No further workup is necessary.
Treatment / Management
Keloids remain a therapeutic dilemma. Not only are they difficult to treat but incomplete therapy can lead to a keloid worsening and growing. Therefore, primary prevention is key. Predisposed individuals should avoid elective procedures if possible, especially ear piercing and tattooing. If accidental trauma occurs or surgical interventions are required, there are ways to minimize and perhaps prevent the development of keloid scar. Minimizing wound tension is important to reduce the risk for keloid development. Rapid primary closure and adequate hemostasis are the cited key elements in tension-free wound closure. Prolonged wound stabilization using silicone sheeting also may help reduce tension on wounds. Compression therapy is noted in the literature to reduce keloid development with pressures of 15 to 45 mmHg recommended for more than 23 hours per day for at least 6 months.
Several modalities alleviate symptoms of existing keloids:
- Corticosteroids- Intralesional steroids are considered the first line in the treatment of keloid scars. Multiple injections at intervals of 4 to 6 weeks are required. Recommended doses range from 10 to 40 mg/cc of triamcinolone. This may be used alone or in combination with other modalities. Topical ointments and steroid impregnated tapes also have been shown to reduce symptoms of itching and burning.
- Cryotherapy- Delivery via spray, contact, or intralesional-needle cryoprobe all have been described. Multiple treatments are required. Freeze-thaw cycles of 10 to 20 seconds are recommended to achieve scar tissue necrosis. Post-treatment pigmentary alteration makes this method less desirable in darker skin types.
- Surgical excision- Due to high recurrence rate between 45% and 100%, this method should always be paired with an adjuvant therapy such as post-surgical radiation or intralesional steroid injections.
- Radiotherapy- Best utilized as adjuvant therapy 24 to 28 hours following excision. Caution should be used in patients less than 18 years of age and in vulnerable areas such as the head, neck, and breast as it carries an inherent risk of carcinogenesis.
- Laser- Successive sessions using 585 nanometers (nn) pulse-dye laser and 1065 nm neodymium-doped yttrium aluminum garnet (ndYAG) laser have been shown to induce flattening and regression of keloids.
- Other treatments including topical imiquimod following excision, intralesional botox, intralesional bleomycin, intralesional 5-fluorouracil, and silicone gel sheeting have also been reported to be successful in treating keloid scars either alone or in combination with the above modalities.
It is important to manage patient expectations as all treatments require multiple sessions and do not uniformly result in complete regression of keloid. The most successful treatment results from the use of multiple modalities and tailoring therapy to meet patient needs.
Differential Diagnosis
When evaluating a patient with suspected keloids, the differential diagnosis is narrow. However, it is important to note key features to determine which lesions warrant skin biopsy. As discussed above, hypertrophic scars can appear very similar to keloids and occur after skin trauma. Hypertrophic scars tend to be smaller and, as a rule, are confined to the area of injury as opposed to keloids which can continue to grow and involve the surrounding skin. Dermatofibroma is another aberrant scar response that typically results in flesh-colored or hyperpigmented papule or nodule. The classic clinical feature of these lesions is central depression when applying lateral pressure, which is known as the “dimple sign.” Dermatofibrosarcoma protuberans is a rare, locally aggressive spindle cell tumor that arises on the trunk and proximal extremities of young adults. In contrast to keloids, these lesions have no preceding trauma and have more irregular borders. Keloidal variants include morphea and scleroderma. These patients would have progressive disease in the absence of a known inciting event and may also show other signs of connective tissue disease. Xanthoma disseminatum is rare, histiocytic proliferation with skin lesions that may resemble keloids. Lesions present acutely in a diffuse symmetric pattern, and systemic involvement may result in the development of diabetes insipidus. Finally, lobomycosis is a deep fungal infection caused by the organism Lacazia loboi. It presents as a slow-growing keloid-like nodule on distal extremities and is associated with exposure to dolphins or rural soil in Central and South America.
Prognosis
Keloidal scars are benign, and treatment is primarily directed toward symptom relief or cosmetic concerns.
Pearls and Other Issues
Keloids have a predilection for darker-skinned individuals. Keloids are a result of aberrant wound healing. In contrast to hypertrophic scars, keloidal tissue extends beyond the area of initial skin injury. Treatment is difficult and rests primarily in symptom relief.
Enhancing Healthcare Team Outcomes
All physicians including nurse practitioners should be aware of keloids. Any healthcare provider doing surgery, administering injections or looking after trauma patients, must educate the patient on keloids. These skin lesions are extremely difficult to treat. Despite the wide number of treatment, none works consistently or reliably. Giving patients false hopes is another major problem when it comes to keloid treatment. Many of the treatments can in fact make the keloid scar look worse. If one has no idea what to do, the best advice is to leave the keloid alone.[10][11]