Continuing Education Activity
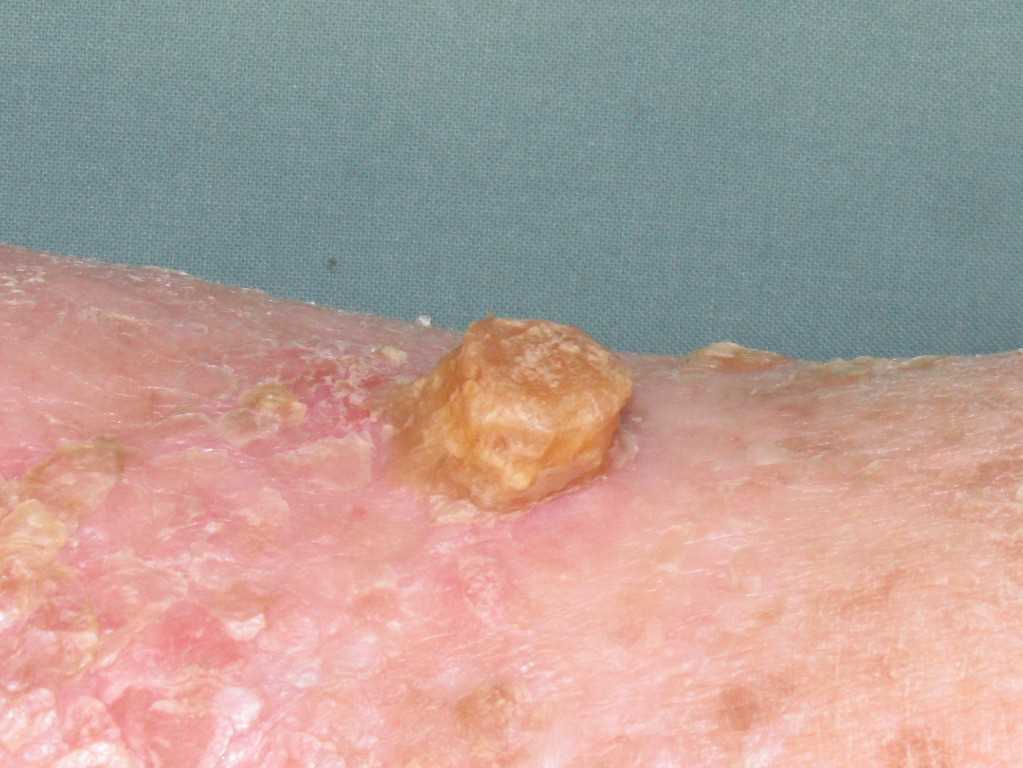
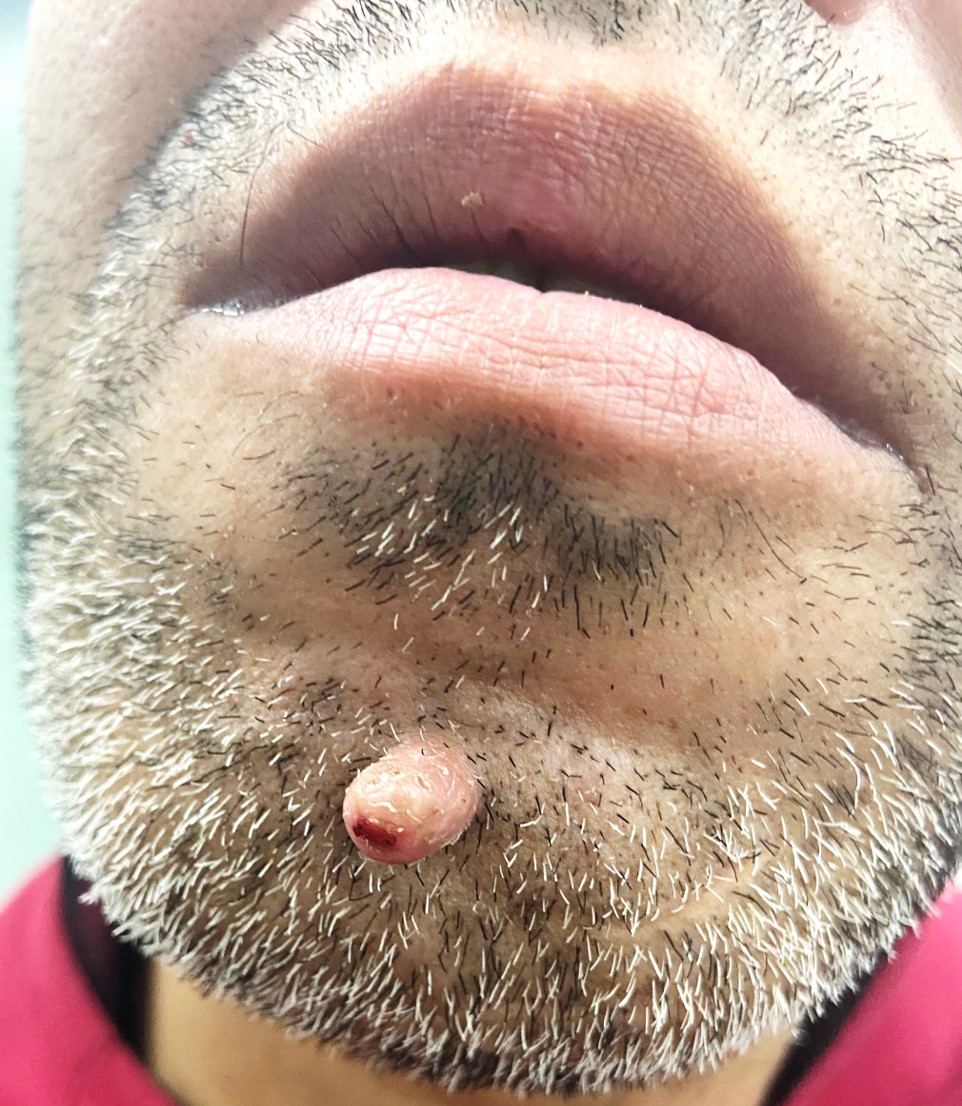
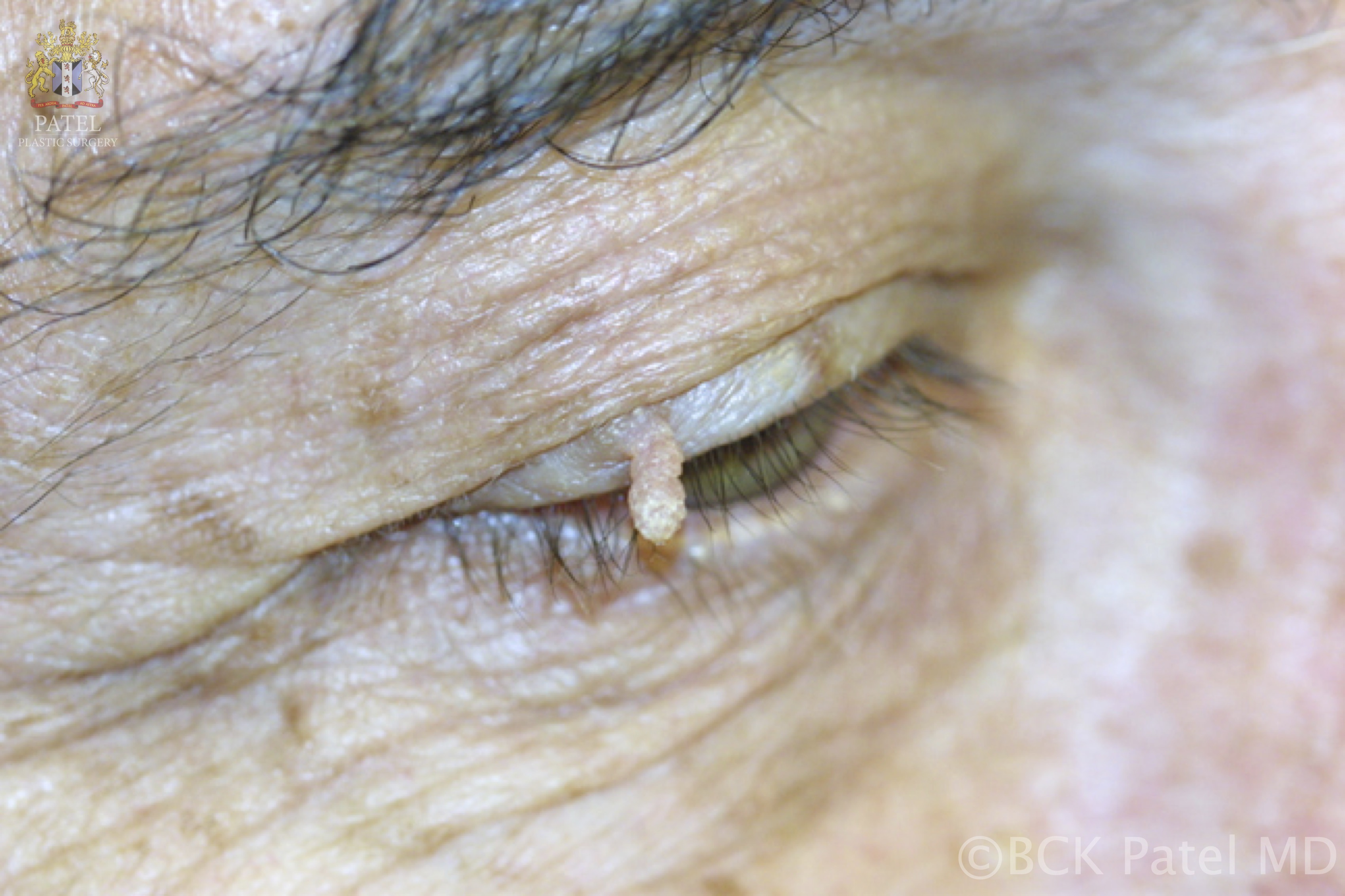
A cutaneous horn, or cornu cutaneum, presents as an uncommon hyperkeratotic epithelial lesion resembling an animal horn, typically exceeding half the diameter of its base. Historically documented since 1588, individuals with these growths were referred to as "horned people" until this misconception was dismantled in the seventeenth century. Composed solely of cornified keratinocytes, these horns manifest as white or yellow protrusions, distinct from animal horns due to their absence of a bony structure.
Despite variable color, size, and shape, histopathological analysis remains pivotal for accurate diagnosis. Epidemiologically linked to age, sex, skin color, location, and lesion dimensions, cutaneous horns signify underlying conditions more significantly than the horns themselves. Consequently, understanding their etiology and associated histopathology stands as a primary focus for clinicians and researchers alike. This activity elucidates the evaluation and management protocols, emphasizing an interprofessional approach to caring for patients with this condition.
Objectives:
Determine the epidemiology of a cutaneous horn.
Identify the appropriate points in the evaluation of a cutaneous horn.
Evaluate the management options available for a cutaneous horn.
Coordinate interprofessional team strategies for improving care coordination and communication to advance the treatment of cutaneous horns and improve outcomes.
Introduction
A cutaneous horn, or cornu cutaneum, is a relatively uncommon, hyperkeratotic epithelial lesion resembling an animal horn, characterized by a height more than half of the diameter of its base.[1][2] The first formally documented case originates from the 1588 description of an elderly Welsh woman, Margeret Gryffith. Her disease and subsequent exploitation in circuses profiting from medical oddities spurred the term "horned people" in popular culture.[3] It wasn't until the mid-17th century that this misconception was debunked by Danish anatomist Thomas Bartholin, who described these horny growths as a tissue tumor arising from the surface of the skin.[4] Cutaneous horns are now widely accepted as reactive cutaneous growths caused by various benign, premalignant, or malignant primary processes.
The cutaneous horn lesion is usually evident upon physical examination and can be described as a white or yellow exophytic protrusion in the shape of an animal horn. Unlike animal horns that generally contain an osseous cast, cutaneous horns consist solely of cornified proliferative keratinocytes without a bony component. The color, size, shape, and dimensions can vary significantly, so histopathological analysis should confirm clinical suspicion.[5]
Although the prevalence and incidence of cutaneous horns have not been established, epidemiological conclusions have formed correlations with age, sex, skin color, location, and dimensions.[6][7] Histopathological evidence asserts the cutaneous horn is relatively unimportant compared to its underlying condition.[3] Consequently, understanding the etiology and associated histopathology behind cutaneous horns has been among the primary concerns of clinicians and researchers.
Etiology
The etiology of cutaneous horns varies as it is a secondary manifestation of a benign, premalignant, or malignant primary disease. The most common cause of benign cutaneous horns is seborrheic or lichenoid keratoses.[7] Other benign causes include infections like human papillomavirus, molluscipoxvirus,[8] rhinosporidiosis,[9] chronic irritation,[8] hemangioma,[8] sarcoidosis,[10] juvenile xanthogranuloma,[11] epidermal nevus,[11] pilomatricoma,[12] angiokeratoma,[11] seborrhoeic keratosis,[6][11] lichenoid keratoses, trichilemmoma, and sebaceous adenoma.[13]
Actinic keratoses are the most common premalignant primary cause of cutaneous horn, whereas squamous cell carcinoma (SCC) is the most common malignant cause.[7] Additional premalignant and malignant causes include arsenical keratosis, pseudoepitheliomatous keratosis, micaceous balanitis, actinic keratosis, Bowen's disease, verrucous carcinoma, basal cell epithelioma, Kaposi's sarcoma, and keratoacanthoma.[8][14] Furthermore, cutaneous horns have been described in cases involving distant concomitant malignancies, such as renal cell carcinoma.[15]
Although the exact pathogenesis of the cutaneous horn is unknown, it is assumed that cellular aging, photodamage, and subsequent epithelial dysfunction contribute to their manifestation. This is supported by findings of sun exposure and old age being the most common comorbidities in patients with cutaneous horns.[15] Although not established, it has been postulated that people with fairer skin are preferentially affected.
Epidemiology
The true incidence and prevalence rates of cutaneous horns are not documented in the literature. However, it is well known that they are more commonly found in people between 60 to 80 years of age. They are also more likely to be premalignant or malignant in geriatric populations. The mean age of patients with benign cutaneous horn base pathology is 8.9 years less than those with premalignant or malignant base pathologies.[6][7]
The sex distribution of benign lesions is equal among males and females; however, males have a greater incidence of premalignant or malignant cutaneous horns.[6] This is possibly attributed to differences in social behaviors. Regardless of whether they are benign, premalignant, or malignant, cutaneous horn lesions are predominantly located in areas most vulnerable to ultraviolet radiation, such as the head, neck, and upper extremities.[3][6] Wider-based lesions are more prevalent in these sun-exposed areas of the body.[6]
These lesions are commonly reported in Caucasians and Asians, less so in people of African descent. This racial predilection could be attributed to the protection of the darkly pigmented skin from ultraviolet rays. This also explains the prevalence of the lesions in the head and neck regions.[16]
Pathophysiology
A cutaneous horn is a well-circumscribed, hyperkeratotic lesion with a height that is more than half of the diameter of its base. It can arise from any part of the skin or mucosa, with its pathophysiology being dependent upon the underlying disease. Lesions associated with benign disease processes tend to grow slowly over a few months to years.[6] However, diseases with a higher mitotic activity rate, such as SCC, can lead to a rapid growth phase and the development of horns. The more significant cumulative actinic damage and higher rates of neoplastic degeneration found in older adults make this population more prone to malignant horns.[7] Lesions with a wider base are more likely to be malignant than those with a narrower base.[6]
Montgomery (1941) classified cutaneous horns into 5 types. These subtypes were distinguished by appearance, histological structure, and causation.[14]
- Cutaneous horn arising from an epidermoid cyst
- Mucosal horn arising from a mucous membrane
- Verrucous cutaneous horn resulting from a wart
- Papillomatous cutaneous horn developing from the keratinizing stratified squamous epithelium
- Filiform cutaneous horn arising from normal or hyperkeratotic skin
The dermatology community has since moved away from Montgomery’s classic subtypes in favor of a classification system focused on underlying etiology. Although patients may still be described as having a Montgomery Type 5 cutaneous horn,[14] histopathological analysis of the underlying lesion and subsequent determination of the underlying pathology is the current model for cutaneous horn classification; namely, benign, premalignant, or malignant with a distinct variety of underlying causations defined for each category.
Histopathology
The histopathological analysis will reveal compact, redundant hyperkeratosis with or without orthokeratosis or parakeratosis. Unlike animal horns, human cutaneous horns contain cystic structures lined by trichilemmal-type epithelium and lack centrally positioned bone.[17] Giant horns (>1 cm in height) are less suitable for microscopic analysis. Histopathology of the underlying disease will be found beneath the cornified projection.[1]
History and Physical
Patients typically present with a hard, conical projection, most commonly seen over the sun-exposed areas like the face, eyelids, forearms, etc. Therefore, a history of poor or improper sun protection behaviors should raise clinical suspicion for the presence of a horn.[1] However, the lesion may be present in sun-protected areas as well. Pain may be an associated symptom, and the presence of pain has been associated with a higher chance of underlying malignancy.[1] Studies overwhelmingly indicate that absolute horn height has less of a contribution, if any, to the primary cause of the disease than factors such as height-to-base ratio, patient age, pain, histological analysis, and sun exposure.[1][3][6][10][11][15][18]
Upon tactile discrimination, the examiner will find a firmly rooted exophytic growth. Absolute widths can vary from a few millimeters to several centimeters in diameter. Absolute heights of cutaneous horns are greater on average than widths by definition but still within the range of millimeters to several centimeters. They are referred to as "giant" when they have a height greater than 1 cm.[19] Although giant horns are rarely encountered, horns up to 25 cm have been reported.[5] Currently, there is no documented correlation between the lifespan of the cutaneous horn and its classification as a benign, premalignant, or malignant lesion.
Regardless of their classification, cutaneous horns are evident, keratinous, elongated, yellowish, or white projections of various sizes.[5] These exophytic projections are conical, cylindrical, pointed, or curved, like a ram’s horn. The base of these lesions may be seen as flat, nodular, or crateriform. Surrounding erythematous inflammation is rare and indicates underlying malignancy. Cutaneous horns may be challenging to distinguish from conditions such as an ectopic nail; consequently, excision and histopathological analysis are required to confirm the suspicion of the cutaneous horn, but more importantly, to assess the underlying etiology of the lesion.[20]
Terrace morphology, indicative of benign disease, and base erythema, prognostic for malignant potential, are likely findings on dermoscopy. Terrace morphology, defined as structural horizontal contours on the side of the horn, was recorded in most cases of benign keratosis, actinic keratosis, and SCC in situ. Invasive SCC recorded the lowest significant incidence of terrace morphology. Base erythema is defined by a red, erythematous area in the base of the horn compared with the background skin within 5 mm from the horn base boundary. Base erythema occurred in over 55% of the 4 diagnostic categories studied by Pyne et al,[1] which include benign keratosis, actinic keratosis, SCC in situ, and invasive SCC. Invasive SCC displayed the greatest incidence (77%) of base erythema. Lastly, horns with a height one-to-two times greater than the base diameter have a higher incidence of malignant potential than those with lower height-to-base diameter ratios.
Evaluation
A clinical diagnosis is feasible in most settings, but many clinicians may pursue a histopathological investigation as a diagnostic adjunct. In cases in which a premalignant or malignant etiology is considered in the differential diagnosis, a biopsy is recommended to elicit the horn’s potentially carcinogenic implications. A deep biopsy or total excision is recommended to obtain a sufficient sample of the suspicious lesion.[4] It is essential to preserve the entire base of the lesion as the most superficial component of the horn consists of retained, dead keratinocytes. Obtaining an improper sample would not reveal the underlying carcinogenic cause for the horn and may lead to a false-negative diagnosis.
Further workup of the disease depends upon the histopathological findings of the primary disease process. Imaging is not required or recommended, and lab testing is unnecessary unless the primary pathology warrants further investigation.
Treatment / Management
Cutaneous horns can be treated surgically, medically, or via laser ablation. However, the cutaneous horn must be diagnosed after histological assessment due to its ability to appear like other conditions, such as an ectopic nail.[20] This assessment also serves as the most accurate method to demonstrate the underlying etiology of the condition, which is a necessary step due to premalignant or malignant concerns.
Historically, cutaneous horns have been treated using simple detachment and cauterization of the base.[5] However, the current standard of care for cutaneous horns is a complete excisional biopsy. Depending upon the histopathological diagnosis, a further management plan can be decided. For benign lesions, observation is warranted, or the lesion may be excised for aesthetic reasons and subsequently monitored periodically. Wide local excision is the preferred treatment for premalignant or malignant cases. Margins should be implemented depending on the diagnosed underlying premalignant or malignant condition. These margins should be consistent with the most updated guidelines for that condition.[21]
Ablative lasers like carbon dioxide or neodymium-doped yttrium aluminum garnet may be preferred for aesthetic considerations and electrocautery.[4][22] Cryotherapy is not a recommended treatment. Despite these alternatives, deep biopsy or total excision remain the treatments of choice, ensuring that the base of the horn is preserved for histological preparations.[4]
Patients with cutaneous horns caused by underlying SCC should also be evaluated for metastasis. For patients with basal cell carcinoma or SCC, follow-up evaluations are necessary for the first three years after diagnosis. Given the other causes for the cutaneous horn, standard follow-up for that entity is sufficient.
Differential Diagnosis
Cutaneous horns must be distinguished from the list of differential diagnoses below. Diagnosis is confirmed via clinical presentation, and histopathological analysis is crucial to determine the underlying etiology.
- Nongenital warts
- Perforating pilomatricoma
- Ectopic nail
- Seborrheic keratosis
- Actinic keratosis (AK)
- SCC
- Keratoacanthoma
- Bowen disease
- Melanoma
- Trichilemmal carcinoma
- Sebaceous adenoma
Prognosis
The prognosis of cutaneous horn lesions depends on the underlying primary disease process. These diseases can be completely benign and painless, where removal is indicated for cosmetic purposes only. However, there is a considerable chance that a premalignant or malignant cause needs to be addressed. Yu et al described a 38.9% rate at which the underlying lesions to a patient’s cutaneous horn are malignant or premalignant.[6] Therefore, a valid prognosis can only be achieved after histopathological analysis of the underlying condition. In one study, AK was found in 83.84% of premalignant cohort cases, while SCC (in situ or invasive) was discovered in 93.75% of malignant cases. This suggests AK and SCC may be the most common primary disease processes in cutaneous horns with carcinogenic potential.[7]
Complications
Patients with a cutaneous horn typically present with a hard, conical projection, usually seen over the sun-exposed areas like the face, eyelids, forearms, etc. Aside from presenting as a cosmetic issue, cutaneous horns may also be associated with pain and rapid growth. More importantly, there is a considerable chance of a premalignant or malignant complication causing the cutaneous horn. Each underlying pathology may have complications, so it is crucial to identify the underlying cause of a patient's horn. On rare occasions, giant cutaneous horns can present with varying protrusions resembling tree branches, impairing hand function.[23][24]
Deterrence and Patient Education
As sun-exposed areas are more commonly affected, counseling regarding sun protection measures is paramount. Sun-protective clothing, sunscreen, shade-seeking, and avoiding peak ultraviolet radiation hours are essential recommendations for patients with a history of prolonged sun exposure. Furthermore, counseling patients on how to perform monthly self-skin checks as well as consistent checkups are routine practices to ensure patient education and long-term wellness.
Enhancing Healthcare Team Outcomes
Cutaneous horns are uncommon, conical-shaped skin protrusions, often keratinized, arising from various underlying lesions. Clinicians encountering cutaneous horns should investigate the base lesion, as they can develop from benign to malignant conditions. Commonly found on sun-exposed areas, these horns may signify actinic keratosis, squamous cell carcinoma, or verruca. Timely biopsy and histopathological analysis are crucial for accurate diagnosis and appropriate management. Treatment involves lesion removal with a focus on the underlying pathology. Clinicians must remain vigilant, considering the potential for malignancy, and ensure comprehensive patient education on sun protection. Regular monitoring and prompt intervention contribute to optimal outcomes in addressing cutaneous horns and their associated skin conditions.
Cutaneous horns are best managed with an interprofessional team approach. Primary consultation or referral should be with a dermatologist, but clinically benign cases may be addressed in the primary care setting. Nursing support staff are essential for a thorough workup. Surgical excision, followed by histopathology, is essential for the diagnosis. As the underlying causes of cutaneous horns are varied, a further management plan should be decided based on the histopathological report.