Continuing Education Activity
This activity outlines the evaluation and management of congenital dermal melanocytosis (Mongolian spot). It explains the role of the interprofessional team in managing and considering the differential diagnoses in patients with this condition. This research was supported (in whole or part) by HCA Healthcare and/or an HCA Healthcare affiliated entity. The views expressed in this publication represent those of the author(s) and do not necessarily represent the official views of HCA Healthcare or any of its affiliated entities.
Objectives:
- Summarize the importance of ophthalmology consult for nevus of Ota.
- Outline the common physical exam findings associated with congenital dermal melanocytosis.
- Review the management options available for congenital dermal melanocytosis and when to pursue further evaluation.
- Explain the importance of improving care coordination among the interprofessional team to enhance the delivery of care for patients with congenital dermal melanocytosis.
Introduction
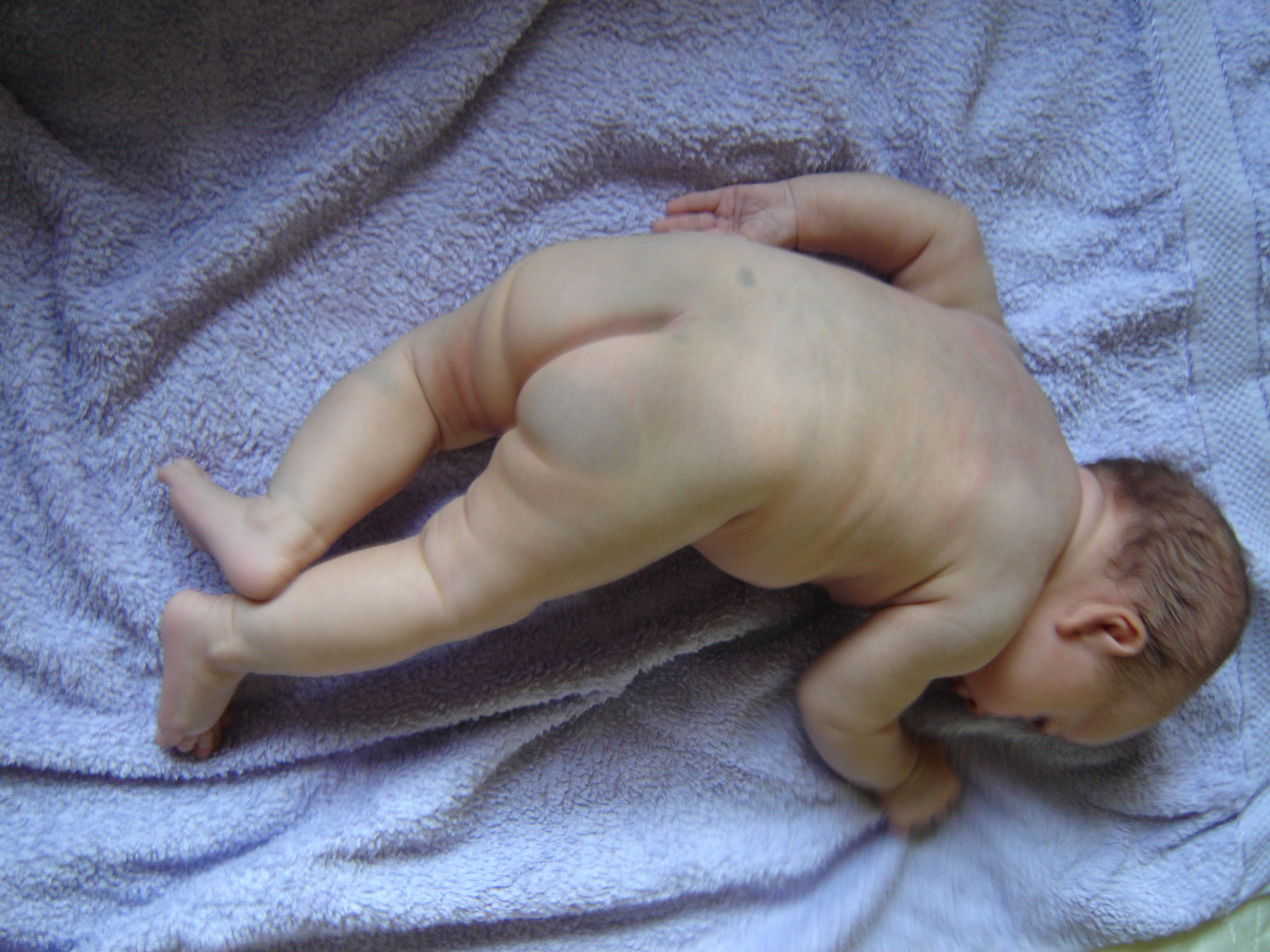
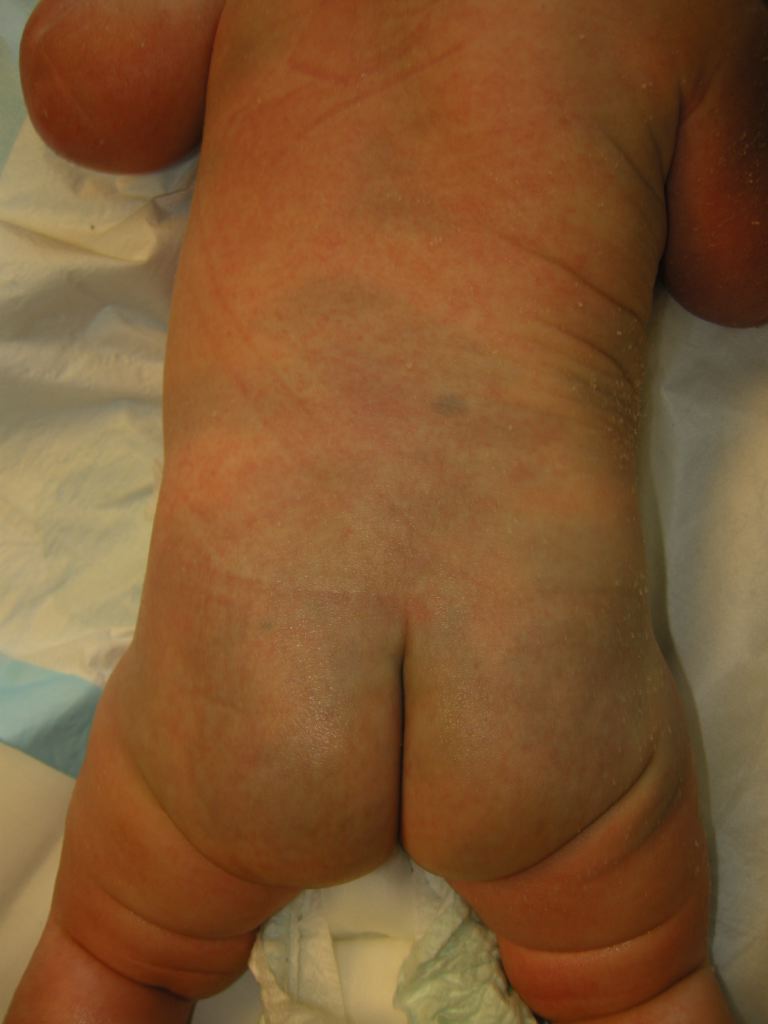
Congenital dermal melanocytosis, also known as Mongolian spot or slate gray nevus, is one of many frequently encountered newborn pigmented lesions. It is a type of dermal melanocytosis, which presents as gray-blue areas of discoloration from birth or shortly thereafter. Congenital dermal melanocytosis is most commonly located in the lumbar and sacral-gluteal region, followed by shoulders in frequency. They most commonly occur in Asian and Black patients, affect both genders equally, and commonly fade by age 1 to 6 years old. Congenital dermal melanocytoses are usually benign and do not require treatment.
Etiology
Congenital dermal melanocytosis occurs from improper migration or clearance of melanocytes from the dermal layer during fetal development.[1] There are currently no preventable factors that have been cited to affect congenital dermal melanocytosis. However, recent data support an association of aberrant congenital dermal melanocytoses with inborn errors of metabolism.[2]
Epidemiology
In congenital dermal melanocytosis, both sexes are equally affected.[2] Most patients are affected at birth or shortly after birth, with a majority of cases having the lesions disappear by 1 year old, rarely persisting after 6 years old.[3][4]
However, the prevalence is affected by population ethnicity, with the highest prevalence occurring in Asian and Black populations.[5] Multiple studies have demonstrated similar ranges in prevalences by ethnicity, as listed below:
- 81% to 100% in Asian populations [4][5][6]
- 95.5-96% of Black populations [5][6]
- 46.3 to 70.1% of Hispanic populations [5][6]
- 9.6% of White populations [5][6]
Pathophysiology
In normal fetal development, melanocytes (derived from neural crest cells) are present in the dermis of the embryo by ten weeks gestational age and migrate to the epidermis between weeks 11 to 14 of gestation. No melanocytes should remain in the dermal layer by week 20 of gestation via migration or macrophage clearance. In congenital dermal melanocytosis, melanocytes remain in the dermis and actively produce melanin. The blue-gray color of affected skin can be explained by the Tyndall effect, where dermal melanin scatters the shorter wavelengths of light (blue light), which reflect to the skin surface. An extracellular fibrous sheath protects the dermal melanocytes. However, this sheath becomes gradually lost and destroyed during fetal life and early childhood.[1]
Histopathology
Spindle-shaped cells that contain pigment located between collagen fibers deep within the dermis.
History and Physical
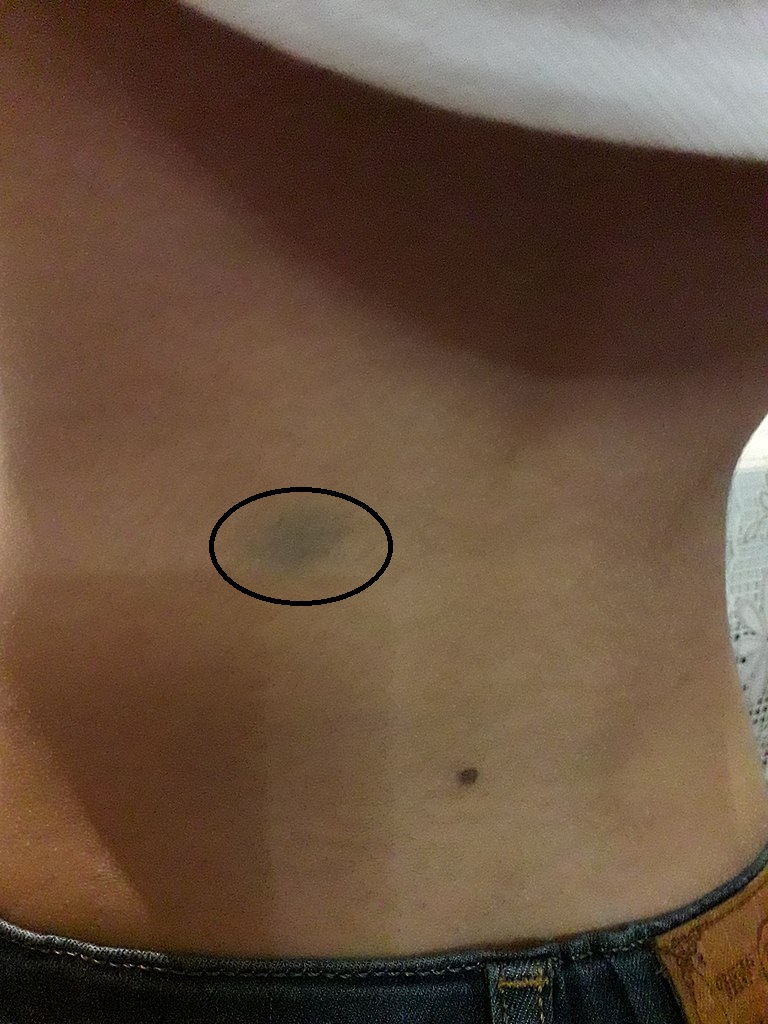
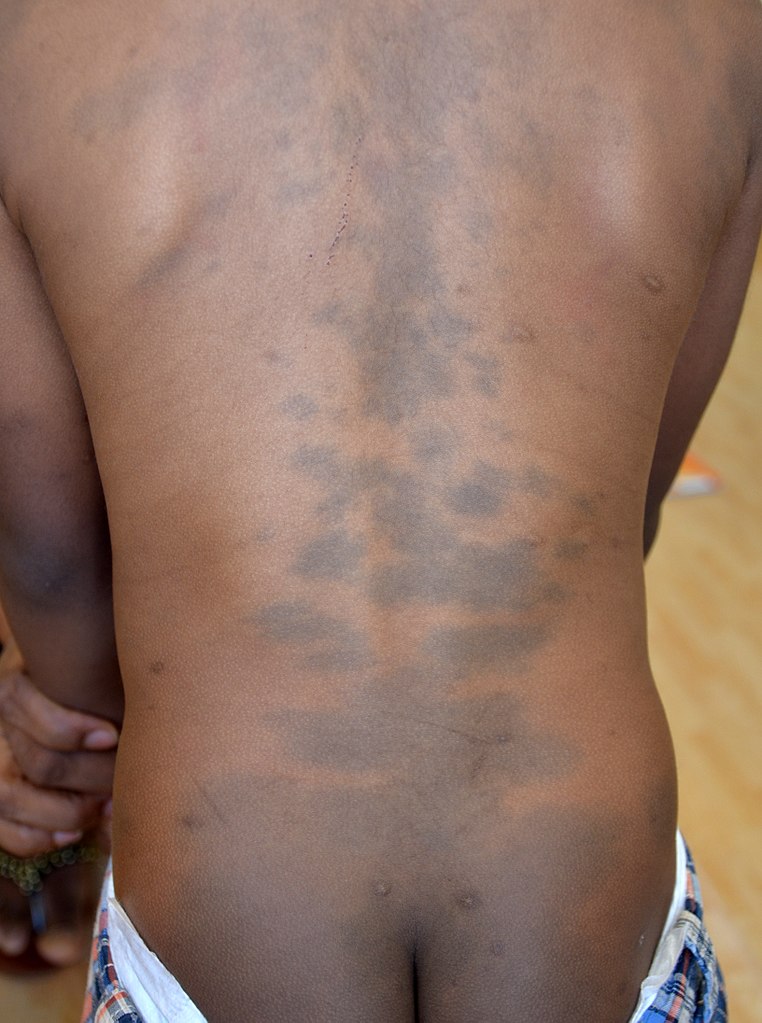
Congenital dermal melanocytosis commonly appears as a single or multiple hyperpigmented macular lesion(s) on the lower lumbar, sacral, or gluteal surface. The pigmentation of the lesion ranges from dark grey, blue, to blue-green. The shape of the lesion can vary from round, oval, or irregular. These lesions can appear at birth or shortly after birth.[1] A majority of cases have less than 5% total body surface area involvement. Aberrant lesions are classified as extra-sacral, and they can occur on the lower extremities, upper extremities, groin, shoulder, and chest.[2] However, extra-sacral lesions that involve the face or orbits may be Nevus of Ota.
Congenital dermal melanocytosis lesions commonly fade by 1 year old, rarely persisting after 6 years old.[3][4] Lesions that are extra-sacral in location, greater than 10 cm, or are darker in color are the cases more likely to persist after 1-year-old.[2]
Asking parents or caretakers about the onset of lesions and the location of the affected site will aid the clinician toward the correct diagnosis. Clinicians should perform a detailed history and physical and use their clinical judgment to assure that congenital dermal melanocytosis is not confused for other possible diagnoses. Congenital dermal melanocytosis can resemble the bruises that occur in non-accidental trauma. Documentation of these lesions on initial evaluation is important to help delineate from suspected abuse in subsequent visits. Congenital dermal melanocytosis should also be differentiated from other dermal melanocytoses such as nevus of Ota (melanocytic pigment around the face and orbits, usually in a unilateral trigeminal nerve distribution) or nevus of Ito (melanocytic pigment involving the neck, supraclavicular and scapular regions).[2]
Evaluation
Congenital dermal melanocytosis is a benign condition, and further laboratory, radiographic, or histologic workup is not necessary.[1]
Ophthalmological evaluation is required in the case of Nevus of Ota (oculodermal melanocytosis), especially if involvement of the sclera is seen.
Treatment / Management
Congenital dermal melanocytosis will commonly fade within 1 year, rarely persisting after 6 years old. However, for extra-sacral lesions can be treated for cosmetic purposes. A previous case of congenital dermal melanocytosis involving the mandibular area reported significant improvement after four treatments with a 755-nm Q-switched alexandrite laser.[7]
Differential Diagnosis
Differential diagnosis of gray-blue lesions includes other dermal melanocytoses and non-accidental trauma. Nevus of Ota (oculodermal melanocytosis) will typically involve the face & orbits in a unilateral trigeminal nerve distribution. Nevus of Ota does not regress and can be associated with orbital melanocytoma, which requires resection.[2] Another dermal melanocytosis that does not regress is Nevus of Ito, where the melanocytic pigment involves the neck, supraclavicular & scapular regions. There have been rare cases of malignant transformations noted, particularly if there are fast-growing nodules.[8] Non-accidental trauma should be particularly considered if there are lesions in atypical areas, tenderness to palpation of the lesion, or multiple lesions in various stages of healing.[9]
Prognosis
Congenital dermal melanocytosis is a benign condition that rarely persists beyond the first decade of life. Congenital dermal melanocytosis does not have malignant transformations, unlike nevus of Ota or nevus of Ito.[1]
Complications
For patients with persistent extra-sacral lesions, treatment may be pursued for cosmetic purposes.
Consultations
Ophthalmological evaluation is required for nevus of Ota, especially when sclera s involved.
Deterrence and Patient Education
Parents should be informed of the benign nature of congenital dermal melanocytosis; it requires no further treatment or evaluation. Parents are educated that this condition should fade by 1 year old and rarely persist past 6 years old. Should extra-sacral lesions persist, laser therapy is a potential option for cosmetic treatment.
Pearls and Other Issues
There have been a number of publications that suggest that congenital dermal melanocytosis may be associated with inborn errors of metabolism, particularly cases where the dermal melanocytosis is extensive. These inborn errors of metabolism include lysosomal storage diseases such as Hurler disease and GM1 gangliosidosis 1.[10] The exact mechanism linking congenital dermal melanocytosis to inborn errors in metabolism is not known, although there are proposed mechanisms involving accumulated metabolites affecting tyrosine kinase receptors on melanocytes, leading to abnormal melanocyte migration.[1]
Enhancing Healthcare Team Outcomes
Pediatricians and primary care providers that work with newborns and infants will frequently encounter congenital dermal melanocytosis in their practice. While congenital dermal melanocytosis is a benign condition that commonly self-resolves within the first decade of life, it is important for the health care providers to be able to recognize lesions that are atypical of congenital dermal melanocytosis as these could be signs of physical abuse or other pathology that warrants further evaluation. Parents and caretakers should be educated by clinicians, nurses, physical therapists, occupational therapists, and pharmacists on the benign nature of this skin condition that requires no further treatment or evaluation. This should alleviate any worries or concerns of the patient’s caretakers.