Continuing Education Activity
Pinna perichondritis requires prompt and effective intervention to prevent potential disfigurement of the external ear and the risk of developing severe soft tissue or systemic infections. Perichondritis of the pinna is a challenging medical concern, and this course is designed to equip healthcare professionals with the knowledge and skills required for its evaluation and management.
This explores the latest diagnostic and treatment approaches for pinna perichondritis, emphasizing the importance of early recognition and intervention. Furthermore, it will highlight the critical role of the interprofessional healthcare team in ensuring optimal patient outcomes. By participating in this program, learners gain a deeper understanding of the condition, enabling them to enhance their clinical competence and contribute to better patient care.
Objectives:
Identify how pinna perichondritis can lead to ear deformity.
Identify the signs and symptoms of pinna perichondritis.
Determine the treatment for pinna perichondritis with consideration of the causal organisms.
Identify how an interprofessional team can work together to identify and treat pinna perichondritis.
Introduction
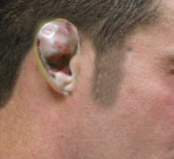
Perichondritis of the pinna is inflammation of the perichondrial layer surrounding the cartilage of the ear. Penetrating trauma to the ear, such as transcartilaginous high ear piercings, is the most common cause of perichondritis. Nonmedical practitioners carry out the majority of ear piercings, and if sterile conditions are not maintained, this can precipitate infection. If the infection is neglected, an abscess can form, which causes perichondrial elevation from the cartilage, resulting in devascularisation. This will cause necrosis and alteration to the shape of the pinna. If blood collects in this space, it may organize and form hard scar tissue, giving the appearance of a cauliflower ear (see Image. Cauliflower Ear). It can also progress to a severe soft tissue or systemic infection if left untreated.
Etiology
There are several causes of perichondritis of the pinna. However, the most identified cause in the literature is penetrating trauma to the cartilaginous pinna.[1][2] Some authors have linked a rise in perichondritis cases in the past decade to the increasing amount of transcartilaginous ear piercings, which, compared to lobule piercings, carry a greater risk of infection or abscess formation.[3] The risk of infection is increased after exposure of the wound to fresh water or hot tubs immediately after the procedure.[4] Less common causes include untreated middle or external ear infections spreading to the pinna and cartilage, iatrogenic (post-surgery), immunosuppression, and minor trauma such as scratching the ear. There is also a significant proportion of patients who have no identifiable cause.[1]
The most common causative organism of perichondritis of the pinna is Pseudomonas aeruginosa, which seems to prefer damaged cartilage. Other causative organisms include Staphylococcus aureus and Escherichia coli.[1][3][5] Perichondritis can also be caused by herpes zoster infection, perhaps from vesicles enabling a route of entry for bacteria to invade.[5]
Epidemiology
Perichondritis of the pinna is not a common condition. Its incidence is unknown; however, it has been reported that the number of cases doubled between 1990 and 1998 in England. This increase was attributed to the increase in ear piercings among adolescents.[6]
Pathophysiology
The perichondrium is a layer of dense connective tissue that surrounds the cartilage. It facilitates the growth and repair of the cartilage. Trauma can cause microfractures of the cartilage and cause the perichondrial layer to strip off the cartilage, resulting in devascularisation and necrosis.[6] The scanty blood supply to this area makes it especially susceptible to infection despite even aseptic techniques of ear piercing.[7] This necrosis leads to cosmetic deformity. If blood collects in the space created by the elevated cartilage, it will collect and harden to form a permanent structural deformation, colloquially known as the "cauliflower ear." If left untreated, perichondritis can lead to infection of the surrounding soft tissue, causing pinna cellulitis or abscess formation.
Histopathology
A histological study was performed by Van Wijk et al, which set out to measure the extent of cartilage damage by ear-piercing techniques on cadavers. They showed that piercing caused the perichondrium to tear off the cartilage, creating a detachment pocket that could enable the formation of an abscess.[8]
History and Physical
Perichondritis of the pinna is a clinical diagnosis. Therefore, a focused history and thorough physical examination are essential. The history should include any recent significant trauma to the lateral face and ear, including piercing, acupuncture, abrasions, burns, lacerations, or pinna hematoma. Clinicians should ask about relevant symptoms such as hearing loss, otorrhea, or cranial nerve abnormalities, which would point to a different diagnosis. Particular attention should be paid to comorbidities in the patient’s past medical history, such as diabetes or immunosuppression, that could increase the likelihood of infections.
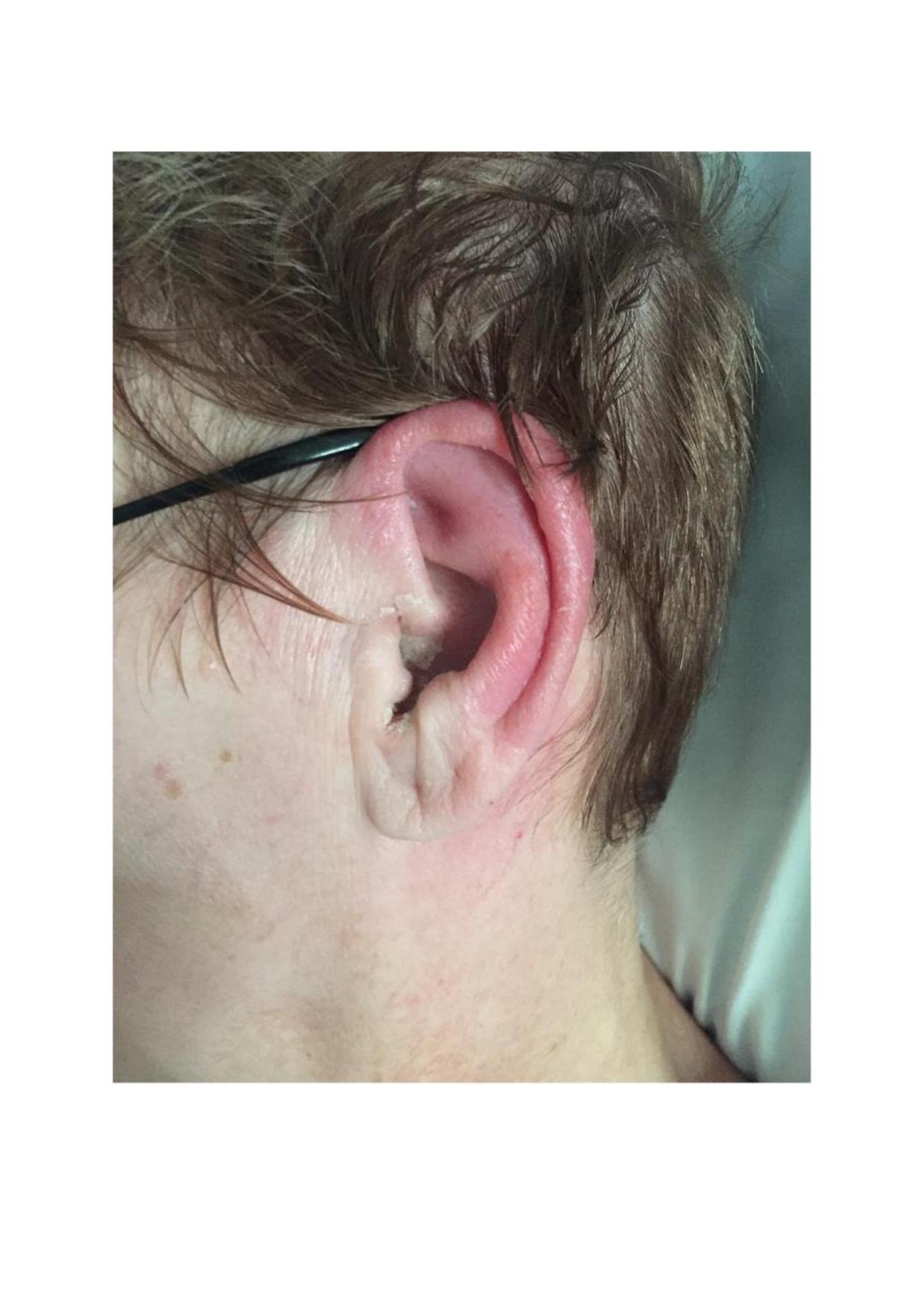
Physical examination should include a comprehensive ear exam with an inspection, palpation, and otoscopy. Patients will typically present with an erythematous, swollen, hot, painful pinna (see Image. Pinna Perichondritis). In perichondritis, the lobule is often spared, helping to differentiate it from pinna cellulitis.[9][10] This is important as there are different causative organisms for both, and if pinna cellulitis is present, it would be prudent to mark the affected area. There may be a small abscess present or necrosis of the soft tissue. Palpation will reveal a tender pinna. To complete the examination mastoid process, pre and post-auricular regions should be examined for tenderness. A cranial nerve exam and neck swelling exam should be performed as indicated. Systemic symptoms such as pyrexia or extension of erythema beyond the pinna suggest that the infection has spread beyond the external ear. Careful otoscopy should be performed, with the unaffected ear examined first. The clinician should look for any debris or discharge, erythema, or swelling in the external ear canal, which would point to perichondritis caused by otitis externa, which is primarily treated with suction clearance and topical antibiotics. The tympanic membrane should also be assessed for an air-fluid level or perforation.
Lastly, if a patient presents with inflammation of both pinnae, nose, and joints or tracheobronchial abnormalities, consider a diagnosis of relapsing polychondritis, which is an autoimmune condition and is primarily treated with oral steroids.[11]
Evaluation
Routine blood tests are not usually indicated in simple pinna perichondritis. However, suppose there is an extended area of swelling, an abscess, or necrosis. In that case, blood tests should be obtained, including complete blood count, urea and electrolytes, c-reactive protein, blood cultures, and coagulation screen. This should also form part of a sepsis screen in an unstable patient. Microbiology swabs should be taken of the affected area and any discharge present. Imaging is not indicated unless there is a suspicion of intracranial pathologies, such as an abscess.
Treatment / Management
Antibiotic therapy is the mainstay of treatment for pinna perichondritis. The management pathway is dependent on the presence or absence of abscess formation. If an abscess is present, the patient should be admitted to the hospital for definitive treatment. This consists of admission blood tests and preparing the patient for surgery while considering an incision and drainage of the pinna to remove the collection of pus or hematoma. If there is no abscess present, the patient should be started on both oral and topical antibiotics. Considering the casual organisms, clinicians should initiate an antibiotic regime that provides adequate coverage for Pseudomonas aeruginosa and Staphylococcus aureus. Clinicians should follow local antimicrobial prescribing guidelines and seek microbiology advice if unsure.
Fluoroquinolone antibiotics are readily available in oral and topical forms and provide excellent staphylococcal and pseudomonal cover. Historically, they have been avoided in the pediatric population due to side effects of arthralgias and tendon rupture.[2] A meta-analysis of fluoroquinolone use in children showed a low incidence of musculoskeletal side effects, which all resolved on medication withdrawal, and no studies have shown growth disturbances associated with its use. This suggests that a short course for a pediatric patient is safe to use.[12] Fluoroquinolone antibiotics are well absorbed with good bioavailability, eliminating the need to use intravenous antibiotics unless the patient is nil by mouth or concerned about an unsafe swallow. However, clinicians should not forget this is a painful condition, and therefore, adequate analgesia should be prescribed alongside treatment.
Differential Diagnosis
Clinicians should be aware of various pathologies that can cause a painful, inflamed external ear. When examining children, it is vital to perform an otoscopy to rule out complicated otitis media, as they will not be able to communicate their symptoms as effectively as adults.
Differential diagnoses that should be considered include:
- Pinna cellulitis
- Otitis externa
- Otitis media
- Dermatological conditions affecting the ear, ie, eczema or psoriasis.
- Malignant otitis media
- Relapsing polychondritis
Prognosis
With prompt diagnosis and treatment with antibiotic therapy, the symptoms should settle in 2 or 3 days. However, symptoms such as pain can persist for up to a month. Cosmetic deformity depends on the severity of the infection and the damage to the underlying cartilage.[1] This is especially important in perichondritis with abscess formation, which requires surgical treatment, and cartilage may be damaged. Patients who have an incision and drainage will require packing and re-dressing the wound to allow it to heal without recollection.
Complications
If left untreated, perichondritis will lead to cartilage necrosis and minor cosmetic deformity or ‘cauliflower ear.’ Perichondritis of the scapha (the hollow part of the helix) has been reported to be associated with a greater risk of ear deformity than the helix itself.[2] The infection can also spread beyond the pinna and cause the patient to become systemically unwell, needing intravenous antibiotics and hospital admission.
Deterrence and Patient Education
Patients should be aware of the increased risk of high ear piercings causing pinna perichondritis, as opposed to simple lobule piercing. If they develop a painful, swollen, red external ear, they should seek professional health advice. Delaying care could cause permanent deformity of the ear.
Enhancing Healthcare Team Outcomes
Pinna perichondritis is an infection of the perichondral lining of the ear cartilage. It is primarily caused by Pseudomonas aeruginosa and Staphylococcus aureus. Patients will present with an erythematous, swollen, hot external ear, with sparing of the lobule. There may also be a collection of pus present. It is commonly caused by minor trauma, such as ear piercings through the cartilaginous pinna, but other causes must be considered.
A prompt diagnosis is needed so the appropriate antibiotic therapy can be started. While this is primarily an ear, nose, and throat (ENT) condition, uncomplicated cases such as those without a collection can be managed in a primary care setting with oral antibiotic therapy. Any concerns regarding antibiotic therapy should prompt consultation from ENT surgeons, infectious disease specialists, and pharmacists. They will be able to advise what the local protocol for antibiotic therapy is in both adult and pediatric patients.
If the medical practitioner has identified a complicated pinna perichondritis with an abscess and necrosis, a referral to the ENT surgeons should be made as management involves surgical incision and drainage or debridement of the pinna. If there is a late presentation of this condition, the patient should be counseled on the possibility of residual cosmetic deformity.
A delay in treatment or misdiagnosis can cause permanent damage, so it is essential to manage this condition quickly and effectively. It is crucial to distinguish pinna perichondritis from relapsing polychondritis as both have different management plans.