Continuing Education Activity
Diphtheria is a toxin-mediated infection primarily caused by Corynebacterium diphtheriae, a member of the Corynebacterium species. This infectious disease is characterized by skin and mucosal infections, occasionally progressing to focal infection after bacteremia. The clinical manifestations of C diphtheriae infection are diverse and depend on factors such as the anatomical site of infection, the immune status of the host, and the production and systemic distribution of toxins.
This comprehensive activity provides an in-depth exploration of diphtheria, covering its epidemiology, pathogenesis, clinical features, diagnosis, and management. Emphasizing the collaborative role of an interprofessional healthcare team, the activity aims to equip healthcare professionals with the knowledge and skills necessary for the practical evaluation and management of patients affected by this highly contagious disease.
Objectives:
Implement evidence-based strategies for the timely and accurate evaluation and diagnosis of diphtheria in clinical practice.
Apply comprehensive knowledge of diphtheria pathogenesis and toxin distribution in developing effective management plans.
Select appropriate interventions, including antitoxins and antibiotics, for treating diphtheria, considering individual patient factors.
Coordinate care efforts for patients with diphtheria, emphasizing the importance of a cohesive and integrated healthcare approach.
Introduction
Corynebacterium diphtheriae, a nonencapsulated, nonmotile, aerobic gram-positive bacillus, is the bacterium responsible for causing diphtheria. The primary risk factor for contracting this disease is the absence of immunization. While individuals may carry the bacterium asymptomatically, it often impacts the respiratory and integumentary systems. Humans serve as the exclusive hosts for this organism, which resides in the upper respiratory tract, and transmission of the bacteria occurs through airborne droplets.
The infection tends to be more prevalent during the spring or winter months. Without antibiotic intervention, its communicability persists for 2 to 6 weeks.[1] Those with diminished antitoxin antibody levels or incomplete immunization are particularly susceptible to infection and may contract the illness upon exposure to a carrier or an individual already afflicted. In this context, a carrier refers to an asymptomatic individual whose cultures test positive for C diphtheriae. As the number of carriers decreases, there is a corresponding decline in the disease occurrence among the population.
The organism's pathogenicity hinges on the production of exotoxins, which can lead to severe complications, primarily affecting the heart muscle and nervous system. Timely diagnosis plays a pivotal role in achieving favorable clinical outcomes, as initiating antitoxin therapy and appropriate antibiotics early on can significantly impact patient prognosis.[2]
Although the disease is more prevalent in tropical regions, it is a global concern. Patients typically present with a distinctive thick, gray, and adherent pseudomembrane on the tonsils and throats. Diagnosis involves isolating the organism, culturing it, and monitoring toxin production. Management includes patient isolation and the administration of antitoxin and antibiotics.
In prevention, vaccination against diphtheria is incorporated into the routine vaccination schedule as part of the combination diphtheria, tetanus toxoid, and acellular pertussis vaccine (DTaP). The adoption of DTaP in the US has remarkably diminished the occurrence of diphtheria. As acquired immunity naturally wanes with time, a booster is recommended to sustain protection. While vaccination does not provide a guarantee against diphtheria, individuals who have received the vaccine tend to experience less severe and fewer fatal diphtheria infections.[3]
Etiology
C diphtheriae is a non–spore-forming gram-positive bacillus characterized by its nonmotile, nonencapsulated nature. Its distinctive club-shaped appearance forms palisades or V- or L-shaped arrangements. Besides C diphtheria, Corynebacterium ulcerans can induce cutaneous diphtheria and, rarely, contribute to respiratory diphtheria cases.[4]
The pathogenic impact of exotoxins extends to both localized and systemic manifestations of the disease. Viral bacteriophages carry the genetic code for exotoxins, facilitating their transmission among bacteria. Three distinct strains of C diphtheriae—gravis, intermedius, and mitis—have been isolated, and all 3 are capable of toxin production.[5]
The pathogenesis of diphtheria involves various etiological factors, including:
- Incomplete or absent immunization [6]
- Waning immunity over time, rendering older individuals without booster vaccination more susceptible to infection
- Low herd immunity
- Travel to endemic areas
- Travel to regions experiencing current epidemics
- Immunocompromised states
- Low socioeconomic status
- Large-scale population movements
- Overcrowded conditions, such as military barracks, jails, and homeless shelters
- Domestic animals [7]
Epidemiology
Since the implementation of the vaccine, the incidence of the disease has witnessed a rapid decline. Before 1920, the US reported approximately 200,000 annually.[8] However, this number has drastically decreased following the introduction of widespread immunization programs, with only around 1000 cases reported annually. Most cases are observed in individuals with low socioeconomic status, living in overcrowded conditions, lacking immunizations, with a travel history from endemic regions, and having comorbid conditions. These numbers remain higher in certain global regions, particularly Southeast Asia and Africa. Regarding mortality in the US, the figures have decreased from 100 to 200 cases to 0.001 per 100,000 population since the advent of vaccinations.
Reports from the World Health Organization (WHO) suggest that diphtheria epidemics continue to pose a health risk in developing countries. India has experienced a higher incidence of diphtheria, primarily attributed to challenges in implementing widespread vaccination efforts.[9] A significant proportion of the global burden of diphtheria is concentrated in India.[9][10]
Diphtheria does not exhibit any racial or sexual preference. While diphtheria is commonly recognized as a childhood disease, predominantly affecting those below 12 years, individuals around the age of 40 and those with comorbid conditions are also susceptible to infection. As immunity against the bacteria naturally wanes, the risk of infection rises for individuals not currently receiving immunizations and booster doses.[11]
Pathophysiology
Humans are the primary reservoir for diphtheria infection; nevertheless, case reports suggest a link between diphtheria and livestock.[12] Infected individuals and asymptomatic carriers can act as a source of C diphtheriae transmission through respiratory droplets, nasal secretions, and, rarely, fomites.
Exotoxin production is the primary mechanism through which the organism manifests its distinctive clinical features. The exotoxin is a singular polypeptide composed of 2 subunits, A and B. The B subunit facilitates the toxin binding to the receptor on the cell membrane, while the A subunit possesses enzymatic properties, cleaving nicotinamide from nicotinamide adenine dinucleotide (NAD). This cleavage inhibits protein synthesis through adenosine diphosphate (ADP)-ribosylation of elongation factor 2 (EF-2). The host's response to the bacteria induces local inflammation in the throat and pharynx, giving rise to a resilient, gray pseudomembrane—an identifiable hallmark of the disease.
Local tissue destruction facilitates the lymphatic and hematologic spread of the toxin to various body systems. This diphtheria toxin may damage distant organs, including the kidneys, myocardium, and the nervous system.[13] Infections resulting from nontoxigenic strains generally exhibit milder severity.
History and Physical
Diphtheria typically initiates with nonspecific flu-like symptoms, including fever, sore throat, and cervical lymphadenopathy. The average incubation period spans 2 to 5 days, ranging from 1 to 10. A travel history from an endemic region with no vaccination records is often indicative. In such instances, healthcare practitioners should be alert to the hallmark features of the disease, notably the presence of a thick, gray, adherent pseudomembrane covering the tonsils and throat. Respiratory tract involvement is common, commencing with mild erythema that later evolves into a merging pseudomembrane.
The pseudomembrane comprises red blood cells (RBCs), white blood cells (WBCs), dead cell debris, and organisms. Attempting to scrape it from the adhering surface often results in bleeding. Typical symptoms and signs of diphtheria encompass low-grade fever, sore throat, malaise, cervical lymphadenopathy, headache, and dysphagia. According to a study by Pancharoen C et al, the most common manifestations of diphtheria included patchy lesions, followed by fever and upper respiratory tract infection.[14] Furthermore, systemic involvement occurs as the toxin leaks into the lymphatic and hematologic system following local tissue destruction.
Cervical adenopathy and swollen mucosa often result in a distinctive "bull neck" appearance in many infected patients.[15] The leading cause of mortality is airway obstruction or suffocation, primarily due to the aspiration of the pseudomembrane.
In cutaneous diphtheria, one can observe ulcerating skin lesions covered by a gray membrane. These lesions do not spread or invade surrounding tissues. The site for these cutaneous lesions typically involves previously injured tissues, often stemming from trauma or preexisting dermatologic lesions.[16][17]
Physical Examination
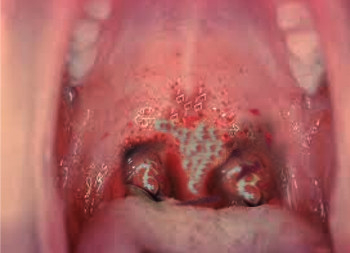
Patients typically exhibit a low-grade fever but appear toxic, often accompanied by a swollen neck. General symptoms include fever, tachycardia, halitosis, and anxiety. A thick, gray, leathery membrane covers the tonsils, oropharynx, soft palate, nasopharynx, and uvula (see Image. Diphtheria in the Oral Cavity). Scraping the pseudomembrane causes bleeding of the underlying mucosa. The patient may hold their head extended due to the bull neck. Occasionally, there can be dysphonia. Respiratory distress manifests as stridor, wheeze, cyanosis, and retractions.
Cardiac involvement occurs after 1 to 2 weeks of illness after improvement in the pharyngeal phase. Cardiact involvment may manifest as follows:
- Myocarditis can present acutely with congestive heart failure and circulatory collapse. Patients can have more subtle features, such as progressive dyspnea, cardiac chamber dilatation, diminished heart sounds, and weakness.[18]
- ST-T wave changes, atrioventricular blocks, and various dysrhythmias may be evident.
- Endocarditis, particularly in the presence of an artificial valve.[19]
Neurological involvement depends on the extent of the pharyngeal infection. Deficits include the following:
- Cranial nerve deficits
- Stocking and glove peripheral sensory neuropathy
- Peripheral neuritis[20]
Evaluation
Diagnosing diphtheria involves a combination of clinical evaluation, laboratory tests, and sometimes imaging studies. An overview of the various tests used to evaluate diphtheria are as follows:
Clinical Evaluation
- Throat culture: A swab is taken from the pseudomembrane or any visible lesions for culture to identify C diphtheriae. The throat swab is cultured on specific media to isolate the bacteria. Commonly used media include Löeffler or Tindale medium, telluride plates, and blood agar. The particular characteristics of these mediums indicate the presence of the organism:
- Tindale medium: C diphtheriae forms a distinctive black colony with halos
- Löffler medium: Metachromatic granules are observed in the presence of C diphtheriae.
- Telluride plate: the typical gray-black color of tellurium is indicative of the organism's presence
- Gram stain: Identifying Gram-positive bacilli with characteristic club-shaped appearance can support the diagnosis. Although Gram staining does not confirm the diagnosis, the initial test is performed in suspected cases. The smear is also stained with methylene blue, which reveals the typical metachromatic granules.
- Patient history and physical examination: Travel history, immunization status, and clinical symptoms such as sore throat, fever, and pseudomembrane formation are considered in the diagnosis.
Laboratory Tests
- Toxin detection: Toxin production by the bacteria can be confirmed through laboratory tests, such as the Elek test, polymerase chain reaction (PCR) testing, and enzyme immunoassay (EIA) test.[21]
- Serology: Blood tests can measure antibody levels against diphtheria toxin, providing information about the patient's immune response.
Imaging Studies
- Chest x-ray: If respiratory symptoms or concerns about complications like pneumonia are present, a chest x-ray may be performed to assess lung involvement. This imaging study may reveal swelling of the soft tissue structure in and around the pharynx, epiglottis, and chest.
- Echocardiogram: In cases of suspected cardiac involvement, an echocardiogram can help assess the function and structure of the heart and possibly reveal valvular vegetation, although this is a rare phenomenon.[22]
Other Laboratory Studies
- CBC: An elevated WBC may indicate an inflammatory response.
- Troponin level: This study may be beneficial to assess the extent of the myocardial injury.[23]
Treatment / Management
The primary treatment approaches for diphtheria involve promptly administering antitoxins and antibiotics. Additionally, the patient should undergo a thorough assessment for potential respiratory and cardiovascular instabilities. In suspected cases of diphtheria, antitoxin should be administered urgently based on clinical judgment without waiting for laboratory confirmation. Suspected cases must be isolated, and stringent droplet precautions should be implemented. Furthermore, the patient should be evaluated for signs of respiratory distress, and ensuring an airway is imperative. Early management also involves continuous cardiac monitoring to address any potential cardiovascular complications.
Diphtheria Antitoxin
Diphtheria antitoxin (DAT), derived from horse antiserum, is crucial in treatment.[24] Antitoxin functions by neutralizing unbound diphtheria toxin circulating in the blood. The antitoxin becomes ineffective once the toxin has bound to the cell membrane. The dosage of antitoxin is tailored to the patient's clinical state and the severity of the condition, and it can be administered intramuscularly or intravenously. Before antitoxin administration, the patient should undergo hypersensitivity testing, and emergency anaphylaxis medication must be readily available at the bedside.
Antibiotic Treatment
The antibiotics of choice for treating diphtheria are erythromycin or penicillin G.[25] Erythromycin is prescribed at a dose of 500 mg 4 times a day for a 2-week duration. Penicillin G is administered intramuscularly, with a dosage of 300,000 units every 12 hours for patients weighing 10 kg or less and 600,000 units every 12 hours for those weighing more than 10 kg. Once the patient can take oral medication, oral penicillin V can be initiated at a dose of 250 mg 4 times daily for 2 weeks. Early initiation of antibiotics is crucial to eliminate the organism promptly, limiting toxin release, expediting patient recovery, and preventing infection spread to close contacts. In cases of antibiotic resistance, linezolid or vancomycin may be considered.
Close contacts, including household members and individuals in direct contact with the infected patient, should receive contact prophylaxis. Medical staff exposed to a patient's respiratory secretions should also undergo prophylaxis. Contact prophylaxis involves a single dose of penicillin G administered as follows:[26]
- 600,000 units intramuscularly for individuals younger than 6 years
- 1.2 million units intramuscularly for individuals 6 or older
Alternatively, oral erythromycin can be given at a dose of 500 mg 4 times a day for 7 to 10 days. Ensuring timely and comprehensive antibiotic treatment is essential for the individual patient, preventing potential outbreaks and minimizing the risk of complications in the broader community.
Differential Diagnosis
Distinguishing diphtheria from other upper respiratory tract infections with similar presentations is crucial. Relevant differentials to consider during the diagnostic process include:
- Epiglottitis: Characterized by acute inflammation of the epiglottis and surrounding structures.[27][28]
- Retropharyngeal abscess: Manifests with high-grade fever and requires urgent drainage.[29]
- Angioedema: Presents as generalized swelling involving the lower dermis and subcutaneous/submucosal tissues.[30]
- Infectious mononucleosis: Features fatigue, malaise, sore throat, fever, nausea, anorexia, and cough. The classic presentation in children includes fever, pharyngitis, and lymphadenopathy.[31][32]
- Pharyngitis: Exhibits sudden onset of sore throat, odynophagia, fever, and cough.[33]
- Oral candidiasis: The grayish pseudomembrane in diphtheria must be differentiated from the whitish appearance of oral candidiasis.[34][35]
- Vincent angina: Involves infection of the gums, presenting with painful, bleeding gums and ulcerative gingiva necrosis.
Prognosis
The prognosis of diphtheria is influenced by several factors:
- High mortality rates are observed in individuals younger than 5 and those older than 40.
- Cases with an onset duration exceeding 4 days are associated with elevated mortality.
- Cardiovascular involvement, particularly atrioventricular and left bundle-branch blocks, is associated with a poor prognosis.
- Systemic involvement is a significant predictor of high mortality rates.[36]
Complications
The primary complications of diphtheria often involve myocarditis and neuritis.[37][38] Fatality occurs in 5% to 10% of cases. Another critical complication arises from pseudomembrane formation in the upper respiratory tract, potentially causing respiratory obstruction, necessitating urgent mechanical ventilation and intubation.[39]
Cardiac Complications
Diphtheria can manifest with myocarditis characterized by cardiac arrhythmias, present as first, second, or third-degree heart block, often leading to circulatory collapse.[23] Electrocardiogram (ECG) changes in affected patients include a prolonged P-R interval and ST and T wave changes.
Neurologic Complications
Neurological complications in diphtheria include nerve weakness or paralysis, particularly involving the cranial nerves and affecting the nerves in the extremities, leading to muscle weakness in the extremities. The involvement of the pharyngeal muscles and the soft palate can result in regurgitating foods and fluids through the nose. While uncommon, encephalitis stemming from diphtheria complications can manifest in children.[40]
Consultations
For the effective management of diphtheria, the following consultations may be essential:
- Centers for Disease Control and Prevention: Given the unavailability of commercially sourced antitoxins, immediate contact with the Centers for Disease Control and Prevention (CDC) is imperative to notify and discuss the case before obtaining the necessary antitoxins.
- Infectious disease center: Suspected cases must be promptly reported to contagious disease centers for early intervention.
- Cardiology: In instances of cardiac complications, consulting cardiology becomes crucial. This ensures a comprehensive assessment of the disease extent and facilitates the implementation of measures required for managing cardiac dysrhythmias and heart block.
- Critical care service: Patients with severe forms of the disease and those experiencing septicemia should be admitted to the intensive care unit, necessitating management by critical care services.
- Otolaryngology and anesthesia: Consultations with an otolaryngologist and anesthesia specialists are essential to determine the extent of the disease spread. Their expertise becomes crucial in cases requiring respiratory distress interventions, such as intubation.
- Pulmonology: Pulmonology consultations aid in evaluating the extent of the disease within the respiratory tract, contributing to a comprehensive understanding of the condition.
Deterrence and Patient Education
Vaccines for diphtheria are formulated as toxoids, which are denatured proteins (bacterial toxins) with an intact receptor binding site capable of eliciting antibody production. Generally, diphtheria vaccination is administered in combination with vaccines targeting tetanus and pertussis. Various forms of the combined diphtheria vaccine include:
- DTaP: Protection against diphtheria, tetanus, and pertussis.
- Tdap: Protection against tetanus, diphtheria, and pertussis
- DT: Protection against diphtheria and tetanus
- td: Protection against tetanus and diphtheria
In the US, the DTaP vaccination schedule is implemented for neonates, with doses administered at ages 2, 4, and 6 months. The fourth dose is between ages 15 and 18 months, and the 5th dose is administered between ages 4 and 6. The booster vaccine is administered at age 11 to 12, utilizing the Tdap vaccine. Subsequently, booster doses of Tdap or td are given every 10 years throughout life. Pregnant individuals who have been fully immunized previously should receive a Tdap vaccine between 27 and 36 weeks of gestation.
Vaccination stands as the cornerstone in preventing diphtheria.[41] Healthcare providers must educate parents on the benefits of routine immunization in preventing the disease. If a vaccination schedule is missed or records are lost, immediate communication with the primary care provider is essential. Given the waning immunity over time, the timely administration of booster doses becomes paramount for the general population. Community-wide awareness campaigns should emphasize the advantages of immunization. In the event of contact with a suspected case, individuals should promptly seek consultation from healthcare professionals. Moreover, individuals diagnosed with diphtheria must understand the significance of isolation and the necessity to limit contact with the general population until deemed safe by healthcare professionals.
For close contacts with recent exposure to diphtheria, effective management involves close surveillance for respiratory or cutaneous symptoms. Immediate isolation of the patient is essential, coupled with swab collection for culture. Erythromycin administration for a duration of 7 to 10 days is recommended. In cases where the individual's immunization status is uncertain, administering a booster dose of diphtheria toxoid is advisable.
Pearls and Other Issues
Key facts to know about diphtheria include the following:
- Diphtheria, caused by C diphtheriae, primarily affects the respiratory and integumentary systems.
- Clinical presentation includes a distinctive pseudomembrane on the tonsils and throat.
- Timely diagnosis is crucial, involving isolation, antitoxin therapy, and antibiotic treatment.
- Patients with suspected or confirmed diphtheria require immediate isolation and appropriate medical management.
- Incomplete immunization and low antitoxin levels increase susceptibility.
- Vaccination is the primary preventive measure, with DTaP and Tdap vaccines recommended at specific ages.
- Timely booster doses help sustain immunity over time.
Enhancing Healthcare Team Outcomes
Diphtheria often presents with nonspecific upper respiratory tract symptoms like fever, sore throat, dysphagia, and headache, posing a diagnostic challenge due to numerous potential differentials. Therefore, gathering a detailed medical history, including travel and vaccination status, becomes crucial for healthcare providers to narrow down possible diagnoses. The emergence of a pseudomembrane serves as a significant indicator of diphtheria. While pediatricians or primary care providers are typically involved in the care of diphtheria patients, it is imperative to engage an interprofessional team of specialists, including an otorhinolaryngologist and a dermatologist.
Involving infectious disease experts is equally essential in managing diphtheria cases. As vital interprofessional team members, nurses play a crucial role in monitoring the patient's vital signs. Collaboration with radiologists and pathologists is essential for accurate diagnosis. Preventive medicine specialists contribute significantly to minimizing diphtheria outbreaks through awareness campaigns and vaccination programs. Early engagement of cardiologists and neurologists can assist in managing complications that may arise during the disease. Notifying public health experts and international organizations is crucial to raising awareness and facilitating coordinated responses in the event of suspected outbreaks. This comprehensive and collaborative approach ensures a well-rounded and effective response to cases of diphtheria.
The outcome of diphtheria depends on early diagnosis and treatment. A well-coordinated healthcare team is instrumental in achieving this goal, effectively preventing potential morbidity and mortality associated with the disease. Therefore, prompt consultation with an interprofessional team is strongly recommended to enhance outcomes and ensure comprehensive care for individuals affected by diphtheria.[42]